Antineoplastic Combinations Market : Global Industry Analysis 2016 - 2025 and Opportunity Assessment 2026 - 2036
Antineoplastic Combinations Market Size and Share Forecast Outlook 2026 to 2036
Historical Data Covered: 2016 - 2025 | Base Year: 2025 | Estimated Year: 2026 | Forecast Period: 2026 - 2036
Antineoplastic Combinations Market Forecast and Outlook 2026 to 2036
The antineoplastic combinations market is likely to be valued at USD 43,754.0 million in 2026 and reach USD 79,847.8 million by 2036, at a CAGR of 6.2%. Value formation reflects the central role of combination regimens in managing tumors with complex biology and adaptive resistance patterns. Oncology practice increasingly relies on pairing cytotoxic agents with targeted or immune-based therapies to extend response duration rather than intensify single-agent dosing. This structure raises average treatment cost per patient through longer therapy courses and cumulative drug exposure. Spending concentrates in hospital oncology centers equipped for coordinated dosing schedules, toxicity surveillance, and protocol-driven care. Guideline inclusion and reimbursement approval determine scale, as combinations are assessed on incremental survival benefit and tolerability rather than novelty alone. Generic cytotoxic backbones moderate overall cost growth, but branded targeted components anchor pricing and shape budget impact assessments.
Quick Stats for Antineoplastic Combinations Market
- Antineoplastic Combinations Market Value (2026): USD 43,754.0 million
- Antineoplastic Combinations Market Forecast Value (2036): USD 79,847.8 million
- Antineoplastic Combinations Market Forecast CAGR 2026 to 2036: 6.2%
- Leading Product Combination by Demand Share: Chemo + Targeted Therapy
- Fastest-Growing Countries: India, China, Brazil, USA, UK
- Top Players in Global Demand: Roche, Merck, Bristol Myers Squibb, AstraZeneca, Pfizer
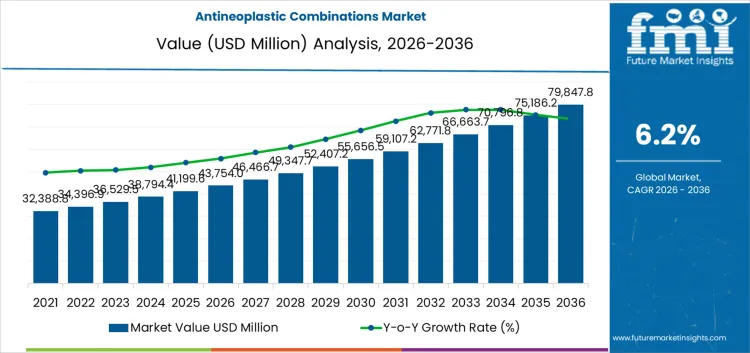
Expansion reflects how treatment pathways have become denser rather than broader. More patients receive multi-agent regimens across successive lines of therapy, increasing total drug utilization over the disease course. Constraints persist through toxicity management capacity, biomarker testing requirements, and payer scrutiny of high-cost combinations. Clinical adoption remains disciplined by evidence maturity, sequencing logic, and real-world tolerability outside trial settings. Operational complexity rises as pharmacies coordinate supply across multiple agents with aligned dosing windows. Health systems with established oncology infrastructure absorb this complexity more readily, while others limit access through protocol restriction. Growth remains supported by outcome-driven protocol adoption and rising treated patient volumes, not by unchecked escalation in combination intensity or unrestricted substitution of single-agent therapies.
Antineoplastic Combinations Market Key Takeaways
| Metric | Value |
|---|---|
| Market Value (2026) | USD 43,754.0 million |
| Market Forecast Value (2036) | USD 79,847.8 million |
| Forecast CAGR 2026 to 2036 | 6.2% |
Why is the Demand for Antineoplastic Combinations Growing?
Demand for antineoplastic combinations is increasing as oncology treatment protocols evolve to manage diverse cancer types with improved therapeutic outcomes. Clinicians prescribe combination regimens that pair cytotoxic agents with targeted therapies or immunomodulators to address tumor heterogeneity, reduce drug resistance, and achieve synergistic action on malignant cells. Treatment guidelines from oncology societies emphasize combination strategies for specific disease states such as advanced solid tumors, hematologic malignancies, and refractory disease where monotherapy often does not achieve sufficient clinical response. Healthcare providers invest in pharmacy preparation, dosing protocols, and treatment monitoring systems to support safe delivery of combination therapies that require careful management of cumulative toxicity and patient tolerance.
