AI-Powered Formulary Management Market
The report analyzes the AI-powered formulary management market by component, deployment, function, end user, application, and region from 2026 to 2036.
Historical Data Covered: 2016 to 2024 | Base Year: 2025 | Estimated Year: 2026 | Forecast Period: 2027 to 2036
AI-Powered Formulary Management Market Size, Market Forecast and Outlook By FMI
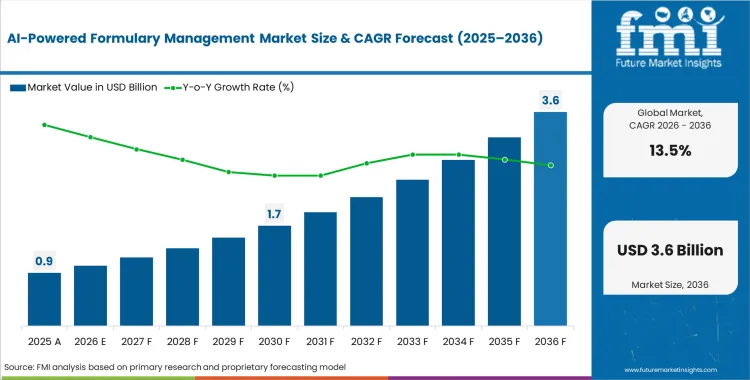
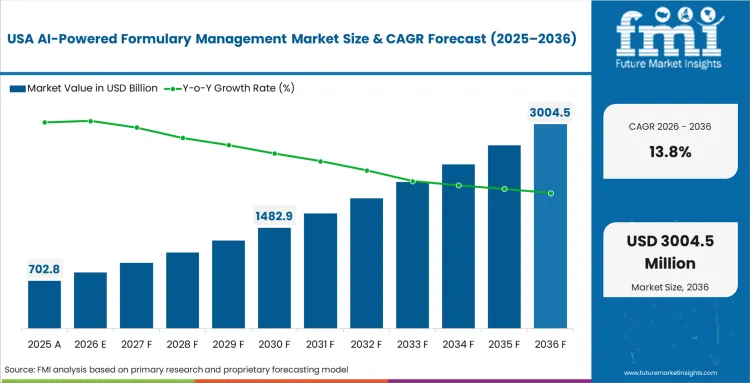
The AI-powered formulary management market crossed a valuation of USD 0.8 billion in 2025, with the industry revenue incline estimated to surpass USD 0.9 billion in 2026 at a CAGR of 13.5% during the forecast period. Continuous progress carries total market expansion to USD 3.2 billion through 2036 as legacy rule engines fail to process complex criteria rapidly enough to meet modern compliance standards.
Summary of AI-Powered Formulary Management Market
- The market is forecast to reach USD 3.2 billion by 2036.
- The market is expected to grow at a CAGR of 13.5% from 2026 to 2036.
- The market was estimated at USD 0.8 billion in 2025.
- The forecast period represents an incremental opportunity of USD 2.3 billion.
- The market focuses on AI-driven software that verifies drug coverage, suggests cost-effective alternatives, and enables real-time prior authorizations.
- Growth is driven by rising demand for instant patient cost visibility and increasing volumes of digital prescriptions.
- Automation is gaining traction as healthcare providers seek to reduce administrative burden and eliminate delays caused by manual approval workflows.
- The United States, Canada, and Saudi Arabia are among the fastest-growing markets, with the United States leading at a 13.8% CAGR through 2036.
- Cloud-based platforms and scalable software solutions dominate due to faster updates, broader data access, and ease of integration.
- Benefit intelligence leads the functional segment, while pharmacy benefit managers remain the primary end users.
- Key players in the market include Optum Rx, CVS Caremark, Express Scripts (Evernorth), Surescripts, DrFirst, CoverMyMeds, and Arrive Health.
Health insurers are under growing pressure to update covered drug lists more frequently as formulary logic becomes more dynamic. Manual spreadsheet-based workflows are losing relevance because they cannot support the speed and accuracy required for ongoing coverage adjustments. Automated policy software is gaining importance by reducing administrative burden across formulary maintenance and improving the consistency of benefit updates. Clinical pharmacy teams, in turn, are likely to devote more attention to exception handling and appeal review rather than routine manual entry.
Adoption also tends to strengthen when automated formulary tools are embedded directly into digital prescribing workflows. Real-time visibility into drug cost and coverage status at the point of prescribing is helping shape earlier treatment decisions with greater reimbursement awareness. Such integration is gradually improving alignment between prescribing behavior, coverage design, and patient access requirements. Demand growth, as a result, reflects a broader shift toward more automated and connected drug benefit management.
United States is projected to expand at a CAGR of 13.8% from 2026 to 2036. Canada is likely to register 12.2% over the same period as legacy systems continue to be modernized across provincial drug benefit environments. Saudi Arabia is estimated to grow at 12.0% from 2026 to 2036, supported by wider healthcare digitization across coverage administration. United Kingdom is projected to witness 11.6% CAGR through 2036, while Germany is expected to record 10.9%. Australia is likely to advance at 10.7% over the forecast period, and Japan is estimated to post 9.8% CAGR from 2026 to 2036. Regional variation is being shaped by differences in electronic prescribing maturity, formulary system integration, and data governance requirements.
Segmental Analysis
AI-Powered Formulary Management Market Analysis by Component
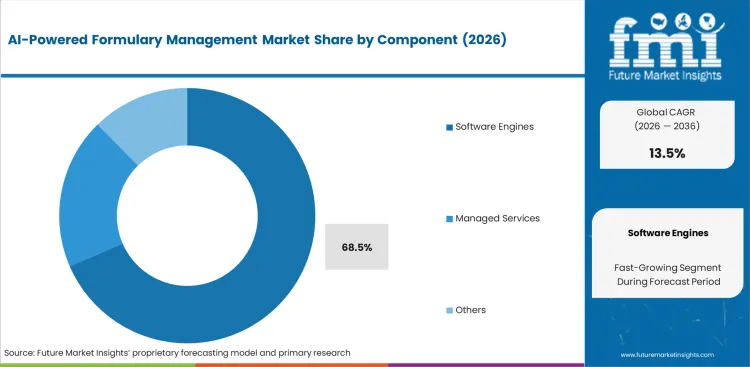
Software engines are anticipated to capture a predicted 68.5% share of the market in 2026 because they form the actual brain of automated tiering. Health networks prioritize buying these core algorithms over hiring external consultants to map out their drug lists manually. Pre-built software instantly processes complex rebate structures and checks patient eligibility without requiring constant human oversight. Customizing these engines allows hospital networks to adapt quickly to sudden changes in pharmaceutical pricing. Relying on outdated manual workflows simply costs too much when healthcare interoperability solutions can connect prescribing software directly to pharmacy benefit databases. Administrators who delay software integration face massive administrative backlogs during the annual enrollment period.
- Initial Licensing Justification: Foundational software licenses bypass the need for massive internal engineering expansions. Benefit administrators gain immediate access to validated clinical pathways.
- Data Security Validation: Maintaining internal control over algorithms prevents sensitive pricing agreements from leaking to external consultants. Compliance officers approve internal software deployments significantly faster than outsourced service models.
- Continuous Update Cycles: Retaining licensed software ensures that tiering logic adapts automatically to new FDA approvals. Executives avoid the hidden costs associated with hiring external implementation groups for every minor policy change.
