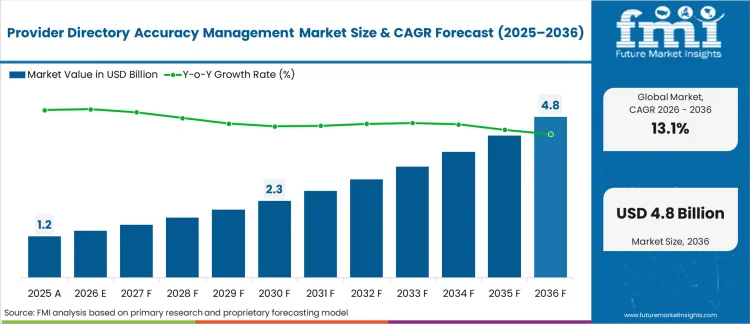
The provider directory accuracy management market was valued at USD 1.2 billion in 2025. The sector is set to reach USD 1.4 billion in 2026 at a CAGR of 13.11% during the forecast period. Sustained investment takes the market to USD 4.8 billion through 2036. The implementation of the No Surprises Act eliminates the era of passive provider roster management, forcing Medicare Advantage Organizations to actively validate network data or face crippling daily fines.
Health plans that delay transitioning from siloed credentialing databases to unified master data environments lose their ability to control out-of-network balance billing costs. The true operational failure point is rarely provider unresponsiveness; rather, it is the internal friction where distinct payer departments continuously overwrite each other's verified data. This structural reality makes advanced clinical data exchange platforms mandatory for surviving CMS network adequacy audits.
Health plan network managers must achieve real-time synchronization between internal credentialing systems and public-facing directories before CMS transitions from enforcement discretion to active, systematic auditing. This requires IT directors to deploy bi-directional APIs capable of parsing Electronic Medical Record updates instantaneously. Once this digital threshold is crossed, health plans permanently reduce the administrative overhead associated with manual outreach campaigns.
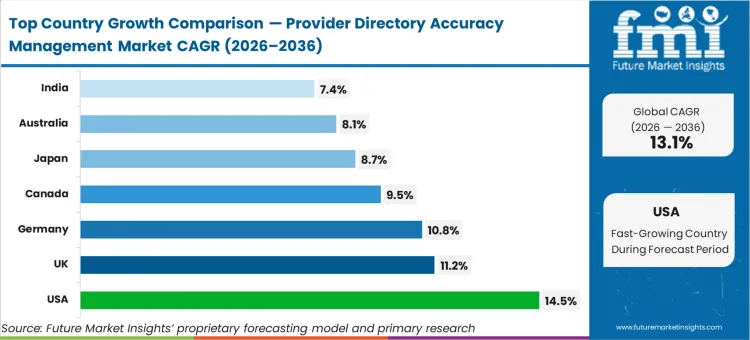
The United States advances at a 14.5% compound annual rate as strict mandates dictate immediate compliance architectures. The United Kingdom tracks an 11.2% CAGR as National Health Service trusts centralize fragmented regional registries. Germany grows at 10.8% driven by the Digital Healthcare Act pushing statutory insurers toward unified digital identities. Canada expands at 9.5% as provincial health ministries mandate standardized referral networks. Japan records an 8.7% rate as an ageing population stresses localized clinic discovery tools. Australia follows at 8.1% amidst private health fund modernization, while India posts a 7.4% expansion rate. This growth spread exists structurally because centralized, single-payer systems require vastly different data validation architectures than fragmented commercial markets.
