Home Care Services Market : Global Industry Analysis 2016 - 2025 and Opportunity Assessment 2026 - 2036
Home Care Services Market is segmented by Service Type (Health Care Services, Non-Health Care Services), End User (Children, Adults, Geriatric Users), Payer Type (Government Programs, Insurance Plans, Self-Pay Users), Duration (Long-Term Care, Short-Term Care), Delivery Type (Skilled Nursing, Rehabilitation Support, Personal Assistance, Companionship Care, Medication Management, Hospice Care, Telehealth Support, Remote Monitoring), Technology Use (Remote Monitoring, Telehealth Support, Digital Care Coordination), and Region. Forecast for 2026 to 2036.
Historical Data Covered: 2016 - 2025 | Base Year: 2025 | Estimated Year: 2026 | Forecast Period: 2026 - 2036
Home Care Services Market Size, Market Forecast and Outlook By FMI
Summary of the Home Care Services Market
- Demand and Growth Drivers
- Aging populations are anticipated to support home care services as families seek clinical care outside hospital use.
- Chronic illness management supports demand for skilled nursing and routine monitoring across long term care needs.
- Digital care coordination is expected to support provider adoption as telehealth and remote monitoring improve daily follow-up.
- Product and Segment View
- Health care services are estimated to lead service type demand, supported by skilled nursing and chronic care delivery.
- Geriatric users lead end-user demand because routine monitoring and aging-in-place preferences keep this segment important.
- Non-health care services are poised to support daily independence through personal assistance and household support.
- Geography and Competitive Outlook
- India is projected to grow as an important country market, supported by organized caregiving demand and urban family care needs.
- United States demand maintain scale because in-home nursing reimbursement and payer coverage support this market.
- Providers combining trained caregiver networks and digital coordination tools are anticipated to handle larger care volumes.
- Analyst Opinion
- Sabyasachi Ghosh, Principal Consultant at FMI says, “Providers who can combine trained caregiver networks with reliable clinical coordination are likely to strengthen their position in the Home Care Services Market through 2036.”
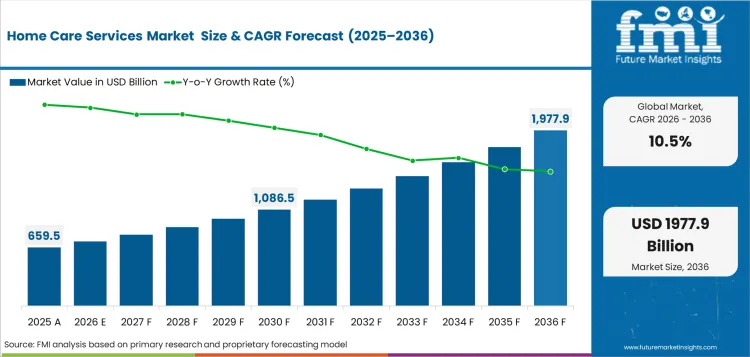
- Home Care Services Market Value Analysis
- Home care services are moving from basic support into a larger clinical care delivery model.
- Clinical home care demand is supported by skilled nursing and chronic care follow-up after hospital discharge.
- Families value familiar care settings as older adults need mobility help and routine monitoring support.
- Provider scale is linked with caregiver availability and digital coordination across patient record systems.
Home Care Services Market Definition
The home care services market covers clinical and non-clinical support delivered through home care services inside private residences for people across age groups. Services cover skilled nursing and rehabilitation support as well as chronic care management and telehealth-assisted monitoring. Daily support services include personal assistance and companionship for patients or older adults needing regular help at home.
Home Care Services Market Inclusions
Market scope encompasses commercially delivered home care services categorized by service type and end user across regional markets. Service type coverage includes health care services and non-health care services delivered through organized care providers. Care delivery coverage includes skilled nursing and post-acute care with remote patient monitoring devices supporting tracked follow-up. The range of revenue sizes is from 2026 to 2036.
Home Care Services Market Exclusions
The scope does not include hospital inpatient care or institutional nursing home services delivered outside private residential settings. Nursing home services and standalone long-term care software are excluded unless bundled with provider-led home care delivery. Unpaid family caregiving is excluded since it does not represent commercially billed home care service revenue.
Home Care Services Market Research Methodology
- Primary Research: FMI analysts reviewed home care providers, healthcare payers, and care delivery specialists across important markets.
- Desk Research: Market sizing used healthcare delivery patterns and reimbursement structures across major home care economies.
- Market Sizing and Forecasting: 2025 value was calculated from 2026 revenue and the stated 10.5% CAGR.
- Data Validation: Segment shares were checked against service type demand and end-user adoption patterns across key countries.
Why is the Home Care Services Market Growing?
- Aging households are increasing demand for home-based support as older adults need routine care after hospital discharge.
- Hospitals and payers are using home care to ease facility pressure and support recovery inside familiar residential environments.
- Digital monitoring and telehealth tools help providers review patient concerns on time and keep care records manageable.
Home care services demand is expanding as aging populations need support outside hospital. Hospitals and payers use home care to reduce facility pressure and support recovery after discharge. Families prefer familiar home environments for long-term support and daily assistance.
Health care services gain priority as chronic disease management needs trained clinical staff at home. Skilled nursing and rehabilitative therapy support patients needing repeated follow-up. Remote patient monitoring devices improve escalation decisions and support safer care between visits.
Digital coordination improves service reliability across caregivers and clinical staff. Telehealth consultations and virtual triage allow timely review of patient concerns. Clear records help providers meet payer documentation needs across home care programs.
Market Segmentation Analysis
- Health care services are estimated to account for 58.7% share in 2026, supported by clinical supervision at home.
- Geriatric users are expected to account for roughly 42% share in 2026, supported by aging-in-place demand.
- Service coverage is divided by service type and end user categories across major regions. Care delivery areas further segment service coverage within large regional healthcare systems.
Home care services market is divided into groups based on service type and end user across residential care settings. Service type includes health care services and non-health care services for clinical support and daily assistance. End user segmentation covers children and adults, along with geriatric users needing home-based care support. Care delivery area includes skilled nursing and post-acute care across home-based recovery needs. Technology use includes remote monitoring and telehealth support for better care coordination across provider networks. By region, the market covers North America, Latin America, Europe, East Asia, South Asia, Oceania, and Middle East and Africa.
