Service led deployment fundamentally restructures the financial profile of mobile gamma camera acquisition by replacing large upfront capital commitments with predictable operating expenditures. Traditional fixed nuclear imaging systems require substantial capital outlays ranging from several hundred thousand to over one million dollars, creating budget approval barriers and long depreciation schedules. Mobile gamma cameras increasingly deploy through leasing structures that convert this capital expense into monthly or annual operating costs, enabling hospitals to preserve capital reserves for other strategic priorities while maintaining access to current imaging technology.
Leasing models typically bundle equipment access with comprehensive service agreements, creating all inclusive pricing that covers maintenance, calibration, regulatory compliance support, and technology refresh cycles. Pay per use arrangements further reduce financial risk by aligning costs directly with clinical utilisation, particularly attractive for facilities with variable nuclear medicine volumes or seasonal demand patterns. Hospitals avoid the residual value risk inherent in outright purchases, as leasing transfers obsolescence exposure to lessors who maintain incentives to optimise asset lifecycle management.
Bundled service agreements embedded within leasing structures eliminate the uncertainty of unplanned maintenance costs and provide budget predictability that hospital finance departments value highly. These contracts typically guarantee uptime levels, response times, and parts availability, shifting operational risk from the hospital to the vendor. The economic advantage intensifies when comparing service inclusive leasing payments against the combined cost of equipment purchase, separate service contracts, and internal administration of maintenance scheduling and regulatory documentation for owned assets.
Mobile gamma cameras achieve superior utilisation rates by serving multiple clinical locations and applications within a single institution, contrasting sharply with fixed systems confined to dedicated nuclear medicine suites. A single mobile unit can support morning thyroid imaging in endocrinology, afternoon sentinel lymph node procedures in surgical suites, and evening cardiac studies in the catheterisation laboratory, maximising productive hours per day compared to stationary equipment that remains idle outside scheduled nuclear medicine appointments.
Shared use models extend this utilisation advantage across organisational boundaries. Hospital systems deploy mobile gamma cameras among satellite facilities, ambulatory surgery centres, and community hospitals that individually lack sufficient volume to justify dedicated fixed installations. This rotation strategy ensures each facility accesses nuclear imaging capability when needed while distributing acquisition and service costs across multiple sites and revenue streams. The mobile unit operates at higher aggregate utilisation than any single fixed system at individual low volume locations.
Surgical applications particularly benefit from mobile deployment economics. Intraoperative gamma cameras support sentinel node biopsy and radioguided surgery without requiring permanent installation in operating rooms where space commands premium value. Hospitals avoid dedicating expensive surgical real estate to specialised imaging equipment that serves only specific procedure types, instead deploying mobile units on demand when clinical protocols require intraoperative nuclear imaging. This flexibility improves both surgical suite utilisation and imaging equipment utilisation simultaneously.
The elimination of patient transport represents an additional utilisation advantage. Mobile gamma cameras travel to patients in intensive care units, emergency departments, and procedural areas where moving critically ill or immediate post operative patients to fixed nuclear medicine departments creates clinical risk and logistical complexity. Bedside imaging capability expands the practical patient population for nuclear studies while reducing delays that would otherwise leave fixed equipment idle awaiting patient arrival.
Comprehensive service contracts bundled with mobile gamma camera deployment shift multiple cost categories from unpredictable, hospital borne expenses to fixed vendor responsibilities with guaranteed performance levels. Preventive maintenance schedules maintained by vendors ensure optimal detector performance and image quality while identifying potential component failures before they cause unplanned downtime. Hospitals avoid the internal costs of employing specialised nuclear imaging equipment technicians or contracting third party service providers on reactive, premium priced terms when failures occur.
Uptime guarantees embedded in service agreements create vendor accountability for operational availability that directly protects clinical revenue. When mobile gamma cameras experience failures, service contracts typically mandate response times measured in hours rather than days, with loaner equipment provisions ensuring clinical continuity. This guaranteed availability reduces the revenue volatility associated with unplanned outages that force procedure cancellations, patient rescheduling, and potential referral of cases to competing facilities.
Radiation safety and regulatory compliance support within service contracts addresses costs that hospitals otherwise manage through internal radiation safety departments or external consultants. Vendors provide calibration documentation, quality assurance testing records, and regulatory submission support required by nuclear regulatory authorities. Mobile gamma camera service agreements commonly include radiation shielding assessment, staff dosimetry guidance, and updated safety protocols when equipment relocates among clinical areas with different physical characteristics and use patterns.
Documentation services reduce administrative burden on hospital radiation safety officers and nuclear medicine technologists who otherwise devote substantial time to compliance recordkeeping. Vendor maintained service logs, calibration certificates, and performance verification reports satisfy regulatory inspection requirements while freeing clinical staff to focus on patient care rather than administrative documentation. This labour cost avoidance, though difficult to quantify precisely, contributes meaningfully to total cost of ownership advantages.