Procurement teams evaluate formulary compatibility, stability profiles, and supply continuity to ensure availability across inpatient oncology units, outpatient infusion centers, and specialty clinics. Growth in cancer incidence and expanded screening programs reinforce clinical reliance on antineoplastic combinations that align with evidence based protocols supporting progression free survival and overall survival endpoints. Oncology research continues to characterize molecular pathways and identify agents that enhance efficacy when paired, which encourages adoption of validated combination regimens in treatment plans. Payers and health systems calibrate coverage policies to reflect clinical benefit and cost impact of combination therapies under value based care frameworks. These clinical drivers and operational priorities are contributing to sustained demand growth in the antineoplastic combinations market.
How Are the Segments Classified in the Antineoplastic Combinations Market?
Demand for antineoplastic combinations is shaped by clinical outcomes improvement goals, resistance management strategies, and evolving oncology treatment guidelines. Combination regimens are selected to enhance efficacy through complementary mechanisms of action across cancer types. Adoption aligns with biomarker-driven therapy selection, protocol standardization, and expanding clinical evidence supporting multi-agent use. Treatment selection prioritizes response durability, safety profiles, and compatibility with existing care pathways. Segment classification reflects differentiation by combination product strategy, therapeutic application focus, and end-user care setting, each influencing prescribing patterns, administration complexity, and treatment scalability.
Which Product Combination Holds the Largest Share of Demand?
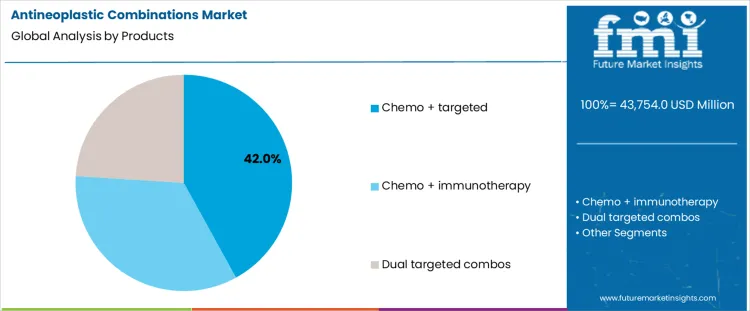
Chemo plus targeted therapy combinations hold 42.0%, representing the largest share among product categories. These regimens integrate cytotoxic backbones with pathway-specific inhibitors to enhance tumor control. Targeted agents improve selectivity while chemotherapy addresses heterogeneous tumor cell populations. Established clinical trial data supports use across multiple solid tumor indications. Chemo plus immunotherapy combinations follow with strong activity in immunogenic cancers. Dual targeted combinations focus on pathway blockade with narrower patient selection. Product segmentation reflects preference for hybrid regimens balancing broad cytotoxic coverage with precision-driven targeting to improve treatment outcomes.
Key Points
-
Hybrid regimens combine cytotoxic and targeted mechanisms.
- Clinical evidence supports broad solid tumor use.
- Other combinations address immune activation or pathway specificity.
How Does Application Segmentation Influence Demand Patterns?
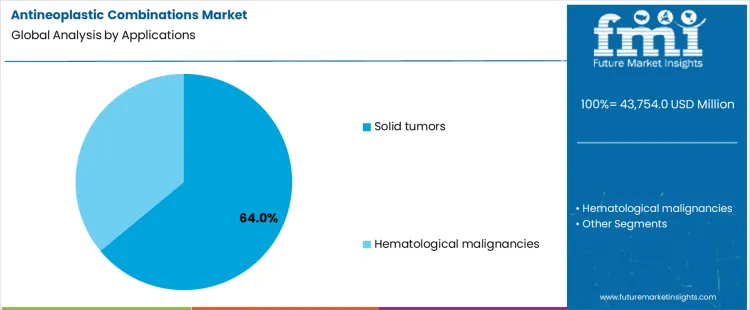
Solid tumor applications account for 64.0%, representing the largest share among therapeutic uses. High prevalence of breast, lung, and gastrointestinal cancers drives extensive combination therapy utilization. Multi-agent regimens address tumor heterogeneity and resistance development in advanced disease stages. Standardized protocols support consistent adoption across oncology practices. Hematological malignancies apply combinations during induction and relapse settings with structured treatment cycles. Application segmentation reflects concentration where disease burden, treatment complexity, and established combination regimens sustain higher utilization across solid tumor oncology care.
Key Points
- Solid tumors represent the majority of combination therapy use.
- Protocol-driven regimens support consistent adoption.
- Hematological uses follow structured, phase-based treatment.
Which End User Accounts for the Highest Share of Demand?
