Imaging Interoperability Middleware Market : Global Industry Analysis 2016 - 2025 and Opportunity Assessment 2026 - 2036
The Imaging Interoperability Middleware Market is segmented by Component (Software, Services), Deployment (Cloud-based, On-premise, Hybrid), End User (Hospitals, Diagnostic Imaging Centers, Ambulatory Surgical Centers), Application (Clinical Imaging, Non-clinical Data Management), and Region. Forecast for 2026 to 2036.
Historical Data Covered: 2016 - 2025 | Base Year: 2025 | Estimated Year: 2026 | Forecast Period: 2026 - 2036
Imaging Interoperability Middleware Market Size, Market Forecast and Outlook By FMI
The imaging interoperability middleware market was valued at USD 4.6 billion in 2025 and is projected to reach USD 4.9 billion in 2026, reflecting a CAGR of 7.12%. Continued investment is expected to drive the market to USD 9.8 billion by 2036, as multi‑site health systems adopt API‑driven architectures to decouple image viewers from legacy storage systems and eliminate proprietary departmental silos.
The shift toward RESTful API-based, vendor-neutral middleware actively dismantles legacy Picture Archiving and Communication Systems (PACS) routing protocols. Multi-site hospital networks face severe integration bottlenecks following mergers and acquisitions, forcing enterprise IT directors to implement advanced healthcare interoperability framework systems. Organizations that delay this transition lose millions in duplicate storage costs and suffer degraded diagnostic throughput. The hidden friction in this ecosystem revolves entirely around reconciling disparate patient identity markers and normalizing proprietary metadata tags before images reach the diagnostic viewer.
Summary of Imaging Interoperability Middleware Market
- Imaging Interoperability Middleware Market Definition
- This market comprises the software and services that translate, normalize, and route clinical imaging data across disparate IT systems. It structurally decouples image storage from diagnostic viewers using API-driven standards.
- Demand Drivers in the Market
- The Fast Healthcare Interoperability Resources (FHIR) R4 mandate forces enterprise IT directors to implement standardized data exchange layers across fragmented hospital networks.
- Referring physician demand for instant, zero-footprint image access compels diagnostic imaging center managers to deploy cloud-native exchange software.
- Stringent pre-operative planning requirements drive ambulatory surgical center administrators to install lightweight interoperability nodes to avoid surgical delays.
- Key Segments Analyzed in the FMI Report
- Software: 61.4% share in 2026, driven by continuous licensing models tied directly to algorithm-based metadata normalization engines.
- Cloud-based: 55.0% share in 2026, advancing as elastic storage requirements outpace the capital expenditure limits of on-premises hospital data centers.
- Hospitals: 41.7% share in 2026, dominating the user base due to immense pressure to consolidate diagnostic workflows following aggressive health system consolidations.
- China: 9.5% compound growth, propelled by strict national mandates to build interconnected medical centers that distribute diagnostic workloads out of tier-3 cities.
- Analyst Opinion at FMI
- Sabyasachi Ghosh, Principal Analyst, Healthcare, says, "The primary challenge lies not in transferring large imaging files, but in accurately reconciling fragmented patient identities and proprietary metadata across diverse network environments. Vendors that cannot deliver reliable, real‑time metadata normalization will encounter significant integration delays and risk losing enterprise contracts to competitors offering seamless, cross‑platform interoperability."
- Strategic Implications / Executive Takeaways
- Multi-site hospital CIOs must decouple legacy viewer applications from underlying storage archives to eliminate millions in duplicate storage costs before the next major acquisition cycle.
- Diagnostic imaging center operators should implement vendor-agnostic routing software to capture higher referral volumes from independent physician practices.
- Imaging IT vendors must natively integrate AI-driven patient identity reconciliation engines or face immediate disqualification during large-scale enterprise imaging procurement events.
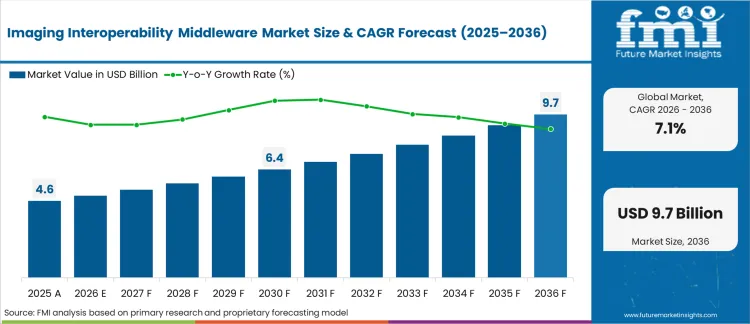
Widespread adoption fundamentally accelerates when major cloud providers natively embed FHIR-compliant imaging ingestion engines into their core infrastructure. Legacy PACS administrators must abandon local, on-premises routing updates within a tight 36-month window to remain compliant with data exchange mandates. This structural shift ensures that advanced middleware becomes the permanent, foundational layer for all future clinical visualizations.
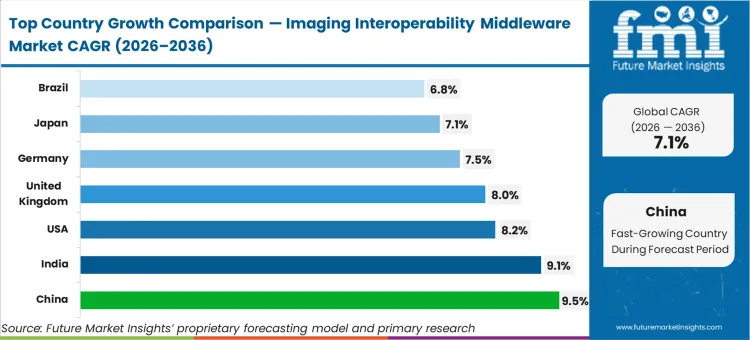
China records a 9.5% CAGR, followed closely by India expanding at 9.1% and the United States advancing at 8.2%. The United Kingdom tracks 8.0% compound growth, while Germany posts a 7.5% rate. Japan grows at 7.1%, and Brazil reaches a 6.8% CAGR. China’s accelerated trajectory stems directly from the National Health Commission's mandate to establish regional interconnected medical centers, which requires immediate provincial-level image-sharing networks to balance diagnostic workloads across urban and rural tiers.
Imaging Interoperability Middleware Market Definition
Imaging interoperability middleware functions as the translation and orchestration layer sitting between disparate medical imaging generation devices, storage repositories, and diagnostic viewing platforms. It standardises both DICOM and non-DICOM visual objects using RESTful APIs and FHIR standards. This technology decouples the image acquisition hardware from the long-term archiving environment, actively normalising metadata and patient identifiers to ensure seamless, real-time data flow across completely heterogeneous healthcare IT environments.
Imaging Interoperability Middleware Market Inclusions
This sector includes independent clinical data routing engines, patient identity reconciliation software, metadata normalization algorithms, and API-based image streaming gateways. It specifically encompasses middleware applications designed to integrate specialty diagnostic formats with broader vendor-neutral archives. Implementation consulting, ongoing managed interoperability services, and hybrid cloud orchestration platforms dedicated to clinical imaging workloads are also thoroughly evaluated.
Imaging Interoperability Middleware Market Exclusions
Primary diagnostic modalities such as MRI or CT scanning hardware are excluded from this analysis. Standalone legacy PACS solutions that lack independent, agnostic routing capabilities are out of scope. General-purpose electronic health record (EHR) software and generalized enterprise storage hardware, while adjacent to the workflow, are omitted because they do not specifically perform the complex image metadata translation required for medical-grade visual interoperability.
Imaging Interoperability Middleware Market Research Methodology
- Primary Research: FMI analysts engaged extensively with Chief Medical Information Officers (CMIOs), enterprise imaging directors, and radiology informatics leads across tier-1 and tier-2 hospital networks.
- Desk Research: The data synthesis aggregated technical compliance documentation from the ONC, European Health Data Space (EHDS) regulatory filings, and HL7 FHIR implementation registries.
