Demand for clinical alarm management in the USA is valued at USD 1.3 billion in 2025 and is projected to reach USD 2.0 billion by 2035, reflecting a CAGR of 4.8%. Growth is driven by heightened patient safety priorities, rising alarm volumes in critical care environments, and the need to reduce alarm fatigue among clinicians. Hospitals invest in intelligent alarm systems to improve workflow efficiency and enhance early response to clinical deterioration.
Solutions represent the leading component category because integrated platforms consolidate alerts, filter out non-actionable signals, and route high-priority notifications to the right care teams. Advanced analytics, interoperability with electronic medical records, and adaptive alarm thresholds strengthen real-time clinical decision support. Vendors emphasize cybersecurity, secure device connectivity, and compliance with patient safety standards.
The West, South, and Northeast regions show strong adoption driven by large hospital networks and ongoing improvement initiatives in acute care settings. Key suppliers include Medtronic, GE Healthcare, Koninklijke Philips N.V., Baxter, and Mindray Medical International Limited. Their strategies focus on scalable deployment models, centralized monitoring capabilities, and optimization services that align alarm systems with operational protocols in high-acuity care environments.
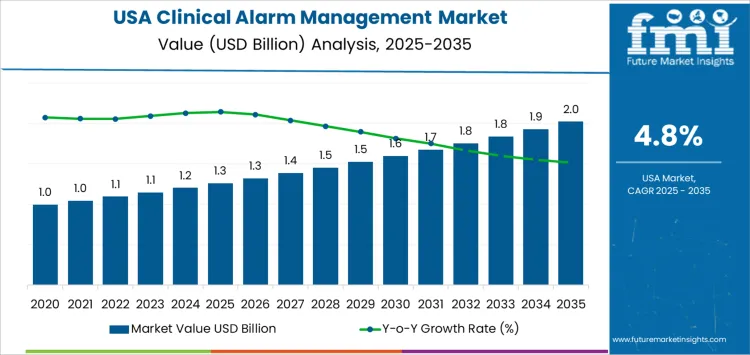
Acceleration in demand for clinical alarm management solutions in the United States is linked to healthcare quality mandates and the need to reduce alarm fatigue. Early in the projection period, hospitals accelerate investments in centralized alarm platforms, smart notification routing, and analytics-driven alarm reduction. Reforms tied to patient safety indicators, nurse efficiency improvement programs, and higher adoption of connected medical devices strengthen the initial growth pace. Integration with electronic health records and IoT-based monitoring also widens early uptake.
Deceleration is gradually appearing as large hospital systems finish deploying enterprise alarm management programs. Once foundational technology and workflow redesign are completed, annual spending shifts from new installations to optimization, software licensing, and incremental upgrades. Smaller healthcare facilities show slower adoption because of budget constraints and limited staff training capacity. Interoperability challenges between legacy equipment and advanced notification systems also create phased implementation rather than rapid scaling.
The pattern shows stronger acceleration in the first half of the forecast period, driven by regulatory urgency and digital transformation goals across major providers. Growth later transitions to a steadier rhythm based on maintenance cycles and continuous compliance, although demand remains sustained by ongoing alerts standardization activities in the United States.
| Metric | Value |
|---|---|
| USA Clinical Alarm Management Sales Value (2025) | USD 1.3 billion |
| USA Clinical Alarm Management Forecast Value (2035) | USD 2.0 billion |
| USA Clinical Alarm Management Forecast CAGR (2025-2035) | 4.8% |
Demand for clinical alarm management solutions in the USA is increasing because hospitals and healthcare facilities face rising pressure to reduce alarm fatigue and improve patient safety. Medical devices such as heart monitors, ventilators and infusion pumps generate frequent alarms, many of which may be non-actionable or false. Alarm management systems help filter and prioritize alerts to ensure staff respond quickly to critical events while reducing unnecessary notifications. Intensive care units, emergency departments and telemetry floors adopt alarm management platforms integrated with nurse call systems and electronic health records. These systems improve care coordination by routing critical alerts to mobile devices or central monitoring stations, reducing response times for urgent patient needs.
Regulatory emphasis on patient safety and new hospital accreditation standards support adoption of alarm management practices. Facility administrators view alarm management as part of quality improvement and risk mitigation strategies. Constraints include costs associated with purchasing and integrating alarm management systems. Implementation requires training staff, revising care protocols and ensuring interoperability with existing devices. Some smaller or resource-limited hospitals may delay adoption until budgets and staffing permit.
