The wound healing ultrasound market is set to record a USD 495.9 million valuation in 2026, with scheduled treatment volume extending that base to USD 1,110.9 million by 2036 at an 8.4% CAGR. The constraint in this field is not equipment availability but therapist hours, room slots, and patient adherence to multi visit protocols. Devices earn their place by shortening sessions, reducing setup friction, and fitting into tightly booked care blocks. Departments standardize routines to keep staff rotation simple. Once a protocol is fixed, changing platforms creates scheduling risk rather than technical risk.
Revenue behavior in this segment follows patient throughput patterns, not capital cycles. Clinics expand capacity by adding shifts or rooms before they add new device types. Missed appointments and interrupted treatment courses shape realized utilization more than theoretical demand. Service interruptions carry an immediate opportunity cost because idle rooms still carry staff cost. Group operators prefer platforms that share probes and consumables across sites to keep logistics simple. Refurbishment and redeployment matter more than frequent replacement. Profit for suppliers follows fleet uptime, service response speed, and redeployment efficiency rather than headline feature sets.
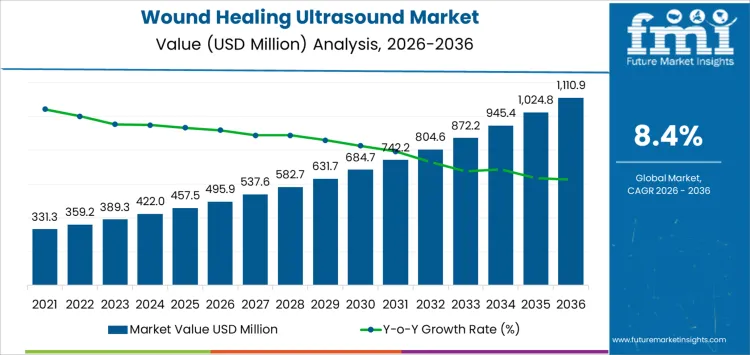
Care pathway design and reimbursement practice shape demand for the wound healing ultrasound market more than overall patient volumes. In 2026, at about USD 495.9 million, use is concentrated in chronic wound clinics, rehabilitation centers, and hospital outpatient departments where treatment protocols emphasize faster closure and lower complication risk. Device selection is tied to clinical guidelines and staff training programs, which fixes purchasing patterns across long equipment life cycles. Utilization rises as providers expand ultrasound assisted therapy into diabetic ulcers, pressure injuries, and post-surgical wounds. The steady increase reflects broader protocol adoption and more sites adding the modality to standard care pathways rather than rapid replacement of existing treatment equipment.
Evidence accumulation and service economics guide the later phase of the wound healing ultrasound market. As value approaches roughly USD 1,110.9 million by 2036, buyers focus on treatment consistency, device uptime, and ease of integration into daily clinic workflow. Manufacturers invest in durability, simplified interfaces, and service support networks as installed bases grow. The move from under five hundred million into the low one point three billion reflects accumulated placement across many care settings rather than a single change in clinical practice standards. Suppliers that combine clinical credibility, reliable equipment performance, and predictable support coverage tend to secure long term positions in wound care therapy portfolios.
| Metric | Value |
|---|---|
| Market Value (2026) | USD 495.9 million |
| Forecast Value (2036) | USD 1,110.9 million |
| Forecast CAGR 2026 to 2036 | 8.4% |
Wound healing ultrasound systems deliver low intensity acoustic energy to stimulate tissue repair in chronic and slow closing wounds. Clinics use them for diabetic foot ulcers, pressure injuries, and post-surgical sites where standard dressings fail to progress closure. Earlier care pathways relied on debridement, topical agents, and compression alone, which left many patients on long treatment cycles. Ultrasound therapy adds a physical stimulus that influences perfusion, cellular activity, and edema management. Providers specify equipment by output stability, applicator design, treatment protocols, and infection control compatibility. Use fits outpatient wound centers and hospital wards because sessions are short and repeatable. Adoption follows protocol reviews rather than equipment refresh cycles, since the modality changes visit structure and staffing patterns over time.