AI-Powered Formulary Management Market Analysis by Deployment
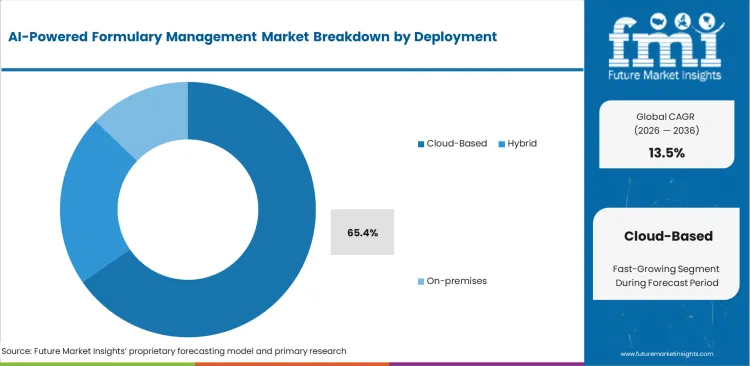
Cloud infrastructure solves the massive data integration problem inherent in modern prescribing networks. Health plans require constant updates to drug pricing and rebate structures across thousands of clinics simultaneously. Driven by their ability to push real-time algorithmic changes without requiring local server maintenance, cloud-based platforms are expected to hold an estimated 65.4% share in 2026. Legacy on-premise setups simply lack the processing speed to handle daily tiering adjustments for millions of covered lives. Hospitals shifting to healthcare cloud computing avoid heavy upfront hardware costs while securing immediate access to global clinical guideline updates. Delaying this transition leaves insurance providers struggling with outdated spreadsheets that leak revenue through inaccurate pharmacy claims.
- Infrastructure Scalability: Cloud hosting allows health plans to expand network capacity without purchasing physical server hardware. System administrators avoid capital expenditure approvals during rapid enrollment growth phases.
- Real-Time Syncing: Pushing drug tier changes through cloud networks updates every connected physician instantly. Network coordinators prevent thousands of prescribing errors that normally occur during the lag time of manual system updates.
- Interoperability Facilitation: Modern application programming interfaces require cloud environments to function securely across different health networks. Compliance officers mandate cloud transitions to meet federal data sharing requirements efficiently.
AI-Powered Formulary Management Market Analysis by Function
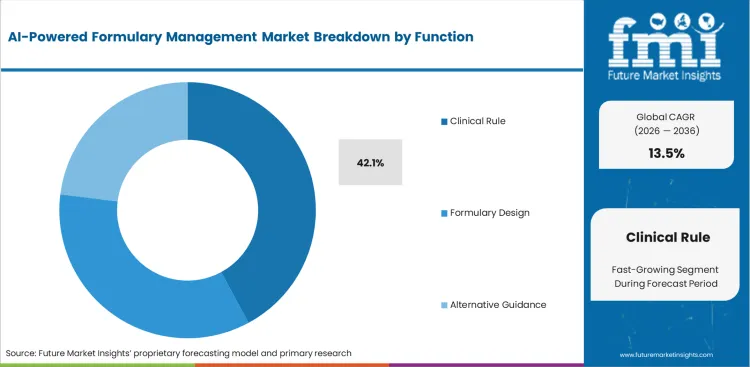
Automating clinical rule verification removes the biggest bottleneck in daily hospital operations. Physicians waste hours every week verifying whether a specific patient's insurance actually covers a prescribed specialty medication. Implementing automated rule-checking engines stops unauthorized prescriptions before they ever reach the pharmacy counter. Artificial intelligence scans patient histories instantly to ensure they meet step-therapy requirements without requiring tedious phone calls to insurance providers. Reducing these administrative delays drastically improves patient care timelines and prevents unexpected out-of-pocket costs. clinical rule checking is poised to garner a 42.1% share in 2026, because it directly solves the most frustrating friction point in the prescribing workflow.
- Unstructured Data Ingestion: Algorithms read and categorize thousands of clinical trial documents autonomously. Formulary strategists eliminate weeks of manual reading and data entry from their workflow.
- Rule Set Generation: Intelligence modules convert complex clinical narratives into binary rules for electronic systems. Clinical pharmacists spend less time debating policy interpretations and more time evaluating patient-specific exceptions.
- Downstream Accuracy Preservation: High-quality benefit intelligence ensures that all subsequent alternative guidance remains clinically sound. Health plan operators prevent catastrophic prescribing errors by securing the foundational data layer first.
AI-Powered Formulary Management Market Analysis by End User
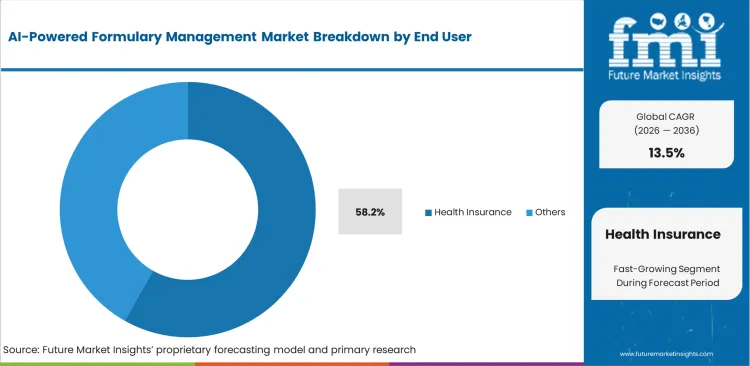
Anticipated to account for a 58.2% share in 2026, health insurance providers rely heavily on artificial intelligence to match complex clinical rules with patient-specific coverage details instantly. Commercial payers face intense pressure to control skyrocketing specialty medication costs across their member networks. Automated tiering allows these organizations to enforce strict rebate negotiations at the point of prescribing rather than catching errors during post-claim audits. Evaluating thousands of new drug applications requires processing power that manual review panels can no longer supply. Integrating these predictive algorithms directly into regional electronic health records prevents costly unauthorized treatments. Organizations failing to adopt automated rule engines quickly lose commercial viability against tech-enabled competitors.
- Contract Enforcement: Algorithms ensure every dispensed medication aligns perfectly with negotiated rebate tiers. Executives eliminate revenue leakage caused by pharmacy-level dispensing variations.
- Scale Execution: Processing millions of daily claims requires automated logic to prevent system bottlenecks. Network coordinators maintain rapid response times at the pharmacy counter despite increasing rule complexity.
- Client Retention: Providing detailed utilization reports proves value to large employer groups. Benefit administrators secure contract renewals by demonstrating clear, algorithmically enforced cost savings.