Demand for clinical alarm management in the United States is driven by the need to reduce alarm fatigue in hospitals and support patient-safety protocols. Healthcare facilities rely on integrated alert workflows to ensure timely caregiver intervention across intensive care, surgical centers, and general wards. Software platforms support real-time alert routing, while service support ensures configuration stability. Adoption aligns with investments in smart healthcare, centralized monitoring, and electronic health communication.
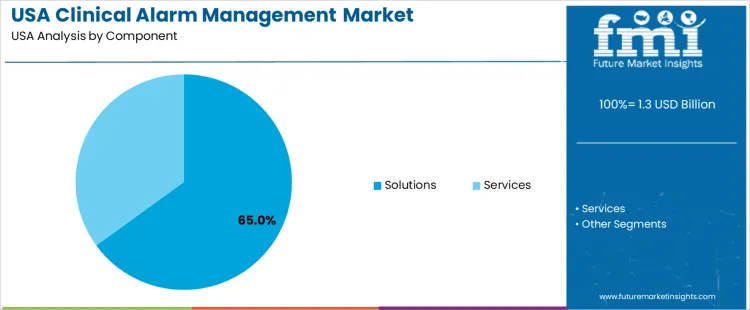
Solutions represent 65.0%. Hospitals depend on analytics-based alarm systems that filter non-actionable alerts while ensuring no delay in high-priority responses. These solutions function across monitors, ventilators, and infusion systems within clinical floors. They improve workflow coordination and enable actionable notifications through secure communication devices. Services account for 35.0%. These include system integration, staff training, and periodic optimization to maintain updated alarm priority settings. Health institutions require scalable performance that addresses environmental noise concerns and improves caregiver productivity. Component selection reflects operational efficiency goals and adherence to patient-safety standards in the USA healthcare landscape.
Key Points:
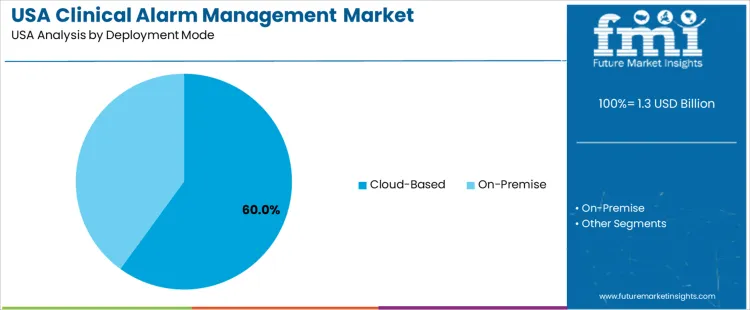
Cloud-based deployment holds 60.0%, supported by rapid implementation, centralized configuration, and multi-facility analytics. Data accessibility enhances clinical coordination and supports continuous improvements in alarm policies across large health networks. On-premise deployment accounts for 40.0%. Some hospitals maintain internal security infrastructure for sensitive patient-monitoring data. Both models reinforce patient-focused alert communication and alarm load management.
Key Points:
In the United States, hospitals deploy more physiological monitoring devices in emergency, critical care and perioperative settings, raising the volume of audible and visual alarms that require clinical response. Alarm fatigue reduction remains a priority for nursing leaders who aim to improve responsiveness to actionable alerts. Health systems adopt centralized alarm platforms that route notifications to mobile devices carried by care teams to reduce missed alarms. Accreditation standards encourage hospitals to document alarm management strategies aimed at improving patient safety. Digital transformation programs link smart beds, infusion pumps and ventilators to alarm middleware that organizes alerts into actionable lists. These patterns sustain procurement aligned with patient safety initiatives and workflow modernization.
Budget allocation challenges, integration complexity and varied readiness across facilities restrain demand.
Hospitals face financial constraints that limit spending on clinical IT systems beyond essential infrastructure. Integration of multiple monitoring brands requires interface development and testing, which extends deployment timelines. Staffing shortages influence the pace of adoption when training time is limited for new alert-management workflows. Smaller facilities with lower device density prioritize simpler notification practices and delay investment in comprehensive platforms. Variability in alarm policies creates differences in technology requirements across departments, which slows standardized purchasing in large health systems. These factors influence how rapidly solutions scale beyond early adopter centers.
Shift toward actionable alarm analytics, increased adoption of mobile notifications and rising interest in cloud-enabled scalability define key trends.
