South Korea established universal Electronic Medical Records adoption earlier than most developed nations through coordinated national policy combined with robust telecommunications infrastructure. The Ministry of Health and Welfare promoted digital health transformation through regulatory incentives, funding mechanisms and standardisation efforts beginning in the early 2000s. Unlike fragmented adoption patterns observed in many countries, South Korean policy created systematic momentum across hospital tiers.
Broadband penetration and telecommunications advancement provided foundational infrastructure enabling cloud based architectures, real time data exchange and high resolution medical imaging transmission. South Korea consistently ranks among global leaders in internet speed and network reliability. This connectivity advantage removed technical barriers that constrained EMR functionality in bandwidth limited environments. Hospitals could deploy advanced features without concerns about network capacity or latency affecting clinical workflows.
Hospital competition dynamics uniquely intensified digital capability development in South Korea. The healthcare system features numerous large tertiary hospitals competing for patient volume and reputation within major metropolitan areas. Unlike single dominant hospital systems common in other nations, South Korean cities host multiple academic medical centers vying for clinical excellence recognition. This competitive pressure creates continuous incentive to differentiate through technology adoption, patient convenience and treatment outcomes visibility.
Historical EMR adoption followed a rapid trajectory once initial systems demonstrated value. Early adopters among university hospitals showcased efficiency gains and quality improvements, creating demonstration effects that accelerated diffusion. Provider associations and professional societies promoted best practices and standardisation. Government certification programs established minimum functionality requirements while allowing competitive differentiation on advanced features. This combination of baseline standards with innovation space enabled both widespread adoption and capability advancement.
Cultural factors reinforcing digital adoption include high technology literacy among clinical staff, patient expectations for digital convenience and administrative efficiency priorities. South Korean physicians generally demonstrate strong computer proficiency and receptiveness to clinical decision support tools. Patients increasingly expect electronic appointment scheduling, test result access and digital communication channels. Hospital administrators face pressure to optimise resource utilisation and reduce administrative overhead through automation.
Tertiary hospitals in South Korea treat substantially more complex case mixes than primary or secondary facilities, creating demand for sophisticated clinical documentation and decision support capabilities. These institutions handle rare diseases, complex surgical procedures and patients with multiple comorbidities requiring multidisciplinary coordination. Standard EMR templates designed for routine care prove inadequate for documenting nuanced clinical reasoning, specialty specific assessments and intricate treatment protocols. Advanced systems provide configurable templates, specialty modules and structured data entry supporting complex care documentation.
Research orientation at university hospitals necessitates EMR architectures facilitating data extraction for clinical studies and quality improvement initiatives. Research teams require structured data capture enabling cohort identification, outcome tracking and statistical analysis. Leading South Korean academic medical centers integrate research data management systems with clinical EMRs, allowing seamless transition from clinical documentation to research datasets. This integration demands sophisticated data architecture, standardised terminologies and query capabilities exceeding requirements at non academic facilities.
Teaching hospital requirements add another functionality dimension as medical education programs depend on EMR systems for trainee supervision, case review and competency assessment. Attending physicians must review and co-sign trainee documentation. Educational programs track procedure volumes, patient exposure diversity and clinical milestones through EMR data. Advanced systems provide educational dashboards, competency tracking modules and structured feedback mechanisms. These teaching specific features drive additional development investment concentrated at academic centers.
Quality reporting and performance monitoring intensify at tertiary hospitals pursuing national rankings and international accreditation. South Korean university hospitals compete for recognition in regional hospital rankings and global academic medical center assessments. These reputation systems increasingly weight quality metrics, patient safety indicators and clinical outcome measures. EMR systems must capture structured quality data, automate reporting workflows and provide real time performance dashboards. Hospitals unable to demonstrate objective quality metrics through robust data systems face competitive disadvantages.