Insights into the Service Type Segment
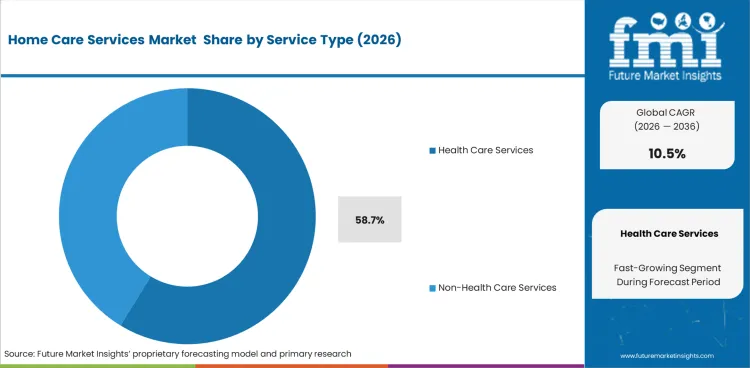
- Health care services are estimated to account for 58.7% share in 2026, supported by skilled nursing and supervised home care.
- The service mix includes health care services and non health care services across clinical care and daily assistance.
Insights into the End User Segment
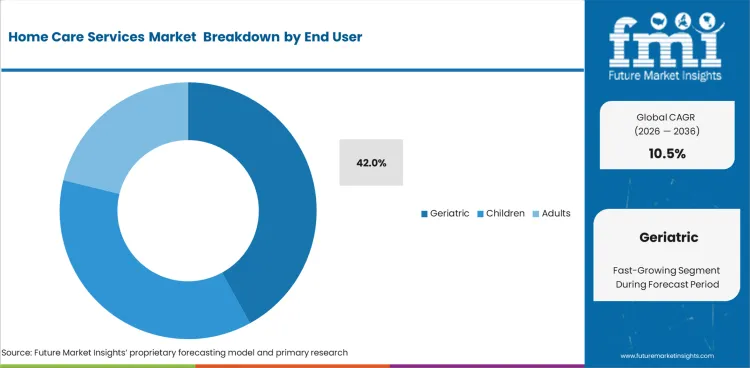
- Geriatric users are expected to hold roughly 42% share in 2026, due to aging-in-place care demand.
- Demand also comes from children and adults, along with geriatric users needing structured support at home.
Insights into the Payer Segment
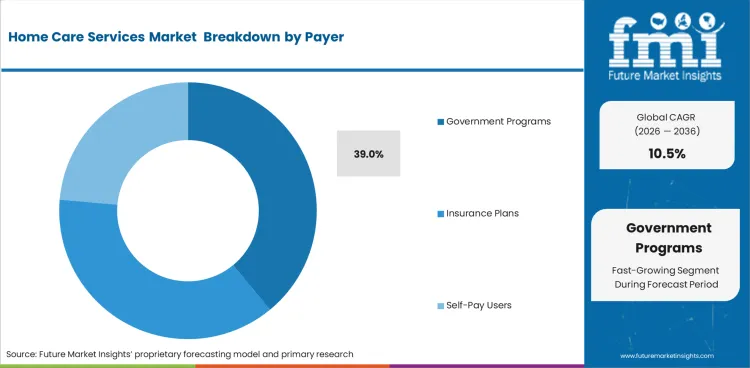
- Government programs are estimated to contribute 39% share in 2026, reflecting funded home nursing and care coverage.
- The payer mix includes government programs and insurance plans, along with self pay users across home care services.
Insights into the Duration Segment
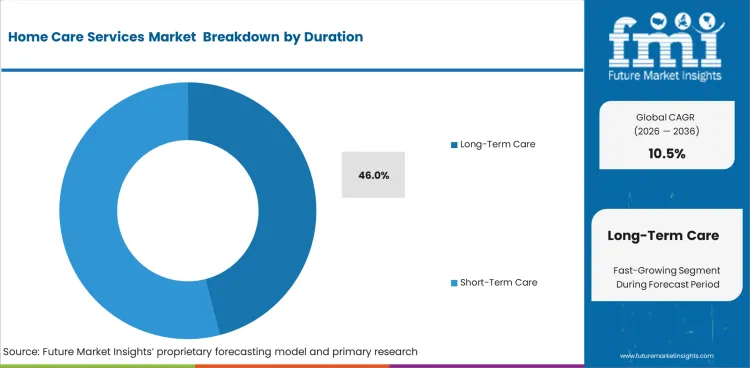
- Long-term care is projected to hold 46% share in 2026, supported by chronic care and older adult support needs.
- Care duration includes long term care and short term care across recovery support and routine home assistance.
Insights into the Delivery Segment
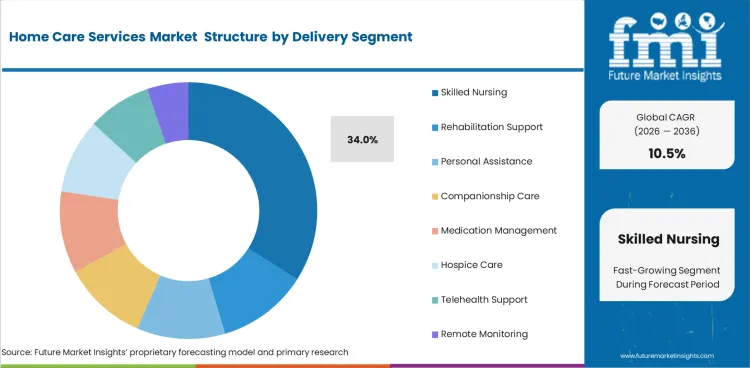
- Skilled nursing is estimated to account for 34% share in 2026, because of medication management and clinical follow-up.
- Service delivery includes skilled nursing and rehabilitation support, along with personal assistance for residential care delivery.
Home Care Services Market Drivers, Restraints, and Opportunities
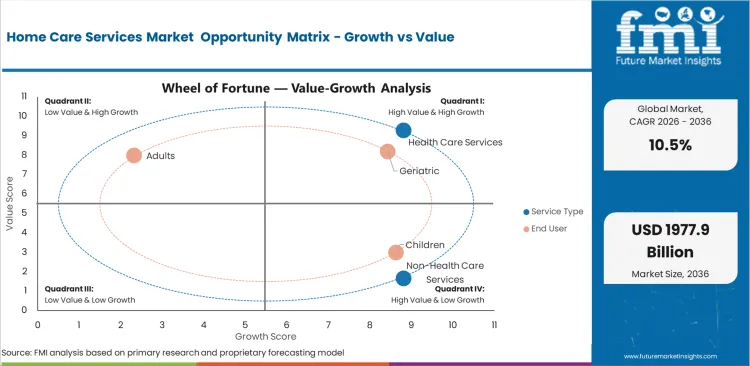
- Aging populations and chronic illness needs create sustained demand for home-based clinical services.