AI-Powered Formulary Management Market Analysis by Application
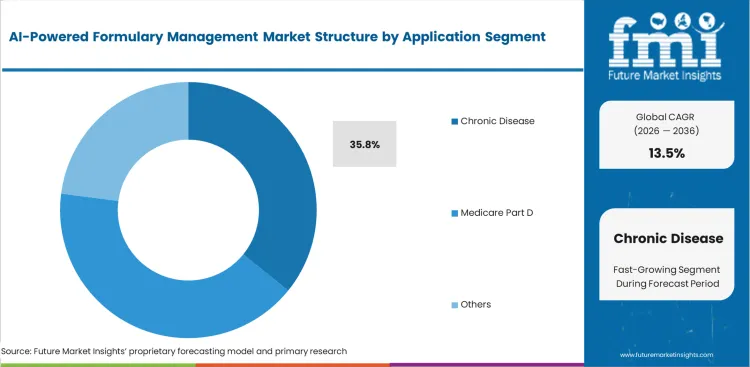
Treating lifelong conditions requires constant medication adjustments that easily overwhelm traditional pharmacy benefit plans. Patients with diabetes or cardiovascular issues frequently switch between expensive specialty drugs as their physical conditions change over time. In 2026, chronic disease management is projected to secure a 35.8% share because health networks must predict and control these long-term pharmaceutical expenses accurately. Algorithms analyze historical claims data to suggest the most cost-effective treatment pathways for chronic patients automatically. Connecting this automated forecasting with population health management tools gives administrators a clear view of future financial risks. Clinics still using manual reviews for chronic care face unpredictable budget overruns every single quarter.
- Scenario Modeling: Algorithms simulate the financial impact of moving specific drugs across different tiers. Formulary strategists present employer groups with accurate cost projections during contract negotiations.
- Customization Speed: Generating a bespoke formulary for a new corporate client takes days rather than months. Health plan operators win competitive bids by demonstrating rapid, flexible benefit design.
- Specialty Drug Containment: Algorithms aggressively steer patients away from high-cost therapeutics when clinically appropriate alternatives exist. Benefit administrators protect employer premiums from unexpected pharmaceutical price spikes.
AI-Powered Formulary Management Market Drivers, Restraints, and Opportunities
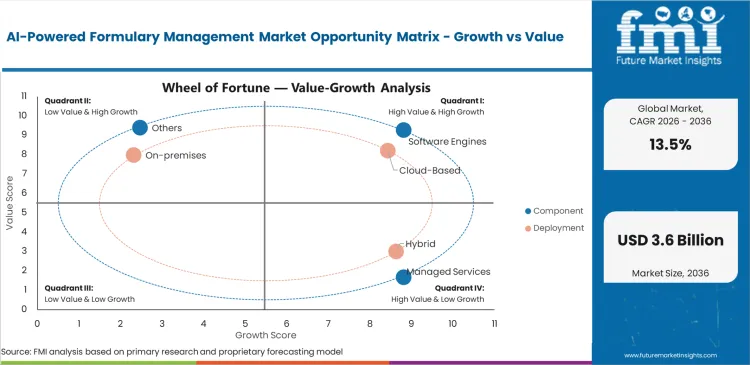
Rapidly changing drug prices force health plans to automate their tiering systems immediately. Manual spreadsheet updates fail to catch daily pricing shifts across thousands of medications, causing significant financial losses. Healthcare networks lose vital negotiating power with pharmaceutical companies when internal data lags behind current market rates. Artificial intelligence instantly processes complex rebate rules and clinical guidelines, aligning approved drug lists with real-time budgets. Hospitals using these automated engines prevent delayed payments and avoid prescribing unapproved, high-cost medications. Automation changes how insurance providers control their pharmacy spending entirely. Replacing outdated quarterly reviews with continuous algorithmic adjustments ensures prescribed treatments always match the most cost-effective coverage options available.
Outdated hospital record systems block the immediate setup of advanced tiering algorithms. Thousands of regional clinics still operate on closed, older databases that simply cannot communicate with modern cloud-based artificial intelligence tools. Connecting these isolated systems requires expensive custom software bridges, delaying active deployment for months. Strict patient privacy regulations complicate this data sharing significantly. Developers must strip all identifying patient information before feeding clinical histories into machine learning models, limiting the predictive accuracy of early setups. Healthcare organizations hesitate to grant external software vendors full access to private claims data. Widespread data fragmentation restricts algorithms from seeing the complete patient history required to make accurate prescribing recommendations.
- Remote Care Integration: Connecting tiering algorithms directly into digital health solutions allows doctors to check drug coverage instantly during online consultations. Physicians avoid prescribing medications that require lengthy prior authorizations, ensuring patients receive treatments without administrative delays.
- Predictive Shortage Alerts: Scanning global supply chain data allows algorithms to identify upcoming medication shortages before they affect local hospitals. Administrators receive automated warnings to switch bulk orders to alternative equivalents, preventing sudden patient care disruptions.
- Chronic Disease Forecasting: Analyzing historical claims data helps health plans predict future medication costs for chronic conditions. Insurance providers adjust yearly budget reserves accurately based on these automated risk profiles rather than relying on outdated demographic estimates.
Regional Analysis
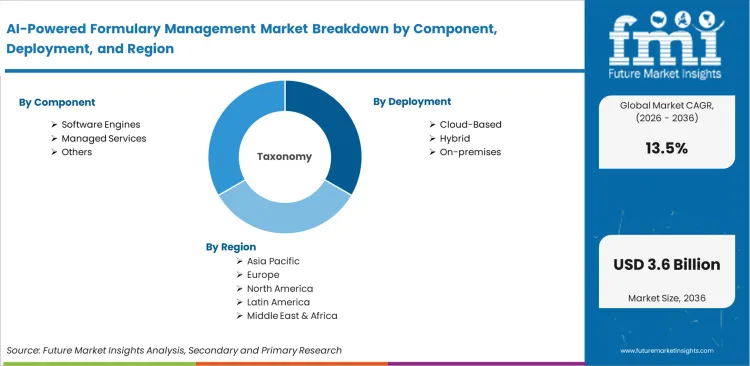
Global adoption of algorithmic tiering relies heavily on existing digital infrastructure and local privacy laws. Regions with centralized prescribing networks adapt quickly to automated workflows, while highly fragmented healthcare systems face longer integration periods. Based on regional analysis, AI-Powered Formulary Management is segmented into North America & Latin America, Europe, Asia-Pacific, and Middle-East across 40 plus countries.
.webp)
| Country | CAGR (2026 to 2036) |
|---|---|
| United States | 13.8% |
| Canada | 12.2% |
| Saudi Arabia | 12.0% |
| United Kingdom | 11.6% |
| Germany | 10.9% |
| Australia | 10.7% |
| Japan | 9.8% |
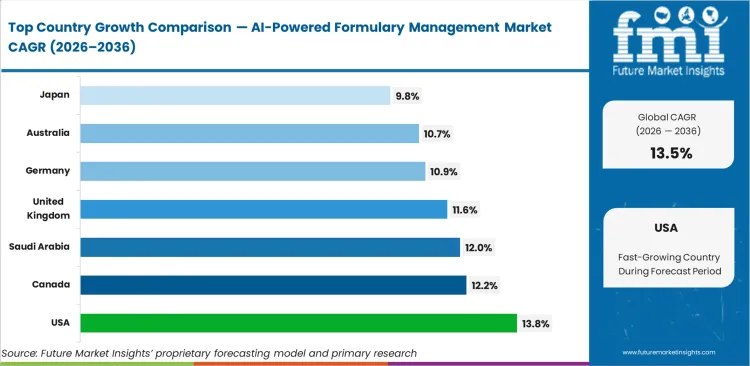
Source: Future Market Insights (FMI) analysis, based on proprietary forecasting model and primary research
North America & Latin America AI-Powered Formulary Management Market Analysis
Extensive electronic prescribing networks shape adoption across this region. Benefit administrators use existing digital setups to send real-time drug tier updates straight to thousands of clinics. AI tools work exceptionally well here because standardized databases already hold decades of patient histories and billing records. Major health plans now fund digital healthcare startups specifically to secure exclusive access to these powerful data engines.
