Native Septic Arthritis Treatment Market : Global Industry Analysis 2016 - 2025 and Opportunity Assessment 2026 - 2036
Native Septic Arthritis Treatment Market Size and Share Forecast Outlook 2026 to 2036
Historical Data Covered: 2016 - 2025 | Base Year: 2025 | Estimated Year: 2026 | Forecast Period: 2026 - 2036
Native Septic Arthritis Treatment Market Forecast and Outlook 2026 to 2036
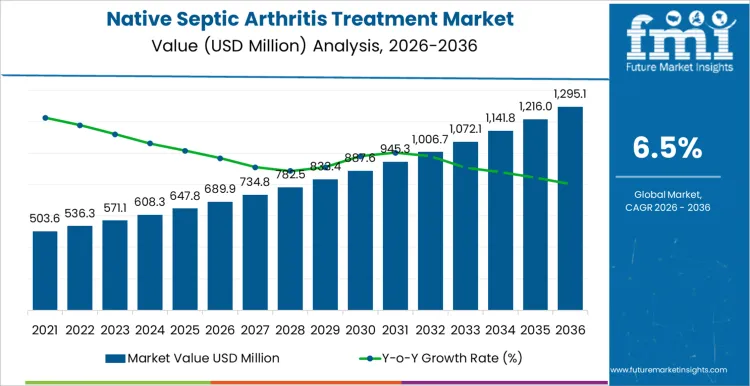
The native septic arthritis treatment market starts 2026 at USD 689.9 million and is expected to reach USD 1,295.1 million by 2036 at a 6.5% CAGR. Adoption is driven by hospital protocols, joint involvement severity, and patient comorbidities rather than brand visibility. Once a treatment regimen is incorporated into clinical pathways, substitutions require additional validation or regulatory approval. Clinicians evaluate efficacy, administration route, and safety profile. Hospitals monitor dosing schedules, stock availability, and procedure planning. Procurement teams track supplier reliability, lot traceability, and service coverage. Care team training and adherence monitoring influence treatment outcomes.
Market growth follows patient volume, protocol adoption, and expansion of hospital infection management programs rather than marketing campaigns. Manufacturers focus on formulation consistency, packaging integrity, and stability under storage conditions. Release requires potency confirmation, sterility verification, and documentation checks. Distribution networks stage stock near high-volume hospitals to maintain uninterrupted therapy access. Technical support provides dosing guidance, adverse event monitoring, and clinician training. Profitability depends on treatment adherence, predictable reorder cycles, and low waste rather than promotional discounts or frequent formulation changes.
Quick Stats for Native Septic Arthritis Treatment Market
- Native Septic Arthritis Treatment Market Value (2026): USD 689.9 million
- Native Septic Arthritis Treatment Market Forecast Value (2036): USD 1,295.1 million
- Native Septic Arthritis Treatment Market Forecast CAGR 2026 to 2036: 6.5%
- Leading Type in Native Septic Arthritis Treatment Market: IV antibiotics
- Key Growth Regions in Native Septic Arthritis Treatment Market: Asia Pacific, North America, Europe
- Top Players in Native Septic Arthritis Treatment Market: Pfizer Inc., Merck & Co., Inc., Sanofi S.A., Roche Holding AG, GlaxoSmithKline plc
What Is the Growth Forecast for the Native Septic Arthritis Treatment Market through 2036?
Clinical pathway adherence and hospital protocol design drive demand in the native septic arthritis treatment market more than overall orthopedic case volume. In 2026, at about USD 689.9 million, use is concentrated in hospitals, orthopedic surgery centers, and infectious disease units where early intervention and standard treatment regimens determine outcomes. Medication selection and surgical device use are guided by institutional protocols and remain consistent across treatment cycles, linking demand to patient admissions and severity patterns rather than short term fluctuations. Growth is supported by broader adoption of standardized antibiotic regimens, joint drainage procedures, and follow up monitoring across multiple centers. The increase reflects integration of best practice pathways rather than rapid replacement of existing therapy approaches.
Supply reliability and therapeutic consistency shape the later phase of the native septic arthritis treatment market. As value approaches roughly USD 1,295.1 million by 2036, buyers focus on availability of guideline compliant medications, device compatibility, and treatment support programs. Manufacturers invest in distribution networks, training, and monitoring support to ensure consistent patient outcomes. The rise from the mid six hundred into the low one point four billion reflects cumulative adoption across multiple hospital systems and referral networks rather than a single surge in case numbers. Suppliers that maintain reliable product performance, consistent delivery, and clinical support tend to secure preferred long term positions in hospital treatment protocols.
Native Septic Arthritis Treatment Market Key Takeaways
| Metric | Value |
|---|---|
| Market Value (2026) | USD 689.9 million |
| Forecast Value (2036) | USD 1,295.1 million |
| Forecast CAGR 2026 to 2036 | 6.5% |
How Is the Native Septic Arthritis Treatment Market Supporting Rapid Infection Control and Joint Preservation?