- Caregiver shortages and training needs limit service expansion across several country markets.
- Digital tools support documentation and timely care review across home environments.
Home care services demand is supported by care transitions from hospitals into homes. Remote monitoring and telehealth improve continuity for patients needing repeated follow-up. Workforce pressure is a major limit for providers scaling clinical and daily assistance services.
Aging Population and Chronic Care Need
Older adults create durable demand for home-based support across major healthcare systems. Chronic illness adds repeated care needs through medication management and routine monitoring. Clinical service demand is high among patients needing post-acute recovery and palliative care. Skilled nursing helps providers manage care plans outside hospital. Geriatric care services support demand among older adults needing structured care at home.
Digital Coordination and Remote Monitoring
Digital coordination improves home care workflows through scheduling and patient record systems. Remote monitoring tools help providers review risk between visits and respond on time to patient changes. Telehealth consultations add clinical access for patients needing frequent review.
Providers using digital tools can support continuity across distributed care staff. Home healthcare software improves documentation and payer review across care networks. Connected RHM (remote healthcare monitoring) supports confidence among families and insurers.
Analysis of Home Care Services Market by Key Countries
.webp)
| Country | CAGR |
|---|---|
| United States | 6.5% |
| China | 7.2% |
| Germany | 7.4% |
| India | 7.8% |
| United Kingdom | 7.0% |
| Japan | 6.9% |
| Brazil | 6.8% |
| Canada | 6.8% |
| France | 7.2% |
| Australia | 6.6% |
Source: Future Market Insights, 2026.
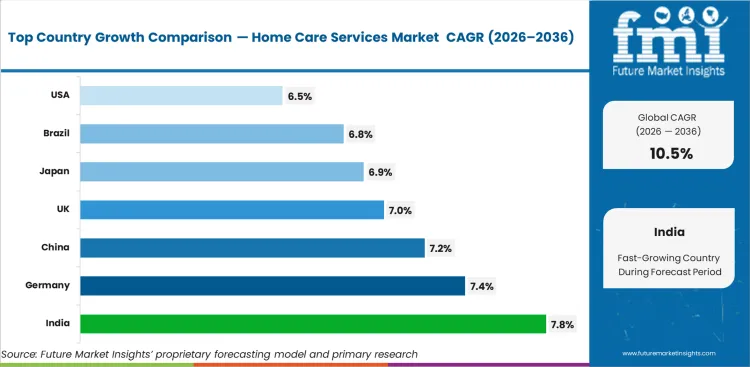
Home Care Services Market CAGR Analysis by Country
- India leads the listed country set with 7.8% CAGR through 2036, because of organized caregiving demand.
- Germany follows with 7.4% CAGR through 2036 as long-term care insurance supports in-home assistance.
- China and France each record 7.2% CAGR through 2036 as home-based care systems expand.
- United States records 6.5% CAGR through 2036 across a mature but large service base.
Global home care services demand is projected to expand at 10.5% CAGR from 2026 to 2036. Country-level CAGRs lie below the global rate in several mature markets since baseline service penetration is already higher.
Demand Outlook for Home Care Services Market in the United States
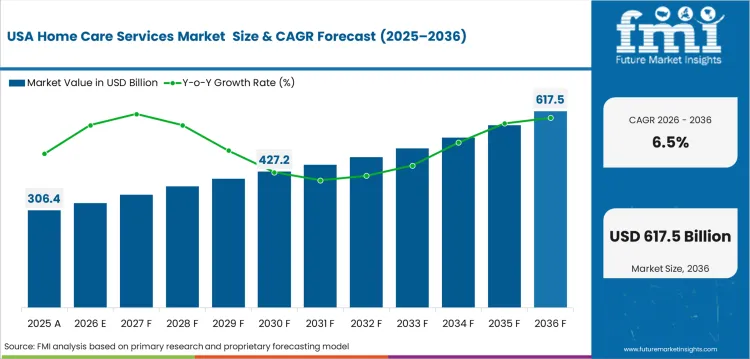
The United States home care services industry value is projected to expand at a CAGR of 6.5% from 2026 to 2036. Medicare Advantage plans and Medicaid waivers support in-home nursing reimbursement. Remote monitoring and telehealth help agencies coordinate care for patients needing regular follow-up.
- In-home nursing reimbursement supports health care services across eligible patient groups.
- Workforce shortages limit faster expansion across agencies serving large patient bases.
- Digital coordination helps providers manage documentation and payer review across home care programs.
Future Outlook for Home Care Services Market in China
Home care services sector in China is estimated to advance at a CAGR of 7.2% through 2036. Population aging and long-term care insurance pilots support organized home care assistance. Urban income levels support paid care services for older adults.
- Long-term care pilots support formal home care adoption across major urban areas.
- Rural access gaps create service quality variation across smaller care markets.
- Mobile scheduling and teleconsultations help organized providers improve service coverage.
Opportunity Analysis of Home Care Services Market in Germany
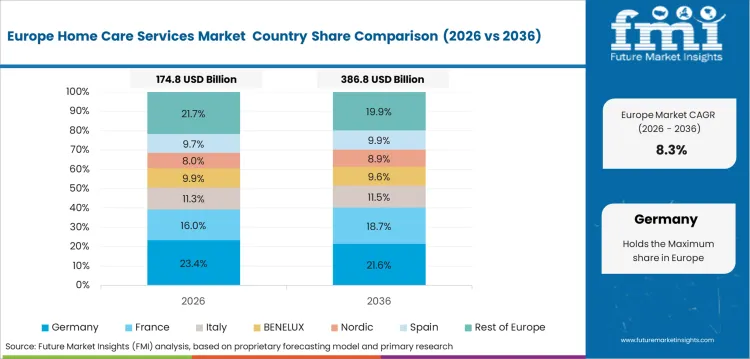
Germany home care services segment is poised to grow at a CAGR of 7.4% during the assessment period. Long-term care insurance supports in-home assistance and nursing services. Dementia care programs support trained home care demand.
- Long-term care insurance supports steady demand for home-based nursing services.
- Digital documentation helps agencies manage payer records and care reviews.
- Staffing pressure continues to limit faster scale across home care agencies.