- United States: United States is projected to expand at a CAGR of 13.8% from 2026 to 2036, supported by rising demand for automated formulary and tiering workflows as drug price changes become harder to manage through manual processes. Fragmented commercial insurance structures are likely to reinforce this shift because health plans increasingly rely on digital systems to manage complex benefit design and rebate alignment. Adoption is also expected to strengthen as payers seek greater speed, consistency, and control in coverage administration.
- Canada: Canada is likely to register a CAGR of 12.2% from 2026 to 2036, supported by continued emphasis on cost-effectiveness review across provincial drug coverage systems. Advanced workflow tools are improving review efficiency by helping public health networks process complex therapeutic data with greater consistency. Demand is also being shaped by the need to assess high-cost specialty drugs without placing excessive strain on manual review capacity.
FMI reports, widespread digital maturity makes North America the main testing ground for advanced tiering models. Regional health systems set clear expectations for how fast software can process and update complex drug lists across huge provider networks.
Europe AI-Powered Formulary Management Market Analysis
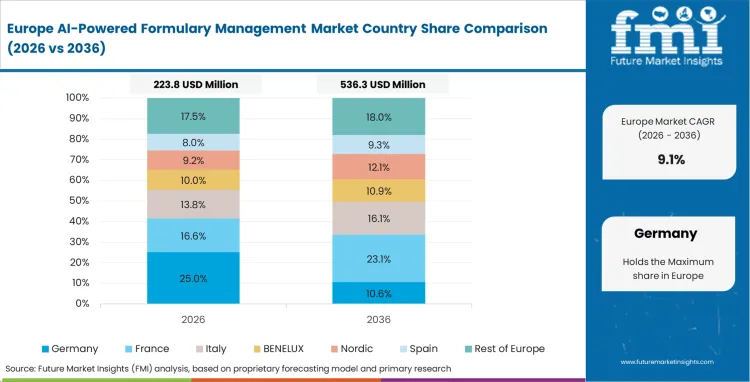
Strict data privacy rules dictate how algorithms process clinical information across European health systems. Compliance officers limit how patient data trains machine learning models, forcing vendors to build highly localized, anonymized intelligence tools. These privacy laws slow down initial software launches but ultimately produce highly secure systems that handle complex national health mandates easily.
- United Kingdom: National Health Service directives mandate strict adherence to standardized clinical guidelines across all trusts. Automated monitoring ensures physicians across different facilities stick to identical tiering protocols without manual oversight. Supported by global digital health initiatives that align regional prescribing habits, demand for algorithmic tiering in the United Kingdom is projected to witness an 11.6% CAGR through 2036.
- Germany: Germany is projected to expand at a CAGR of 10.9% from 2026 to 2036, supported by growing use of automated evidence-gathering systems across statutory health insurance workflows. Documentation requirements around therapeutic exceptions are likely to sustain demand for tools that improve review speed and administrative consistency. Adoption is also being reinforced by the need to reduce reimbursement delays for high-cost treatments across hospital-linked care pathways.
FMI analyses, European deployment focuses heavily on compliance and secure data handling rather than pure commercial speed. Platforms proven effective under these strict data constraints easily adapt to other highly regulated global markets.
Asia-Pacific AI-Powered Formulary Management Market Analysis
Rapid modernization of hospital IT networks pushes algorithmic integration across major Asian health systems. Administrators focus on replacing paper-based pharmacy records with unified digital platforms capable of supporting advanced automation. AI adoption depends almost entirely on securing government funding for foundational electronic health records before sophisticated tiering software can actually function.
- Australia: Australia is projected to expand at a CAGR of 10.7% from 2026 to 2036, supported by strong availability of centralized health data across public drug management systems. Such data depth is likely to improve the performance of clinical decision tools used in subsidy evaluation and formulary review. Adoption is also expected to strengthen as public health systems seek better identification of cost and utilization patterns within large drug coverage programs.
- Japan: Japan is likely to register a CAGR of 9.8% from 2026 to 2036, supported by rising pressure on medication management systems as the population ages and long-term treatment volumes increase. Automation is gaining relevance in chronic care drug tiering because health plans require more efficient ways to manage growing case complexity. Demand is also being reinforced by the need to improve consistency in formulary decisions across high-volume care settings.
FMI assesses, modernization efforts across Asia-Pacific vary wildly depending on national investment in digital health records. Countries with established central databases move quickly into predictive formulary modeling, bypassing older manual spreadsheet workflows entirely.
Middle-East AI-Powered Formulary Management Market Analysis
Sweeping national digitization mandates force immediate architectural upgrades across Middle-Eastern health sectors. Ministry of Health directives require hospitals to adopt unified electronic prescribing standards immediately. This government-driven pressure accelerates the deployment of sophisticated tiering engines, bypassing the slow adoption phases seen in other regions.
- Saudi Arabia: Saudi Arabia is projected to expand at a CAGR of 12.0% from 2026 to 2036, supported by continued digitization across healthcare administration and coverage management systems. AI-enabled tiering tools are likely to gain traction as state-funded insurance programs place greater emphasis on workflow efficiency and rule-based formulary control. Adoption is also expected to strengthen as newer healthcare facilities incorporate automated decision support more directly into prescribing and reimbursement infrastructure.
FMI notes, aggressive government funding allows Middle-Eastern healthcare networks to leapfrog older technologies. Integrating advanced artificial intelligence happens concurrently with basic electronic record rollouts, creating modern infrastructure from day one.
Competitive Aligners for Market Players
Market concentration among leading formulary software providers is raising entry barriers for newer participants. Large pharmacy benefit platforms benefit from broad installed user bases, which strengthens their influence over connectivity expectations across provider and payer networks. Smaller health plans, in many cases, are more likely to rely on outsourced healthcare API connectivity rather than building full internal infrastructure. Such a shift helps them maintain processing efficiency without carrying the full burden of development and integration costs.
Historical claims data remains a central competitive advantage in this market. Established vendors are better positioned to refine predictive models because they operate with broader and more mature clinical data assets. New entrants face a more demanding path, as platform development depends on both functional medication management capability and access to sufficiently reliable clinical data for validation. Vendor selection in formulary management software increasingly reflects confidence in model consistency, data depth, and operational reliability across enterprise-scale deployments.
Healthcare organizations are also placing greater emphasis on interoperability to reduce long-term dependence on a single software provider. Platform selection is increasingly shaped by modular architecture, especially where formulary tools must connect with broader value-based healthcare services and external clinical systems. Limited interoperability can restrict expansion beyond pilot-stage use cases and slow enterprise adoption. Flexible infrastructure, by contrast, is more likely to support wider implementation across complex care and reimbursement environments.