Multidisciplinary care coordination demands at tertiary facilities require EMR functionality enabling seamless information sharing across specialties, departments and care settings. Complex patients receive care from numerous specialists who must access comprehensive patient histories, review test results from multiple departments and coordinate treatment plans. Advanced EMR systems provide unified patient views, cross departmental messaging and care plan visibility. Integration depth differentiates sophisticated systems from basic documentation platforms.
Government supported smart hospital programs established technology standards, funded pilot implementations and created demonstration sites showcasing advanced digital health capabilities. The Ministry of Health and Welfare designated specific hospitals as smart hospital development sites, providing financial support for innovative technology deployment. These programs accelerated adoption of emerging capabilities including artificial intelligence integration, Internet of Things sensor networks and advanced analytics platforms. Vendors targeting South Korean hospitals must align product roadmaps with smart hospital initiative priorities.
Interoperability mandates within smart hospital frameworks require EMR vendors to support standardised data exchange protocols including HL7 FHIR and DICOM for medical imaging. Government programs established certification requirements ensuring systems can exchange patient data across institutions and integrate with national health information networks. Vendors cannot compete effectively without demonstrated interoperability compliance. This regulatory requirement prevents proprietary data lock in strategies and forces investment in standards based architectures.
Data platform requirements in smart hospital programs emphasise structured data capture, analytics readiness and algorithm compatibility. Government initiatives promote clinical decision support algorithm development and deployment, necessitating EMR architectures exposing structured clinical data through application programming interfaces. Vendors must design data models supporting machine learning applications, real time risk prediction and population health analytics. Systems with unstructured text based documentation cannot meet smart hospital data platform expectations.
Integration mandates with imaging, pharmacy and laboratory systems create comprehensive digital ecosystem requirements. Smart hospital certification assesses seamless workflow integration across hospital departments. PACS integration must enable radiologists and clinicians to access imaging directly within EMR workflows. Pharmacy systems must support computerised physician order entry with clinical decision support for drug interactions and allergies. Laboratory integration requires bidirectional communication with automated result delivery and critical value alerting. Vendors offering partial integration face disadvantages against comprehensive platform providers.
Cybersecurity requirements within government programs mandate robust data protection, access controls and audit capabilities. Smart hospital initiatives established security standards aligned with international healthcare data protection frameworks. EMR vendors must demonstrate encryption capabilities, role based access controls, comprehensive audit logging and incident response procedures. Security certification becomes table stakes for participating in smart hospital procurements.
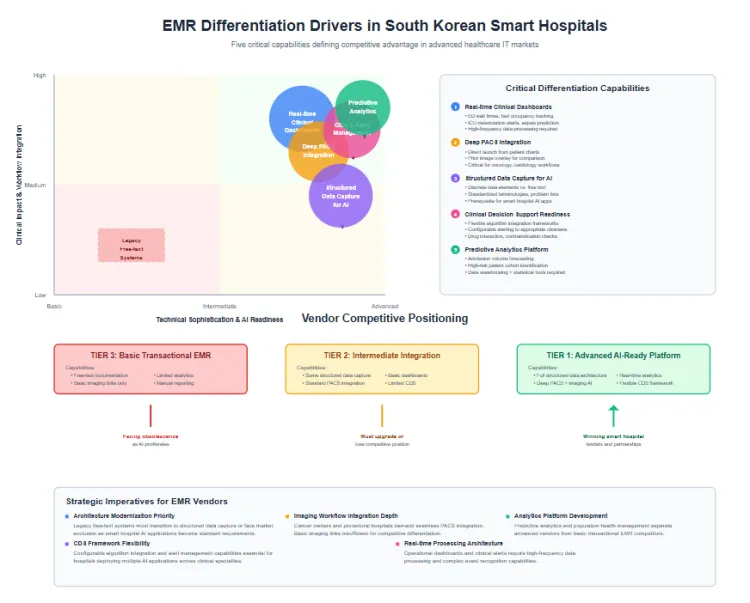
Real time clinical dashboards emerged as critical differentiation factors as hospitals compete on operational efficiency and outcome transparency. Leading South Korean hospital systems deploy executive dashboards displaying emergency department wait times, bed occupancy, surgical throughput and quality metrics updated continuously. Clinical dashboards provide intensive care unit teams with patient deterioration alerts, sepsis risk predictions and ventilator weaning readiness indicators. These real time intelligence capabilities require EMR architectures with high frequency data processing, complex event recognition and visualisation sophistication.