Analytics dashboards highlight alarm frequency, response times and root causes to support improvement programs within nursing and biomedical engineering teams. Mobile routing supports silent communication and maintains patient rest in recovery areas while ensuring rapid clinician awareness. Cloud-based alarm platforms enable remote system updates and scalability for expanding networks across multiple campuses. Middleware designs incorporate role-based escalation rules that align alerts with staff responsibility and reduce unnecessary interruptions.
Demand for clinical alarm management in the United States is supported by patient-safety mandates, expansion of connected medical devices, and focus on reducing alarm fatigue across hospitals. Health systems adopt intelligent alarm analytics to improve clinical responsiveness and comply with regulatory expectations for actionable alerts. Procurement teams evaluate workflow optimization, device-integration compatibility, and cybersecurity readiness. West USA leads with 5.6% CAGR, followed by South USA at 5.0%, Northeast USA at 4.5%, and Midwest USA at 3.9%. Budget planning emphasizes alarm governance programs and scalable deployment of centralized monitoring solutions.
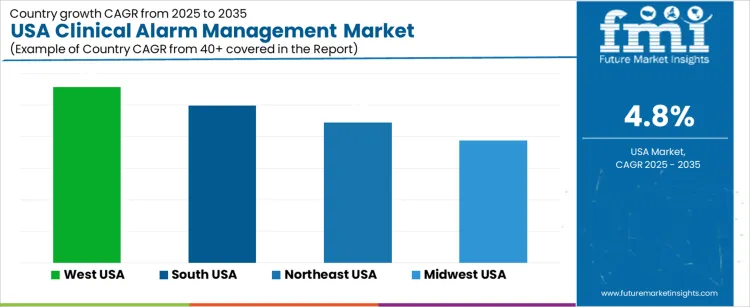
| Region | CAGR (2025-2035) |
|---|---|
| West USA | 5.6% |
| South USA | 5.0% |
| Northeast USA | 4.5% |
| Midwest USA | 3.9% |
West USA reports 5.6% CAGR, driven by hospital modernization projects and early adoption of digital-monitoring ecosystems across California and Washington. Health networks implement alarm-filtering systems to support nursing efficiency during high patient throughput. Integration with EHR-connected smart alarms improves care coordination within intensive-care and telemetry units. Procurement focuses on scalable analytics engines capable of interpreting multisignal streams from wearable sensors and fixed bedside monitors. Stakeholders evaluate interoperability with legacy devices to avoid infrastructure disruption during deployment phases.
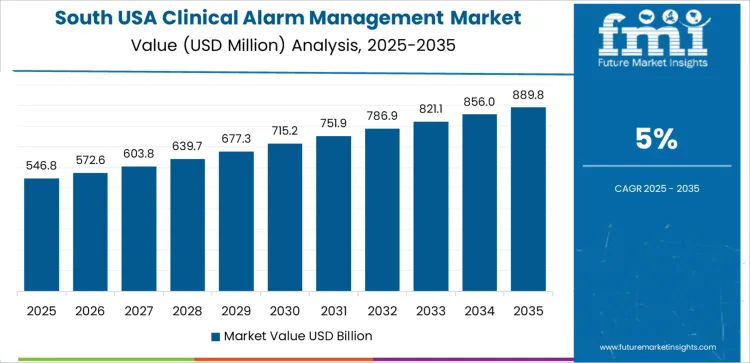
South USA grows at 5.0% CAGR, influenced by rising hospital occupancy in Texas and Florida. Large health systems seek unified alarm-escalation platforms to maintain patient oversight across expanded critical-care units. Staff-support requirements guide investment in mobile alerting systems that route actionable alarms to care teams. Training programs reinforce alarm-response accuracy in emergency departments. Buyers assess vendor support capabilities linked to cybersecurity, uptime assurance, and round-the-clock technical service coverage.
Northeast USA achieves 4.5% CAGR, shaped by regulated patient-safety standards across New York and Massachusetts. Hospitals pursue precision alarm targeting to reduce noise levels on inpatient floors. Academic medical centers collaborate with vendors on AI-powered analytics to evaluate alarm relevance. Implementation programs emphasize structured alarm-governance committees and measurable alert-reduction targets. Procurement includes requirements for robust data integrity during device integration across multivendor environments.
Midwest USA posts 3.9% CAGR, linked to operational efficiency initiatives in regional hospital groups. Facilities adopt centralized alarm-management hubs to support reduced staffing ratios during off-peak shifts. Focus remains on technologies that allow consistent alarm routing across step-down, general-care, and long-term-care units. Decision-makers review total cost of ownership and ease of configuration when updating existing alerting environments. Local distributors sustain implementation continuity through on-site maintenance support.