- Market-Sizing and Forecasting: The baseline derives from cross-referencing global hospital M&A IT integration budgets with historical replacement cycles of legacy departmental silos, applying non-linear adoption curves for cloud-based routing software.
- Data Validation and Update Cycle: Projections were cross-validated using publicly disclosed cloud integration contracts from leading healthcare IT vendors and specialised vendor-neutral architecture RFPs.
Imaging Interoperability Middleware Market Key Takeaways
| Metric | Details |
|---|---|
| Industry Size (2026) | USD 4.9 billion |
| Industry Value (2036) | USD 9.8 billion |
| CAGR (2026-2036) | 7.12% |
Source: Future Market Insights (FMI) analysis, based on a proprietary forecasting model and primary research
Segmental Analysis
Imaging Interoperability Middleware Market Analysis by Component
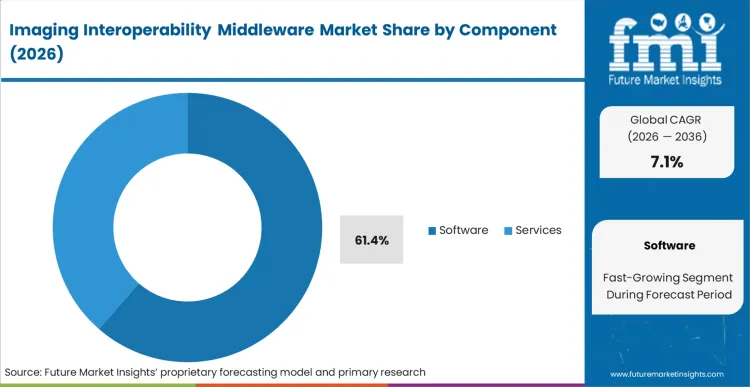
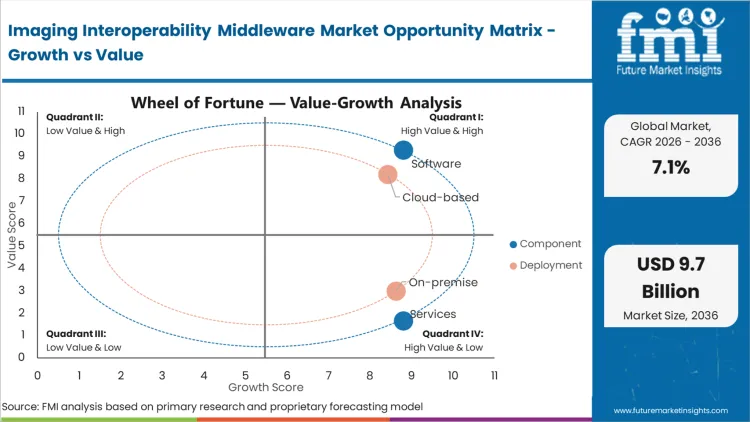
Legacy monolithic systems are rapidly failing modern healthcare networks, dictating the aggressive shift toward independent software engines that natively untangle proprietary data formats. Software holds a dominant 61.4% share in 2026 because the core complexity of image exchange relies entirely on algorithmic metadata normalisation rather than hardware routing. Enterprise imaging directors mandate these virtualized software layers to ensure that all DICOM and non-DICOM objects stream seamlessly, irrespective of the underlying physical storage infrastructure.
FMI analysts opine that recurring software licensing models, particularly those based on transaction volume, secure long-term vendor revenue stability. As hospital networks expand, IT administrators who delay software-defined interoperability upgrades face critical failures in integrating newly acquired clinical facilities into their primary picture archiving architectures.
- Algorithmic translation: Dynamic tag morphing automatically aligns mismatched proprietary metadata from disparate modalities into unified HL7 FHIR standards. Health system CIOs utilizing this engine eliminate the need for manual data reconciliation during hospital acquisitions.
- Identity reconciliation: Master Patient Index (MPI) integration tools actively scan incoming image streams to resolve duplicate or conflicting patient records in real-time. Informatics directors deploying this module prevent life-threatening diagnostic errors caused by mismatched patient histories.
- Protocol bridging: Specialized API gateways translate legacy closed-loop transmission signals into modern, web-friendly RESTful architectures. Network architects implementing these bridges drastically accelerate zero-footprint image viewing across mobile diagnostic devices.
Imaging Interoperability Middleware Market Analysis by Deployment
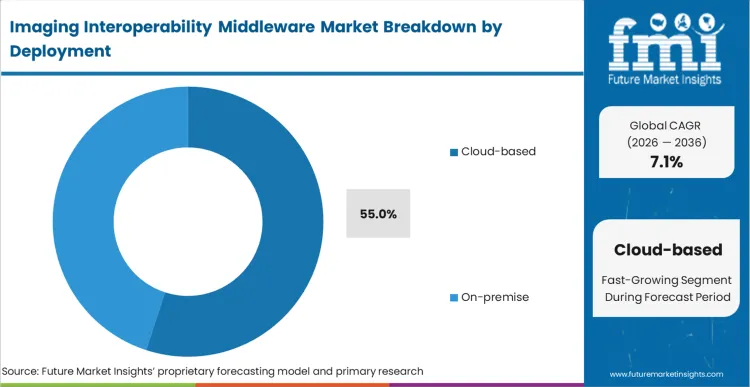
Cloud-based environments represent the specific compliance and scalability threshold that forces immediate buyer action across regional health systems. Cloud-based deployment commands 55.0% of the market share in 2026, driven explicitly by the exponential growth of multi-terabyte specialty imaging datasets that shatter the physical constraints of on-premises servers. Hospital IT procurement teams prioritize these hosted platforms to immediately sidestep massive capital expenditures associated with localized disaster recovery infrastructure.
According to FMI's estimates, the inherent elasticity of cloud models directly supports the variable influx of high-resolution cloud-based medical imaging data from outpatient clinics. Facility managers who fail to migrate their middleware to scalable cloud environments suffer severe application downtime and degraded system performance during peak diagnostic periods.
- Elastic scalability: Auto-provisioning cloud architectures instantly expand computing resources to handle unpredictable surges in complex 3D and 4D imaging studies. Enterprise architects utilizing this flexibility maintain sub-second image retrieval times regardless of concurrent user loads.
- Hosted compliance: Managed cloud providers enforce continuous, automated security updates that adhere strictly to evolving HIPAA and EHDS data sovereignty regulations. Data privacy officers migrating to these platforms immediately offload the enormous liability of localized security breaches.
- Disaster resilience: Geo-redundant cloud storage nodes replicate critical image metadata across multiple physical locations automatically. Clinical continuity directors operating in these environments guarantee uninterrupted diagnostic access during catastrophic localized network failures.
Imaging Interoperability Middleware Market Analysis by End User
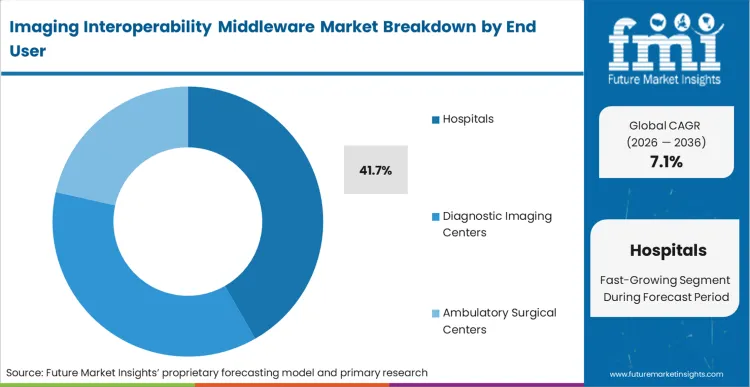
Hospitals dominate this market with a 41.7% share in 2026, fused directly to the structural dependency created by massive, multi-departmental IT consolidation strategies. Chief Medical Information Officers (CMIOs) operate the most fragmented imaging ecosystems in the industry, often managing dozens of distinct specialty silos that critically impair collaborative patient care.
Based on FMI's assessment, the immediate pressure to unify these fragmented digital pathology adoption workflows drives aggressive investment into vendor-agnostic middleware platforms. Multi-site hospital directors must eliminate these data silos to achieve true longitudinal patient records. Executives who rely on legacy departmental routing face insurmountable financial penalties related to duplicate storage, while simultaneously crippling their cross-functional diagnostic tumor boards.