Key Players in AI-Powered Formulary Management Market
- Optum Rx
- CVS Caremark
- Express Scripts by Evernorth
- Surescripts
- DrFirst
- CoverMyMeds
- Arrive Health
Scope of the Report
| Metric | Value |
|---|---|
| Quantitative Units | USD 0.9 billion to USD 3.2 billion, at a CAGR of 13.5% |
| Market Definition | Systems utilizing machine learning to automate drug tiering, ingest clinical evidence, and provide prescribing guidance to optimize healthcare costs and compliance. |
| Segmentation | Component, Deployment, Function, End user, Application |
| Regions Covered | North America & Latin America, Europe, Asia-Pacific, Middle-East |
| Countries Covered | United States, Canada, Saudi Arabia, United Kingdom, Germany, Australia, Japan |
| Key Companies Profiled | Optum Rx, CVS Caremark, Express Scripts by Evernorth, Surescripts, DrFirst, CoverMyMeds, Arrive Health |
| Forecast Period | 2026 to 2036 |
| Approach | Software licensing volumes and managed service contract renewals cross-validated by vendor disclosures. |
Source: Future Market Insights (FMI) analysis, based on proprietary forecasting model and primary research
Segments
Component
- Software platforms
- Implementation services
- Managed services
Deployment
- Cloud-based
- Hybrid
- On-premises
Function
- Benefit intelligence
- Formulary design
- Alternative guidance
- ePA automation
- Utilization analytics
End User
- PBMs
- Health plans
- Health systems
- EHR vendors
- TPAs
Application
- Commercial plans
- Medicare Part D
- Medicaid
- Employer plans
- Specialty drugs
Regions:
- Asia Pacific
- India
- China
- Japan
- South Korea
- Indonesia
- Australia & New Zealand
- ASEAN
- Rest of Asia Pacific
- Europe
- Germany
- Italy
- France
- United Kingdom
- Spain
- Benelux
- Nordics
- Central & Eastern Europe
- Rest of Europe
- North America
- United States
- Canada
- Mexico
- Latin America
- Brazil
- Argentina
- Chile
- Rest of Latin America
- Middle East & Africa
- Kingdom of Saudi Arabia
- United Arab Emirates
- South Africa
- Turkey
- Rest of Middle East & Africa
Bibliography
- Sibbesen, J. B., Trickett, H., & Yzaguirre, S. (2026). An evaluation of six artificial intelligence tools for formulary management. JACCP: Journal of the American College of Clinical Pharmacy.
- Abu-Shraie, N. (2025). Could human pharmacy and therapeutics committees be replaced with artificial intelligence systems? American Journal of Health-System Pharmacy, 82(14), 772–774.
- Preti, L. M., Bazzano, A., Mazzoleni, G., Cagnin, C., & Nante, N. (2024). Implementation of machine learning applications in health care organizations: Systematic review of empirical studies. Journal of Medical Internet Research, 26, e55897.
- Hamishehkar, H., & Shahidi, M. (2025). Impact of artificial intelligence on the future of clinical pharmacy and hospital settings. Journal of Research in Pharmacy Practice, 14(3), 87–97.
- Jessica, H., Tan, E. C. K., Lai, K., & Kalisch-Ellett, L. (2025). Applications of artificial intelligence in current pharmacy practice: A scoping review. Research in Social and Administrative Pharmacy.
This bibliography is provided for reader reference. The full FMI report contains the complete reference list with primary source documentation.
This Report Addresses
- Algorithmic disruption of traditional rebate processing mechanisms across commercial health plans.
- Structural integration of real-time alternative guidance into physician prescribing workflows.
- Financial impact of automated tiering updates on pharmacy benefit operating margins.
- Evaluation of cloud-based infrastructure demands for processing massive daily pharmacy claims.
- Regional divergence in electronic prescribing maturity impacting global software deployment.
- Competitive tactics utilized by established vendors to lock in enterprise health networks.
- Emerging applications of natural language processing for parsing complex employer pricing contracts.
- Qualification requirements for securing hospital IT budgets during systemic modernization phases.
Frequently Asked Questions
What is the projected value of the market in 2036?
Revenue is anticipated to cross USD 3.2 billion by 2036, reflecting massive payer investments to automate complex specialty drug tiering.
What is the expected CAGR for this sector?
Demand is poised to expand at a CAGR of 13.5% as legacy rule engines fail to process clinical data efficiently.
Which component segment leads adoption?
Software platforms are estimated to account for 62% share in 2026 because foundational algorithms represent the core operational requirement for payers.
Why do cloud-based deployments dominate?
The cloud-based category holds 68% share because ensuring immediate interoperability across thousands of clinics is impossible on isolated servers.
What function commands the highest share?
Benefit intelligence captures 34% share because ingesting unstructured clinical data remains the most labor-intensive bottleneck in policy administration.
Which end user dictates market direction?
PBMs are set to represent 39% share as they leverage algorithmic efficiency to process billions of pharmacy claims annually.
Which application segment is growing fastest?
Commercial plans account for 36% share due to competitive pressures demanding highly customized benefit designs for employer groups.
How fast is the United States adopting these tools?
United States adoption scales at 13.8% CAGR, driven directly by highly fragmented commercial insurance networks forcing rapid algorithmic deployment.
What limits adoption in smaller health networks?
Integrating complex employer pricing contracts into standard algorithmic logic creates severe operational friction that smaller IT budgets struggle to resolve.
How do European privacy laws impact software architecture?
Compliance officers strictly limit how patient data trains machine learning models, forcing vendors to develop highly localized intelligence tools.
Why is Canada upgrading its infrastructure?
Provincial health authorities demand rigorous cost-effectiveness data, driving a 12.2% CAGR as administrators parse this data algorithmically.
What accelerates Middle-Eastern integration?
Sweeping national digitization mandates compel immediate architectural upgrades across hospitals, resulting in a 12.0% CAGR in Saudi Arabia.
How do algorithms influence point-of-prescribing behavior?
Making alternative guidance visible immediately reduces administrative friction and fundamentally alters how physicians select initial therapies.
Why do mid-sized health plans struggle to compete independently?
They lack the vast troves of historical claims data necessary to train predictive models as accurately as the established market giants.
How do hospitals resist vendor lock-in?
Network coordinators aggressively demand open application programming interfaces and modular software architectures during contract negotiations.
What role does real-world evidence play in tiering?
Pharmacy network leads utilize algorithms analyzing real world evidence solutions to validate tier placement and gain negotiating leverage.
Why do some purely clinical vendors fail during pilot phases?
They focus entirely on clinical accuracy while failing to parse the highly customized pricing agreements that actually govern health plan economics.
How does automated tiering reduce grievance expenses?
Replacing static spreadsheets with dynamic intelligence ensures policies remain accurate, drastically lowering the volume of provider appeals.
What drives adoption in Japan?
Aging populations strain traditional architectures, forcing health plan operators to automate chronic care drug tiering to manage the demographic shift.
How do PBMs utilize AI for contract enforcement?
Algorithms ensure every dispensed medication aligns perfectly with negotiated rebate tiers, eliminating revenue leakage at the pharmacy counter.
Why do commercial plans require rapid scenario modeling?
Generating a bespoke formulary quickly allows insurers to present accurate cost projections and win lucrative corporate contracts during bidding.
What is the primary constraint holding back fully automated contracting?
True semantic understanding of customized legal agreements remains a significant technological hurdle for current natural language processing models.
How does cloud architecture prevent manual prescribing errors?
Pushing drug tier changes through cloud networks updates every connected physician instantly, eliminating the dangerous lag time of manual system revisions.
What changes structurally for clinical pharmacists post-implementation?
Incorporating advanced software shifts their operational burden away from routine tiering assignments, allowing focus entirely on complex patient appeals.