| Metric | Details |
|---|---|
| Industry Size (2026) | USD 1.4 billion |
| Industry Value (2036) | USD 4.8 billion |
| CAGR (2026-2036) | 13.11% |
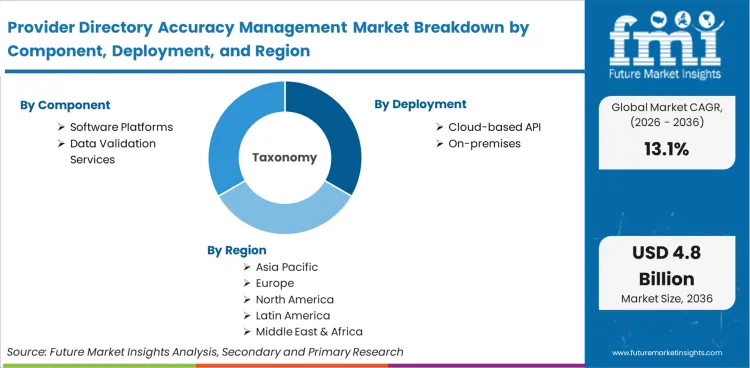
The Provider Directory Accuracy Management Market encompasses the software, platforms, and outsourced services utilized by healthcare payers to ingest, verify, and syndicate provider demographic and credentialing data. It fundamentally resolves the misalignment between internal payer contracting systems and public-facing physician rosters. The market is distinguished from general credentialing software by its exclusive focus on real-time network adequacy compliance, ensuring patients are not subjected to balance billing due to outdated directory listings.
Core inclusions consist of API-driven roster ingestion engines, continuous data validation platforms, automated physician outreach portals, and master data management systems built specifically for health plans. The market also includes proprietary data lakes that cross-reference external sources like the National Plan and Provider Enumeration System (NPPES) against internal payer records to establish a verifiable gold record for every practitioner.
The market explicitly excludes standalone Electronic Health Record (EHR) systems, general hospital billing software, and consumer-facing appointment scheduling apps like Zocdoc. It also excludes core claims adjudication platforms. These technologies are excluded because their primary function is clinical documentation or financial transaction processing, rather than the systematic validation of provider network participation data for regulatory compliance.
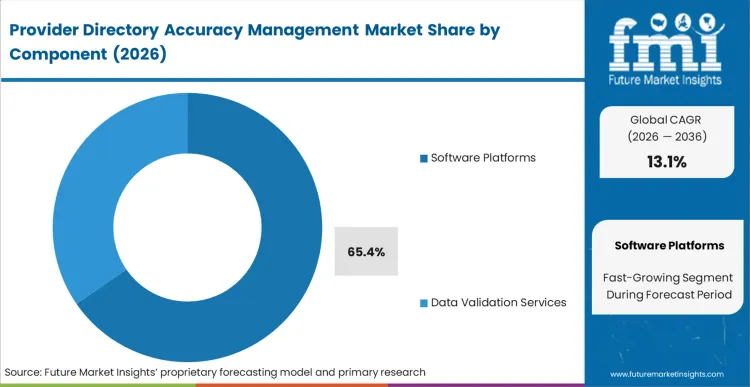
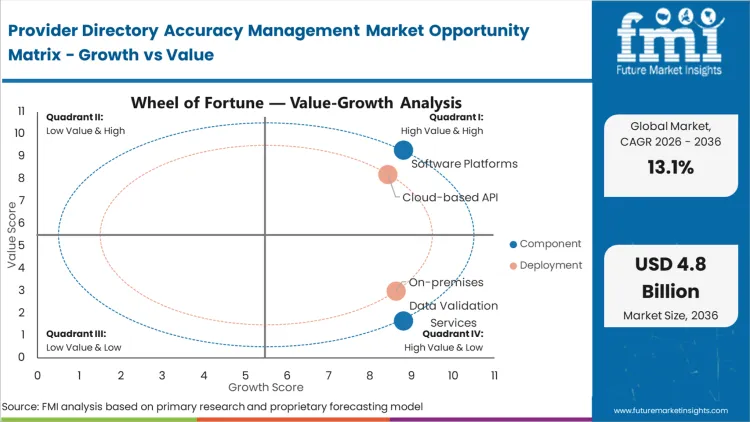
The manual dissemination of spreadsheets and bulk faxes is actively failing under the weight of the CMS two-day update mandate, positioning software platforms as the absolute requirement for compliance. Based on FMI's assessment, Software Platforms dominate with a 65.4% share in 2026 because human data entry cannot scale to meet 90-day rolling validation cycles across tens of thousands of practitioners. Health plan IT directors must replace batch processing with robotic process automation capable of continuous matching against external primary sources. If network operations teams attempt to meet requirements using legacy methods, they guarantee eventual systemic failure and subsequent regulatory fines.