PACS integration depth determines workflow efficiency for image intensive specialties including radiology, cardiology and oncology. Advanced integration enables clinicians to launch imaging studies directly from patient charts, overlay prior imaging for comparison and annotate images within integrated viewers. South Korean hospitals treating high volumes of cancer patients and performing complex procedures demand seamless imaging access during clinical decision making. Vendors offering basic imaging links cannot match workflow efficiency of deeply integrated solutions.
Structured data capture mechanisms prepare EMR systems for clinical decision support algorithm deployment. South Korean smart hospital initiatives promote AI applications including diagnostic support, treatment recommendation and patient deterioration prediction. These algorithms require structured input data rather than free text clinical notes. Leading EMR vendors redesigned documentation interfaces to capture discrete data elements, standardised terminologies and structured problem lists. Systems retaining legacy free text documentation architectures face obsolescence as AI applications proliferate.
Clinical decision support readiness extends beyond data structure to include algorithm integration frameworks and alert management capabilities. Hospitals deploying sepsis prediction algorithms require EMR platforms that execute risk calculations continuously, deliver alerts to appropriate clinicians and track response actions. Medication safety algorithms checking for drug interactions and contraindications must integrate seamlessly into prescribing workflows. Vendor platforms with flexible algorithm integration architectures and configurable alerting win competitive differentiation.
Predictive analytics capabilities for population health management and resource planning represent advanced functionality tiers. South Korean hospitals use EMR data to predict admission volumes, identify high risk patient cohorts and optimise staffing allocation. These applications require data warehousing capabilities, statistical analysis tools and forecasting algorithms. Vendors offering basic transactional EMR functionality without analytics platforms cannot address sophisticated hospital requirements.
South Korean tertiary hospitals allocate IT budgets exceeding global benchmarks, with expenditures per bed substantially higher than regional averages. This investment capacity enables comprehensive system implementations including full clinical workflows, departmental integrations and advanced analytics modules. High spending levels support extensive vendor services including customisation, training, optimisation and continuous enhancement. Vendors price premium offerings confidently knowing leading hospitals possess budget authority for sophisticated implementations.
Procurement processes at major South Korean hospitals emphasise long term partnerships over transactional vendor relationships. Hospitals recognise that EMR implementations require years of workflow optimisation, user training and continuous enhancement. Request for proposal evaluations assess vendor stability, upgrade pathways and commitment to innovation alongside current functionality. Selection committees include clinical leadership, IT staff and hospital administration to ensure comprehensive stakeholder alignment. Winning vendors establish deep relationships extending across organisational levels.
Multi year contracts with guaranteed upgrade and support commitments provide revenue predictability enabling sustained vendor investment in platform advancement. South Korean hospital contracts typically span five to ten years with renewal provisions. These agreements include service level commitments, regular feature releases and dedicated support resources. Long contract duration justifies vendor investment in hospital specific customisations and integration development. Pricing includes both license fees and ongoing support costs calculated across contract lifespans.
Customisation depth at large South Korean hospitals creates significant system specificity that elevates switching costs. Tertiary hospitals configure EMR systems extensively to match specialty workflows, clinical protocols and departmental preferences. Custom order sets, clinical templates, decision support rules and interface configurations accumulate over implementation years. Switching vendors would require rebuilding this customisation library, retraining thousands of users and managing clinical workflow disruption. These switching barriers provide pricing resilience to incumbent vendors during contract renewals.