- Consolidated archiving: Centralized middleware controllers allow massive health systems to route diverse departmental images into a single, highly optimized vendor-neutral repository. Enterprise storage directors executing this strategy immediately reclaim millions in budget previously wasted on siloed departmental hardware.
- Workflow orchestration: Intelligent routing protocols automatically direct critical trauma imaging studies to the most appropriate on-call specialist based on real-time availability. Emergency department administrators leveraging these protocols drastically reduce treatment delays for acute stroke and trauma patients.
- Cross-enterprise viewing: Universal access engines permit any authorized physician to securely view high-fidelity imaging directly from the core electronic health record interface. Chief clinical officers mandating this access drastically enhance multi-disciplinary diagnostic accuracy and surgical planning efficiency.
Imaging Interoperability Middleware Market Analysis by Application
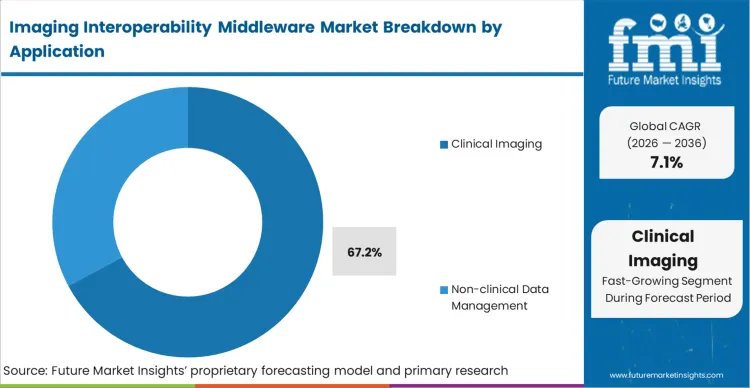
The operational gap this segment specifically exists to solve is the systemic delay in delivering high-fidelity diagnostic visuals to the point of care. Clinical Imaging commands 67.2% of the market in 2026, as the immediate interpretation of radiology, cardiology, and oncology studies dictates the fundamental revenue cycle of the entire healthcare organization. Departmental directors are fundamentally compelled to acquire robust middleware to ensure real-time rendering of complex anatomical models across distributed networks.
In FMI's view, the integration of real-time clinical visual data directly into electronic health records is now a basic qualification standard for modern remote diagnostic consultation. Healthcare providers who fail to integrate robust clinical imaging middleware face catastrophic delays in critical care interventions and rapidly lose referral confidence from their affiliated physician networks.
- Diagnostic streaming: Real-time pixel rendering algorithms transmit diagnostic-quality images to low-bandwidth remote workstations without transferring massive source files. Teleradiology directors deploying these algorithms guarantee immediate diagnostic turnaround times regardless of the reading physician's geographic location.
- Multi-disciplinary collaboration: Synchronized session tools allow disparate specialists across different hospital campuses to interactively manipulate the same 3D clinical image simultaneously. Oncology board coordinators utilizing these platforms dramatically accelerate complex, multi-stage treatment planning.
- Specialty ingestion: Purpose-built format converters ingest non-standard clinical visuals like visible light photography and endoscopy video directly into the patient's unified timeline. Clinical workflow managers implementing these converters completely eliminate the severe blind spots caused by unmanaged external specialty data.
Imaging Interoperability Middleware Market Drivers, Restraints, and Opportunities
The Fast Healthcare Interoperability Resources (FHIR) R4 standard mandate from the ONC systematically forces multi-site hospital networks to abandon proprietary integration methodologies in favor of open, API-driven data exchange architectures. This aggressive regulatory pressure dictates that enterprise IT directors permanently replace legacy point-to-point interfaces with centralized, vendor-agnostic middleware layers to achieve compliance. This regulatory trigger accelerates market expansion as systems that previously functioned in isolation must now securely expose standardized image metadata to external networks. Organizations that refuse to modernize their routing layers lose access to lucrative value-based care contracts and face severe federal information-blocking penalties.
Stringent internal network security protocols and legacy hardware bottlenecks heavily restrict the rapid deployment of cloud-native middleware solutions in rural or critically underfunded healthcare facilities. The specific technical gap emerges when outdated local area networks (LANs) simply lack the bandwidth necessary to support dynamic API traffic and large-scale metadata synchronization. While edge-computing caching nodes are emerging as a workaround to stabilize intermittent connectivity, they inherently create new localized maintenance burdens that defeat the primary purpose of centralized cloud interoperability.
Opportunities in the Imaging Interoperability Middleware Market
- AI-Native Metadata Normalization: Advanced machine learning algorithms allow software developers to instantly map and normalize thousands of proprietary DICOM tags into universal FHIR profiles without manual intervention. Health IT integrators deploying these AI engines capture massive market share by cutting implementation timelines for hospital M&A projects by over seventy percent.
- Outpatient Integration Hubs: Purpose-built, lightweight API gateways allow regional health exchanges to seamlessly ingest imaging data from highly fragmented independent imaging centers. Managed service providers offering these hubs secure exclusive, long-term healthcare application integration contracts by dramatically reducing referral leakage for large enterprise hospital networks.
- Non-DICOM Enterprise Orchestration: Specialized video and image parsers enable system architects to route visible light media, surgical MP4s, and digital pathology slides directly into the core imaging archive. Enterprise imaging directors implementing these comprehensive orchestrators capture immense operational value by eliminating rogue, unmanaged data silos hidden across secondary specialty departments.
Regional Analysis
Based on the regional analysis, the Imaging Interoperability Middleware market is segmented into North America, Latin America, Europe, East Asia, South Asia & Pacific, and Middle East & Africa across 40 plus countries.
.webp)
| Country | CAGR (2026 to 2036) |
|---|---|
| China | 9.5% |
| India | 9.1% |
| United States | 8.2% |
| United Kingdom | 8.0% |
| Germany | 7.5% |
| Japan | 7.1% |
| Brazil | 6.8% |
Source: Future Market Insights (FMI) analysis, based on proprietary forecasting model and primary research
East Asia Imaging Interoperability Middleware Market Analysis
Specific government mandates heavily dictate the structural adoption of interoperability platforms across East Asia, distinguishing it sharply from organic, market-driven regions. The National Health Commission's aggressive policy to construct interconnected regional medical centers forces provincial health authorities to immediately establish vast, standardized image-sharing networks. This regulatory environment explicitly requires the immediate untangling of highly localized, proprietary hospital IT systems to enable smooth data flow across the entire healthcare continuum.
FMI analysts observe that the rapid deployment of these centralized clinical visualization platforms acts as the fundamental backbone for redistributing diagnostic labor away from severely overburdened urban facilities.
- China: Demand is advancing at 9.5% compound between 2026 and 2036.The National Health Commission in China enforces strict data-sharing mandates that actively push diagnostic workloads from tier-3 urban mega-hospitals to regional tier-2 facilities. This specific policy framework requires provincial IT directors to rapidly deploy vendor-neutral interoperability gateways to support the massive volume of cross-facility image transfers. Highly publicised state investments into national health IT grids confirm this immediate shift toward comprehensive data liquidity. Hospital administrators who fail to integrate these mandated routing engines face severe funding restrictions and operational isolation.
- Japan: Japan's rapidly ageing demographic forces regional care networks to adopt highly efficient, low-latency image exchange platforms to support expanding home-based and remote care initiatives. This demographic pressure pushes health system planners to upgrade legacy on-premises silos with dynamic cloud middleware. Extensive national health insurance subsidies for digitalization projects actively support this specific transition. Tracking 7.1% annual growth to 2036, Japan demonstrates steady expansion. Care network aggregators delaying these upgrades lose the ability to efficiently coordinate complex geriatric interventions across disparate provider networks.
FMI's report includes detailed analysis of South Korea and Taiwan. Government-backed smart hospital initiatives across these nations actively incentivize the complete replacement of closed-loop PACS systems with open FHIR architectures.