Native septic arthritis treatment focuses on eliminating bacterial infection in affected joints while preserving mobility and minimizing long-term damage. Historically, management relied on systemic antibiotics and open surgical drainage, which often required prolonged hospitalization and carried risk of incomplete clearance. Current approaches combine targeted intravenous or oral antibiotic regimens with arthroscopic or minimally invasive drainage techniques, supported by diagnostic imaging and laboratory monitoring. Clinicians evaluate therapies based on pathogen coverage, tissue penetration, dosing flexibility, and patient tolerance. Adoption is concentrated in orthopedic, pediatric, and rheumatology centers where early intervention affects recovery, functional outcomes, and risk of permanent joint impairment. Treatment choice also impacts length of stay, rehabilitation planning, and resource utilization.
Pharmaceutical and device suppliers differentiate products through spectrum of activity, safety profile, delivery options, and procedure compatibility rather than unit cost alone. Earlier interventions used broad empirical treatments, which limited optimization and data on outcomes. Current protocols prioritize standardized antimicrobial regimens, optimized drainage tools, and minimally invasive techniques for repeatable results. Hospitals assess total operational value through faster infection resolution, reduced readmission rates, and preservation of joint function, rather than acquisition price. Suppliers support adoption through technical guidance, training, and evidence-based protocols. Over time, demand tracks hospital admissions for septic arthritis, increasing awareness of early detection, and adoption of minimally invasive drainage approaches, creating opportunities for manufacturers of both therapeutic agents and specialized procedural devices.
What Factors Are Shaping the Demand for Native Septic Arthritis Treatment Market in 2026 by Products and Applications?
Clinical severity, rapid infection control, and adherence to pediatric and adult care protocols drive the Native Septic Arthritis Treatment Market in 2026 rather than short-term procurement trends. Hospitals and orthopedic centers select therapies based on infection site, antibiotic resistance diagnosis profile, and patient comorbidities. Segment adoption is influenced by route of administration, dosing complexity, and monitoring requirements. Suppliers that provide dosing guidance, patient adherence programs, and reliable supply chains are positioned to secure repeat orders. Market growth is concentrated in knee and hip joint infections, offering predictable volumes for manufacturers capable of combining therapeutic efficacy, clinical guidance, and service reliability to support hospital adoption.
How Does Product Selection Influence Supplier Responsibilities and Clinical Integration in the Native Septic Arthritis Treatment Market?
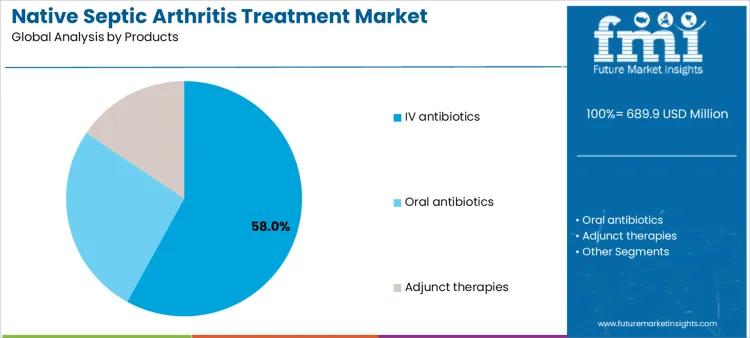
IV antibiotics account for roughly 58% of demand due to their ability to achieve rapid systemic concentrations, particularly in acute or severe joint infections. Suppliers supporting these therapies must ensure cold-chain integrity, infusion device compatibility, and staff training for safe administration. Oral antibiotics are applied for step-down therapy or mild infections, emphasizing adherence support, patient education, and consistent inventory availability. Adjunct therapies, including anti-inflammatory or supportive treatments, create additional service opportunities by requiring guidance on dosing schedules and therapy integration. Product choice determines supplier engagement in training, adherence programs, and regulatory documentation, which directly influences long-term adoption.
Administration route and therapy characteristics further shape workflow planning and supplier strategy. IV fluid drug device antibiotic use requires infusion equipment, monitoring infrastructure, and clinical staff competency, increasing supplier involvement in training and technical support. Oral antibiotics simplify administration but necessitate adherence monitoring and predictable supply chains. Adjunct therapies, while lower in volume, demand precise guidance and integration with primary treatment regimens. Hospitals standardizing on specific product types benefit from reduced procedural variability but depend on suppliers for technical guidance and consistent supply. Companies that provide comprehensive support and patient education can strengthen adoption and maximize account retention.
Why Does Application Mix Determine Volume Concentration and Supplier Strategy in the Native Septic Arthritis Treatment Market?