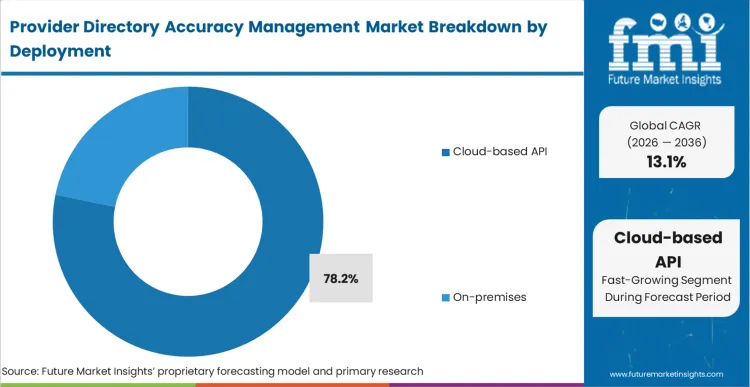
Cloud-based APIs hold a 78.2% share in 2026 due to the fundamental structural necessity of connecting disparate external data lakes directly to internal payer routing engines. FMI analysts opine that on-premises deployments are inherently unsuited for the bi-directional data flow required to keep public directories synchronized with live clinic realities. Cloud infrastructure allows vendor solutions to cross-reference National Plan and Provider Enumeration System (NPPES) updates in real-time. Systems integrators establishing this cloud infrastructure deployment enable payers to react instantaneously to provider location changes, averting the out-of-network billing liabilities associated with delayed manual uploads.
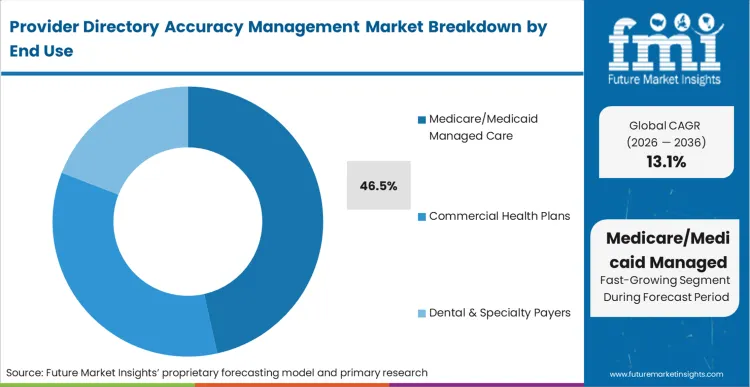
Medicare Advantage Organizations (MAOs) operate under direct threat of CMS star rating downgrades and civil monetary penalties for directory inaccuracies. This severe regulatory condition ensures Medicare/Medicaid Managed Care leads the segment with a 46.5% share in 2026. According to FMI's estimates, commercial plans face different but equally punitive pressures from the No Surprises Act, forcing them into rapid adoption, but MAOs remain the foundation of the market due to longer-standing audit frameworks. Dental network administrators are also compelled to upgrade capabilities as provider volatility increases. Government program directors who fail to deploy automated validation frameworks face immediate suspension of their ability to enroll new beneficiaries.
The rapid expansion of digital health ecosystems is shifting the competitive landscape for technology vendors, as payers and providers increasingly prioritize platforms capable of supporting longitudinal patient engagement. Instead of focusing solely on transactional data exchanges, organizations are investing in systems that integrate behavioral insights, population‑level trends, and predictive analytics to deliver personalized care pathways. This emerging model emphasizes proactive intervention, identifying risks before they escalate, while enabling care teams to coordinate seamlessly across virtual, in‑person, and community‑based settings. Companies that can unify these capabilities into a single, interoperable framework are positioned to define the next decade of healthcare innovation.