In-depth Analysis of Home Care Services Market in India
Home care services industry in India is estimated to advance at a CAGR of 7.8% by 2036. Longer lifespans and lifestyle diseases support demand for organized caregiving. Urban migration raises paid care needs among families separated by distance.
- Organized caregiving demand is rising across urban families needing trusted support.
- Physiotherapy and chronic care services support paid home care adoption.
- Uneven regulation creates a trust gap between organized providers and informal care.
Sales Analysis of Home Care Services Market in the United Kingdom
The United Kingdom home care services sector is poised to expand at a CAGR of 7.0% during the assessment period. Community care policy and domiciliary support programs support home care service demand. Rehabilitation and palliative services support broader home care use.
- Domiciliary support programs help move eligible care into residential settings.
- Integrated care systems improve coordination between hospitals and community providers.
- Workforce shortages affect care schedules across agencies serving older adults.
In-depth Analysis of Home Care Services Market in Japan
Japan home care services sector is predicted to advance at a CAGR of 6.9% from 2026 to 2036. Municipal networks and home reimbursement support daily assistance and physician visits. Tele rehabilitation and assistive robotics may reduce pressure in specific care tasks.
- Municipal care networks support daily assistance for older adults living at home.
- Home reimbursement supports physician visits and prevention programs across older households.
- Workforce limits create demand for digital support and assistive care tools.
Demand Outlook for Home Care Services Market in Brazil
Brazil home care services industry is estimated to expand at a CAGR of 6.8% over the forecast years. Urban families seek alternatives to crowded hospitals and long facility stays. Private provider packages support chronic disease monitoring and home care assistance.
- Private care packages support home monitoring among urban patient groups.
- Hospital partnerships improve referral flow for home-based recovery services.
- Nurse shortages constrain faster expansion across large metropolitan service markets.
Competitive Landscape and Strategic Positioning
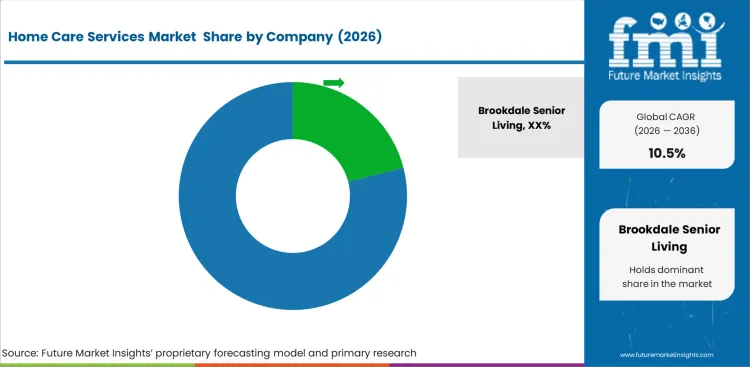
- Brookdale Senior Living links senior living communities with home-based clinical service access.
- LHC Group uses hospital relationships and physician networks to support home health referrals.
- Amedisys builds service depth across home health and hospice care programs.
Competition centers on service reach and payer alignment across home care delivery. Providers need clinical quality and operational discipline to manage patient needs inside residential environments. Leading providers can support referral networks through trained caregivers and digital records.
Brookdale Senior Living competes through senior living communities and home care clinical services. LHC Group competes through partnerships with hospitals and physician groups. Amedisys supports its position through home health and personal care services.
Kindred Healthcare uses hybrid care models that extend hospital level capabilities into the home. Encompass Health focuses on therapy based models and remote oversight tools. Regional operators compete through pediatric support and palliative services.
Key Companies in the Home Care Services Market
Key global companies leading the home care services market include:
- Brookdale Senior Living, LHC Group, and Amedisys Inc. have strong care delivery networks across senior care and home health services. Their positions are supported by clinical service depth and referral access across organized care channels.
- Kindred Healthcare LLC and Encompass Health Corporation have built positions across therapy-led care and home recovery support. Their operating models support patients moving from facility care into residential recovery programs.
- Interim HealthCare, AccentCare, and BAYADA Home Health Care have strong regional presence across personal care and skilled nursing services. Addus HomeCare and Visiting Nurse Service of New York also support organized home care delivery across selected markets.
Competitive Benchmarking: Home Care Services Market
| Company | Service Breadth | Clinical Care Depth | Payer Alignment | Digital Care Capability | Geographic Footprint |
|---|---|---|---|---|---|
| Brookdale Senior Living | High | Medium | Moderate | Medium | USA |
| LHC Group | High | High | Strong | High | USA |
| Amedisys Inc. | High | High | Strong | High | USA |
| Kindred Healthcare LLC | Medium | High | Strong | Medium | USA |
| Encompass Health Corporation | Medium | High | Strong | High | USA |
| Interim HealthCare | High | Medium | Moderate | Medium | USA |
| AccentCare | High | High | Strong | High | USA |
| BAYADA Home Health Care | High | High | Moderate | Medium | USA and International |
| Addus HomeCare | Medium | Medium | Strong | Medium | USA |
| Visiting Nurse Service of New York | Medium | High | Strong | Medium | USA |
Source: Future Market Insights, 2026.
Recent Developments
- In December 2024 Addus HomeCare acquired Gentiva’s personal care operations and added services for 16,000 daily consumers across seven states while becoming Texas’s largest provider.
- In March 2026 Aveanna Healthcare agreed to acquire Family First Homecare to expand pediatric home care and skilled private duty nursing across seven states.
Key Players in the Home Care Services Market:
Major Global Players:
- Brookdale Senior Living
- LHC Group
- Amedisys Inc.
- Kindred Healthcare LLC
- Encompass Health Corporation
Regional and Community-Focused Players:
- Interim HealthCare
- AccentCare
- BAYADA Home Health Care
- Addus HomeCare
- Visiting Nurse Service of New York
Report Scope and Coverage

| Parameter | Details |
|---|---|
| Quantitative Units | USD 659.5 billion to USD 1,789.9 billion, at a CAGR of 10.5% |
| Market Definition | Home care services cover clinical and daily support delivered in residential settings. |
| Regions Covered | North America; Latin America; Europe; East Asia; South Asia and Pacific; Middle East and Africa |
| Countries Covered | United States; China; Germany; India; United Kingdom; Japan; Brazil; Canada; France; Australia |
| Key Companies Profiled | Brookdale Senior Living; LHC Group; Amedisys Inc.; Kindred Healthcare LLC; Encompass Health Corporation |
| Forecast Period | 2026 to 2036 |
| Approach | Hybrid bottom-up and top-down methodology using service demand and regional adoption patterns. |
Source: Future Market Insights, 2026.