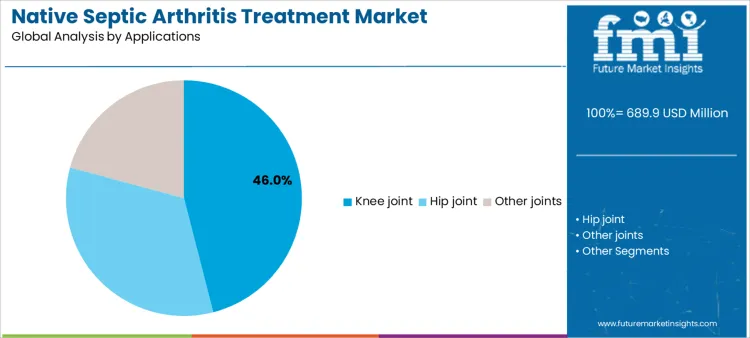
Knee joint infections represent approximately 46% of market demand because these cases occur most frequently and require rapid intervention with reliable therapies. Hip joint infections, while less frequent, involve more complex procedural management and dosing considerations, offering high-value opportunities for suppliers. Other joints, including shoulder, elbow, and ankle, generate smaller volumes but require precise therapy selection and monitoring. Application-specific needs guide inventory planning, staff training, and service provision. Suppliers aligning their offerings with high-volume knee infections and specialized hip or other joint interventions can maximize market penetration and predictable revenue streams.
Clinical application patterns further influence supplier engagement and resource allocation. Facilities treating knee infections prioritize rapid therapeutic availability, adherence monitoring, and clinical guidance to ensure positive outcomes. Hip joint infections demand targeted support, infusion infrastructure, and patient education programs, increasing supplier involvement. Smaller or less frequent joint infections require specialized guidance and consumable availability. Segment shares are determined by infection prevalence, treatment complexity, and workflow integration rather than short-term purchasing trends. Suppliers providing training, reliable supply, and clinical support can secure long-term contracts and enhance adoption across multiple joint treatment programs.
How is the Native Septic Arthritis Treatment Market Being Defined by Clinical Outcomes and Infection Control?
The Native Septic Arthritis Treatment Market is shaped by how hospitals and orthopedic centers manage rapid infection clearance and joint preservation. Therapies and interventions are evaluated based on efficacy, safety, and speed of action, with consideration for patient age and comorbidities. Selection decisions involve orthopedic surgeons, infectious disease diagnostics, and hospital procurement teams. Suppliers that provide treatments with reliable outcomes, clear dosing guidance, and supporting clinical documentation are preferred. This positions therapies as critical components of care plans rather than optional interventions, emphasizing predictable clinical results, patient safety, and procedural integration.
How Are Standardized Treatment Protocols Influencing Supplier Expectations in the Native Septic Arthritis Treatment Market?
Healthcare providers increasingly follow standardized protocols to ensure consistent diagnosis, early intervention, and reduced complications. This drives demand in the Native Septic Arthritis Treatment Market toward therapies that integrate with accepted clinical guidelines, support surgical and pharmacologic intervention, and offer predictable patient response. Buyers prefer treatments with validated efficacy, clear administration instructions, and supporting monitoring tools. Suppliers are evaluated on product consistency, regulatory compliance, and clinical support rather than on minor formulation differences. Therapies aligned with standard protocols are more likely to be adopted across multiple hospitals and care teams.
Where is Recurring Demand Being Built in the Native Septic Arthritis Treatment Market?
Recurring demand comes from hospitals, orthopedic units, and specialized infectious disease centers managing ongoing or repeat cases of native joint infections. Each treatment course or surgical intervention generates predictable orders for antibiotics, drainage devices, or adjunctive therapies. The Native Septic Arthritis Treatment Market also benefits from multi-site hospital networks standardizing on approved therapy regimens. Suppliers that provide dosing support, training, and reliable supply chains secure long-term engagement. Embedding therapies into standard care protocols ensures ongoing demand tied to patient volume and repeat interventions.
Why do Cost and Clinical Risk Considerations Limit Broader Adoption in the Native Septic Arthritis Treatment Market?
High treatment costs, potential side effects, and surgical complexity limit adoption in smaller or low-volume hospitals. The market also faces adoption constraints from regulatory approvals, protocol verification, and physician preference for familiar approaches. Clinicians are cautious about switching treatments mid-therapy due to infection progression risk. Suppliers entering the market must provide clinical support, documentation, and reliable product availability. Adoption is concentrated in high-volume orthopedic and infectious disease centers where patient outcomes and procedural safety are critical.
What is the Demand for Native Septic Arthritis Treatment by Country?
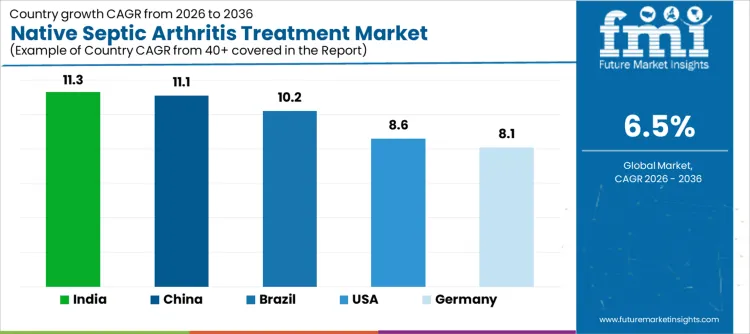
| Country | CAGR |
|---|---|
| USA | 8.6% |
| Brazil | 10.2% |
| China | 11.1% |
| India | 11.3% |
| Germany | 8.1% |
Demand for native septic arthritis treatment is rising as hospitals, orthopedic centers, and pediatric clinics expand early intervention, surgical, and antimicrobial therapy options to improve patient outcomes. India leads with an 11.3% CAGR, supported by growing hospital infrastructure, higher incidence reporting, and adoption of advanced diagnostic and treatment protocols. China follows at 11.1%, driven by large patient volumes, investment in orthopedic care, and rising awareness of early treatment benefits. Brazil records 10.2%, reflecting expansion of healthcare access and improved treatment protocols. The USA grows at 8.6%, shaped by steady procedure volumes and adoption of minimally invasive techniques. Germany, at 8.1%, reflects stable demand in a mature healthcare system with standardized clinical management.