South Asia & Pacific Imaging Interoperability Middleware Market Analysis
Specific physical digital infrastructure constraints and rapidly expanding greenfield hospital construction completely define the South Asia market dynamic. Unlike regions burdened by decades of legacy technical debt, newly constructed multi-specialty corporate hospital chains in this region are actively deploying cloud-native middleware architectures from day one. This proactive procurement practice allows organizations to entirely bypass the painful process of unspooling siloed departmental archives. FMI projections indicate that these organizations heavily leverage API-driven infrastructure to rapidly scale their geographic footprint across underserved tier-2 and tier-3 cities without replicating expensive local data centers.
- India: The rapid expansion of corporate hospital chains in India enables the immediate, greenfield deployment of advanced cloud-native imaging middleware without the friction of legacy system rip-and-replace. This infrastructural advantage allows enterprise IT leaders to immediately centralize diagnostic reporting hubs across vast geographic regions. Projected at 9.1% compound growth over the forecast period, the trajectory remains robust. Soaring private equity investments into digital healthcare startups directly validate the aggressive architectural modernization. Capital project directors who construct facilities using outdated, closed-loop proprietary storage immediately saddle their organizations with massive future integration liabilities.
FMI's report includes comprehensive evaluation of Australia and Southeast Asia. The widespread deployment of national digital health records in these adjacent areas forces private operators to standardize their image metadata outputs for seamless public integration.
North America Imaging Interoperability Middleware Market Analysis
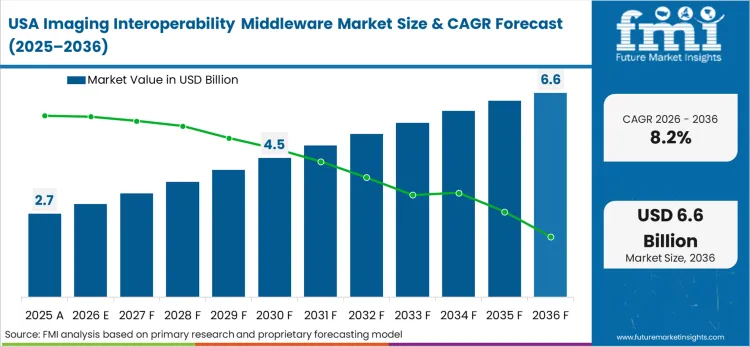
Intense cost structure pressures and margin consolidation dictate the North American transition toward software-defined interoperability. The unrelenting wave of mergers and acquisitions across the healthcare sector creates impossibly complex, fragmented IT environments that threaten clinical safety. To counteract these margin pressures, massive integrated delivery networks are utilizing advanced middleware to radically consolidate their imaging vendor portfolios. Based on FMI's assessment, the primary objective is to aggressively negotiate enterprise-level licensing agreements by untangling clinical data from specific hardware vendors, thereby restoring critical pricing leverage to the hospital networks.
- United States: Strict enforcement of the ONC's information-blocking regulations in the United States requires massive integrated delivery networks to guarantee instant, patient-authorized access to all diagnostic imaging records. This intense regulatory pressure forces enterprise architecture teams to deploy FHIR-native interoperability layers that bridge dozens of disparate, inherited departmental archives. Multi-million-dollar fines attached to non-compliance serve as the ultimate operational catalyst for this architectural overhaul. Expanding at 8.2% between 2026 and 2036, the market demonstrates relentless maturity. System integrators who cannot rapidly normalize complex metadata tags across acquired hospital networks face immediate contract termination.
FMI's report includes coverage of Canada. Provincial health ministries are currently orchestrating massive, cross-jurisdictional procurement programs designed to establish unified, vendor-neutral imaging repositories that span entire regions.
Europe Imaging Interoperability Middleware Market Analysis
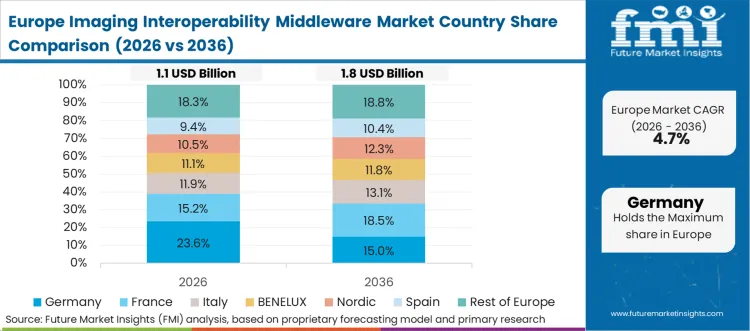
The European Health Data Space (EHDS) directive serves as the absolute policy-led lens defining this region's aggressive interoperability roadmap. The mandate legally compels healthcare providers to dismantle proprietary data lock-ins, ensuring that a patient's imaging history moves fluidly across international borders. European hospital consortiums are actively replacing localized data silos with highly standardized, cross-border API gateways. FMI analysts observe that the continent's fragmented, multi-vendor landscape is rapidly coalescing around these central integration engines to meet the looming compliance deadlines established by the European Commission.
- United Kingdom: The NHS's centralized push for integrated care systems in the United Kingdom compels regional trusts to implement unified interoperability middleware that entirely bypasses localized hospital silos. This structural mandate forces regional IT procurement leads to select vendor-agnostic platforms capable of seamlessly serving primary, secondary, and social care providers simultaneously. Anchored to an 8.0% annual expansion through the decade, the region shows focused modernization. Widespread pilot programs demonstrating cross-trust diagnostic load balancing confirm the operational urgency of these specific deployments. Network operators who ignore this unified integration directives lose critical access to highly consolidated NHS funding streams.
- Germany: Germany's Hospital Future Act (KHZG) directly subsidizes the modernization of clinical IT infrastructure, specifically targeting the elimination of isolated, proprietary imaging archives. This massive capital injection empowers clinical IT directors to immediately rip out legacy PACS networks in favor of open, interoperable outpatient facility technology. The rapid surge in certified FHIR implementation projects across German university hospitals verifies this structural shift. Sustaining a 7.5% CAGR to 2036, the nation's progress is heavily fortified. Facility owners who fail to secure these federal modernization funds severely compromise their competitive diagnostic capabilities against heavily subsidized regional peers.
FMI's report includes detailed examination of France, Italy, and Spain. Expanding cross-border patient mobility initiatives heavily pressure these nations to adopt completely uniform metadata exchange protocols.
Latin America Imaging Interoperability Middleware Market Analysis
Highly specific margin pressures and limited capital availability define Latin America's unique approach to imaging interoperability. To circumvent the massive upfront costs associated with completely replacing outdated PACS infrastructure, regional health networks heavily favor lightweight, subscription-based middleware nodes that simply bridge existing systems. This specific economic constraint forces providers to prioritize intelligent routing software that dramatically extends the lifecycle of their current storage investments while immediately solving localized image-sharing bottlenecks.
- Brazil: Severe budget constraints within Brazil's expansive public health system (SUS) dictate the deployment of highly efficient, lightweight middleware nodes designed to extract maximum value from existing, ageing PACS infrastructure. This economic reality forces regional health secretaries to prioritize API wrappers that enable basic image sharing without requiring massive, comprehensive server overhauls. Increasing utilization of hybrid-cloud caching protocols across remote diagnostic outposts confirms this highly pragmatic integration strategy. Sustaining a 6.8% CAGR to 2036, the market reflects careful, measured expansion. Procurement specification leads who pursue monolithic, capital-intensive interoperability overhauls rapidly deplete their budgets, leaving vast operational gaps across the wider care network.
FMI's report includes coverage of Mexico and Argentina. Widespread expansion of private diagnostic networks in these areas drives targeted investments into localized image exchange software to capture referral volume.
Competitive Aligners for Market Players
The imaging interoperability middleware market is moderately consolidated, heavily defined by immense technical barriers surrounding deep EHR integration, complex metadata normalization capabilities, and FHIR standard certifications. Leading providers such as GE HealthCare, Philips, and Siemens Healthineers actively leverage their massive existing hardware and software installed bases to secure highly entrenched competitive positions. Hospital networks attempting to decouple their infrastructure heavily scrutinize a vendor’s proven capacity to handle highly specialized, non-DICOM image types without corrupting the underlying data architecture. The primary competitive variable buyers use to distinguish qualified vendors is the absolute speed and accuracy of the platform's automated patient identity reconciliation engine.