Home Care Services Market by Segment
Home Care Services Market Segmented by Service Type:
- Health Care Services
- Non-Health Care Services
Home Care Services Market Segmented by End User:
- Children
- Adults
- Geriatric
Home Care Services Market Segmented by Payer Type:
- Government Programs
- Insurance Plans
- Self-Pay Users
Home Care Services Market Segmented by Duration:
- Long-Term Care
- Short-Term Care
Home Care Services Market Segmented by Delivery Type:
- Skilled Nursing
- Rehabilitation Support
- Personal Assistance
- Companionship Care
- Medication Management
- Hospice Care
- Telehealth Support
- Remote Monitoring
Home Care Services Market by Region:
- North America
- USA
- Canada
- Mexico
- Latin America
- Brazil
- Chile
- Rest of Latin America
- Europe
- Germany
- UK
- Italy
- Spain
- France
- Rest of Europe
- East Asia
- China
- Japan
- South Korea
- South Asia and Pacific
- India
- ASEAN
- Australia & New Zealand
- Rest of South Asia and Pacific
- Middle East and Africa
- Saudi Arabia
- Other GCC Countries
- South Africa
- Rest of Middle East and Africa
Research Sources and Bibliography
- Addus HomeCare Corporation. (2024, December 2). Addus HomeCare completes acquisition of personal care operations of Gentiva.
- Aveanna Healthcare Holdings Inc. (2026, March 12). Aveanna Healthcare Holdings announces agreement to acquire Family First Homecare
- Amedisys Inc. (2024). Home health, hospice, and personal care
- Brookdale Senior Living. (2024). Brookdale HealthPlus® Communities Deliver Value, Opportunity for Patients and HCPs
This Report Answers
- What is the current and future size of the home care services market?
- How fast is the home care services market expected to expand between 2026 and 2036?
- Which service type is likely to lead the market by 2026?
- Which end-user segment is expected to account for the highest demand by 2026?
- What factors are supporting demand for home care services globally?
- How are digital coordination tools influencing home care service adoption?
- Why is geriatric care a major demand center for home care services?
- How are workforce shortages affecting provider scale across the market?
- Which countries are projected to record faster expansion through 2036?
- What is supporting market expansion in India and Germany?
- Who are the key companies active in the home care services market?
- How does FMI estimate and validate the home care services forecast?
Frequently Asked Questions
What is the global market demand for Home Care Services in 2026?
In 2026, the global market for home care services is expected to be worth USD 659.5 billion.
How big will the market for Home Care Services be in 2036?
By 2036, the market for home care services is expected to be worth USD 1,789.9 billion.
How much is demand for Home Care Services expected to expand between 2026 and 2036?
Between 2026 and 2036, demand for home care services is expected to expand at a CAGR of 10.5%.
Which service type segment is likely to be the leading seller globally by 2026?
Health care services will make up 58.7% share in 2026 across service type demand.
What is causing demand to rise in India?
India home care services demand is projected to expand at a CAGR of 7.8% through 2036, supported by organized caregiving and lifestyle disease needs.
What is causing demand to rise in the United States?
United States home care services demand is projected to expand at a CAGR of 6.5% through 2036, supported by home nursing reimbursement and remote monitoring.
What does this report mean by Home Care Services Market definition?
Home care services market includes clinical and daily support delivered inside residential settings for patients and older adults.
Table of Content
- Executive Summary
- Global Market Outlook
- Demand to side Trends
- Supply to side Trends
- Technology Roadmap Analysis
- Analysis and Recommendations
- Market Overview
- Market Coverage / Taxonomy
- Market Definition / Scope / Limitations
- Research Methodology
- Chapter Orientation
- Analytical Lens and Working Hypotheses
- Market Structure, Signals, and Trend Drivers
- Benchmarking and Cross-market Comparability
- Market Sizing, Forecasting, and Opportunity Mapping
- Research Design and Evidence Framework
- Desk Research Programme (Secondary Evidence)
- Company Annual and Sustainability Reports
- Peer-reviewed Journals and Academic Literature
- Corporate Websites, Product Literature, and Technical Notes
- Earnings Decks and Investor Briefings
- Statutory Filings and Regulatory Disclosures
- Technical White Papers and Standards Notes
- Trade Journals, Industry Magazines, and Analyst Briefs
- Conference Proceedings, Webinars, and Seminar Materials
- Government Statistics Portals and Public Data Releases
- Press Releases and Reputable Media Coverage
- Specialist Newsletters and Curated Briefings
- Sector Databases and Reference Repositories
- FMI Internal Proprietary Databases and Historical Market Datasets
- Subscription Datasets and Paid Sources
- Social Channels, Communities, and Digital Listening Inputs
- Additional Desk Sources
- Expert Input and Fieldwork (Primary Evidence)
- Primary Modes
- Qualitative Interviews and Expert Elicitation
- Quantitative Surveys and Structured Data Capture
- Blended Approach
- Why Primary Evidence is Used
- Field Techniques
- Interviews
- Surveys
- Focus Groups
- Observational and In-context Research
- Social and Community Interactions
- Stakeholder Universe Engaged
- C-suite Leaders
- Board Members
- Presidents and Vice Presidents
- R&D and Innovation Heads
- Technical Specialists
- Domain Subject-matter Experts
- Scientists
- Physicians and Other Healthcare Professionals
- Governance, Ethics, and Data Stewardship
- Research Ethics
- Data Integrity and Handling
- Primary Modes
- Tooling, Models, and Reference Databases
- Desk Research Programme (Secondary Evidence)
- Data Engineering and Model Build
- Data Acquisition and Ingestion
- Cleaning, Normalisation, and Verification
- Synthesis, Triangulation, and Analysis
- Quality Assurance and Audit Trail
- Market Background
- Market Dynamics
- Drivers
- Restraints
- Opportunity
- Trends
- Scenario Forecast
- Demand in Optimistic Scenario
- Demand in Likely Scenario
- Demand in Conservative Scenario
- Opportunity Map Analysis
- Product Life Cycle Analysis
- Supply Chain Analysis
- Investment Feasibility Matrix
- Value Chain Analysis
- PESTLE and Porter’s Analysis
- Regulatory Landscape
- Regional Parent Market Outlook
- Production and Consumption Statistics
- Import and Export Statistics
- Market Dynamics
- Global Market Analysis 2021 to 2025 and Forecast, 2026 to 2036
- Historical Market Size Value (USD Million) Analysis, 2021 to 2025
- Current and Future Market Size Value (USD Million) Projections, 2026 to 2036
- Y to o to Y Growth Trend Analysis
- Absolute $ Opportunity Analysis
- Global Market Pricing Analysis 2021 to 2025 and Forecast 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Service Type
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Service Type , 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Service Type , 2026 to 2036
- Health Care Services
- Non-Health Care Services
- Health Care Services