How Are Orthopedic Surgical Programs Driving Demand in the Native Septic Arthritis Treatment Market in the United States?
United States demand for native septic arthritis treatments is advancing along an 8.6% CAGR as orthopedic surgery programs expand minimally invasive procedures and inpatient joint infection management. Procurement authority rests with orthopedic service line committees, infection control teams, and hospital capital boards. Adoption focuses on intravenous antibiotics, arthroscopic lavage devices, and targeted therapy protocols for pediatric and adult patients. Once a treatment approach is validated, it is standardized across multiple hospital networks and surgical units. Supplier selection emphasizes clinical efficacy, product availability, and integration with existing therapeutic workflows. Import systems dominate advanced antibiotic delivery devices, while domestic suppliers cover standard protocols. Capital allocation follows program expansion and procedure growth. Replacement cycles track case volume. Commercial success depends on inclusion in hospital formularies, clinical program adoption, and multi-year supply agreements.
Why Are Private Hospital Networks Driving Growth in the Native Septic Arthritis Treatment Market in Brazil?
Brazil is experiencing a 10.2% CAGR in native septic arthritis treatment due to expanding private hospital orthopedic units and specialized surgical centers. Procurement authority resides with hospital network purchasing offices, surgical committees, and infection control teams. Adoption focuses on rapid pathogen identification, targeted intravenous antibiotic regimens, and arthroscopic or open joint washout. Import devices dominate high specification interventions, while local suppliers provide standard care instruments. Once approved, deployment spreads across multiple affiliated hospitals. Training programs, protocol alignment, and quality monitoring influence adoption. Capital allocation follows hospital expansion and orthopedic program growth. Replacement cycles track procedural intensity rather than device age. Commercial success depends on inclusion in network approved formularies, reference site adoption, and long-term supply agreements rather than sales to individual departments or clinics.
What Institutional Programs Are Driving Growth in the Native Septic Arthritis Treatment Market in China?
China is experiencing an 11.1% CAGR in native septic arthritis treatments due to hospital network expansion, orthopedic capacity building, and infection management programs. Large tertiary hospitals and pediatric units control most procurement. Adoption emphasizes antibiotic selection, arthroscopic lavage devices, and post-operative infection monitoring. Domestic suppliers cover routine protocols while international brands dominate advanced delivery and monitoring systems. Procurement follows tender processes and multi-year hospital capital plans. Once validated, treatments are implemented across multiple departments and affiliated hospitals. Training programs, physician adherence to protocols, and procedural standardization influence adoption. Replacement cycles follow case volume. Capital allocation aligns with hospital expansion and program scaling. Commercial success depends on inclusion in national and provincial hospital formularies and framework agreements rather than isolated clinic or small hospital sales.
Why Are Hospital Orthopedic Program Expansions Driving Growth in the Native Septic Arthritis Treatment Market in India?
India is experiencing an 11.3% CAGR in native septic arthritis treatments as hospital orthopedic programs and surgical units expand, particularly in tertiary care centers and specialty pediatric units. Procurement authority resides with orthopedic committees and hospital pharmacy boards. Device and therapy selection emphasizes targeted antibiotic protocols, arthroscopic lavage devices, and adherence to clinical infection control guidelines. Import systems dominate high acuity cases, while domestic suppliers cover routine care needs. Once approved, treatments are deployed across multiple affiliated hospitals. Training, protocol adherence, and monitoring programs influence adoption. Replacement cycles follow procedural load and patient throughput. Budget allocation aligns with hospital expansions and new service line openings. Commercial success depends on inclusion in hospital formularies, network framework agreements, and reference program adoption rather than individual clinic purchases.
How Are Guidelines and Reimbursement Structures Shaping the Native Septic Arthritis Treatment Market in Germany?
Germany is experiencing an 8.1% CAGR in native septic arthritis treatments due to structured clinical guidelines, reimbursement frameworks, and standardized hospital protocols. University hospitals and regional orthopedic centers control most procurement. Adoption focuses on targeted antibiotic regimens, surgical washout procedures, and post-operative monitoring. Evaluation emphasizes safety, efficacy, and workflow integration with orthopedic units. Procurement follows health technology assessment and hospital capital approval processes. Import products dominate advanced therapy delivery, while domestic suppliers cover routine protocols. Once approved, deployment spreads across multiple departments and hospitals. Training, documentation, and protocol adherence influence utilization. Replacement cycles follow procedural intensity. Budget allocation aligns with orthopedic program expansion. Commercial success depends on inclusion in hospital frameworks, guideline adherence, and reference site adoption rather than isolated departmental or clinic sales.