Purchasing decisions involve wound care directors, nursing leadership, and finance teams because treatment time and consumable use affect clinic capacity. Earlier deployments were limited to specialist centers, which kept volumes small and training informal. Current programs focus on standard protocols, shared devices across rooms, and documented outcomes for audit review. Manufacturers compete on applicator durability, calibration control, and service response rather than peak power claims. Providers evaluate total cost through visit counts, staff utilization, and healing progression, not device price alone. Reimbursement rules and coding clarity shape utilization patterns in each health system. Distributors add value through training and maintenance coverage. Demand tracks chronic disease and aging populations, where clinics seek shorter courses while keeping complication rates within targets defined.
Specification in Wound Healing Ultrasound Market is driven by clinical protocol selection, reimbursement positioning, and integration into wound care pathways rather than by routine device replacement. Once a therapy approach is adopted within a facility or network, equipment choice becomes part of standardized treatment algorithms and staff training programs. This links demand to expansion of wound care services, protocol updates, and consolidation of treatment centers. Segment structure reflects differences in energy delivery, treatment depth, and session duration. Buyers prioritize clinical evidence support, ease of use in outpatient settings, and predictable maintenance because therapy utilization depends on workflow fit and patient throughput. Volume development therefore follows service line growth and care model standardization rather than short term fluctuations in patient visits.
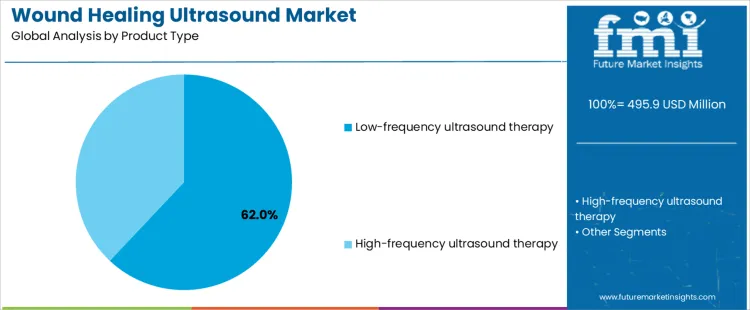
Low frequency ultrasound therapy represents about 62% of demand in the Wound Healing Ultrasound Market because it supports debridement, stimulation of tissue response, and management of chronic wound environments. These systems are integrated into routine wound care protocols and can be applied across a wide range of lesion types. High frequency ultrasound therapy serves more targeted applications focused on superficial tissue and diagnostic adjacent use, which limits its role in complex wound management. The two categories differ in power requirements, applicator design, and treatment time per session, which affects patient scheduling and staff utilization. Each type establishes distinct training requirements, maintenance routines, and consumable usage patterns.
From an operational and financial perspective, product type choice fixes the service delivery model. Low frequency systems support higher utilization across diverse cases, which improves equipment amortization. High frequency systems are used in narrower indications, resulting in lower utilization but simpler procedures. Once a clinic or hospital standardizes on a modality, changes are uncommon because protocols, reimbursement coding, and staff competencies are aligned to that choice. Demand by product type therefore follows clinical pathway adoption and evidence based guideline evolution rather than short term purchasing preferences.
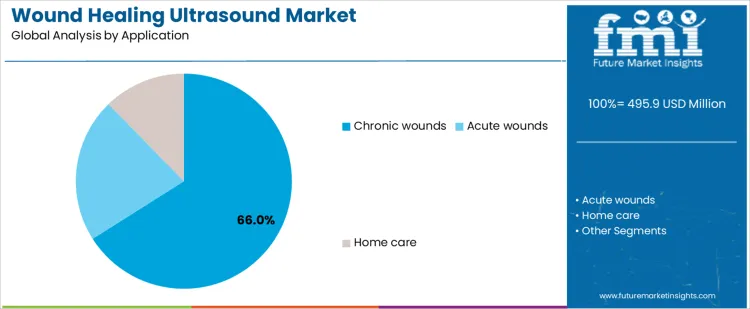
Chronic wounds account for about 66% of demand in the Wound Healing Ultrasound Market because these conditions require repeated interventions over extended treatment periods. This creates sustained utilization in specialized wound care clinics and outpatient departments. Acute wounds involve shorter treatment courses and are often managed through conventional methods, which limits device usage frequency. Home care represents a smaller but growing setting, where portability, ease of operation, and safety features influence adoption. These differences explain why equipment deployment concentrates in facilities managing long term wound populations rather than in general surgical or emergency care settings.