Integration complexity with departmental systems, medical devices and analytics platforms creates technical lock in that reinforces vendor relationships. South Korean hospitals connect EMR systems to dozens of ancillary systems including PACS, laboratory information systems, pharmacy systems, surgical scheduling platforms and billing systems. Each integration represents development investment, interface testing and ongoing maintenance. Replacing core EMR platforms necessitates rebuilding entire integration ecosystems. This technical interdependency makes vendor switching prohibitively disruptive for established implementations.
SOURCES
South Korean tertiary hospitals compete intensely on clinical reputation, research productivity and patient satisfaction, creating strong incentive to differentiate through digital capability. Government smart hospital programs provide funding support and establish digital excellence as accreditation criterion. High IT literacy among clinical staff and patients increases receptiveness to advanced features. These factors combine to justify IT investment levels exceeding many international peers.
Integrated systems eliminate workflow interruptions from switching between applications and manual data transcription. Clinicians access all patient information within unified interfaces, reducing time spent navigating multiple systems. Automated result delivery and critical value alerts accelerate clinical decision making. Order entry integration with clinical decision support reduces errors and inappropriate test ordering. These efficiency gains translate to faster treatment initiation and improved throughput.
Extensive workflow customisation, interface integrations with departmental systems, accumulated clinical templates and user training investment create high switching costs. Rebuilding customisations requires months of configuration work. Interface redevelopment and testing disrupts integrated workflows. Staff retraining impacts productivity across thousands of users. Clinical workflow changes during transitions risk safety incidents. These barriers make switching economically and operationally prohibitive for established implementations.
South Korean smart hospital programs emphasise AI capability deployment, making algorithm compatibility a competitive requirement. Hospitals evaluate EMR architectures for structured data capture, API availability and real time processing capability needed for AI applications. Systems unable to support clinical decision support algorithms face obsolescence as AI adoption accelerates. AI readiness becomes purchasing criterion even before specific algorithms are deployed.
Core principles including government coordination, interoperability standards and competitive quality transparency apply broadly. However, South Korean implementation intensity requires substantial per bed IT investment and high technology literacy among clinical staff. Lower resource settings may adopt simplified versions focusing on essential interoperability and basic clinical decision support. Full replication of advanced analytics and deep integration requires comparable investment commitment and infrastructure maturity.
Medical Electronics Market Analysis by Type, Application, Component, and Region through 2025 to 2035
Electronic Batch Records Market Analysis by End User and Region through 2035
The Medical-Grade Flexible Electronics Bending and Fatigue Test Systems Market is segmented by Test Mode (Cyclic Bending, Dynamic Fatigue, Torsion, Peel, Custom Fixtures), System Type (Benchtop, Electrodynamic, Servohydraulic, Micro-force, Environmental), Application (Wearable Patches, Implantables, Smart Catheters, Neuro Interfaces, Biosensor Strips), End User (Medtech OEMs, Contract Labs, University Labs, CDMOs, Hospitals), Sales Channel (Direct Sales, Distributors, Integrators, Service Contracts, Retrofits), and Region.
USA Electronic Health Records (EHR) Market Size and Share Forecast Outlook 2025 to 2035
The electronics adhesives market is segmented by Chemistry (Epoxy, Silicone, Acrylic, Polyurethane, UV-curable and Specialty Adhesives), Application (Encapsulation, Surface Mounting, Conformal Coating Support, Thermal Management Bonding, Wire Tacking and Component Assembly, Display and Sensor Bonding), Formulation Type (Conductive Adhesives, Non-conductive Adhesives, Thermally Conductive Adhesives, Optically Clear Adhesives), End-use Industry (Consumer Electronics, Semiconductors and Packaging, Automotive Electronics, Telecommunications, Industrial Electronics, Medical Electronics), Curing Method (Heat Cure, UV Cure, Moisture Cure, Dual Cure), Sales Channel (Direct OEM Supply, Electronics Manufacturing Service Providers, Industrial Distributors, Contract Formulators), and Region. Forecast for 2026 to 2036.