How Do Pharmaceutical Companies Compete for Clinical Adoption in the Native Septic Arthritis Treatment Market?
Native septic arthritis treatment selection occurs within hospital formularies, infectious disease protocols, and orthopedic care pathways rather than routine catalog comparison. Clinicians define pathogen spectrum coverage, dosing regimen, renal adjustment, and route of administration before approving therapies. Pfizer, Merck, Sanofi, Roche, GlaxoSmithKline compete at guideline development and tender evaluation stages. Once a therapy enters standard protocols, nursing workflows, pharmacy stocking, and monitoring schedules anchor the choice. Pfizer leverages broad-spectrum intravenous formulations and clinical experience in musculoskeletal infections. Merck positions therapies with robust safety data and dosing flexibility. Sanofi focuses on hospital adoption through guideline inclusion and formulary support. Roche provides targeted biologic adjunct therapies where needed. GlaxoSmithKline emphasizes antimicrobial stewardship alignment and multi-site protocol support.
Competitive positioning reflects efficacy, safety profile, dosing convenience, and institutional support rather than pricing alone. Clinicians assess clearance rates, joint penetration, bactericidal activity, and adverse event profile during selection. Pharmacy teams review stability, storage requirements, and batch traceability. Hospitals favor suppliers able to support multi-site standardization and clinical education programs. Pfizer secures positions where intravenous broad coverage is standard. Merck gains share through flexibility in renal dosing and tolerability. Sanofi competes in institutions that value guideline integration and formulary assistance. Roche participates in cases requiring adjunctive biologic support. GlaxoSmithKline holds positions through stewardship program alignment. Market share varies by hospital size, orthopedic caseload, pathogen prevalence, and institutional treatment protocols.
Key Players in the Native Septic Arthritis Treatment Market
- Pfizer Inc.
- Merck & Co., Inc.
- Sanofi S.A.
- Roche Holding AG
- GlaxoSmithKline plc
Scope of the Report
| Items | Values |
|---|---|
| Quantitative Units (2026) | USD million |
| Product Type | IV antibiotics; Oral antibiotics; Adjunct therapies |
| Application | Knee joint; Hip joint; Other joints |
| End User / Sales Channel | Hospitals; Clinics; Home care |
| Region | Asia Pacific; Europe; North America; Latin America; Middle East & Africa |
| Countries Covered | United States, Canada, Mexico, Germany, United Kingdom, France, Italy, Spain, Nordic, BENELUX, China, Japan, South Korea, India, Australia & New Zealand, ASEAN, Brazil, Chile, Saudi Arabia, Turkey, South Africa, Rest of regions |
| Key Companies Profiled | Pfizer Inc.; Merck & Co., Inc.; Sanofi S.A.; Roche Holding AG; GlaxoSmithKline plc |
| Additional Attributes | Dollar by sales by product and application, IV versus oral therapy mix, knee versus hip case split, average treatment duration, hospital protocol driven usage, inventory and cold chain needs, dosing and monitoring workload, repeat admission impact, regulatory and antimicrobial stewardship compliance |
Native Septic Arthritis Treatment Market Segmentation
Products:
- IV antibiotics
- Oral antibiotics
- Adjunct therapies
Applications:
- Knee joint
- Hip joint
- Other joints
End User / Sales Channel:
- Hospitals
- Clinics
- Home care
Region
- Asia Pacific
- China
- Japan
- South Korea
- India
- Australia & New Zealand
- ASEAN
- Rest of Asia Pacific
- Europe
- Germany
- United Kingdom
- France
- Italy
- Spain
- Nordic
- BENELUX
- Rest of Europe
- North America
- United States
- Canada
- Mexico
- Latin America
- Brazil
- Chile
- Rest of Latin America
- Middle East & Africa
- Kingdom of Saudi Arabia
- Other GCC Countries
- Turkey
- South Africa
- Other African Union
- Rest of Middle East & Africa
Bibliography
- American Academy of Pediatrics Committee on Infectious Diseases. (2025). Updated guidance on osteoarticular infections in children: Diagnosis, antimicrobial therapy, and follow‑up. Pediatrics, 155(1), e20241234.
- 4. Kowalski, T., & Brown, P. (2024). Optimizing diagnostic pathways for acute septic arthritis in emergency and orthopedic care. Journal of Bone and Joint Infection, 9(1), 12–21.
- 5. Williams, R. J., & Patel, S. (2024). Antibiotic stewardship and treatment algorithms for adult septic arthritis: A systematic review. Journal of Antimicrobial Chemotherapy, 79(7), 1804–1815.
Frequently Asked Questions
How big is the native septic arthritis treatment market in 2026?
The global native septic arthritis treatment market is estimated to be valued at USD 689.9 million in 2026.
What will be the size of native septic arthritis treatment market in 2036?
The market size for the native septic arthritis treatment market is projected to reach USD 1,295.1 million by 2036.
How much will be the native septic arthritis treatment market growth between 2026 and 2036?