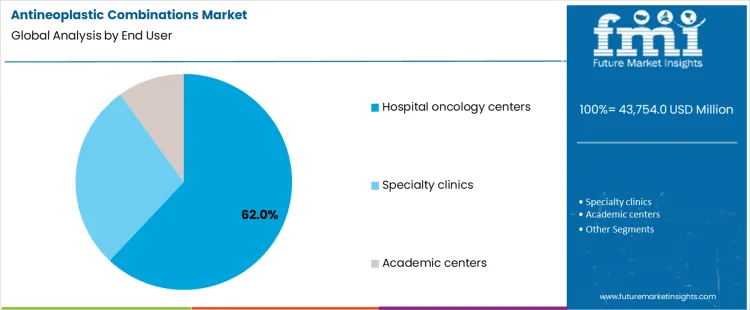
Hospital oncology centers account for 62.0%, representing the largest share among end users. These centers manage complex infusion regimens requiring multidisciplinary oversight. Infrastructure supports combination therapy administration, monitoring, and adverse event management. Centralized pharmacy services enable protocol adherence and dose coordination. Specialty clinics deliver combination treatments with focused outpatient services. Academic centers contribute through clinical trials and guideline development. End-user segmentation reflects concentration where infrastructure, clinical expertise, and patient volume support safe and effective delivery of multi-agent antineoplastic regimens.
Key Points
- Hospitals manage complex combination therapy delivery.
- Centralized services support protocol compliance.
- Other settings focus on outpatient care or research roles.
What are the Key Dynamics in the Antineoplastic Combinations Market?
Demand for antineoplastic combinations reflects oncology treatment strategies that use multiple agents to improve response rates and delay resistance. Adoption concentrates across solid tumors and hematologic malignancies in hospital oncology centers and infusion clinics. Global scope aligns with protocol-driven cancer care and guideline-based regimens. Usage centers on fixed or protocol-defined combinations of cytotoxic agents, targeted therapies, and immunotherapies administered across first-line through salvage settings.
How do clinical synergy requirements and protocol standardization shape adoption?
Cancer treatment often requires multi-agent regimens to address tumor heterogeneity and pathway redundancy. Demand increases where combination therapy delivers additive or synergistic efficacy compared with monotherapy. Standardized protocols define dosing, sequencing, and cycle length, enabling reproducible outcomes across care centers. Combination regimens support higher response rates in curative-intent settings such as lymphomas and early-stage solid tumors. Targeted agents and immunotherapies are frequently layered onto cytotoxic backbones to enhance durability of response. Regulatory approvals tied to specific combinations reinforce adoption within labeled indications. Multidisciplinary oncology practice relies on combination regimens to align surgery, radiation, and systemic therapy. Adoption reflects dependence on evidence-backed protocols that balance efficacy with manageable toxicity.
How do toxicity management complexity and cost exposure influence market scalability?
Combination regimens amplify cumulative toxicity risk, increasing need for supportive care and monitoring infrastructure. Demand sensitivity rises where myelosuppression, cardiotoxicity, or immune-related adverse events limit patient eligibility. Dose modifications and treatment delays affect regimen intensity and outcomes. Drug-drug interactions add prescribing complexity across multi-agent schedules. Cost exposure increases when branded targeted or immune agents are combined with established therapies. Reimbursement policies vary by region and indication, affecting access consistency. Manufacturing and supply coordination across multiple agents increases logistical burden. Resistance emergence still occurs despite combinations, necessitating line-of-therapy progression. Scalability remains constrained by toxicity management capacity, economic pressure, and regimen complexity across diverse oncology settings.
How Is Demand for Antineoplastic Combinations Evolving Globally?
Demand for antineoplastic combinations is expanding globally due to protocol-driven oncology care, rising cancer prevalence, and improved survival outcomes from multi-agent regimens. Combination therapy remains standard across solid tumors and hematological malignancies, integrating cytotoxic, targeted, and supportive agents. Public reimbursement policies and clinical guidelines sustain adoption across hospital oncology settings. Treatment sequencing and resistance management reinforce continued combination use. Growth rates in India at 7.9%, China at 7.7%, Brazil at 7.4%, USA at 6.8%, and the UK at 5.7% indicate sustained expansion driven by patient volume growth, protocol complexity, and access scaling rather than monotherapy substitution.
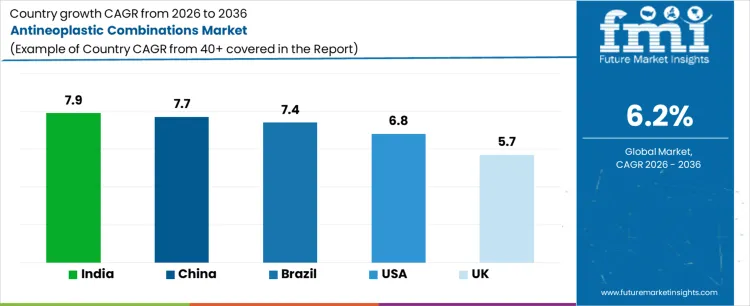
| Country | CAGR (%) |
|---|---|
| India | 7.9% |
| China | 7.7% |
| Brazil | 7.4% |
| USA | 6.8% |
| UK | 5.7% |
What Is Driving Strong Growth of Antineoplastic Combination Demand in India?