Challenger organizations and specialized software firms compete aggressively by developing highly advanced, AI-native metadata normalization engines that drastically undercut the implementation timelines of legacy incumbents. Companies like Mach7 Technologies and Sectra AB hold specific structural advantages in their ability to dynamically ingest and route fragmented specialty imaging files seamlessly. A critical capability for any challenger is offering lightweight, vendor-neutral archives that operate entirely free from the proprietary lock-ins typical of older PACS environments. To successfully displace an entrenched incumbent, a challenger must prove their platform can achieve complete system interoperability within a fraction of the traditional deployment schedule.
To aggressively prevent vendor lock-in, massive multi-site buyers are increasingly adopting strict multi-vendor procurement programs and demanding absolute compliance with open API standards. This intense structural tension pits hospital IT directors, who demand total data liquidity, against dominant vendors attempting to protect lucrative, closed-ecosystem revenue streams. By forcing adherence to independent IHE profiles and FHIR standards, buyers severely limit the pricing power of even the most dominant market players. The competitive trajectory toward 2036 indicates that the market will become increasingly defined by specialized, agile software firms that excel exclusively in pure data orchestration.
Key Players in Imaging Interoperability Middleware Market
- GE HealthCare
- Koninklijke Philips N.V.
- FUJIFILM Corporation
- Siemens Healthineers
- Merative
- Agfa-Gevaert Group
- Sectra AB
- Mach7 Technologies
Scope of the Report
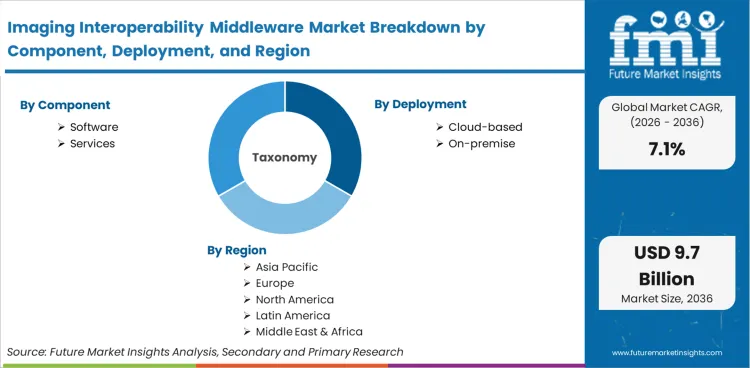
| Metric | Value |
|---|---|
| Quantitative Units | USD 4.9 billion to USD 9.8 billion, at a CAGR of 7.12% |
| Market Definition | Software and services that translate, normalize, and route clinical imaging data across disparate IT systems, structurally decoupling image storage from diagnostic viewers using API-driven standards. |
| Component Segmentation | Software, Services |
| Deployment Segmentation | Cloud-based, On-premise, Hybrid |
| End User Segmentation | Hospitals, Diagnostic Imaging Centers, Ambulatory Surgical Centers |
| Application Segmentation | Clinical Imaging, Non-clinical Data Management |
| Regions Covered | North America, Latin America, Europe, East Asia, South Asia & Pacific, Middle East & Africa |
| Countries Covered | China, India, United States, United Kingdom, Germany, Japan, Brazil, and 40 plus countries |
| Key Companies Profiled | GE HealthCare, Koninklijke Philips N.V., FUJIFILM Corporation, Siemens Healthineers, Merative, Agfa-Gevaert Group, Sectra AB, Mach7 Technologies |
| Forecast Period | 2026 to 2036 |
| Approach | Executive interviews targeted CMIOs and regional healthcare data privacy officers. The baseline modeling assessed the total addressable base of isolated departmental image repositories to model the total conversion volume toward neutral routing architectures, validated against public vendor implementation disclosures. |
Source: Future Market Insights (FMI) analysis, based on proprietary forecasting model and primary research
Imaging Interoperability Middleware Market Analysis by Segments
Component:
- Software
- Services
Deployment:
- Cloud-based
- On-premise
- Hybrid
End User:
- Hospitals
- Diagnostic Imaging Centers
- Ambulatory Surgical Centers
Application:
- Clinical Imaging
- Non-clinical Data Management
Region:
- North America
- United States
- Canada
- Mexico
- Latin America
- Brazil
- Argentina
- Chile
- Rest of Latin America
- Europe
- Germany
- United Kingdom
- France
- Italy
- Spain
- Benelux
- Rest of Europe
- East Asia
- China
- Japan
- South Korea
- South Asia
- India
- ASEAN
- Rest of South Asia
- Oceania
- Australia
- New Zealand
- Middle East & Africa
- Kingdom of Saudi Arabia
- United Arab Emirates
- South Africa
- Rest of Middle East & Africa
Bibliography
- Office of the National Coordinator for Health Information Technology. (2024). 2024 Interoperability Standards Advisory reference edition. USA Department of Health and Human Services.
- USA Department of Health and Human Services, Office of the Assistant Secretary for Technology Policy/Office of the National Coordinator for Health Information Technology. (2026). Request for information: Diagnostic imaging interoperability standards and certification. Federal Register.
- National Electrical Manufacturers Association. (2024). Digital Imaging and Communications in Medicine (DICOM) supplement 244: Frame deflate transfer syntax. DICOM Standards Committee.
- Integrating the Healthcare Enterprise International, Inc. (2024). IHE radiology technical framework, volume 1 (RAD TF-1): Integration profiles (Rev. 22.0, Final Text).
- Radiological Society of North America. (2024, October 4). Re: Health Data, Technology, and Interoperability: Patient Engagement, Information Sharing, and Public Health Interoperability (HTI-2) proposed rule (RIN 0955-AA06).
- Tejani, A. S., Bialecki, B., O’Donnell, K., Sippel Schmidt, T., Kohli, M. D., & Alkasab, T. (2024). Standardizing imaging findings representation: Harnessing Common Data Elements semantics and Fast Healthcare Interoperability Resources structures. Journal of the American Medical Informatics Association, 31(8), 1735-1742.
- Roth, C. J., Petersilge, C., Clunie, D., Towbin, A. J., Cram, D., Primo, R., Li, X., Berkowitz, S. J., Barnosky, V., & Krupinski, E. A. (2024). HIMSS-SIIM enterprise imaging community white papers: Reflections and future directions. Journal of Imaging Informatics in Medicine, 37(2), 429-443.
This bibliography is provided for reader reference. The full FMI report contains the complete reference list with primary source documentation.
This Report Addresses
- Market intelligence to support strategic decision making across independent clinical data routing engines, patient identity reconciliation software, and metadata normalization algorithms unique to this market
- Market size estimation and 10-year revenue forecasts from 2026 to 2036, supported by HL7 FHIR implementation registries and ONC technical compliance documentation tracking
- Growth opportunity mapping across deployment and end user categories with emphasis on cloud providers natively embedding FHIR-compliant imaging ingestion engines
- Segment and regional revenue forecasts covering software and API-based gateways across multi-site hospital networks and stringent European EHDS regulatory contexts
- Competition strategy assessment including deep EHR integration capabilities, complex metadata normalization speeds, and FHIR standard certifications
- Technology development tracking including RESTful API-based middleware, Master Patient Index (MPI) integration tools, dynamic tag morphing, and non-DICOM enterprise orchestrators discussed in this article
- Market access analysis covering regional health exchange programs, outpatient integration hubs, and national digital health records initiatives
- Market report delivery in PDF, Excel, PPT, and interactive dashboard formats for executive strategy, enterprise IT architecture planning, and operational benchmarking use
Frequently Asked Questions
How large is the Imaging Interoperability Middleware Market in 2026?
The sector is set to cross USD 4.9 billion in 2026, driven fundamentally by enterprise IT directors seeking to aggressively decouple image acquisition hardware from long-term archiving environments.
What will it be valued at by 2036?