The native septic arthritis treatment market is expected to grow at a 6.5% CAGR between 2026 and 2036.
What are the key product types in the native septic arthritis treatment market?
The key product types in native septic arthritis treatment market are iv antibiotics, oral antibiotics and adjunct therapies.
Which applications segment to contribute significant share in the native septic arthritis treatment market in 2026?
In terms of applications, knee joint segment to command 46.0% share in the native septic arthritis treatment market in 2026.
Table of Content
- Executive Summary
- Global Market Outlook
- Demand to side Trends
- Supply to side Trends
- Technology Roadmap Analysis
- Analysis and Recommendations
- Market Overview
- Market Coverage / Taxonomy
- Market Definition / Scope / Limitations
- Market Background
- Market Dynamics
- Drivers
- Restraints
- Opportunity
- Trends
- Scenario Forecast
- Demand in Optimistic Scenario
- Demand in Likely Scenario
- Demand in Conservative Scenario
- Opportunity Map Analysis
- Product Life Cycle Analysis
- Supply Chain Analysis
- Investment Feasibility Matrix
- Value Chain Analysis
- PESTLE and Porter’s Analysis
- Regulatory Landscape
- Regional Parent Market Outlook
- Production and Consumption Statistics
- Import and Export Statistics
- Market Dynamics
- Global Market Analysis 2021 to 2025 and Forecast, 2026 to 2036
- Historical Market Size Value (USD Million) Analysis, 2021 to 2025
- Current and Future Market Size Value (USD Million) Projections, 2026 to 2036
- Y to o to Y Growth Trend Analysis
- Absolute $ Opportunity Analysis
- Global Market Pricing Analysis 2021 to 2025 and Forecast 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Products
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Products , 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Products , 2026 to 2036
- IV antibiotics
- Oral antibiotics
- Adjunct therapies
- IV antibiotics
- Y to o to Y Growth Trend Analysis By Products , 2021 to 2025
- Absolute $ Opportunity Analysis By Products , 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Applications
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Applications, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Applications, 2026 to 2036
- Knee joint
- Hip joint
- Other joints
- Knee joint
- Y to o to Y Growth Trend Analysis By Applications, 2021 to 2025
- Absolute $ Opportunity Analysis By Applications, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By End User
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By End User, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By End User, 2026 to 2036
- Hospitals
- Clinics
- Home care
- Hospitals
- Y to o to Y Growth Trend Analysis By End User, 2021 to 2025
- Absolute $ Opportunity Analysis By End User, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Region
- Introduction
- Historical Market Size Value (USD Million) Analysis By Region, 2021 to 2025
- Current Market Size Value (USD Million) Analysis and Forecast By Region, 2026 to 2036
- North America
- Latin America
- Western Europe
- Eastern Europe
- East Asia
- South Asia and Pacific
- Middle East & Africa
- Market Attractiveness Analysis By Region
- North America Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- USA
- Canada
- Mexico
- By Products
- By Applications
- By End User
- By Country
- Market Attractiveness Analysis
- By Country
- By Products
- By Applications
- By End User
- Key Takeaways
- Latin America Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Brazil
- Chile
- Rest of Latin America
- By Products
- By Applications
- By End User
- By Country
- Market Attractiveness Analysis
- By Country
- By Products
- By Applications
- By End User
- Key Takeaways
- Western Europe Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Germany
- UK
- Italy
- Spain
- France
- Nordic
- BENELUX
- Rest of Western Europe
- By Products
- By Applications
- By End User
- By Country
- Market Attractiveness Analysis
- By Country
- By Products
- By Applications
- By End User
- Key Takeaways
- Eastern Europe Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Russia
- Poland
- Hungary
- Balkan & Baltic
- Rest of Eastern Europe
- By Products
- By Applications
- By End User
- By Country
- Market Attractiveness Analysis
- By Country
- By Products
- By Applications
- By End User
- Key Takeaways
- East Asia Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- China
- Japan
- South Korea
- By Products
- By Applications
- By End User
- By Country
- Market Attractiveness Analysis
- By Country
- By Products
- By Applications
- By End User
- Key Takeaways
- South Asia and Pacific Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- India
- ASEAN
- Australia & New Zealand
- Rest of South Asia and Pacific
- By Products
- By Applications
- By End User
- By Country
- Market Attractiveness Analysis
- By Country
- By Products
- By Applications
- By End User
- Key Takeaways
- Middle East & Africa Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Kingdom of Saudi Arabia
- Other GCC Countries
- Turkiye
- South Africa
- Other African Union
- Rest of Middle East & Africa
- By Products
- By Applications
- By End User
- By Country
- Market Attractiveness Analysis
- By Country
- By Products
- By Applications
- By End User
- Key Takeaways
- Key Countries Market Analysis
- USA
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Canada
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Mexico
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Brazil
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Chile
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Germany
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- UK
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Italy
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Spain