Table of Content
- Executive Summary
- Global Market Outlook
- Demand to side Trends
- Supply to side Trends
- Technology Roadmap Analysis
- Analysis and Recommendations
- Market Overview
- Market Coverage / Taxonomy
- Market Definition / Scope / Limitations
- Research Methodology
- Chapter Orientation
- Analytical Lens and Working Hypotheses
- Market Structure, Signals, and Trend Drivers
- Benchmarking and Cross-market Comparability
- Market Sizing, Forecasting, and Opportunity Mapping
- Research Design and Evidence Framework
- Desk Research Programme (Secondary Evidence)
- Company Annual and Sustainability Reports
- Peer-reviewed Journals and Academic Literature
- Corporate Websites, Product Literature, and Technical Notes
- Earnings Decks and Investor Briefings
- Statutory Filings and Regulatory Disclosures
- Technical White Papers and Standards Notes
- Trade Journals, Industry Magazines, and Analyst Briefs
- Conference Proceedings, Webinars, and Seminar Materials
- Government Statistics Portals and Public Data Releases
- Press Releases and Reputable Media Coverage
- Specialist Newsletters and Curated Briefings
- Sector Databases and Reference Repositories
- FMI Internal Proprietary Databases and Historical Market Datasets
- Subscription Datasets and Paid Sources
- Social Channels, Communities, and Digital Listening Inputs
- Additional Desk Sources
- Expert Input and Fieldwork (Primary Evidence)
- Primary Modes
- Qualitative Interviews and Expert Elicitation
- Quantitative Surveys and Structured Data Capture
- Blended Approach
- Why Primary Evidence is Used
- Field Techniques
- Interviews
- Surveys
- Focus Groups
- Observational and In-context Research
- Social and Community Interactions
- Stakeholder Universe Engaged
- C-suite Leaders
- Board Members
- Presidents and Vice Presidents
- R&D and Innovation Heads
- Technical Specialists
- Domain Subject-matter Experts
- Scientists
- Physicians and Other Healthcare Professionals
- Governance, Ethics, and Data Stewardship
- Research Ethics
- Data Integrity and Handling
- Primary Modes
- Tooling, Models, and Reference Databases
- Desk Research Programme (Secondary Evidence)
- Data Engineering and Model Build
- Data Acquisition and Ingestion
- Cleaning, Normalisation, and Verification
- Synthesis, Triangulation, and Analysis
- Quality Assurance and Audit Trail
- Market Background
- Market Dynamics
- Drivers
- Restraints
- Opportunity
- Trends
- Scenario Forecast
- Demand in Optimistic Scenario
- Demand in Likely Scenario
- Demand in Conservative Scenario
- Opportunity Map Analysis
- Product Life Cycle Analysis
- Supply Chain Analysis
- Investment Feasibility Matrix
- Value Chain Analysis
- PESTLE and Porter’s Analysis
- Regulatory Landscape
- Regional Parent Market Outlook
- Production and Consumption Statistics
- Import and Export Statistics
- Market Dynamics
- Global Market Analysis 2021 to 2025 and Forecast, 2026 to 2036
- Historical Market Size Value (USD Million) Analysis, 2021 to 2025
- Current and Future Market Size Value (USD Million) Projections, 2026 to 2036
- Y to o to Y Growth Trend Analysis
- Absolute $ Opportunity Analysis
- Global Market Pricing Analysis 2021 to 2025 and Forecast 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Component
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Component , 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Component , 2026 to 2036
- Software Engines
- Managed Services
- Others
- Software Engines
- Y to o to Y Growth Trend Analysis By Component , 2021 to 2025
- Absolute $ Opportunity Analysis By Component , 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Deployment
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Deployment, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Deployment, 2026 to 2036
- Cloud-Based
- Hybrid
- On-premises
- Cloud-Based
- Y to o to Y Growth Trend Analysis By Deployment, 2021 to 2025
- Absolute $ Opportunity Analysis By Deployment, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Function
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Function, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Function, 2026 to 2036
- Clinical Rule
- Formulary Design
- Alternative Guidance
- Clinical Rule
- Y to o to Y Growth Trend Analysis By Function, 2021 to 2025
- Absolute $ Opportunity Analysis By Function, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By End User
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By End User, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By End User, 2026 to 2036
- Health Insurance
- Others
- Health Insurance
- Y to o to Y Growth Trend Analysis By End User, 2021 to 2025
- Absolute $ Opportunity Analysis By End User, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Application
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Application, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Application, 2026 to 2036
- Chronic Disease
- Medicare Part D
- Others
- Chronic Disease
- Y to o to Y Growth Trend Analysis By Application, 2021 to 2025
- Absolute $ Opportunity Analysis By Application, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Region
- Introduction
- Historical Market Size Value (USD Million) Analysis By Region, 2021 to 2025
- Current Market Size Value (USD Million) Analysis and Forecast By Region, 2026 to 2036
- North America
- Latin America
- Western Europe
- Eastern Europe
- East Asia
- South Asia and Pacific
- Middle East & Africa
- Market Attractiveness Analysis By Region
- North America Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- USA
- Canada
- Mexico
- By Component
- By Deployment
- By Function
- By End User
- By Application
- By Country
- Market Attractiveness Analysis
- By Country
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Key Takeaways
- Latin America Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Brazil
- Chile
- Rest of Latin America
- By Component
- By Deployment
- By Function
- By End User
- By Application
- By Country
- Market Attractiveness Analysis
- By Country
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Key Takeaways
- Western Europe Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Germany
- UK
- Italy
- Spain
- France
- Nordic
- BENELUX
- Rest of Western Europe
- By Component
- By Deployment
- By Function
- By End User
- By Application
- By Country
- Market Attractiveness Analysis
- By Country
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Key Takeaways
- Eastern Europe Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Russia
- Poland
- Hungary
- Balkan & Baltic
- Rest of Eastern Europe
- By Component
- By Deployment
- By Function
- By End User
- By Application
- By Country
- Market Attractiveness Analysis
- By Country
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Key Takeaways
- East Asia Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- China
- Japan
- South Korea
- By Component
- By Deployment
- By Function
- By End User
- By Application
- By Country
- Market Attractiveness Analysis
- By Country
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Key Takeaways
- South Asia and Pacific Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- India
- ASEAN
- Australia & New Zealand
- Rest of South Asia and Pacific
- By Component
- By Deployment
- By Function
- By End User
- By Application
- By Country
- Market Attractiveness Analysis
- By Country
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Key Takeaways
- Middle East & Africa Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Kingdom of Saudi Arabia
- Other GCC Countries
- Turkiye
- South Africa
- Other African Union
- Rest of Middle East & Africa
- By Component
- By Deployment
- By Function
- By End User
- By Application
- By Country
- Market Attractiveness Analysis
- By Country
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Key Takeaways
- Key Countries Market Analysis
- USA
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Canada
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Mexico
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Brazil
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Chile
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Germany
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- UK
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Italy
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Spain
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- France