The valuation reaches USD 9.8 billion through 2036 as multi-site health systems mandate API-driven decoupling of image viewers from legacy storage archives to eliminate proprietary departmental silos.
What CAGR is projected?
A robust 7.12% compound growth rate is projected, anchored securely to the mandatory enforcement of FHIR data-sharing standards across consolidated hospital networks.
Which Component segment leads?
Software leads with 61.4% share in 2026, completely reliant on continuous algorithm-based metadata normalization engines rather than localized hardware scaling.
Which Deployment segment leads?
Cloud-based platforms dominate, expanding rapidly as elastic storage requirements outpace the strict capital expenditure limits of on-premise hospital data centers.
Which End User segment leads?
Hospitals maintain a 41.7% structural concentration, driven by the intense operational pressure to unify immensely fragmented multi-departmental IT silos following acquisitions.
What drives rapid growth?
The Fast Healthcare Interoperability Resources (FHIR) R4 standard mandate systematically forces multi-site hospital networks to permanently abandon proprietary point-to-point interfaces in favor of standardized API architectures.
What is the primary restraint?
Severely outdated local area network (LAN) bandwidth within rural healthcare facilities specifically restricts the deployment of dynamic, high-traffic API layers necessary for real-time metadata synchronization.
Which country grows fastest?
China accelerates at a 9.5% compound rate, propelled by the National Health Commission's strict mandates requiring provincial health authorities to rapidly deploy interconnected image-sharing networks.
How does the ONC mandate affect adoption?
Stringent federal information-blocking regulations compel integrated delivery networks to guarantee instant, standardized access to diagnostic imaging records, forcing rapid middleware modernization to avoid massive financial penalties.
What technology shift defines this sector?
The industry has fundamentally shifted from proprietary, siloed Picture Archiving and Communication Systems (PACS) routing toward RESTful API-based, vendor-neutral middleware that seamlessly orchestrates both DICOM and non-DICOM objects.
How do challengers displace incumbents?
Specialized software firms outmaneuver dominant legacy hardware providers by deploying highly advanced, AI-native metadata normalization engines that drastically undercut the implementation timelines of traditional enterprise hospital integration projects.
How does identity reconciliation impact workflow?
Master Patient Index (MPI) integration tools resolve duplicate patient records in real-time, preventing severe diagnostic errors before critical clinical images ever reach the core diagnostic viewing interface.
Why are ambulatory surgical centers investing in nodes?
Outpatient facilities are forced to deploy lightweight interoperability nodes to meet strict pre-operative surgical planning timelines, avoiding costly procedural delays caused by fragmented imaging access.
What advantage do cloud platforms offer?
Managed cloud providers enforce automated security updates that adhere precisely to EHDS and HIPAA regulations, immediately offloading massive data liability from localized hospital privacy officers.
How does the EHDS framework affect Europe?
The directive compels European hospital consortiums to actively replace localized data silos with highly standardized, cross-border API gateways, completely eliminating legacy vendor lock-ins across regional trusts.
Why does Brazil favor lightweight nodes?
Severe budget constraints force Brazilian health secretaries to prioritize API wrappers that extend the operational lifecycle of existing PACS hardware without requiring massive, capital-intensive server replacements.
What structural barrier limits enterprise viewing?
Unmanaged external specialty data, such as visible light photography and endoscopy video, severely disrupts unified timelines until system architects deploy comprehensive non-DICOM orchestration platforms.
How do referring physicians drive outpatient middleware?
Referring physicians increasingly demand zero-footprint, instant diagnostic viewer access, compelling diagnostic imaging centers to rapidly deploy cloud-native exchange software to prevent massive referral leakage.
What role does AI play in integration?
Advanced machine learning algorithms automatically map and normalize thousands of proprietary DICOM tags into universal FHIR profiles, eliminating the manual data translation that previously stalled integration projects.
Why are corporate chains in India scaling quickly?
Newly constructed corporate hospital networks deploy cloud-native middleware architectures from day one, entirely bypassing the legacy technical debt and localized hardware silos that cripple older organizations.
What forces legacy PACS administrators to adapt?
Major cloud providers natively embedding FHIR-compliant imaging ingestion engines force local IT administrators to abandon on-premise routing updates within a tight window to maintain basic system relevancy.
How is the UK NHS responding to integration mandates?
Regional NHS trusts are selecting vendor-agnostic platforms capable of seamlessly serving primary and secondary care simultaneously, perfectly aligning with centralized directives for highly integrated care systems.
What will the middleware layer look like by 2036?
The middleware layer will entirely decouple image visualization from physical storage, establishing a headless imaging ecosystem where diagnostic algorithms query normalized visual data indiscriminately across the global cloud.
Table of Content
- Executive Summary
- Global Market Outlook
- Demand-side Trends
- Supply-side Trends
- Technology Roadmap Analysis
- Analysis and Recommendations
- Market Overview
- Market Coverage / Taxonomy
- Market Definition / Scope / Limitations
- Research Methodology
- Chapter Orientation
- Analytical Lens and Working Hypotheses
- Market Structure, Signals, and Trend Drivers
- Benchmarking and Cross-market Comparability
- Market Sizing, Forecasting, and Opportunity Mapping
- Research Design and Evidence Framework
- Desk Research Programme (Secondary Evidence)
- Company Annual and Sustainability Reports
- Peer-reviewed Journals and Academic Literature
- Corporate Websites, Product Literature, and Technical Notes
- Earnings Decks and Investor Briefings
- Statutory Filings and Regulatory Disclosures
- Technical White Papers and Standards Notes
- Trade Journals, Industry Magazines, and Analyst Briefs
- Conference Proceedings, Webinars, and Seminar Materials
- Government Statistics Portals and Public Data Releases
- Press Releases and Reputable Media Coverage
- Specialist Newsletters and Curated Briefings
- Sector Databases and Reference Repositories
- FMI Internal Proprietary Databases and Historical Market Datasets
- Subscription Datasets and Paid Sources
- Social Channels, Communities, and Digital Listening Inputs
- Additional Desk Sources
- Expert Input and Fieldwork (Primary Evidence)
- Primary Modes
- Qualitative Interviews and Expert Elicitation
- Quantitative Surveys and Structured Data Capture
- Blended Approach
- Why Primary Evidence is Used
- Field Techniques
- Interviews
- Surveys
- Focus Groups
- Observational and In-context Research
- Social and Community Interactions
- Stakeholder Universe Engaged
- C-suite Leaders
- Board Members
- Presidents and Vice Presidents
- R&D and Innovation Heads
- Technical Specialists
- Domain Subject-matter Experts
- Scientists
- Physicians and Other Healthcare Professionals
- Governance, Ethics, and Data Stewardship
- Research Ethics
- Data Integrity and Handling
- Primary Modes
- Tooling, Models, and Reference Databases
- Desk Research Programme (Secondary Evidence)
- Data Engineering and Model Build
- Data Acquisition and Ingestion
- Cleaning, Normalisation, and Verification
- Synthesis, Triangulation, and Analysis
- Quality Assurance and Audit Trail
- Market Background
- Market Dynamics
- Drivers
- Restraints
- Opportunity
- Trends
- Scenario Forecast
- Demand in Optimistic Scenario
- Demand in Likely Scenario
- Demand in Conservative Scenario
- Opportunity Map Analysis
- Product Life Cycle Analysis
- Supply Chain Analysis
- Investment Feasibility Matrix
- Value Chain Analysis
- PESTLE and Porter’s Analysis
- Regulatory Landscape
- Regional Parent Market Outlook
- Production and Consumption Statistics
- Import and Export Statistics
- Market Dynamics
- Global Market Analysis 2021 to 2025 and Forecast, 2026 to 2036
- Historical Market Size Value (USD Million) Analysis, 2021 to 2025
- Current and Future Market Size Value (USD Million) Projections, 2026 to 2036
- Y-o-Y Growth Trend Analysis
- Absolute $ Opportunity Analysis
- Global Market Pricing Analysis 2021 to 2025 and Forecast 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Component
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Component , 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Component , 2026 to 2036
- Software
- Services
- Software
- Y-o-Y Growth Trend Analysis By Component , 2021 to 2025
- Absolute $ Opportunity Analysis By Component , 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Deployment