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- France
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- India
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- ASEAN
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Australia & New Zealand
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- China
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Japan
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- South Korea
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Russia
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Poland
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Hungary
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Kingdom of Saudi Arabia
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- Turkiye
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- South Africa
- Pricing Analysis
- Market Share Analysis, 2025
- By Products
- By Applications
- By End User
- USA
- Market Structure Analysis
- Competition Dashboard
- Competition Benchmarking
- Market Share Analysis of Top Players
- By Regional
- By Products
- By Applications
- By End User
- Competition Analysis
- Competition Deep Dive
- Pfizer
- Overview
- Product Portfolio
- Profitability by Market Segments (Product/Age /Sales Channel/Region)
- Sales Footprint
- Strategy Overview
- Marketing Strategy
- Product Strategy
- Channel Strategy
- Merck
- Sanofi
- Roche
- GSK
- Others
- Pfizer
- Competition Deep Dive
- Assumptions & Acronyms Used
- Research Methodology
List of Tables
- Table 1: Global Market Value (USD Million) Forecast by Region, 2021 to 2036
- Table 2: Global Market Value (USD Million) Forecast by Products , 2021 to 2036
- Table 3: Global Market Value (USD Million) Forecast by Applications, 2021 to 2036
- Table 4: Global Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 5: North America Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 6: North America Market Value (USD Million) Forecast by Products , 2021 to 2036
- Table 7: North America Market Value (USD Million) Forecast by Applications, 2021 to 2036
- Table 8: North America Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 9: Latin America Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 10: Latin America Market Value (USD Million) Forecast by Products , 2021 to 2036
- Table 11: Latin America Market Value (USD Million) Forecast by Applications, 2021 to 2036
- Table 12: Latin America Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 13: Western Europe Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 14: Western Europe Market Value (USD Million) Forecast by Products , 2021 to 2036
- Table 15: Western Europe Market Value (USD Million) Forecast by Applications, 2021 to 2036
- Table 16: Western Europe Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 17: Eastern Europe Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 18: Eastern Europe Market Value (USD Million) Forecast by Products , 2021 to 2036
- Table 19: Eastern Europe Market Value (USD Million) Forecast by Applications, 2021 to 2036
- Table 20: Eastern Europe Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 21: East Asia Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 22: East Asia Market Value (USD Million) Forecast by Products , 2021 to 2036
- Table 23: East Asia Market Value (USD Million) Forecast by Applications, 2021 to 2036
- Table 24: East Asia Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 25: South Asia and Pacific Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 26: South Asia and Pacific Market Value (USD Million) Forecast by Products , 2021 to 2036
- Table 27: South Asia and Pacific Market Value (USD Million) Forecast by Applications, 2021 to 2036
- Table 28: South Asia and Pacific Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 29: Middle East & Africa Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 30: Middle East & Africa Market Value (USD Million) Forecast by Products , 2021 to 2036
- Table 31: Middle East & Africa Market Value (USD Million) Forecast by Applications, 2021 to 2036
- Table 32: Middle East & Africa Market Value (USD Million) Forecast by End User, 2021 to 2036
List of Figures
- Figure 1: Global Market Pricing Analysis
- Figure 2: Global Market Value (USD Million) Forecast 2021 to 2036
- Figure 3: Global Market Value Share and BPS Analysis by Products , 2026 and 2036
- Figure 4: Global Market Y-o-Y Growth Comparison by Products , 2026 to 2036
- Figure 5: Global Market Attractiveness Analysis by Products
- Figure 6: Global Market Value Share and BPS Analysis by Applications, 2026 and 2036
- Figure 7: Global Market Y-o-Y Growth Comparison by Applications, 2026 to 2036
- Figure 8: Global Market Attractiveness Analysis by Applications
- Figure 9: Global Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 10: Global Market Y-o-Y Growth Comparison by End User, 2026 to 2036
- Figure 11: Global Market Attractiveness Analysis by End User
- Figure 12: Global Market Value (USD Million) Share and BPS Analysis by Region, 2026 and 2036
- Figure 13: Global Market Y-o-Y Growth Comparison by Region, 2026 to 2036
- Figure 14: Global Market Attractiveness Analysis by Region
- Figure 15: North America Market Incremental Dollar Opportunity, 2026 to 2036
- Figure 16: Latin America Market Incremental Dollar Opportunity, 2026 to 2036
- Figure 17: Western Europe Market Incremental Dollar Opportunity, 2026 to 2036
- Figure 18: Eastern Europe Market Incremental Dollar Opportunity, 2026 to 2036
- Figure 19: East Asia Market Incremental Dollar Opportunity, 2026 to 2036
- Figure 20: South Asia and Pacific Market Incremental Dollar Opportunity, 2026 to 2036
- Figure 21: Middle East & Africa Market Incremental Dollar Opportunity, 2026 to 2036