Application mix also shapes purchasing and deployment models. Chronic wound centers invest in equipment as part of long term service capability development. Acute care providers acquire devices selectively to support specific protocols. Home care providers require simplified systems and training support, which slows adoption and limits volume. The resulting demand structure concentrates utilization in chronic care environments while other settings contribute incremental growth. Segment shares therefore move with demographic trends, prevalence of chronic conditions, and organization of wound care services rather than with short term changes in injury incidence.
The Wound Healing Ultrasound Market is shaped by how reliably ultrasound therapy can be delivered within routine wound care protocols. Chronic wound treatment depends on repeated sessions, consistent dosing, and good patient compliance. Buyers focus on ease of use, treatment time, device reliability, and compatibility with existing wound care routines. Selection decisions involve wound care clinicians, nursing teams, and hospital procurement groups. This positions ultrasound therapy devices as part of daily clinical operations rather than as specialized equipment used only in limited cases, making workflow integration and treatment repeatability central to adoption decisions.
Wound care providers increasingly follow structured treatment pathways to ensure consistent outcomes across patients and care settings. This is changing expectations in the Wound Healing Ultrasound Market toward devices that support predictable treatment parameters and simple operation. Clinicians prefer systems that can be used across different wound types without complex setup. This reduces training burden and minimizes variation between operators. As a result, device evaluation focuses on treatment consistency, clear user guidance, and compatibility with existing documentation practices rather than on complex feature sets that are rarely used in routine care.
Ongoing treatment volume is being built in long-term care facilities, outpatient wound clinics, and home care programs that manage large numbers of chronic wound patients. These settings create repeat usage because patients require multiple treatment sessions over extended periods. The Wound Healing Ultrasound Market also benefits when providers expand service lines focused on diabetic foot ulcers, pressure injuries, and post-surgical wounds. There is opportunity for suppliers that support training, protocol development, and service programs. Being integrated into standard care pathways creates recurring device utilization and repeat consumable or service revenue.
Healthcare providers rely on clinical guidelines and reimbursement policies when adopting new therapies. If coverage is unclear or evidence is seen as insufficient, adoption slows. The Wound Healing Ultrasound Market faces scrutiny because clinicians must justify time and resource allocation for each therapy session. In addition, some providers remain comfortable with established treatment methods and are cautious about adding new modalities. Equipment cost, training needs, and scheduling impact also affect decisions. These factors keep usage concentrated in practices that already specialize in advanced wound care rather than across all care settings.
| Country | CAGR |
|---|---|
| USA | 11.2% |
| Brazil | 11.7% |
| China | 12.2% |
| India | 12.4% |
| Germany | 9.4% |
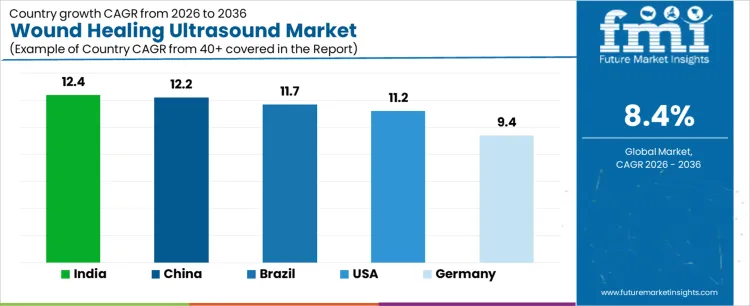
Demand for wound healing ultrasound is rising as hospitals and clinics expand advanced wound care programs for chronic ulcers, post-surgical wounds, and trauma cases. India leads with a 12.4% CAGR, supported by growing diabetes related wound burden, expansion of specialty wound care centers, and wider adoption in mid-sized hospitals. China follows at 12.2%, driven by large patient volumes, modernization of hospital equipment, and focus on reducing healing time and complications. Brazil records 11.7%, reflecting broader access to advanced wound management in private and public facilities. The USA grows at 11.2%, shaped by outpatient wound care clinics and reimbursement backed therapy adoption. Germany, at 9.4%, reflects structured uptake in a mature clinical environment.