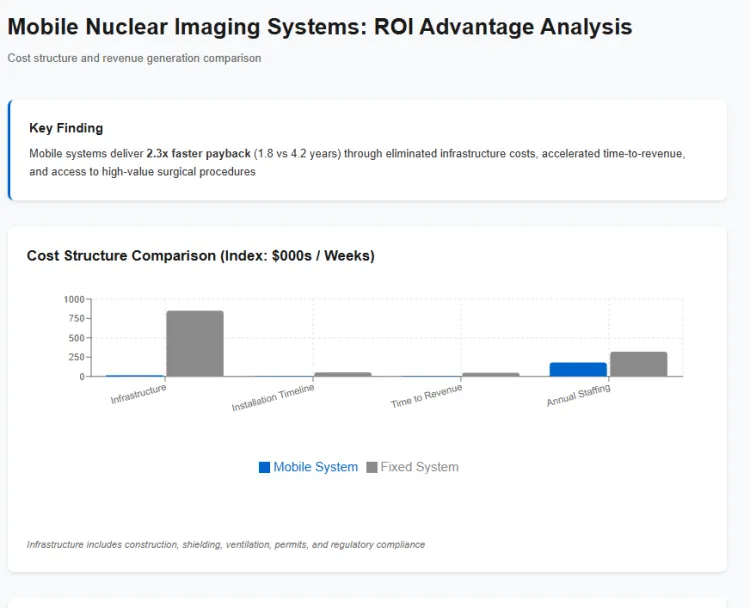
Mobile gamma camera ROI calculations exclude major cost categories required for fixed nuclear medicine installations, fundamentally altering payback period assessments. Hospitals avoid constructing dedicated shielded imaging rooms, eliminating architectural design fees, building permits, construction management, and installation timelines measured in months or years. A fixed nuclear medicine suite requires lead lined walls, specialised ventilation, radiation monitoring equipment, and compliance with stringent regulatory standards governing permanent nuclear medicine facilities. Mobile systems operate within existing clinical spaces using temporary shielding if necessary, reducing facility modification costs to minor electrical and network connectivity requirements.
The time to revenue generation differs dramatically between mobile and fixed systems. Mobile gamma cameras can begin generating clinical revenue within weeks of deployment following staff training and basic operational setup. Fixed installations require prolonged planning, construction, regulatory approval, and commissioning processes that defer revenue realisation for extended periods while capital costs accumulate. This accelerated time to clinical productivity improves ROI calculations substantially, particularly for hospitals requiring rapid capacity expansion or service line development.
Revenue opportunity calculations increasingly favour mobile systems for hospitals pursuing procedural volume growth in surgical and interventional applications. Sentinel lymph node mapping and radioguided surgery generate higher reimbursement per procedure than many diagnostic nuclear imaging studies, yet require imaging capability in operating rooms and procedural suites rather than diagnostic departments. Mobile deployment captures this high value clinical revenue without the impossibility of installing fixed nuclear imaging equipment in surgical environments designed for other purposes.
Avoided costs extend to staff optimisation. Mobile gamma cameras enable nuclear medicine technologists to serve multiple departments and facilities rather than remaining dedicated to single fixed locations with variable scheduling demands. This workforce flexibility reduces idle labour costs during slow periods and enables institutions to match staffing levels to actual imaging volumes rather than maintaining constant coverage for dedicated fixed installations.
Original equipment manufacturer service strategies increasingly emphasise long term customer relationships over transactional equipment sales, recognising that predictable service revenue streams provide more stable business models than episodic capital equipment purchases. OEMs structure service contracts with pricing that encourages multi year commitments, offering progressively lower annual costs for extended terms that lock hospitals into specific vendor relationships. These pricing strategies benefit both parties when vendors deliver reliable service, but create switching costs that hospital procurement must evaluate carefully.
Upgrade pathways embedded within service agreements influence renewal decisions by offering technology refresh options at predetermined pricing rather than requiring full replacement purchases. Hospitals gain access to detector improvements, software enhancements, and connectivity upgrades without capital budget approval processes, maintaining competitive imaging capability through evolutionary rather than revolutionary equipment changes. This approach extends effective equipment lifecycles and smooths technology adoption costs across longer periods.
Vendor lock in dynamics emerge when hospitals become dependent on proprietary service networks, specialised training, and integration with existing vendor ecosystems. OEMs leverage installed base relationships to cross sell complementary imaging modalities, enterprise imaging software, and professional services that deepen customer dependence on single vendor solutions. Hospital procurement officers increasingly evaluate total vendor relationship costs rather than isolated equipment or service pricing, assessing whether OEM service strategies align with institutional goals for flexibility and competitive leverage.