Demand for antineoplastic combinations in India is growing at a CAGR of 7.9%, supported by increasing cancer incidence and protocol-based treatment expansion. Public oncology centers rely on multi-drug regimens to improve response rates across common cancers. Government insurance schemes expand coverage for combination therapies within defined treatment pathways. Late-stage diagnosis increases use of aggressive multi-agent protocols. Domestic manufacturing of generics supports affordability and supply continuity. Growth reflects treatment volume expansion and guideline adherence rather than rapid transition toward single-agent targeted therapies.
- Rising cancer incidence and late-stage presentation
- Public oncology center reliance on combination protocols
- Government insurance coverage for defined regimens
- Strong domestic generic drug manufacturing
Why Is China Sustaining Rapid Uptake of Antineoplastic Combination Therapies?
Antineoplastic combination demand in China is expanding at a CAGR of 7.7%, driven by standardized oncology protocols and expanding hospital capacity. National treatment guidelines promote combination regimens to enhance efficacy and manage resistance. Inclusion of multiple agents within reimbursement lists supports utilization. Expansion of oncology services beyond major cities increases patient access. Integration of targeted drugs with cytotoxic backbones remains common. Growth reflects system-wide scaling of protocol-driven care rather than replacement of combinations with novel monotherapies.
- National guideline emphasis on combination regimens
- Reimbursement inclusion for multi-agent therapies
- Oncology service expansion into secondary cities
- Continued integration of targeted and cytotoxic agents
How Is Brazil Supporting Growth in Antineoplastic Combination Usage?
Demand for antineoplastic combinations in Brazil is growing at a CAGR of 7.4%, supported by public healthcare oncology delivery and increasing diagnosis rates. Public hospitals prioritize combination therapies aligned with national treatment guidelines. Limited access to high-cost monotherapies sustains reliance on established multi-agent regimens. Regional oncology center expansion improves treatment reach. Combination protocols address heterogeneous patient responses. Growth reflects public system scale and affordability considerations rather than rapid innovation-driven therapy shifts.
- Public healthcare reliance on guideline-based combinations
- Affordability constraints limiting monotherapy uptake
- Expansion of regional oncology treatment centers
- Protocol use to manage varied patient responses
What Factors Are Driving Antineoplastic Combination Demand in United States?
Antineoplastic combination demand in the United States is expanding at a CAGR of 6.8%, supported by advanced oncology protocols and broad treatment access. Clinical guidelines frequently specify combination regimens to improve outcomes and delay resistance. Insurance coverage supports multi-drug therapy across care settings. High prevalence of complex cancer cases sustains combination usage. Integration of immunotherapy and targeted agents with chemotherapy remains common. Growth reflects protocol sophistication and patient volume stability rather than increased dependence on single-agent therapies.
- Guideline-driven use of multi-agent oncology regimens
- Broad insurance coverage for combination therapies
- High prevalence of complex cancer indications
- Integration of novel agents into combination protocols
Why Is the UK Experiencing Moderate Growth in Antineoplastic Combinations?
Demand for antineoplastic combinations in United Kingdom is growing at a CAGR of 5.7%, driven by NHS treatment pathways and rising cancer prevalence. National clinical guidelines include combination regimens for multiple tumor types. Health technology assessments emphasize cost-effectiveness within combination protocols. Access to novel agents remains selectively managed. Aging demographics increase treated patient volumes. Growth remains moderate, reflecting structured adoption and controlled budget allocation rather than rapid escalation of combination therapy intensity.
- NHS guideline inclusion of combination regimens
- Cost-effectiveness focus in treatment selection
- Selective access to newer oncology agents
- Aging population increasing treatment demand
What is the competitive landscape of demand for the antineoplastic combinations market globally?
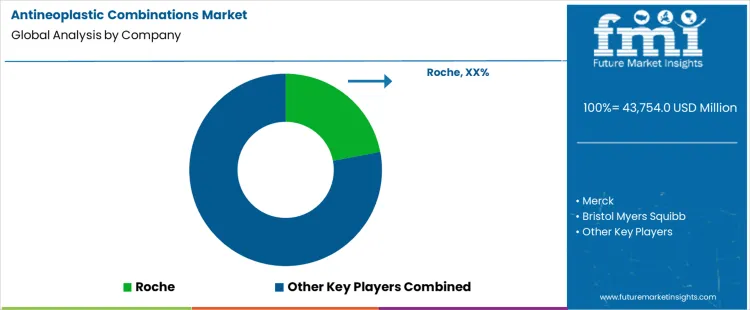
Demand for antineoplastic combinations is driven by clinical evidence supporting multi-mechanism regimens across solid tumors and hematologic malignancies. Oncologists and hospital buyers evaluate survival outcomes, toxicity balance, dosing compatibility, and sequencing flexibility within treatment protocols. Procurement teams assess regulatory approvals by indication, guideline inclusion, pharmacovigilance data, and availability across care settings. Purchasing behavior emphasizes reimbursement alignment, formulary positioning, supply continuity, and manufacturer support for combination trials. Trend in the antineoplastic combinations market reflects expanding use of chemo-immunotherapy and targeted combinations as standard first-line or maintenance regimens in high-incidence cancers.