Clinical pathway integration across hospital networks keeps wound care demand in the United States on an 11.2% CAGR path. Procurement decisions sit with wound care committees and capital review boards. Adoption focuses on chronic ulcers, post-surgical wounds, and diabetic foot management. Device choice emphasizes dosing control, treatment time, and documentation output for reimbursement files. Once a platform is approved, deployment expands across multiple sites inside the same network. Training programs and protocol alignment influence utilization rates. Import systems serve higher acuity centers. Local service coverage affects uptime planning. Spending follows clinic expansion and service line growth plans. Replacement cycles remain long. Commercial success depends on inclusion in standardized care pathways and reference programs rather than isolated department purchases today.
Private hospital investment and outpatient wound clinics keep Wound Healing Ultrasound Market demand in Brazil on an 11.7% CAGR path. Purchasing authority concentrates inside large hospital groups and specialty care chains. Use cases include pressure injuries, vascular ulcers, and trauma recovery. Device evaluation balances treatment throughput, reliability, and training burden. Import platforms dominate early deployments. Local distributors manage installation and clinical education. Once a system gains acceptance, rollout extends across affiliated centers. Reimbursement documentation and audit readiness influence utilization. Procurement timing aligns with clinic openings and service line upgrades. Public sector adoption remains slower. Replacement cycles stay long. Commercial success depends on access to leading groups and reference sites rather than broad distributor shelf presence or fragmented clinic sales today.
National chronic disease programs and hospital expansion keep Wound Healing Ultrasound Market demand in China on a 12.2% CAGR path. Tertiary hospitals and regional centers control most purchase decisions. Deployment targets diabetic foot care, post-operative recovery, and complex ulcers. Domestic suppliers cover standard systems while international brands serve advanced platforms. Tender processes and multi-year plans shape timing. Data capture and report formats influence selection. Training scale and service reach affect rollout speed. Once approved, systems are replicated across many sites. Spending follows facility upgrades and capacity growth. Replacement demand remains limited. Commercial success depends on placement inside public hospital catalogs and provincial programs rather than pursuit of small private clinics and long procurement cycles today across regions nationwide.
Network expansion of wound clinics and specialty hospitals keeps Wound Healing Ultrasound Market demand in India on a 12.4% CAGR path. Central medical committees and chain operators guide nominations. Use cases include diabetic ulcers, surgical wounds, and trauma recovery. Device choice emphasizes ease of use, training speed, and operating reliability. Import platforms serve higher acuity centers. Domestic suppliers address routine workloads. Procurement aligns with new clinic openings and capacity additions. Pilot programs precede wider rollout. Documentation requirements influence utilization. Service coverage affects uptime planning. Replacement cycles remain long. Commercial success depends on participation in chain level programs and reference deployments rather than selling to independent clinics and regional hospital groups during multi year expansion plans today across states nationwide programs.
Clinical guideline adoption and reimbursement discipline keep Wound Healing Ultrasound Market demand in Germany on a 9.4% CAGR path. University hospitals and large care centers control most purchases. Evaluation emphasizes evidence quality, treatment protocols, and documentation output. Procurement follows health technology assessment steps and budget cycles. Import suppliers dominate due to performance expectations. Once approved, systems deploy across departments with shared workflows. Training and audit readiness influence utilization. Spending aligns with quality improvement initiatives and outpatient expansion. Replacement cycles stay long. Data integration affects reporting efficiency. Commercial success depends on guideline inclusion and framework access rather than individual physician preference or small clinic buying and regional hospital networks under multiyear planning cycles today nationwide programs with steady funding approvals.