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Deployment, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Deployment, 2026 to 2036
- Cloud-based
- On-premise
- Cloud-based
- Y-o-Y Growth Trend Analysis By Deployment, 2021 to 2025
- Absolute $ Opportunity Analysis By Deployment, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By End User
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By End User, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By End User, 2026 to 2036
- Hospitals
- Diagnostic Imaging Centers
- Ambulatory Surgical Centers
- Hospitals
- Y-o-Y Growth Trend Analysis By End User, 2021 to 2025
- Absolute $ Opportunity Analysis By End User, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Application
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Application, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Application, 2026 to 2036
- Clinical Imaging
- Non-clinical Data Management
- Clinical Imaging
- Y-o-Y Growth Trend Analysis By Application, 2021 to 2025
- Absolute $ Opportunity Analysis By Application, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Region
- Introduction
- Historical Market Size Value (USD Million) Analysis By Region, 2021 to 2025
- Current Market Size Value (USD Million) Analysis and Forecast By Region, 2026 to 2036
- North America
- Latin America
- Western Europe
- Eastern Europe
- East Asia
- South Asia and Pacific
- Middle East & Africa
- Market Attractiveness Analysis By Region
- North America Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- USA
- Canada
- Mexico
- By Component
- By Deployment
- By End User
- By Application
- By Country
- Market Attractiveness Analysis
- By Country
- By Component
- By Deployment
- By End User
- By Application
- Key Takeaways
- Latin America Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Brazil
- Chile
- Rest of Latin America
- By Component
- By Deployment
- By End User
- By Application
- By Country
- Market Attractiveness Analysis
- By Country
- By Component
- By Deployment
- By End User
- By Application
- Key Takeaways
- Western Europe Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Germany
- UK
- Italy
- Spain
- France
- Nordic
- BENELUX
- Rest of Western Europe
- By Component
- By Deployment
- By End User
- By Application
- By Country
- Market Attractiveness Analysis
- By Country
- By Component
- By Deployment
- By End User
- By Application
- Key Takeaways
- Eastern Europe Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Russia
- Poland
- Hungary
- Balkan & Baltic
- Rest of Eastern Europe
- By Component
- By Deployment
- By End User
- By Application
- By Country
- Market Attractiveness Analysis
- By Country
- By Component
- By Deployment
- By End User
- By Application
- Key Takeaways
- East Asia Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- China
- Japan
- South Korea
- By Component
- By Deployment
- By End User
- By Application
- By Country
- Market Attractiveness Analysis
- By Country
- By Component
- By Deployment
- By End User
- By Application
- Key Takeaways
- South Asia and Pacific Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- India
- ASEAN
- Australia & New Zealand
- Rest of South Asia and Pacific
- By Component
- By Deployment
- By End User
- By Application
- By Country
- Market Attractiveness Analysis
- By Country
- By Component
- By Deployment
- By End User
- By Application
- Key Takeaways
- Middle East & Africa Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Kingdom of Saudi Arabia
- Other GCC Countries
- Turkiye
- South Africa
- Other African Union
- Rest of Middle East & Africa
- By Component
- By Deployment
- By End User
- By Application
- By Country
- Market Attractiveness Analysis
- By Country
- By Component
- By Deployment
- By End User
- By Application
- Key Takeaways
- Key Countries Market Analysis
- USA
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- Canada
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- Mexico
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- Brazil
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- Chile
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- Germany
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- UK
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- Italy
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- Spain
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- France
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- India
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- ASEAN
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- Australia & New Zealand
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- China
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- Japan
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- South Korea
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- Russia
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- Poland
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- Hungary
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- Kingdom of Saudi Arabia
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- Turkiye
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- South Africa
- Pricing Analysis
- Market Share Analysis, 2025
- By Component
- By Deployment
- By End User
- By Application
- USA
- Market Structure Analysis
- Competition Dashboard
- Competition Benchmarking
- Market Share Analysis of Top Players
- By Regional
- By Component
- By Deployment
- By End User
- By Application
- Competition Analysis
- Competition Deep Dive
- GE HealthCare
- Overview
- Product Portfolio
- Profitability by Market Segments (Product/Age /Sales Channel/Region)
- Sales Footprint
- Strategy Overview
- Marketing Strategy
- Product Strategy
- Channel Strategy
- Koninklijke Philips N.V.
- FUJIFILM Corporation
- Siemens Healthineers
- Merative
- Agfa-Gevaert Group
- Sectra AB
- GE HealthCare
- Competition Deep Dive
- Assumptions & Acronyms Used
List of Tables
- Table 1: Global Market Value (USD Million) Forecast by Region, 2021 to 2036
- Table 2: Global Market Value (USD Million) Forecast by Component , 2021 to 2036
- Table 3: Global Market Value (USD Million) Forecast by Deployment, 2021 to 2036
- Table 4: Global Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 5: Global Market Value (USD Million) Forecast by Application, 2021 to 2036
- Table 6: North America Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 7: North America Market Value (USD Million) Forecast by Component , 2021 to 2036
- Table 8: North America Market Value (USD Million) Forecast by Deployment, 2021 to 2036
- Table 9: North America Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 10: North America Market Value (USD Million) Forecast by Application, 2021 to 2036
- Table 11: Latin America Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 12: Latin America Market Value (USD Million) Forecast by Component , 2021 to 2036
- Table 13: Latin America Market Value (USD Million) Forecast by Deployment, 2021 to 2036
- Table 14: Latin America Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 15: Latin America Market Value (USD Million) Forecast by Application, 2021 to 2036
- Table 16: Western Europe Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 17: Western Europe Market Value (USD Million) Forecast by Component , 2021 to 2036
- Table 18: Western Europe Market Value (USD Million) Forecast by Deployment, 2021 to 2036
- Table 19: Western Europe Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 20: Western Europe Market Value (USD Million) Forecast by Application, 2021 to 2036
- Table 21: Eastern Europe Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 22: Eastern Europe Market Value (USD Million) Forecast by Component , 2021 to 2036
- Table 23: Eastern Europe Market Value (USD Million) Forecast by Deployment, 2021 to 2036
- Table 24: Eastern Europe Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 25: Eastern Europe Market Value (USD Million) Forecast by Application, 2021 to 2036
- Table 26: East Asia Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 27: East Asia Market Value (USD Million) Forecast by Component , 2021 to 2036
- Table 28: East Asia Market Value (USD Million) Forecast by Deployment, 2021 to 2036
- Table 29: East Asia Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 30: East Asia Market Value (USD Million) Forecast by Application, 2021 to 2036
- Table 31: South Asia and Pacific Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 32: South Asia and Pacific Market Value (USD Million) Forecast by Component , 2021 to 2036
- Table 33: South Asia and Pacific Market Value (USD Million) Forecast by Deployment, 2021 to 2036
- Table 34: South Asia and Pacific Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 35: South Asia and Pacific Market Value (USD Million) Forecast by Application, 2021 to 2036
- Table 36: Middle East & Africa Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 37: Middle East & Africa Market Value (USD Million) Forecast by Component , 2021 to 2036
- Table 38: Middle East & Africa Market Value (USD Million) Forecast by Deployment, 2021 to 2036
- Table 39: Middle East & Africa Market Value (USD Million) Forecast by End User, 2021 to 2036
- Table 40: Middle East & Africa Market Value (USD Million) Forecast by Application, 2021 to 2036