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- India
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- ASEAN
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Australia & New Zealand
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- China
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Japan
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- South Korea
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Russia
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Poland
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Hungary
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Kingdom of Saudi Arabia
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Turkiye
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- South Africa
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By Function
- By End User
- By Application
- USA
- Market Structure Analysis
- Competition Dashboard
- Competition Benchmarking
- Market Share Analysis of Top Players
- By Regional
- By Component
- By Deployment
- By Function
- By End User
- By Application
- Competition Analysis
- Competition Deep Dive
- Optum Rx
- Overview
- Product Portfolio
- Profitability by Market Segments (Product/Age /Sales Channel/Region)
- Sales Footprint
- Strategy Overview
- Marketing Strategy
- Product Strategy
- Channel Strategy
- CVS Caremark
- Express Scripts by Evernorth
- Surescripts
- DrFirst
- CoverMyMeds
- Arrive Health
- Optum Rx
- Competition Deep Dive
- Assumptions & Acronyms Used
List of Tables
- Table 1: Global Market Value (USD Million) Forecast by Region, 2021 to 2036
- Table 2: Global Market Value (USD Million) Forecast by Component , 2021 to 2036
- Table 3: Global Market Value (USD Million) Forecast by Deployment, 2021 to 2036
- Table 4: Global Market Value (USD Million) Forecast by Function, 2021 to 2036
- Table 5: Global Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 6: Global Market Value (USD Million) Forecast by Application, 2021 to 2036
- Table 7: North America Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 8: North America Market Value (USD Million) Forecast by Component , 2021 to 2036
- Table 9: North America Market Value (USD Million) Forecast by Deployment, 2021 to 2036
- Table 10: North America Market Value (USD Million) Forecast by Function, 2021 to 2036
- Table 11: North America Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 12: North America Market Value (USD Million) Forecast by Application, 2021 to 2036
- Table 13: Latin America Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 14: Latin America Market Value (USD Million) Forecast by Component , 2021 to 2036
- Table 15: Latin America Market Value (USD Million) Forecast by Deployment, 2021 to 2036
- Table 16: Latin America Market Value (USD Million) Forecast by Function, 2021 to 2036
- Table 17: Latin America Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 18: Latin America Market Value (USD Million) Forecast by Application, 2021 to 2036
- Table 19: Western Europe Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 20: Western Europe Market Value (USD Million) Forecast by Component , 2021 to 2036
- Table 21: Western Europe Market Value (USD Million) Forecast by Deployment, 2021 to 2036
- Table 22: Western Europe Market Value (USD Million) Forecast by Function, 2021 to 2036
- Table 23: Western Europe Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 24: Western Europe Market Value (USD Million) Forecast by Application, 2021 to 2036
- Table 25: Eastern Europe Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 26: Eastern Europe Market Value (USD Million) Forecast by Component , 2021 to 2036
- Table 27: Eastern Europe Market Value (USD Million) Forecast by Deployment, 2021 to 2036
- Table 28: Eastern Europe Market Value (USD Million) Forecast by Function, 2021 to 2036
- Table 29: Eastern Europe Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 30: Eastern Europe Market Value (USD Million) Forecast by Application, 2021 to 2036
- Table 31: East Asia Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 32: East Asia Market Value (USD Million) Forecast by Component , 2021 to 2036
- Table 33: East Asia Market Value (USD Million) Forecast by Deployment, 2021 to 2036
- Table 34: East Asia Market Value (USD Million) Forecast by Function, 2021 to 2036
- Table 35: East Asia Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 36: East Asia Market Value (USD Million) Forecast by Application, 2021 to 2036
- Table 37: South Asia and Pacific Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 38: South Asia and Pacific Market Value (USD Million) Forecast by Component , 2021 to 2036
- Table 39: South Asia and Pacific Market Value (USD Million) Forecast by Deployment, 2021 to 2036
- Table 40: South Asia and Pacific Market Value (USD Million) Forecast by Function, 2021 to 2036
- Table 41: South Asia and Pacific Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 42: South Asia and Pacific Market Value (USD Million) Forecast by Application, 2021 to 2036
- Table 43: Middle East & Africa Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 44: Middle East & Africa Market Value (USD Million) Forecast by Component , 2021 to 2036
- Table 45: Middle East & Africa Market Value (USD Million) Forecast by Deployment, 2021 to 2036
- Table 46: Middle East & Africa Market Value (USD Million) Forecast by Function, 2021 to 2036
- Table 47: Middle East & Africa Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 48: Middle East & Africa Market Value (USD Million) Forecast by Application, 2021 to 2036
List of Figures
- Figure 1: Global Market Pricing Analysis
- Figure 2: Global Market Value (USD Million) Forecast 2021-2036
- Figure 3: Global Market Value Share and BPS Analysis by Component , 2026 and 2036
- Figure 4: Global Market Y-o-Y Growth Comparison by Component , 2026-2036
- Figure 5: Global Market Attractiveness Analysis by Component
- Figure 6: Global Market Value Share and BPS Analysis by Deployment, 2026 and 2036
- Figure 7: Global Market Y-o-Y Growth Comparison by Deployment, 2026-2036
- Figure 8: Global Market Attractiveness Analysis by Deployment
- Figure 9: Global Market Value Share and BPS Analysis by Function, 2026 and 2036
- Figure 10: Global Market Y-o-Y Growth Comparison by Function, 2026-2036
- Figure 11: Global Market Attractiveness Analysis by Function
- Figure 12: Global Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 13: Global Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 14: Global Market Attractiveness Analysis by End User
- Figure 15: Global Market Value Share and BPS Analysis by Application, 2026 and 2036
- Figure 16: Global Market Y-o-Y Growth Comparison by Application, 2026-2036
- Figure 17: Global Market Attractiveness Analysis by Application
- Figure 18: Global Market Value (USD Million) Share and BPS Analysis by Region, 2026 and 2036
- Figure 19: Global Market Y-o-Y Growth Comparison by Region, 2026-2036
- Figure 20: Global Market Attractiveness Analysis by Region
- Figure 21: North America Market Incremental Dollar Opportunity, 2026-2036
- Figure 22: Latin America Market Incremental Dollar Opportunity, 2026-2036
- Figure 23: Western Europe Market Incremental Dollar Opportunity, 2026-2036
- Figure 24: Eastern Europe Market Incremental Dollar Opportunity, 2026-2036
- Figure 25: East Asia Market Incremental Dollar Opportunity, 2026-2036
- Figure 26: South Asia and Pacific Market Incremental Dollar Opportunity, 2026-2036
- Figure 27: Middle East & Africa Market Incremental Dollar Opportunity, 2026-2036
- Figure 28: North America Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 29: North America Market Value Share and BPS Analysis by Component , 2026 and 2036
- Figure 30: North America Market Y-o-Y Growth Comparison by Component , 2026-2036
- Figure 31: North America Market Attractiveness Analysis by Component
- Figure 32: North America Market Value Share and BPS Analysis by Deployment, 2026 and 2036
- Figure 33: North America Market Y-o-Y Growth Comparison by Deployment, 2026-2036
- Figure 34: North America Market Attractiveness Analysis by Deployment
- Figure 35: North America Market Value Share and BPS Analysis by Function, 2026 and 2036
- Figure 36: North America Market Y-o-Y Growth Comparison by Function, 2026-2036
- Figure 37: North America Market Attractiveness Analysis by Function