Wound healing ultrasound system selection follows clinical pathway design and nursing workflow rather than simple equipment comparison. Care teams define wound types, treatment frequency, bedside handling, and infection control steps before choosing devices. Misonix, Sanuwave, Smith and Nephew, Medtronic, Arobella compete through different clinical use cases and deployment models. Once a device enters protocols, staff training, consumable stocking, and documentation practices fix the platform. Misonix holds positions in debridement oriented workflows with established procedure sets. Sanuwave targets regenerative stimulation approaches for chronic wounds. Smith and Nephew links ultrasound tools with broader wound care portfolios. Medtronic approaches the field through hospital capital equipment relationships. Arobella focuses on compact systems for clinics and outpatient centers.
Competitive outcomes reflect clinical confidence, ease of use, and service coverage rather than headline technical claims. Committees examine evidence strength, treatment time, patient tolerance, and cleaning procedures during evaluation. Nursing managers value devices that fit ward routines and reduce handling complexity. Procurement teams review consumable usage, maintenance intervals, and training burden. Misonix benefits from established placement in surgical and advanced wound care settings. Sanuwave secures interest where regenerative protocols guide therapy choices. Smith and Nephew gains leverage through integrated dressing and therapy programs. Medtronic holds positions in institutions that standardize capital equipment sourcing. Arobella competes in cost sensitive outpatient environments that require portable systems. Market positions vary by care setting, reimbursement rules, and clinical governance models.
| Items | Values |
|---|---|
| Quantitative Units (2026) | USD Million |
| Product Type | Low-frequency ultrasound therapy; High-frequency ultrasound therapy |
| Application | Chronic wounds; Acute wounds |
| End User | Hospitals; Wound care clinics; Home care |
| Region | Asia Pacific; Europe; North America; Latin America; Middle East & Africa |
| Countries Covered | United States, Canada, Mexico, Germany, United Kingdom, France, Italy, Spain, Nordic, BENELUX, China, Japan, South Korea, India, Australia & New Zealand, ASEAN, Brazil, Chile, Saudi Arabia, Turkey, South Africa, Rest of regions |
| Key Companies Profiled | Misonix; Sanuwave; Smith & Nephew; Medtronic; Arobella |
| Additional Attributes | Dollar by sales by product type and application, installed base by care setting, utilization rate by clinic type, service and maintenance intensity, reimbursement driven adoption patterns, training and protocol standardization impact, redeployment and refurbishment flows, uptime and session throughput metrics |
How big is the wound healing ultrasound market in 2026?
The global wound healing ultrasound market is estimated to be valued at USD 495.9 million in 2026.
What will be the size of wound healing ultrasound market in 2036?
The market size for the wound healing ultrasound market is projected to reach USD 1,110.9 million by 2036.
How much will be the wound healing ultrasound market growth between 2026 and 2036?
The wound healing ultrasound market is expected to grow at a 8.4% CAGR between 2026 and 2036.
What are the key product types in the wound healing ultrasound market?
The key product types in wound healing ultrasound market are low-frequency ultrasound therapy and high-frequency ultrasound therapy.
Which application segment to contribute significant share in the wound healing ultrasound market in 2026?
In terms of application, chronic wounds segment to command 66.0% share in the wound healing ultrasound market in 2026.
Full Research Suite comprises of:
Market outlook & trends analysis
Interviews & case studies
Strategic recommendations
Vendor profiles & capabilities analysis
5-year forecasts
8 regions and 60+ country-level data splits
Market segment data splits
12 months of continuous data updates
DELIVERED AS:
PDF EXCEL ONLINE

Thank you!
You will receive an email from our Business Development Manager. Please be sure to check your SPAM/JUNK folder too.