List of Figures
- Figure 1: Global Market Pricing Analysis
- Figure 2: Global Market Value (USD Million) Forecast 2021-2036
- Figure 3: Global Market Value Share and BPS Analysis by Component , 2026 and 2036
- Figure 4: Global Market Y-o-Y Growth Comparison by Component , 2026-2036
- Figure 5: Global Market Attractiveness Analysis by Component
- Figure 6: Global Market Value Share and BPS Analysis by Deployment, 2026 and 2036
- Figure 7: Global Market Y-o-Y Growth Comparison by Deployment, 2026-2036
- Figure 8: Global Market Attractiveness Analysis by Deployment
- Figure 9: Global Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 10: Global Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 11: Global Market Attractiveness Analysis by End User
- Figure 12: Global Market Value Share and BPS Analysis by Application, 2026 and 2036
- Figure 13: Global Market Y-o-Y Growth Comparison by Application, 2026-2036
- Figure 14: Global Market Attractiveness Analysis by Application
- Figure 15: Global Market Value (USD Million) Share and BPS Analysis by Region, 2026 and 2036
- Figure 16: Global Market Y-o-Y Growth Comparison by Region, 2026-2036
- Figure 17: Global Market Attractiveness Analysis by Region
- Figure 18: North America Market Incremental Dollar Opportunity, 2026-2036
- Figure 19: Latin America Market Incremental Dollar Opportunity, 2026-2036
- Figure 20: Western Europe Market Incremental Dollar Opportunity, 2026-2036
- Figure 21: Eastern Europe Market Incremental Dollar Opportunity, 2026-2036
- Figure 22: East Asia Market Incremental Dollar Opportunity, 2026-2036
- Figure 23: South Asia and Pacific Market Incremental Dollar Opportunity, 2026-2036
- Figure 24: Middle East & Africa Market Incremental Dollar Opportunity, 2026-2036
- Figure 25: North America Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 26: North America Market Value Share and BPS Analysis by Component , 2026 and 2036
- Figure 27: North America Market Y-o-Y Growth Comparison by Component , 2026-2036
- Figure 28: North America Market Attractiveness Analysis by Component
- Figure 29: North America Market Value Share and BPS Analysis by Deployment, 2026 and 2036
- Figure 30: North America Market Y-o-Y Growth Comparison by Deployment, 2026-2036
- Figure 31: North America Market Attractiveness Analysis by Deployment
- Figure 32: North America Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 33: North America Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 34: North America Market Attractiveness Analysis by End User
- Figure 35: North America Market Value Share and BPS Analysis by Application, 2026 and 2036
- Figure 36: North America Market Y-o-Y Growth Comparison by Application, 2026-2036
- Figure 37: North America Market Attractiveness Analysis by Application
- Figure 38: Latin America Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 39: Latin America Market Value Share and BPS Analysis by Component , 2026 and 2036
- Figure 40: Latin America Market Y-o-Y Growth Comparison by Component , 2026-2036
- Figure 41: Latin America Market Attractiveness Analysis by Component
- Figure 42: Latin America Market Value Share and BPS Analysis by Deployment, 2026 and 2036
- Figure 43: Latin America Market Y-o-Y Growth Comparison by Deployment, 2026-2036
- Figure 44: Latin America Market Attractiveness Analysis by Deployment
- Figure 45: Latin America Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 46: Latin America Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 47: Latin America Market Attractiveness Analysis by End User
- Figure 48: Latin America Market Value Share and BPS Analysis by Application, 2026 and 2036
- Figure 49: Latin America Market Y-o-Y Growth Comparison by Application, 2026-2036
- Figure 50: Latin America Market Attractiveness Analysis by Application
- Figure 51: Western Europe Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 52: Western Europe Market Value Share and BPS Analysis by Component , 2026 and 2036
- Figure 53: Western Europe Market Y-o-Y Growth Comparison by Component , 2026-2036
- Figure 54: Western Europe Market Attractiveness Analysis by Component
- Figure 55: Western Europe Market Value Share and BPS Analysis by Deployment, 2026 and 2036
- Figure 56: Western Europe Market Y-o-Y Growth Comparison by Deployment, 2026-2036
- Figure 57: Western Europe Market Attractiveness Analysis by Deployment
- Figure 58: Western Europe Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 59: Western Europe Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 60: Western Europe Market Attractiveness Analysis by End User
- Figure 61: Western Europe Market Value Share and BPS Analysis by Application, 2026 and 2036
- Figure 62: Western Europe Market Y-o-Y Growth Comparison by Application, 2026-2036
- Figure 63: Western Europe Market Attractiveness Analysis by Application
- Figure 64: Eastern Europe Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 65: Eastern Europe Market Value Share and BPS Analysis by Component , 2026 and 2036
- Figure 66: Eastern Europe Market Y-o-Y Growth Comparison by Component , 2026-2036
- Figure 67: Eastern Europe Market Attractiveness Analysis by Component
- Figure 68: Eastern Europe Market Value Share and BPS Analysis by Deployment, 2026 and 2036
- Figure 69: Eastern Europe Market Y-o-Y Growth Comparison by Deployment, 2026-2036
- Figure 70: Eastern Europe Market Attractiveness Analysis by Deployment
- Figure 71: Eastern Europe Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 72: Eastern Europe Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 73: Eastern Europe Market Attractiveness Analysis by End User
- Figure 74: Eastern Europe Market Value Share and BPS Analysis by Application, 2026 and 2036
- Figure 75: Eastern Europe Market Y-o-Y Growth Comparison by Application, 2026-2036
- Figure 76: Eastern Europe Market Attractiveness Analysis by Application
- Figure 77: East Asia Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 78: East Asia Market Value Share and BPS Analysis by Component , 2026 and 2036
- Figure 79: East Asia Market Y-o-Y Growth Comparison by Component , 2026-2036
- Figure 80: East Asia Market Attractiveness Analysis by Component
- Figure 81: East Asia Market Value Share and BPS Analysis by Deployment, 2026 and 2036
- Figure 82: East Asia Market Y-o-Y Growth Comparison by Deployment, 2026-2036
- Figure 83: East Asia Market Attractiveness Analysis by Deployment
- Figure 84: East Asia Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 85: East Asia Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 86: East Asia Market Attractiveness Analysis by End User
- Figure 87: East Asia Market Value Share and BPS Analysis by Application, 2026 and 2036
- Figure 88: East Asia Market Y-o-Y Growth Comparison by Application, 2026-2036
- Figure 89: East Asia Market Attractiveness Analysis by Application
- Figure 90: South Asia and Pacific Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 91: South Asia and Pacific Market Value Share and BPS Analysis by Component , 2026 and 2036
- Figure 92: South Asia and Pacific Market Y-o-Y Growth Comparison by Component , 2026-2036
- Figure 93: South Asia and Pacific Market Attractiveness Analysis by Component
- Figure 94: South Asia and Pacific Market Value Share and BPS Analysis by Deployment, 2026 and 2036
- Figure 95: South Asia and Pacific Market Y-o-Y Growth Comparison by Deployment, 2026-2036
- Figure 96: South Asia and Pacific Market Attractiveness Analysis by Deployment
- Figure 97: South Asia and Pacific Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 98: South Asia and Pacific Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 99: South Asia and Pacific Market Attractiveness Analysis by End User
- Figure 100: South Asia and Pacific Market Value Share and BPS Analysis by Application, 2026 and 2036
- Figure 101: South Asia and Pacific Market Y-o-Y Growth Comparison by Application, 2026-2036
- Figure 102: South Asia and Pacific Market Attractiveness Analysis by Application
- Figure 103: Middle East & Africa Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 104: Middle East & Africa Market Value Share and BPS Analysis by Component , 2026 and 2036
- Figure 105: Middle East & Africa Market Y-o-Y Growth Comparison by Component , 2026-2036
- Figure 106: Middle East & Africa Market Attractiveness Analysis by Component
- Figure 107: Middle East & Africa Market Value Share and BPS Analysis by Deployment, 2026 and 2036
- Figure 108: Middle East & Africa Market Y-o-Y Growth Comparison by Deployment, 2026-2036
- Figure 109: Middle East & Africa Market Attractiveness Analysis by Deployment
- Figure 110: Middle East & Africa Market Value Share and BPS Analysis by End User, 2026 and 2036
- Figure 111: Middle East & Africa Market Y-o-Y Growth Comparison by End User, 2026-2036
- Figure 112: Middle East & Africa Market Attractiveness Analysis by End User
- Figure 113: Middle East & Africa Market Value Share and BPS Analysis by Application, 2026 and 2036
- Figure 114: Middle East & Africa Market Y-o-Y Growth Comparison by Application, 2026-2036
- Figure 115: Middle East & Africa Market Attractiveness Analysis by Application
- Figure 116: Global Market - Tier Structure Analysis
- Figure 117: Global Market - Company Share Analysis