- Figure 38: North America Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 39: North America Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 40: North America Market Attractiveness Analysis by End User
- Figure 41: North America Market Value Share and BPS Analysis by Application, 2026 and 2036
- Figure 42: North America Market Y-o-Y Growth Comparison by Application, 2026-2036
- Figure 43: North America Market Attractiveness Analysis by Application
- Figure 44: Latin America Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 45: Latin America Market Value Share and BPS Analysis by Component , 2026 and 2036
- Figure 46: Latin America Market Y-o-Y Growth Comparison by Component , 2026-2036
- Figure 47: Latin America Market Attractiveness Analysis by Component
- Figure 48: Latin America Market Value Share and BPS Analysis by Deployment, 2026 and 2036
- Figure 49: Latin America Market Y-o-Y Growth Comparison by Deployment, 2026-2036
- Figure 50: Latin America Market Attractiveness Analysis by Deployment
- Figure 51: Latin America Market Value Share and BPS Analysis by Function, 2026 and 2036
- Figure 52: Latin America Market Y-o-Y Growth Comparison by Function, 2026-2036
- Figure 53: Latin America Market Attractiveness Analysis by Function
- Figure 54: Latin America Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 55: Latin America Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 56: Latin America Market Attractiveness Analysis by End User
- Figure 57: Latin America Market Value Share and BPS Analysis by Application, 2026 and 2036
- Figure 58: Latin America Market Y-o-Y Growth Comparison by Application, 2026-2036
- Figure 59: Latin America Market Attractiveness Analysis by Application
- Figure 60: Western Europe Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 61: Western Europe Market Value Share and BPS Analysis by Component , 2026 and 2036
- Figure 62: Western Europe Market Y-o-Y Growth Comparison by Component , 2026-2036
- Figure 63: Western Europe Market Attractiveness Analysis by Component
- Figure 64: Western Europe Market Value Share and BPS Analysis by Deployment, 2026 and 2036
- Figure 65: Western Europe Market Y-o-Y Growth Comparison by Deployment, 2026-2036
- Figure 66: Western Europe Market Attractiveness Analysis by Deployment
- Figure 67: Western Europe Market Value Share and BPS Analysis by Function, 2026 and 2036
- Figure 68: Western Europe Market Y-o-Y Growth Comparison by Function, 2026-2036
- Figure 69: Western Europe Market Attractiveness Analysis by Function
- Figure 70: Western Europe Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 71: Western Europe Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 72: Western Europe Market Attractiveness Analysis by End User
- Figure 73: Western Europe Market Value Share and BPS Analysis by Application, 2026 and 2036
- Figure 74: Western Europe Market Y-o-Y Growth Comparison by Application, 2026-2036
- Figure 75: Western Europe Market Attractiveness Analysis by Application
- Figure 76: Eastern Europe Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 77: Eastern Europe Market Value Share and BPS Analysis by Component , 2026 and 2036
- Figure 78: Eastern Europe Market Y-o-Y Growth Comparison by Component , 2026-2036
- Figure 79: Eastern Europe Market Attractiveness Analysis by Component
- Figure 80: Eastern Europe Market Value Share and BPS Analysis by Deployment, 2026 and 2036
- Figure 81: Eastern Europe Market Y-o-Y Growth Comparison by Deployment, 2026-2036
- Figure 82: Eastern Europe Market Attractiveness Analysis by Deployment
- Figure 83: Eastern Europe Market Value Share and BPS Analysis by Function, 2026 and 2036
- Figure 84: Eastern Europe Market Y-o-Y Growth Comparison by Function, 2026-2036
- Figure 85: Eastern Europe Market Attractiveness Analysis by Function
- Figure 86: Eastern Europe Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 87: Eastern Europe Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 88: Eastern Europe Market Attractiveness Analysis by End User
- Figure 89: Eastern Europe Market Value Share and BPS Analysis by Application, 2026 and 2036
- Figure 90: Eastern Europe Market Y-o-Y Growth Comparison by Application, 2026-2036
- Figure 91: Eastern Europe Market Attractiveness Analysis by Application
- Figure 92: East Asia Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 93: East Asia Market Value Share and BPS Analysis by Component , 2026 and 2036
- Figure 94: East Asia Market Y-o-Y Growth Comparison by Component , 2026-2036
- Figure 95: East Asia Market Attractiveness Analysis by Component
- Figure 96: East Asia Market Value Share and BPS Analysis by Deployment, 2026 and 2036
- Figure 97: East Asia Market Y-o-Y Growth Comparison by Deployment, 2026-2036
- Figure 98: East Asia Market Attractiveness Analysis by Deployment
- Figure 99: East Asia Market Value Share and BPS Analysis by Function, 2026 and 2036
- Figure 100: East Asia Market Y-o-Y Growth Comparison by Function, 2026-2036
- Figure 101: East Asia Market Attractiveness Analysis by Function
- Figure 102: East Asia Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 103: East Asia Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 104: East Asia Market Attractiveness Analysis by End User
- Figure 105: East Asia Market Value Share and BPS Analysis by Application, 2026 and 2036
- Figure 106: East Asia Market Y-o-Y Growth Comparison by Application, 2026-2036
- Figure 107: East Asia Market Attractiveness Analysis by Application
- Figure 108: South Asia and Pacific Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 109: South Asia and Pacific Market Value Share and BPS Analysis by Component , 2026 and 2036
- Figure 110: South Asia and Pacific Market Y-o-Y Growth Comparison by Component , 2026-2036
- Figure 111: South Asia and Pacific Market Attractiveness Analysis by Component
- Figure 112: South Asia and Pacific Market Value Share and BPS Analysis by Deployment, 2026 and 2036
- Figure 113: South Asia and Pacific Market Y-o-Y Growth Comparison by Deployment, 2026-2036
- Figure 114: South Asia and Pacific Market Attractiveness Analysis by Deployment
- Figure 115: South Asia and Pacific Market Value Share and BPS Analysis by Function, 2026 and 2036
- Figure 116: South Asia and Pacific Market Y-o-Y Growth Comparison by Function, 2026-2036
- Figure 117: South Asia and Pacific Market Attractiveness Analysis by Function
- Figure 118: South Asia and Pacific Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 119: South Asia and Pacific Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 120: South Asia and Pacific Market Attractiveness Analysis by End User
- Figure 121: South Asia and Pacific Market Value Share and BPS Analysis by Application, 2026 and 2036
- Figure 122: South Asia and Pacific Market Y-o-Y Growth Comparison by Application, 2026-2036
- Figure 123: South Asia and Pacific Market Attractiveness Analysis by Application
- Figure 124: Middle East & Africa Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 125: Middle East & Africa Market Value Share and BPS Analysis by Component , 2026 and 2036
- Figure 126: Middle East & Africa Market Y-o-Y Growth Comparison by Component , 2026-2036
- Figure 127: Middle East & Africa Market Attractiveness Analysis by Component
- Figure 128: Middle East & Africa Market Value Share and BPS Analysis by Deployment, 2026 and 2036
- Figure 129: Middle East & Africa Market Y-o-Y Growth Comparison by Deployment, 2026-2036
- Figure 130: Middle East & Africa Market Attractiveness Analysis by Deployment
- Figure 131: Middle East & Africa Market Value Share and BPS Analysis by Function, 2026 and 2036
- Figure 132: Middle East & Africa Market Y-o-Y Growth Comparison by Function, 2026-2036
- Figure 133: Middle East & Africa Market Attractiveness Analysis by Function
- Figure 134: Middle East & Africa Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 135: Middle East & Africa Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 136: Middle East & Africa Market Attractiveness Analysis by End User
- Figure 137: Middle East & Africa Market Value Share and BPS Analysis by Application, 2026 and 2036
- Figure 138: Middle East & Africa Market Y-o-Y Growth Comparison by Application, 2026-2036
- Figure 139: Middle East & Africa Market Attractiveness Analysis by Application
- Figure 140: Global Market - Tier Structure Analysis
- Figure 141: Global Market - Company Share Analysis