Roche leads competitive positioning through combination regimens integrating monoclonal antibodies, targeted agents, and backbone chemotherapies across multiple tumor indications. Merck supports demand with checkpoint inhibitor-based combinations supported by extensive clinical development programs. Bristol Myers Squibb competes through dual immunotherapy and chemo-immunotherapy combinations with established adoption in oncology centers. AstraZeneca maintains relevance via targeted therapy combinations paired with chemotherapy in lung, breast, and hematologic cancers. Pfizer participates through combination regimens leveraging oncology portfolios and global commercialization capabilities. Competitive differentiation centers on clinical trial breadth, regulatory reach, guideline inclusion, and sustained manufacturing reliability.
Key Players in the Antineoplastic Combinations Market
- Roche
- Merck
- Bristol Myers Squibb
- AstraZeneca
- Pfizer
- Others
Scope of the Report
| Items | Values |
|---|---|
| Quantitative Units | USD million |
| Products | Chemo + targeted; Chemo + immunotherapy; Dual targeted combos |
| Applications | Solid tumors; Hematological malignancies |
| End User | Hospital oncology centers; Specialty clinics; Academic centers |
| Regions Covered | Asia Pacific, Europe, North America, Latin America, Middle East & Africa |
| Countries Covered | India, China, Brazil, USA, UK, and 40+ countries |
| Key Companies Profiled | Roche; Merck; Bristol Myers Squibb; AstraZeneca; Pfizer; Others |
| Additional Attributes | Dollar sales by product combination, application, end user, and sales channel; clinical adoption driven by efficacy in resistant tumor profiles and line-of-therapy positioning; regimen complexity influencing treatment duration and cost; regulatory approvals shaping combination eligibility; hospital protocol standardization affecting uptake across oncology centers; reimbursement alignment and biomarker testing availability guiding prescribing behavior in solid and hematological malignancies. |
Antineoplastic Combinations Market by Segment
Products:
- Chemo + targeted
- Chemo + immunotherapy
- Dual targeted combos
Applications:
- Solid tumors
- Hematological malignancies
End User:
- Hospital oncology centers
- Specialty clinics
- Academic centers
Region:
- Asia Pacific
- China
- Japan
- South Korea
- India
- Australia & New Zealand
- ASEAN
- Rest of Asia Pacific
- Europe
- Germany
- United Kingdom
- France
- Italy
- Spain
- Nordic
- BENELUX
- Rest of Europe
- North America
- United States
- Canada
- Mexico
- Latin America
- Brazil
- Chile
- Rest of Latin America
- Middle East & Africa
- Kingdom of Saudi Arabia
- Other GCC Countries
- Turkey
- South Africa
- Other African Union
- Rest of Middle East & Africa
Bibliography
- World Health Organization. (2025). Model list of essential medicines: 24th list (antineoplastic and combination therapies). WHO.
- International Agency for Research on Cancer. (2024). Global cancer statistics 2024: Cancer incidence, mortality, and prevalence worldwide. World Health Organization.
- United States Food and Drug Administration. (2024). Clinical considerations for oncology combination products and co-development of antineoplastic agents (FDA Guidance No. CDER-ONC-2024-05). U.S. Department of Health and Human Services.
Frequently Asked Questions
How big is the antineoplastic combinations market in 2026?
The global antineoplastic combinations market is estimated to be valued at USD 43,754.0 million in 2026.
What will be the size of antineoplastic combinations market in 2036?
The market size for the antineoplastic combinations market is projected to reach USD 79,847.8 million by 2036.
How much will be the antineoplastic combinations market growth between 2026 and 2036?
The antineoplastic combinations market is expected to grow at a 6.2% CAGR between 2026 and 2036.
What are the key product types in the antineoplastic combinations market?
The key product types in antineoplastic combinations market are chemo + targeted, chemo + immunotherapy and dual targeted combos.
Which applications segment to contribute significant share in the antineoplastic combinations market in 2026?
In terms of applications, solid tumors segment to command 64.0% share in the antineoplastic combinations market in 2026.