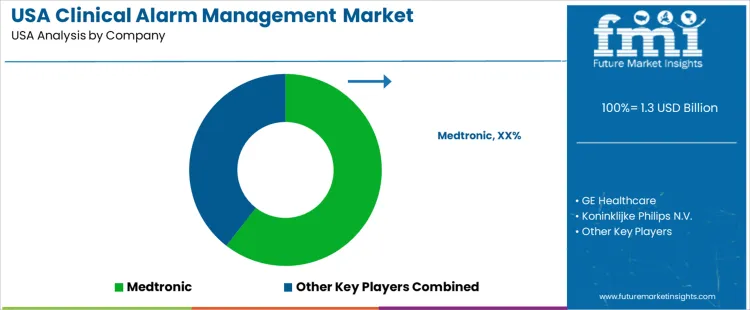
Demand for clinical alarm management solutions in the United States aligns with hospital requirements to reduce alarm fatigue, improve patient-monitoring accuracy, and streamline alert workflows across critical-care units. Purchasing criteria focus on device interoperability, alert-routing precision, cybersecurity controls, and EHR connectivity. Reliability during high-acuity care and support for Joint Commission compliance influence selection among large health systems and regional hospitals.
Medtronic holds an estimated 60.5% share supported by broad deployment of patient-monitoring platforms that include configurable alarm logic, caregiver notification, and integration within established clinical-communication systems. Its footprint across intensive care and perioperative environments strengthens retention where staff rely on consistent device behavior. GE Healthcare provides alarm-signal processing features aligned to multi-parameter monitors used in emergency departments and cardiac care, enabling standardized alert settings across mixed device fleets. Koninklijke Philips N.V. participates through scalable hospital-wide alarm solutions that enable centralized oversight and analytics, helping organizations adjust alarm protocols.
Baxter contributes with infusion-system alert controls that align to medication-safety workflows inside USA hospitals. Mindray Medical International Limited supplies monitoring equipment used in facilities, balancing cost efficiency with the required alarm-reliability standards across diverse care settings. Competitive advantage depends on accurate prioritization of events, secure data routing, and service coverage that minimizes clinical downtime.
| Items | Values |
|---|---|
| Quantitative Units | USD billion |
| Component | Solutions, Services |
| Deployment Mode | Cloud-Based, On-Premise |
| End User | Hospitals, Clinics, Ambulatory Surgical Centers, Long Term & Palliative Care Centers, Home Care, Others |
| Application | Orthopedic Implants, Dental Implants, Craniomaxillofacial Implant |
| Regions Covered | West USA, South USA, Northeast USA, Midwest USA |
| Key Companies Profiled | Medtronic, GE Healthcare, Koninklijke Philips N.V., Baxter, Mindray Medical International Limited |
| Additional Attributes | Dollar sales by component, deployment mode, end-user, and clinical application; regional growth trends across key USA healthcare systems; adoption of cloud-enabled alarm analytics and centralized alarm response platforms; compliance with alarm fatigue reduction guidelines set by clinical safety bodies; integration with EHR, nurse call systems, and patient monitoring ecosystems to enhance workflow efficiency and patient safety outcomes. |
How big is the demand for clinical alarm management in USA in 2025?
The demand for clinical alarm management in USA is estimated to be valued at USD 1.3 billion in 2025.
What will be the size of clinical alarm management in USA in 2035?
The market size for the clinical alarm management in USA is projected to reach USD 2.0 billion by 2035.
How much will be the demand for clinical alarm management in USA growth between 2025 and 2035?
The demand for clinical alarm management in USA is expected to grow at a 4.8% CAGR between 2025 and 2035.
What are the key product types in the clinical alarm management in USA?
The key product types in clinical alarm management in USA are solutions and services.
Which deployment mode segment is expected to contribute significant share in the clinical alarm management in USA in 2025?
In terms of deployment mode, cloud-based segment is expected to command 60.0% share in the clinical alarm management in USA in 2025.
Full Research Suite comprises of:
Market outlook & trends analysis
Interviews & case studies
Strategic recommendations
Vendor profiles & capabilities analysis
5-year forecasts
8 regions and 60+ country-level data splits
Market segment data splits
12 months of continuous data updates
DELIVERED AS:
PDF EXCEL ONLINE

Thank you!
You will receive an email from our Business Development Manager. Please be sure to check your SPAM/JUNK folder too.