- Figure 22: North America Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 23: North America Market Value Share and BPS Analysis by Products , 2026 and 2036
- Figure 24: North America Market Y-o-Y Growth Comparison by Products , 2026 to 2036
- Figure 25: North America Market Attractiveness Analysis by Products
- Figure 26: North America Market Value Share and BPS Analysis by Applications, 2026 and 2036
- Figure 27: North America Market Y-o-Y Growth Comparison by Applications, 2026 to 2036
- Figure 28: North America Market Attractiveness Analysis by Applications
- Figure 29: North America Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 30: North America Market Y-o-Y Growth Comparison by End User, 2026 to 2036
- Figure 31: North America Market Attractiveness Analysis by End User
- Figure 32: Latin America Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 33: Latin America Market Value Share and BPS Analysis by Products , 2026 and 2036
- Figure 34: Latin America Market Y-o-Y Growth Comparison by Products , 2026 to 2036
- Figure 35: Latin America Market Attractiveness Analysis by Products
- Figure 36: Latin America Market Value Share and BPS Analysis by Applications, 2026 and 2036
- Figure 37: Latin America Market Y-o-Y Growth Comparison by Applications, 2026 to 2036
- Figure 38: Latin America Market Attractiveness Analysis by Applications
- Figure 39: Latin America Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 40: Latin America Market Y-o-Y Growth Comparison by End User, 2026 to 2036
- Figure 41: Latin America Market Attractiveness Analysis by End User
- Figure 42: Western Europe Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 43: Western Europe Market Value Share and BPS Analysis by Products , 2026 and 2036
- Figure 44: Western Europe Market Y-o-Y Growth Comparison by Products , 2026 to 2036
- Figure 45: Western Europe Market Attractiveness Analysis by Products
- Figure 46: Western Europe Market Value Share and BPS Analysis by Applications, 2026 and 2036
- Figure 47: Western Europe Market Y-o-Y Growth Comparison by Applications, 2026 to 2036
- Figure 48: Western Europe Market Attractiveness Analysis by Applications
- Figure 49: Western Europe Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 50: Western Europe Market Y-o-Y Growth Comparison by End User, 2026 to 2036
- Figure 51: Western Europe Market Attractiveness Analysis by End User
- Figure 52: Eastern Europe Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 53: Eastern Europe Market Value Share and BPS Analysis by Products , 2026 and 2036
- Figure 54: Eastern Europe Market Y-o-Y Growth Comparison by Products , 2026 to 2036
- Figure 55: Eastern Europe Market Attractiveness Analysis by Products
- Figure 56: Eastern Europe Market Value Share and BPS Analysis by Applications, 2026 and 2036
- Figure 57: Eastern Europe Market Y-o-Y Growth Comparison by Applications, 2026 to 2036
- Figure 58: Eastern Europe Market Attractiveness Analysis by Applications
- Figure 59: Eastern Europe Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 60: Eastern Europe Market Y-o-Y Growth Comparison by End User, 2026 to 2036
- Figure 61: Eastern Europe Market Attractiveness Analysis by End User
- Figure 62: East Asia Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 63: East Asia Market Value Share and BPS Analysis by Products , 2026 and 2036
- Figure 64: East Asia Market Y-o-Y Growth Comparison by Products , 2026 to 2036
- Figure 65: East Asia Market Attractiveness Analysis by Products
- Figure 66: East Asia Market Value Share and BPS Analysis by Applications, 2026 and 2036
- Figure 67: East Asia Market Y-o-Y Growth Comparison by Applications, 2026 to 2036
- Figure 68: East Asia Market Attractiveness Analysis by Applications
- Figure 69: East Asia Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 70: East Asia Market Y-o-Y Growth Comparison by End User, 2026 to 2036
- Figure 71: East Asia Market Attractiveness Analysis by End User
- Figure 72: South Asia and Pacific Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 73: South Asia and Pacific Market Value Share and BPS Analysis by Products , 2026 and 2036
- Figure 74: South Asia and Pacific Market Y-o-Y Growth Comparison by Products , 2026 to 2036
- Figure 75: South Asia and Pacific Market Attractiveness Analysis by Products
- Figure 76: South Asia and Pacific Market Value Share and BPS Analysis by Applications, 2026 and 2036
- Figure 77: South Asia and Pacific Market Y-o-Y Growth Comparison by Applications, 2026 to 2036
- Figure 78: South Asia and Pacific Market Attractiveness Analysis by Applications
- Figure 79: South Asia and Pacific Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 80: South Asia and Pacific Market Y-o-Y Growth Comparison by End User, 2026 to 2036
- Figure 81: South Asia and Pacific Market Attractiveness Analysis by End User
- Figure 82: Middle East & Africa Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 83: Middle East & Africa Market Value Share and BPS Analysis by Products , 2026 and 2036
- Figure 84: Middle East & Africa Market Y-o-Y Growth Comparison by Products , 2026 to 2036
- Figure 85: Middle East & Africa Market Attractiveness Analysis by Products
- Figure 86: Middle East & Africa Market Value Share and BPS Analysis by Applications, 2026 and 2036
- Figure 87: Middle East & Africa Market Y-o-Y Growth Comparison by Applications, 2026 to 2036
- Figure 88: Middle East & Africa Market Attractiveness Analysis by Applications
- Figure 89: Middle East & Africa Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 90: Middle East & Africa Market Y-o-Y Growth Comparison by End User, 2026 to 2036
- Figure 91: Middle East & Africa Market Attractiveness Analysis by End User
- Figure 92: Global Market - Tier Structure Analysis
- Figure 93: Global Market - Company Share Analysis