Table of Content
- Executive Summary
- Global Market Outlook
- Demand to side Trends
- Supply to side Trends
- Technology Roadmap Analysis
- Analysis and Recommendations
- Market Overview
- Market Coverage / Taxonomy
- Market Definition / Scope / Limitations
- Market Background
- Market Dynamics
- Drivers
- Restraints
- Opportunity
- Trends
- Scenario Forecast
- Demand in Optimistic Scenario
- Demand in Likely Scenario
- Demand in Conservative Scenario
- Opportunity Map Analysis
- Product Life Cycle Analysis
- Supply Chain Analysis
- Investment Feasibility Matrix
- Value Chain Analysis
- PESTLE and Porter’s Analysis
- Regulatory Landscape
- Regional Parent Market Outlook
- Production and Consumption Statistics
- Import and Export Statistics
- Market Dynamics
- Global Market Analysis 2021 to 2025 and Forecast, 2026 to 2036
- Historical Market Size Value (USD Million) Analysis, 2021 to 2025
- Current and Future Market Size Value (USD Million) Projections, 2026 to 2036
- Y to o to Y Growth Trend Analysis
- Absolute $ Opportunity Analysis
- Global Market Pricing Analysis 2021 to 2025 and Forecast 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Products
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Products , 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Products , 2026 to 2036
- Chemo + targeted
- Chemo + immunotherapy
- Dual targeted combos
- Chemo + targeted
- Y to o to Y Growth Trend Analysis By Products , 2021 to 2025
- Absolute $ Opportunity Analysis By Products , 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Applications
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Applications, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Applications, 2026 to 2036
- Solid tumors
- Hematological malignancies
- Solid tumors
- Y to o to Y Growth Trend Analysis By Applications, 2021 to 2025
- Absolute $ Opportunity Analysis By Applications, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By End User
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By End User, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By End User, 2026 to 2036
- Hospital oncology centers
- Specialty clinics
- Academic centers
- Hospital oncology centers
- Y to o to Y Growth Trend Analysis By End User, 2021 to 2025
- Absolute $ Opportunity Analysis By End User, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Region
- Introduction
- Historical Market Size Value (USD Million) Analysis By Region, 2021 to 2025
- Current Market Size Value (USD Million) Analysis and Forecast By Region, 2026 to 2036
- North America
- Latin America
- Western Europe
- Eastern Europe
- East Asia
- South Asia and Pacific
- Middle East & Africa
- Market Attractiveness Analysis By Region
- North America Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- USA
- Canada
- Mexico
- By Products
- By Applications
- By End User
- By Country
- Market Attractiveness Analysis
- By Country
- By Products
- By Applications
- By End User
- Key Takeaways
- Latin America Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Brazil
- Chile
- Rest of Latin America
- By Products
- By Applications
- By End User
- By Country
- Market Attractiveness Analysis
- By Country
- By Products
- By Applications
- By End User
- Key Takeaways
- Western Europe Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Germany
- UK
- Italy
- Spain
- France
- Nordic
- BENELUX
- Rest of Western Europe
- By Products
- By Applications
- By End User
- By Country
- Market Attractiveness Analysis
- By Country
- By Products
- By Applications
- By End User
- Key Takeaways
- Eastern Europe Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Russia
- Poland
- Hungary
- Balkan & Baltic
- Rest of Eastern Europe
- By Products
- By Applications
- By End User
- By Country
- Market Attractiveness Analysis
- By Country
- By Products
- By Applications
- By End User
- Key Takeaways
- East Asia Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- China
- Japan
- South Korea
- By Products
- By Applications
- By End User
- By Country
- Market Attractiveness Analysis
- By Country
- By Products
- By Applications
- By End User
- Key Takeaways
- South Asia and Pacific Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- India
- ASEAN
- Australia & New Zealand
- Rest of South Asia and Pacific
- By Products
- By Applications
- By End User
- By Country
- Market Attractiveness Analysis
- By Country
- By Products
- By Applications
- By End User
- Key Takeaways
- Middle East & Africa Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Kingdom of Saudi Arabia
- Other GCC Countries
- Turkiye
- South Africa
- Other African Union
- Rest of Middle East & Africa
- By Products
- By Applications
- By End User
- By Country
- Market Attractiveness Analysis
- By Country
- By Products
- By Applications
- By End User
- Key Takeaways
- Key Countries Market Analysis
- USA
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Canada
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Mexico
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Brazil
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Chile
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Germany
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- UK
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Italy
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Spain
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- France
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- India
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- ASEAN
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Australia & New Zealand