- Y to o to Y Growth Trend Analysis By Service Type , 2021 to 2025
- Absolute $ Opportunity Analysis By Service Type , 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By End User
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By End User, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By End User, 2026 to 2036
- Geriatric
- Children
- Adults
- Geriatric
- Y to o to Y Growth Trend Analysis By End User, 2021 to 2025
- Absolute $ Opportunity Analysis By End User, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Payer
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Payer, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Payer, 2026 to 2036
- Government Programs
- Insurance Plans
- Self-Pay Users
- Government Programs
- Y to o to Y Growth Trend Analysis By Payer, 2021 to 2025
- Absolute $ Opportunity Analysis By Payer, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Duration
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Duration, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Duration, 2026 to 2036
- Long-Term Care
- Short-Term Care
- Long-Term Care
- Y to o to Y Growth Trend Analysis By Duration, 2021 to 2025
- Absolute $ Opportunity Analysis By Duration, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Delivery
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Delivery, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Delivery, 2026 to 2036
- Skilled Nursing
- Rehabilitation Support
- Personal Assistance
- Companionship Care
- Medication Management
- Hospice Care
- Telehealth Support
- Remote Monitoring
- Skilled Nursing
- Y to o to Y Growth Trend Analysis By Delivery, 2021 to 2025
- Absolute $ Opportunity Analysis By Delivery, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Region
- Introduction
- Historical Market Size Value (USD Million) Analysis By Region, 2021 to 2025
- Current Market Size Value (USD Million) Analysis and Forecast By Region, 2026 to 2036
- North America
- Latin America
- Western Europe
- Eastern Europe
- East Asia
- South Asia and Pacific
- Middle East & Africa
- Market Attractiveness Analysis By Region
- North America Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- USA
- Canada
- Mexico
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- By Country
- Market Attractiveness Analysis
- By Country
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Key Takeaways
- Latin America Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Brazil
- Chile
- Rest of Latin America
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- By Country
- Market Attractiveness Analysis
- By Country
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Key Takeaways
- Western Europe Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Germany
- UK
- Italy
- Spain
- France
- Nordic
- BENELUX
- Rest of Western Europe
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- By Country
- Market Attractiveness Analysis
- By Country
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Key Takeaways
- Eastern Europe Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Russia
- Poland
- Hungary
- Balkan & Baltic
- Rest of Eastern Europe
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- By Country
- Market Attractiveness Analysis
- By Country
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Key Takeaways
- East Asia Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- China
- Japan
- South Korea
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- By Country
- Market Attractiveness Analysis
- By Country
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Key Takeaways
- South Asia and Pacific Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- India
- ASEAN
- Australia & New Zealand
- Rest of South Asia and Pacific
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- By Country
- Market Attractiveness Analysis
- By Country
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Key Takeaways
- Middle East & Africa Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Kingdom of Saudi Arabia
- Other GCC Countries
- Turkiye
- South Africa
- Other African Union
- Rest of Middle East & Africa
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- By Country
- Market Attractiveness Analysis
- By Country
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Key Takeaways
- Key Countries Market Analysis
- USA
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Canada
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Mexico
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Brazil
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Chile
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Germany
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- UK
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Italy
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Spain
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- France
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- India
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- ASEAN
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Australia & New Zealand
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- China
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Japan
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- South Korea
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Russia
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Poland
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Hungary
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Kingdom of Saudi Arabia
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Turkiye
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- South Africa
- Pricing Analysis
- Market Share Analysis, 2025
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- USA
- Market Structure Analysis
- Competition Dashboard
- Competition Benchmarking
- Market Share Analysis of Top Players
- By Regional
- By Service Type
- By End User
- By Payer
- By Duration
- By Delivery
- Competition Analysis
- Competition Deep Dive
- Brookdale Senior Living
- Overview
- Product Portfolio
- Profitability by Market Segments (Product/Age /Sales Channel/Region)
- Sales Footprint
- Strategy Overview
- Marketing Strategy
- Product Strategy
- Channel Strategy
- LHC Group
- Amedisys Inc.
- Kindred Healthcare LLC
- Encompass Health Corporation
- Interim HealthCare
- AccentCare
- BAYADA Home Health Care
- Addus HomeCare
- Visiting Nurse Service of New York
- Brookdale Senior Living
- Competition Deep Dive
- Assumptions & Acronyms Used
List of Tables
- Table 1: Global Market Value (USD Million) Forecast by Region, 2021 to 2036
- Table 2: Global Market Value (USD Million) Forecast by Service Type , 2021 to 2036
- Table 3: Global Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 4: Global Market Value (USD Million) Forecast by Payer, 2021 to 2036
- Table 5: Global Market Value (USD Million) Forecast by Duration, 2021 to 2036
- Table 6: Global Market Value (USD Million) Forecast by Delivery, 2021 to 2036
- Table 7: North America Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 8: North America Market Value (USD Million) Forecast by Service Type , 2021 to 2036