The primary operational friction restraining the market is the deep fragmentation of internal payer databases. Health plans typically operate separate, siloed systems for claims processing, provider credentialing, and network contracting, leading to scenarios where a validated update in one system is overwritten by outdated legacy data from another. The emerging workaround involves deploying overarching Master Data Management (MDM) layers to establish a "gold record," but this requires massive internal change management. This structural limit means even the best external validation software will fail if the payer's internal data governance remains disjointed.
Opportunities in the Provider Directory Accuracy Management Market
Based on the regional analysis, the Provider Directory Accuracy Management market is segmented into North America, Latin America, Europe, East Asia, South Asia, Oceania, and Middle East and Africa across 40 plus countries.
.webp)
| Country | CAGR (2026 to 2036) |
|---|---|
| United States | 14.5% |
| United Kingdom | 11.2% |
| Germany | 10.8% |
| Canada | 9.5% |
| Japan | 8.7% |
| Australia | 8.1% |
| India | 7.4% |
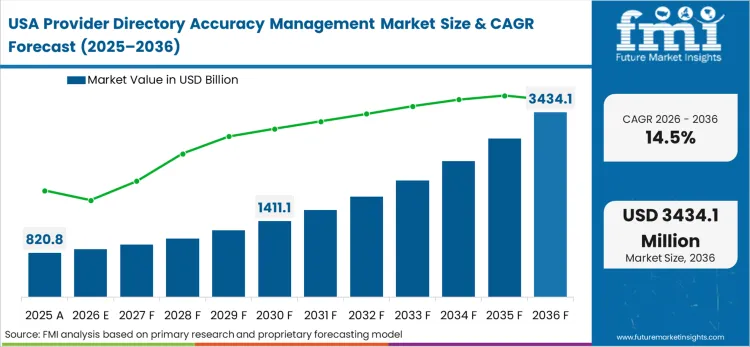
Regulations forces the absolute restructuring of payer directories across North America. Unlike regions experimenting with centralized registries, the privatized nature of the US healthcare system places the entire burden of data validation directly on individual commercial and Medicare insurers. Based on FMI's assessment, this necessitates the rapid deployment of massive, proprietary data lakes capable of syndicating updates across thousands of disconnected systems. Health plan executives operating within this punitive framework must invest in API-driven health informatics infrastructure or face catastrophic daily fines.
FMI's report includes comprehensive evaluation of Mexico and other Latin American healthcare ecosystems. The ongoing digitalization of private health insurance networks in these emerging economies relies heavily on adopting established data governance frameworks from their northern counterparts.
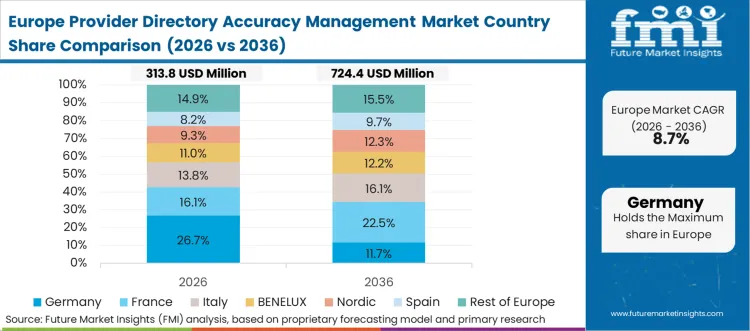
Specific policy directives regarding digital identity and secure data exchange drive the European dynamic, prioritizing patient data rights alongside provider accuracy. European health systems are deeply engaged in building centralized, state-sponsored registries rather than relying on fragmented commercial health plan directories. In FMI's view, this forces vendors to build solutions that integrate seamlessly with national digital health architectures rather than proprietary payer silos.
FMI's report includes detailed analysis of France, Italy, and the Nordics. Across these member states, the broader European Health Data Space initiative is accelerating the standardization of provider attributes.