Service pricing transparency varies significantly among OEMs, with some vendors providing clear, published service rates while others negotiate pricing based on institutional relationships and competitive dynamics. Hospitals with strong procurement capabilities extract favourable terms by benchmarking service costs across vendors and demanding performance based pricing tied to uptime guarantees and response time commitments. Weak service pricing transparency creates information asymmetry that disadvantages hospitals lacking sophisticated procurement analytics.
The shift toward subscription based models where hospitals essentially rent imaging capability rather than owning equipment represents the logical endpoint of service intensive commercialisation. These models transfer all ownership risks to vendors while providing hospitals maximum flexibility to adopt emerging technologies and adjust capacity to demand fluctuations. Whether subscription economics ultimately prove more or less expensive than traditional ownership depends heavily on utilisation rates, technology evolution speed, and vendor pricing discipline over contract lifecycles.

Bibliography
Purchase price represents only the initial capital outlay, while total cost of ownership encompasses maintenance, service contracts, regulatory compliance, facility modifications, staff training, financing costs, and opportunity costs of capital throughout the equipment lifecycle. Mobile gamma cameras often have higher utilisation and lower ancillary costs despite potentially comparable equipment prices, making lifecycle economics more predictive of financial impact than upfront cost alone.
Leasing converts large capital expenditures into operating expenses, preserving capital budgets for other strategic priorities while spreading costs across multiple fiscal years. Operating expense treatment often faces fewer approval hurdles than capital purchases and provides budget predictability through fixed monthly payments. However, cumulative lease payments typically exceed outright purchase costs, requiring hospitals to balance budget flexibility against long term cost efficiency.
Guaranteed response times for service calls, availability of loaner equipment during repairs, preventive maintenance frequency, parts inventory access, and vendor technical expertise specific to nuclear imaging systems prove most critical. Uptime guarantees with financial penalties for missed targets align vendor incentives with hospital operational needs, while comprehensive calibration and quality assurance services maintain regulatory compliance without internal resource demands.
Shared usage requires careful scheduling coordination to ensure equipment availability when clinically needed, particularly for urgent or unplanned procedures. Hospitals mitigate access concerns through scheduling software, clear priority protocols for emergency cases, and maintaining sufficient equipment inventory to serve peak demand across sharing facilities. Well managed shared models improve overall access by bringing nuclear imaging capability to locations that otherwise lack dedicated equipment.
Payback periods vary widely based on utilisation rates, reimbursement levels, and deployment models, but typically range from eighteen months to four years for mobile systems compared to four to seven years for fixed installations. Higher utilisation enabled by mobility and avoided facility construction costs accelerate payback substantially. Service intensive leasing models may not have distinct payback periods but demonstrate value through ongoing positive contribution margins.
Mobile Chipset Market is segmented by Clock Speed (1.5 GHz, 800 MHz, 1.6 GHz–2.5 GHz, 2.6 GHz–3.5 GHz), Frequency Type (Sub-6GHz, mmWave, Sub-6GHz + mmWave), Processing Node Type (7 Nm, 10 Nm, Other Node Types), and Region. Forecast for 2026 to 2036.
Mobile Operating Rooms Market is segmented by Product (Mobile Operating Rooms), Service (Diagnostic Service), Sales Channel (Retail, Brand Stores, E-Commerce), and Region. Forecast for 2026 to 2036.
Mobile Clinic Market The mobile clinic market is segmented by Clinic Type (Maternal Health Clinic, Neonatal and Infant Health Clinic, Child and Adolescent Health Clinic, Reproductive Health and Contraceptive Services Clinic, Mental Health Clinic, Dental Care Clinic, ENT Clinic, Geriatric Care Clinic, OPD Clinic, Diagnostic/Screening Clinic, Emergency Care Clinic), Design Layout (Single Exam Room, Double Exam Room, Triple Exam Room) and Vehicle Type (Mobile Medical Vans, Mobile Medical Bus). Forecast for 2025 to 2035.
Mobile Payment Transaction Market is segmented by Technology (SMS Mobile Payment Transactions, WAP-WEB, USSD, NFC), Purpose (Money Transfer, Merchandise Purchase, Bill Payment, Ticketing, Others), Application (Retail Payments, Transportation Payments, Hospitality Payments, Utility Payments, E Commerce Payments), and Region. Forecast for 2026 to 2036.
Gamma Knife Market is segmented by Disease Indication (Brain Metastasis, Cancer, Arteriovenous Malformation, Trigeminal Neuralgia, Others), Anatomy (Head, Neck, Other Body Parts), End User (Hospitals, Specialty Clinics, Ambulatory Surgical Centers), and Region. Forecast for 2026 to 2036.