- Table 9: North America Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 10: North America Market Value (USD Million) Forecast by Payer, 2021 to 2036
- Table 11: North America Market Value (USD Million) Forecast by Duration, 2021 to 2036
- Table 12: North America Market Value (USD Million) Forecast by Delivery, 2021 to 2036
- Table 13: Latin America Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 14: Latin America Market Value (USD Million) Forecast by Service Type , 2021 to 2036
- Table 15: Latin America Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 16: Latin America Market Value (USD Million) Forecast by Payer, 2021 to 2036
- Table 17: Latin America Market Value (USD Million) Forecast by Duration, 2021 to 2036
- Table 18: Latin America Market Value (USD Million) Forecast by Delivery, 2021 to 2036
- Table 19: Western Europe Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 20: Western Europe Market Value (USD Million) Forecast by Service Type , 2021 to 2036
- Table 21: Western Europe Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 22: Western Europe Market Value (USD Million) Forecast by Payer, 2021 to 2036
- Table 23: Western Europe Market Value (USD Million) Forecast by Duration, 2021 to 2036
- Table 24: Western Europe Market Value (USD Million) Forecast by Delivery, 2021 to 2036
- Table 25: Eastern Europe Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 26: Eastern Europe Market Value (USD Million) Forecast by Service Type , 2021 to 2036
- Table 27: Eastern Europe Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 28: Eastern Europe Market Value (USD Million) Forecast by Payer, 2021 to 2036
- Table 29: Eastern Europe Market Value (USD Million) Forecast by Duration, 2021 to 2036
- Table 30: Eastern Europe Market Value (USD Million) Forecast by Delivery, 2021 to 2036
- Table 31: East Asia Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 32: East Asia Market Value (USD Million) Forecast by Service Type , 2021 to 2036
- Table 33: East Asia Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 34: East Asia Market Value (USD Million) Forecast by Payer, 2021 to 2036
- Table 35: East Asia Market Value (USD Million) Forecast by Duration, 2021 to 2036
- Table 36: East Asia Market Value (USD Million) Forecast by Delivery, 2021 to 2036
- Table 37: South Asia and Pacific Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 38: South Asia and Pacific Market Value (USD Million) Forecast by Service Type , 2021 to 2036
- Table 39: South Asia and Pacific Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 40: South Asia and Pacific Market Value (USD Million) Forecast by Payer, 2021 to 2036
- Table 41: South Asia and Pacific Market Value (USD Million) Forecast by Duration, 2021 to 2036
- Table 42: South Asia and Pacific Market Value (USD Million) Forecast by Delivery, 2021 to 2036
- Table 43: Middle East & Africa Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 44: Middle East & Africa Market Value (USD Million) Forecast by Service Type , 2021 to 2036
- Table 45: Middle East & Africa Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 46: Middle East & Africa Market Value (USD Million) Forecast by Payer, 2021 to 2036
- Table 47: Middle East & Africa Market Value (USD Million) Forecast by Duration, 2021 to 2036
- Table 48: Middle East & Africa Market Value (USD Million) Forecast by Delivery, 2021 to 2036
List of Figures
- Figure 1: Global Market Pricing Analysis
- Figure 2: Global Market Value (USD Million) Forecast 2021-2036
- Figure 3: Global Market Value Share and BPS Analysis by Service Type , 2026 and 2036
- Figure 4: Global Market Y-o-Y Growth Comparison by Service Type , 2026-2036
- Figure 5: Global Market Attractiveness Analysis by Service Type
- Figure 6: Global Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 7: Global Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 8: Global Market Attractiveness Analysis by End User
- Figure 9: Global Market Value Share and BPS Analysis by Payer, 2026 and 2036
- Figure 10: Global Market Y-o-Y Growth Comparison by Payer, 2026-2036
- Figure 11: Global Market Attractiveness Analysis by Payer
- Figure 12: Global Market Value Share and BPS Analysis by Duration, 2026 and 2036
- Figure 13: Global Market Y-o-Y Growth Comparison by Duration, 2026-2036
- Figure 14: Global Market Attractiveness Analysis by Duration
- Figure 15: Global Market Value Share and BPS Analysis by Delivery, 2026 and 2036
- Figure 16: Global Market Y-o-Y Growth Comparison by Delivery, 2026-2036
- Figure 17: Global Market Attractiveness Analysis by Delivery
- Figure 18: Global Market Value (USD Million) Share and BPS Analysis by Region, 2026 and 2036
- Figure 19: Global Market Y-o-Y Growth Comparison by Region, 2026-2036
- Figure 20: Global Market Attractiveness Analysis by Region
- Figure 21: North America Market Incremental Dollar Opportunity, 2026-2036
- Figure 22: Latin America Market Incremental Dollar Opportunity, 2026-2036
- Figure 23: Western Europe Market Incremental Dollar Opportunity, 2026-2036
- Figure 24: Eastern Europe Market Incremental Dollar Opportunity, 2026-2036
- Figure 25: East Asia Market Incremental Dollar Opportunity, 2026-2036
- Figure 26: South Asia and Pacific Market Incremental Dollar Opportunity, 2026-2036
- Figure 27: Middle East & Africa Market Incremental Dollar Opportunity, 2026-2036
- Figure 28: North America Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 29: North America Market Value Share and BPS Analysis by Service Type , 2026 and 2036
- Figure 30: North America Market Y-o-Y Growth Comparison by Service Type , 2026-2036
- Figure 31: North America Market Attractiveness Analysis by Service Type
- Figure 32: North America Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 33: North America Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 34: North America Market Attractiveness Analysis by End User
- Figure 35: North America Market Value Share and BPS Analysis by Payer, 2026 and 2036
- Figure 36: North America Market Y-o-Y Growth Comparison by Payer, 2026-2036
- Figure 37: North America Market Attractiveness Analysis by Payer
- Figure 38: North America Market Value Share and BPS Analysis by Duration, 2026 and 2036
- Figure 39: North America Market Y-o-Y Growth Comparison by Duration, 2026-2036
- Figure 40: North America Market Attractiveness Analysis by Duration
- Figure 41: North America Market Value Share and BPS Analysis by Delivery, 2026 and 2036
- Figure 42: North America Market Y-o-Y Growth Comparison by Delivery, 2026-2036
- Figure 43: North America Market Attractiveness Analysis by Delivery
- Figure 44: Latin America Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 45: Latin America Market Value Share and BPS Analysis by Service Type , 2026 and 2036
- Figure 46: Latin America Market Y-o-Y Growth Comparison by Service Type , 2026-2036
- Figure 47: Latin America Market Attractiveness Analysis by Service Type
- Figure 48: Latin America Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 49: Latin America Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 50: Latin America Market Attractiveness Analysis by End User
- Figure 51: Latin America Market Value Share and BPS Analysis by Payer, 2026 and 2036
- Figure 52: Latin America Market Y-o-Y Growth Comparison by Payer, 2026-2036