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- China
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Japan
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- South Korea
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Russia
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Poland
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Hungary
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Kingdom of Saudi Arabia
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Turkiye
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- South Africa
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- USA
- Market Structure Analysis
- Competition Dashboard
- Competition Benchmarking
- Market Share Analysis of Top Players
- By Regional
- By Products
- By Applications
- By End User
- Competition Analysis
- Competition Deep Dive
- Roche
- Overview
- Product Portfolio
- Profitability by Market Segments (Product/Age /Sales Channel/Region)
- Sales Footprint
- Strategy Overview
- Marketing Strategy
- Product Strategy
- Channel Strategy
- Merck
- Bristol Myers Squibb
- AstraZeneca
- Pfizer
- Others
- Roche
- Competition Deep Dive
- Assumptions & Acronyms Used
- Research Methodology
List of Tables
- Table 1: Global Market Value (USD Million) Forecast by Region, 2021 to 2036
- Table 2: Global Market Value (USD Million) Forecast by Products , 2021 to 2036
- Table 3: Global Market Value (USD Million) Forecast by Applications, 2021 to 2036
- Table 4: Global Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 5: North America Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 6: North America Market Value (USD Million) Forecast by Products , 2021 to 2036
- Table 7: North America Market Value (USD Million) Forecast by Applications, 2021 to 2036
- Table 8: North America Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 9: Latin America Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 10: Latin America Market Value (USD Million) Forecast by Products , 2021 to 2036
- Table 11: Latin America Market Value (USD Million) Forecast by Applications, 2021 to 2036
- Table 12: Latin America Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 13: Western Europe Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 14: Western Europe Market Value (USD Million) Forecast by Products , 2021 to 2036
- Table 15: Western Europe Market Value (USD Million) Forecast by Applications, 2021 to 2036
- Table 16: Western Europe Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 17: Eastern Europe Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 18: Eastern Europe Market Value (USD Million) Forecast by Products , 2021 to 2036
- Table 19: Eastern Europe Market Value (USD Million) Forecast by Applications, 2021 to 2036
- Table 20: Eastern Europe Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 21: East Asia Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 22: East Asia Market Value (USD Million) Forecast by Products , 2021 to 2036
- Table 23: East Asia Market Value (USD Million) Forecast by Applications, 2021 to 2036
- Table 24: East Asia Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 25: South Asia and Pacific Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 26: South Asia and Pacific Market Value (USD Million) Forecast by Products , 2021 to 2036
- Table 27: South Asia and Pacific Market Value (USD Million) Forecast by Applications, 2021 to 2036
- Table 28: South Asia and Pacific Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 29: Middle East & Africa Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 30: Middle East & Africa Market Value (USD Million) Forecast by Products , 2021 to 2036
- Table 31: Middle East & Africa Market Value (USD Million) Forecast by Applications, 2021 to 2036
- Table 32: Middle East & Africa Market Value (USD Million) Forecast by End User, 2021 to 2036
List of Figures
- Figure 1: Global Market Pricing Analysis
- Figure 2: Global Market Value (USD Million) Forecast 2021 to 2036
- Figure 3: Global Market Value Share and BPS Analysis by Products , 2026 and 2036
- Figure 4: Global Market Y-o-Y Growth Comparison by Products , 2026 to 2036
- Figure 5: Global Market Attractiveness Analysis by Products
- Figure 6: Global Market Value Share and BPS Analysis by Applications, 2026 and 2036
- Figure 7: Global Market Y-o-Y Growth Comparison by Applications, 2026 to 2036
- Figure 8: Global Market Attractiveness Analysis by Applications
- Figure 9: Global Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 10: Global Market Y-o-Y Growth Comparison by End User, 2026 to 2036
- Figure 11: Global Market Attractiveness Analysis by End User
- Figure 12: Global Market Value (USD Million) Share and BPS Analysis by Region, 2026 and 2036
- Figure 13: Global Market Y-o-Y Growth Comparison by Region, 2026 to 2036
- Figure 14: Global Market Attractiveness Analysis by Region
- Figure 15: North America Market Incremental Dollar Opportunity, 2026 to 2036
- Figure 16: Latin America Market Incremental Dollar Opportunity, 2026 to 2036
- Figure 17: Western Europe Market Incremental Dollar Opportunity, 2026 to 2036
- Figure 18: Eastern Europe Market Incremental Dollar Opportunity, 2026 to 2036
- Figure 19: East Asia Market Incremental Dollar Opportunity, 2026 to 2036
- Figure 20: South Asia and Pacific Market Incremental Dollar Opportunity, 2026 to 2036
- Figure 21: Middle East & Africa Market Incremental Dollar Opportunity, 2026 to 2036
- Figure 22: North America Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 23: North America Market Value Share and BPS Analysis by Products , 2026 and 2036
- Figure 24: North America Market Y-o-Y Growth Comparison by Products , 2026 to 2036