Specific digital infrastructure investments and rapidly aging demographics dictate the transition toward advanced provider discovery tools in East Asia. As populations age, the necessity for accurate, hyper-localized clinic and specialist data becomes critical for daily healthcare access. FMI analysts opine that vendors succeeding in this region must optimize their platforms for mobile-first patient populations and deeply integrated regional health information exchanges.
FMI's report includes coverage of South Korea and Southeast Asia. The push for smart hospital ecosystems in these regions is heavily reliant on establishing foundational master data management for all medical personnel.
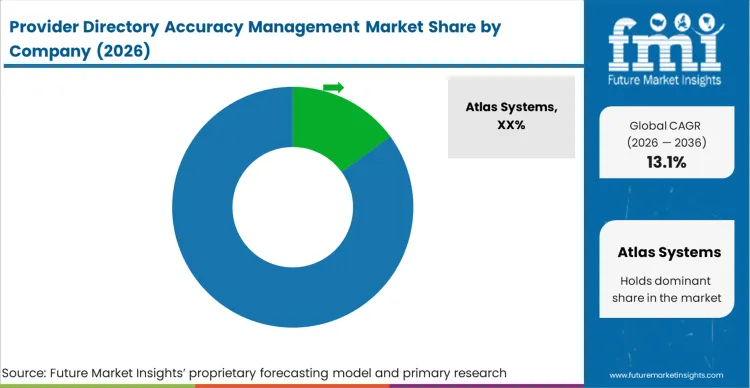
The Provider Directory Accuracy Management market is moderately consolidated around a few massive data aggregators and specialized software developers. This structure exists because creating a verifiable "gold record" requires aggregating billions of data points from primary sources, establishing a massive barrier to entry based on raw data access. Companies like LexisNexis Risk Solutions, CAQH, and ProviderTrust lead by offering vast, pre-validated proprietary data lakes. Buyers utilize the breadth and historical accuracy of these data lakes as the primary competitive variable to distinguish qualified enterprise vendors from smaller, unproven startups.
To disrupt these incumbents, a challenger must build capabilities that bypass the traditional "data lake" approach and instead focus on real-time extraction. Innovative firms are developing bi-directional APIs that read directly from hospital Electronic Health Records and credentialing software, updating the payer directory instantaneously without any manual intervention from the physician. Vendors demonstrating this level of frictionless bi-directional data syndication secure a massive structural advantage. Challengers entering this market must entirely solve the issue of "provider portal fatigue" to gain any significant traction.
Large health plans prevent vendor lock-in by establishing internal Master Data Management (MDM) systems that sit above any single vendor's validation tool. Buyers want control of their internal "gold record," while dominant vendors want payers fully reliant on their external proprietary data subscriptions. This tension limits the pricing power of data aggregators, forcing them to compete heavily on the speed and integration capabilities of their APIs. As the market progresses to 2036, it will become less concentrated around raw data providers and more competitive among workflow automation specialists who can effectively harmonize disparate internal payer systems.
| Metric | Value |
|---|---|
| Quantitative Units | USD 1.4 billion to USD 4.8 billion, at a CAGR of 13.11% |
| Market Definition | The market provides the digital infrastructure and data validation services health plans require to keep public provider directories synchronized with actual contracting status, eliminating surprise billing risks caused by inaccurate network rosters. |
| Component Segmentation | Software Platforms, Data Validation Services |
| Deployment Segmentation | Cloud-based API, On-premises |
| End User Segmentation | Commercial Health Plans, Medicare/Medicaid Managed Care, Dental & Specialty Payers |
| Regions Covered | North America, Latin America, Europe, East Asia, South Asia, Oceania, Middle East and Africa |
| Countries Covered | United States, United Kingdom, Germany, Canada, Japan, Australia, India, and 40 plus countries |
| Key Companies Profiled | Atlas Systems, LexisNexis Risk Solutions, InterSystems, ProviderTrust, Quest Analytics, SKYGEN, IQVIA, CAQH |
| Forecast Period | 2026 to 2036 |
| Approach | FMI analysts interviewed Chief Network Officers and Compliance Directors at major health plans. Forecasts rely on CMS enforcement timeline modeling, validated against the commercial adoption rates of API-driven roster management tools. |
This bibliography is provided for reader reference. The full FMI report contains the complete reference list with primary source documentation.