- Figure 53: Latin America Market Attractiveness Analysis by Payer
- Figure 54: Latin America Market Value Share and BPS Analysis by Duration, 2026 and 2036
- Figure 55: Latin America Market Y-o-Y Growth Comparison by Duration, 2026-2036
- Figure 56: Latin America Market Attractiveness Analysis by Duration
- Figure 57: Latin America Market Value Share and BPS Analysis by Delivery, 2026 and 2036
- Figure 58: Latin America Market Y-o-Y Growth Comparison by Delivery, 2026-2036
- Figure 59: Latin America Market Attractiveness Analysis by Delivery
- Figure 60: Western Europe Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 61: Western Europe Market Value Share and BPS Analysis by Service Type , 2026 and 2036
- Figure 62: Western Europe Market Y-o-Y Growth Comparison by Service Type , 2026-2036
- Figure 63: Western Europe Market Attractiveness Analysis by Service Type
- Figure 64: Western Europe Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 65: Western Europe Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 66: Western Europe Market Attractiveness Analysis by End User
- Figure 67: Western Europe Market Value Share and BPS Analysis by Payer, 2026 and 2036
- Figure 68: Western Europe Market Y-o-Y Growth Comparison by Payer, 2026-2036
- Figure 69: Western Europe Market Attractiveness Analysis by Payer
- Figure 70: Western Europe Market Value Share and BPS Analysis by Duration, 2026 and 2036
- Figure 71: Western Europe Market Y-o-Y Growth Comparison by Duration, 2026-2036
- Figure 72: Western Europe Market Attractiveness Analysis by Duration
- Figure 73: Western Europe Market Value Share and BPS Analysis by Delivery, 2026 and 2036
- Figure 74: Western Europe Market Y-o-Y Growth Comparison by Delivery, 2026-2036
- Figure 75: Western Europe Market Attractiveness Analysis by Delivery
- Figure 76: Eastern Europe Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 77: Eastern Europe Market Value Share and BPS Analysis by Service Type , 2026 and 2036
- Figure 78: Eastern Europe Market Y-o-Y Growth Comparison by Service Type , 2026-2036
- Figure 79: Eastern Europe Market Attractiveness Analysis by Service Type
- Figure 80: Eastern Europe Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 81: Eastern Europe Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 82: Eastern Europe Market Attractiveness Analysis by End User
- Figure 83: Eastern Europe Market Value Share and BPS Analysis by Payer, 2026 and 2036
- Figure 84: Eastern Europe Market Y-o-Y Growth Comparison by Payer, 2026-2036
- Figure 85: Eastern Europe Market Attractiveness Analysis by Payer
- Figure 86: Eastern Europe Market Value Share and BPS Analysis by Duration, 2026 and 2036
- Figure 87: Eastern Europe Market Y-o-Y Growth Comparison by Duration, 2026-2036
- Figure 88: Eastern Europe Market Attractiveness Analysis by Duration
- Figure 89: Eastern Europe Market Value Share and BPS Analysis by Delivery, 2026 and 2036
- Figure 90: Eastern Europe Market Y-o-Y Growth Comparison by Delivery, 2026-2036
- Figure 91: Eastern Europe Market Attractiveness Analysis by Delivery
- Figure 92: East Asia Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 93: East Asia Market Value Share and BPS Analysis by Service Type , 2026 and 2036
- Figure 94: East Asia Market Y-o-Y Growth Comparison by Service Type , 2026-2036
- Figure 95: East Asia Market Attractiveness Analysis by Service Type
- Figure 96: East Asia Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 97: East Asia Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 98: East Asia Market Attractiveness Analysis by End User
- Figure 99: East Asia Market Value Share and BPS Analysis by Payer, 2026 and 2036
- Figure 100: East Asia Market Y-o-Y Growth Comparison by Payer, 2026-2036
- Figure 101: East Asia Market Attractiveness Analysis by Payer
- Figure 102: East Asia Market Value Share and BPS Analysis by Duration, 2026 and 2036
- Figure 103: East Asia Market Y-o-Y Growth Comparison by Duration, 2026-2036
- Figure 104: East Asia Market Attractiveness Analysis by Duration
- Figure 105: East Asia Market Value Share and BPS Analysis by Delivery, 2026 and 2036
- Figure 106: East Asia Market Y-o-Y Growth Comparison by Delivery, 2026-2036
- Figure 107: East Asia Market Attractiveness Analysis by Delivery
- Figure 108: South Asia and Pacific Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 109: South Asia and Pacific Market Value Share and BPS Analysis by Service Type , 2026 and 2036
- Figure 110: South Asia and Pacific Market Y-o-Y Growth Comparison by Service Type , 2026-2036
- Figure 111: South Asia and Pacific Market Attractiveness Analysis by Service Type
- Figure 112: South Asia and Pacific Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 113: South Asia and Pacific Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 114: South Asia and Pacific Market Attractiveness Analysis by End User
- Figure 115: South Asia and Pacific Market Value Share and BPS Analysis by Payer, 2026 and 2036
- Figure 116: South Asia and Pacific Market Y-o-Y Growth Comparison by Payer, 2026-2036
- Figure 117: South Asia and Pacific Market Attractiveness Analysis by Payer
- Figure 118: South Asia and Pacific Market Value Share and BPS Analysis by Duration, 2026 and 2036
- Figure 119: South Asia and Pacific Market Y-o-Y Growth Comparison by Duration, 2026-2036
- Figure 120: South Asia and Pacific Market Attractiveness Analysis by Duration
- Figure 121: South Asia and Pacific Market Value Share and BPS Analysis by Delivery, 2026 and 2036
- Figure 122: South Asia and Pacific Market Y-o-Y Growth Comparison by Delivery, 2026-2036
- Figure 123: South Asia and Pacific Market Attractiveness Analysis by Delivery
- Figure 124: Middle East & Africa Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 125: Middle East & Africa Market Value Share and BPS Analysis by Service Type , 2026 and 2036
- Figure 126: Middle East & Africa Market Y-o-Y Growth Comparison by Service Type , 2026-2036
- Figure 127: Middle East & Africa Market Attractiveness Analysis by Service Type
- Figure 128: Middle East & Africa Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 129: Middle East & Africa Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 130: Middle East & Africa Market Attractiveness Analysis by End User
- Figure 131: Middle East & Africa Market Value Share and BPS Analysis by Payer, 2026 and 2036
- Figure 132: Middle East & Africa Market Y-o-Y Growth Comparison by Payer, 2026-2036
- Figure 133: Middle East & Africa Market Attractiveness Analysis by Payer
- Figure 134: Middle East & Africa Market Value Share and BPS Analysis by Duration, 2026 and 2036
- Figure 135: Middle East & Africa Market Y-o-Y Growth Comparison by Duration, 2026-2036
- Figure 136: Middle East & Africa Market Attractiveness Analysis by Duration
- Figure 137: Middle East & Africa Market Value Share and BPS Analysis by Delivery, 2026 and 2036
- Figure 138: Middle East & Africa Market Y-o-Y Growth Comparison by Delivery, 2026-2036
- Figure 139: Middle East & Africa Market Attractiveness Analysis by Delivery
- Figure 140: Global Market - Tier Structure Analysis
- Figure 141: Global Market - Company Share Analysis