- Figure 25: North America Market Attractiveness Analysis by Products
- Figure 26: North America Market Value Share and BPS Analysis by Applications, 2026 and 2036
- Figure 27: North America Market Y-o-Y Growth Comparison by Applications, 2026 to 2036
- Figure 28: North America Market Attractiveness Analysis by Applications
- Figure 29: North America Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 30: North America Market Y-o-Y Growth Comparison by End User, 2026 to 2036
- Figure 31: North America Market Attractiveness Analysis by End User
- Figure 32: Latin America Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 33: Latin America Market Value Share and BPS Analysis by Products , 2026 and 2036
- Figure 34: Latin America Market Y-o-Y Growth Comparison by Products , 2026 to 2036
- Figure 35: Latin America Market Attractiveness Analysis by Products
- Figure 36: Latin America Market Value Share and BPS Analysis by Applications, 2026 and 2036
- Figure 37: Latin America Market Y-o-Y Growth Comparison by Applications, 2026 to 2036
- Figure 38: Latin America Market Attractiveness Analysis by Applications
- Figure 39: Latin America Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 40: Latin America Market Y-o-Y Growth Comparison by End User, 2026 to 2036
- Figure 41: Latin America Market Attractiveness Analysis by End User
- Figure 42: Western Europe Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 43: Western Europe Market Value Share and BPS Analysis by Products , 2026 and 2036
- Figure 44: Western Europe Market Y-o-Y Growth Comparison by Products , 2026 to 2036
- Figure 45: Western Europe Market Attractiveness Analysis by Products
- Figure 46: Western Europe Market Value Share and BPS Analysis by Applications, 2026 and 2036
- Figure 47: Western Europe Market Y-o-Y Growth Comparison by Applications, 2026 to 2036
- Figure 48: Western Europe Market Attractiveness Analysis by Applications
- Figure 49: Western Europe Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 50: Western Europe Market Y-o-Y Growth Comparison by End User, 2026 to 2036
- Figure 51: Western Europe Market Attractiveness Analysis by End User
- Figure 52: Eastern Europe Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 53: Eastern Europe Market Value Share and BPS Analysis by Products , 2026 and 2036
- Figure 54: Eastern Europe Market Y-o-Y Growth Comparison by Products , 2026 to 2036
- Figure 55: Eastern Europe Market Attractiveness Analysis by Products
- Figure 56: Eastern Europe Market Value Share and BPS Analysis by Applications, 2026 and 2036
- Figure 57: Eastern Europe Market Y-o-Y Growth Comparison by Applications, 2026 to 2036
- Figure 58: Eastern Europe Market Attractiveness Analysis by Applications
- Figure 59: Eastern Europe Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 60: Eastern Europe Market Y-o-Y Growth Comparison by End User, 2026 to 2036
- Figure 61: Eastern Europe Market Attractiveness Analysis by End User
- Figure 62: East Asia Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 63: East Asia Market Value Share and BPS Analysis by Products , 2026 and 2036
- Figure 64: East Asia Market Y-o-Y Growth Comparison by Products , 2026 to 2036
- Figure 65: East Asia Market Attractiveness Analysis by Products
- Figure 66: East Asia Market Value Share and BPS Analysis by Applications, 2026 and 2036
- Figure 67: East Asia Market Y-o-Y Growth Comparison by Applications, 2026 to 2036
- Figure 68: East Asia Market Attractiveness Analysis by Applications
- Figure 69: East Asia Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 70: East Asia Market Y-o-Y Growth Comparison by End User, 2026 to 2036
- Figure 71: East Asia Market Attractiveness Analysis by End User
- Figure 72: South Asia and Pacific Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 73: South Asia and Pacific Market Value Share and BPS Analysis by Products , 2026 and 2036
- Figure 74: South Asia and Pacific Market Y-o-Y Growth Comparison by Products , 2026 to 2036
- Figure 75: South Asia and Pacific Market Attractiveness Analysis by Products
- Figure 76: South Asia and Pacific Market Value Share and BPS Analysis by Applications, 2026 and 2036
- Figure 77: South Asia and Pacific Market Y-o-Y Growth Comparison by Applications, 2026 to 2036
- Figure 78: South Asia and Pacific Market Attractiveness Analysis by Applications
- Figure 79: South Asia and Pacific Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 80: South Asia and Pacific Market Y-o-Y Growth Comparison by End User, 2026 to 2036
- Figure 81: South Asia and Pacific Market Attractiveness Analysis by End User
- Figure 82: Middle East & Africa Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 83: Middle East & Africa Market Value Share and BPS Analysis by Products , 2026 and 2036
- Figure 84: Middle East & Africa Market Y-o-Y Growth Comparison by Products , 2026 to 2036
- Figure 85: Middle East & Africa Market Attractiveness Analysis by Products
- Figure 86: Middle East & Africa Market Value Share and BPS Analysis by Applications, 2026 and 2036
- Figure 87: Middle East & Africa Market Y-o-Y Growth Comparison by Applications, 2026 to 2036
- Figure 88: Middle East & Africa Market Attractiveness Analysis by Applications
- Figure 89: Middle East & Africa Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 90: Middle East & Africa Market Y-o-Y Growth Comparison by End User, 2026 to 2036
- Figure 91: Middle East & Africa Market Attractiveness Analysis by End User
- Figure 92: Global Market - Tier Structure Analysis
- Figure 93: Global Market - Company Share Analysis