How large is the Provider Directory Accuracy Management Market in 2026?
The market is poised to reach USD 1.4 billion in 2026, driven directly by massive payer investments to avoid balance billing liabilities.
What will it be valued at by 2036?
It is projected to reach USD 4.8 billion by 2036 as manual roster updates become structurally impossible to maintain.
What CAGR is projected?
A 13.11% CAGR is projected, structurally supported by the strict 90-day verification mandates enforced by federal regulators.
Which Component segment leads?
Software Platforms lead with a 65.4% share in 2026, as algorithmic matching completely displaces legacy fax and phone-based outreach.
Which Deployment segment leads?
Cloud-based API deployment holds a 78.2% share, enabling the real-time syndication required to update directories within 48 hours.
Which End User segment leads?
Medicare/Medicaid Managed Care captures 46.5% of the market because MAOs face direct, severe civil monetary penalties for directory inaccuracies.
What drives rapid growth?
The regulations force health plans to guarantee accurate out-of-network status or absorb the resulting patient billing discrepancies.
What is the primary restraint?
Deep fragmentation within payer databases prevents external validation tools from establishing a permanent "gold record" when internal teams continuously overwrite data.
Which country grows fastest?
The United States grows fastest at 14.5%, directly reacting to the unparalleled punitive framework of the No Surprises Act.
How does the No Surprises Act impact this technology?
It explicitly mandates that commercial insurers verify provider network status every 90 days and update any changes within two business days.
Why are bi-directional APIs replacing provider portals?
Physicians experience severe administrative fatigue from updating multiple payer portals; APIs extract the data directly from EHRs without manual intervention.
How do large data aggregators dominate the landscape?
Incumbents rely on massive, proprietary data lakes built over decades, which provide payers an immediate accuracy uplift upon initial implementation.
Why is Master Data Management critical here?
Without an MDM layer to establish a single source of truth, claims, credentialing, and network teams will perpetually corrupt their own directories.
What role does AI play in directory management?
Machine learning algorithms detect anomalies, such as a practitioner listed at 15 simultaneous physical locations, before the error is published.
How does Medicare Advantage auditing differ from commercial plans?
MAOs face direct threats to their highly lucrative star ratings and federal bonus payments if they fail CMS secret-shopper network tests.
Why is the UK market growing at 11.2%?
The NHS is systematically attempting to centralize fragmented regional trust registries into unified digital infrastructure.
How do dental payers manage directory accuracy?
Dental network administrators use highly configurable MDM engines specifically designed to handle the high-turnover nature of clinic support staff.
Can robotic process automation solve the 48-hour update rule?
Yes, RPA is the only mathematically viable way to ingest, verify, and syndicate thousands of daily provider demographic changes within the CMS window.
What is the impact of National Provider Identifier (NPI) cross-referencing?
Platform vendors constantly cross-reference internal records against the federal NPPES database to ensure the foundational identity of the physician remains accurate.
Why are on-premises solutions losing market share?
They lack the elastic computing power and external connectivity required to execute real-time syndication with massive external credentialing databases.
How do vendors prevent provider portal fatigue?
They implement "validate once" frameworks that syndicate a single physician update across multiple health plans simultaneously.
What methodology supports the 13.11% forecast?
Growth models anchor to the total volume of active health plan networks multiplied by the minimum IT investment required to achieve regulatory compliance.
Full Research Suite comprises of:
Market outlook & trends analysis
Interviews & case studies
Strategic recommendations
Vendor profiles & capabilities analysis
5-year forecasts
8 regions and 60+ country-level data splits
Market segment data splits
12 months of continuous data updates
DELIVERED AS:
PDF EXCEL ONLINE

Thank you!
You will receive an email from our Business Development Manager. Please be sure to check your SPAM/JUNK folder too.