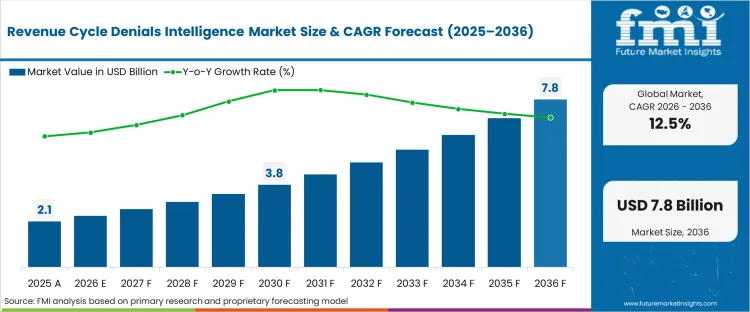
The revenue cycle denials intelligence market was valued at USD 2.1 billion in 2025 and is projected to reach USD 2.4 billion in 2026, reflecting a CAGR of 12.5%. Continued investment is expected to drive market expansion to USD 7.8 billion by 2036, as healthcare providers adopt advanced intelligence solutions to counter increasingly automated payer claim denials and preserve collection performance.
Revenue cycle directors are currently forced to decide between bolting third-party intelligence modules onto legacy electronic health records or migrating entire financial operations to unified platforms. The stakes of delaying this architectural choice materialize as deteriorating days in accounts receivable, as legacy human-in-the-loop triage fails against automated payer adjudication. While standard metrics track recovery rates, predictive billing workflows reveal that the actual financial leakage occurs in the hidden administrative cost of the appeal process itself.
Growth becomes self-reinforcing only when real-time clinical natural language processing fully integrates with 835/837 EDI feeds. Health system Chief Information Officers trigger this inflection by abandoning batch-file claims processing in favor of pre-submission algorithmic clearance. Once this architectural gate is crossed, health systems shift from retrospective recovery to proactive margin defense.
India is estimated to advance at 15.5%, leading the geographic expansion as outsourced Global Capability Centers handling Western claims deploy advanced toolsets to manage rising transaction volumes. Brazil tracks at 14.8%, followed by China expanding at 14.2% as large urban hospital networks transition from manual ledger systems directly to automated claim tracking. Germany follows at 13.5% and the UK at 12.8%, where centralized procurement frameworks push regional health trusts toward standardized financial clearance protocols. Japan expands at 11.8%, while the USA registers 11.2% growth. The divergence across this range reflects a strict separation between markets optimizing outsourced labor productivity and those defending against aggressive commercial payer algorithms.
| Metric | Details |
|---|---|
| Industry Size (2026) | USD 2.4 billion |
| Industry Value (2036) | USD 7.8 billion |
| CAGR (2026-2036) | 12.50% |
Revenue Cycle Denials Intelligence encompasses the software algorithms and analytical frameworks deployed by healthcare providers to predict, identify, and resolve rejected or unpaid medical claims. It is functionally distinct from standard medical billing software because it does not merely route claims; it applies machine learning to historical adjudication data to identify root-cause failure patterns and simulate payer responses before submission.
The scope includes predictive denial modeling software, automated claim tracking applications, retrospective denial analysis platforms, and specialized consulting services directly tied to algorithm implementation. The inclusion of healthcare payer interoperability components is restricted to modules specifically functioning to translate payer remittance advice into actionable provider workflows.
Basic electronic health record systems without predictive financial capabilities are explicitly outside the scope. Standard debt collection software and patient-facing payment portals are excluded because their functional boundary addresses patient-responsibility revenue rather than commercial or government payer adjudication friction.
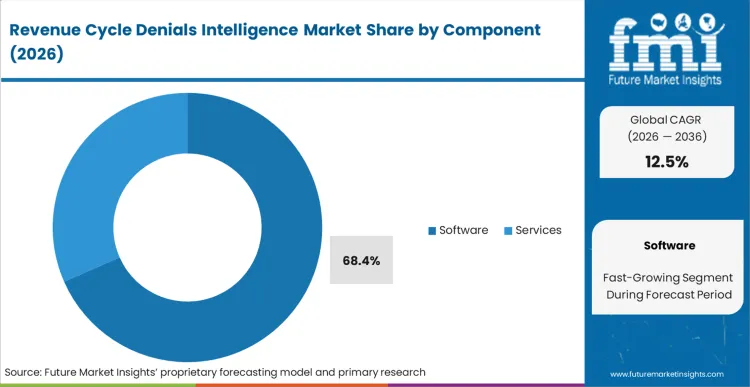
Manual ledger review and basic rules engines failed to keep pace as commercial payers transitioned to algorithmic adjudication. Software holds 68.4% of the industry because human-in-the-loop triage is mathematically unscalable against the volume of automated 835/837 EDI denials generated by modern payer systems.
According to FMI's estimates, Chief Financial Officers now prioritize software that autonomously maps denial codes back to the originating clinical documentation. This intelligence layer shifts the billing department's function from individual claim correction to systemic workflow redesign. Facilities relying on legacy manual appeals face insurmountable administrative costs that rapidly consume the margins of recovered claims. A medical billing infrastructure that lacks this predictive software component operates at a permanent structural disadvantage.
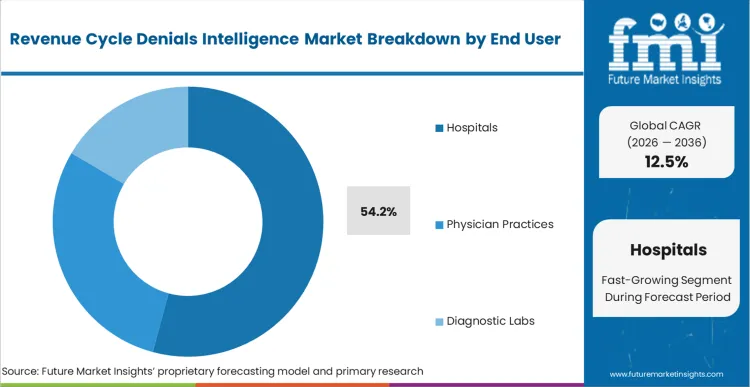
High-acuity medical facilities face the immediate operational choice between scaling their administrative headcount or automating their clearance protocols. Hospitals dominate this dimension with 54.2% share, driven entirely by their concentration of complex, multi-day inpatient claims that attract the highest rate of payer scrutiny.
In FMI's view, the sheer density of clinical data generated during a hospital stay creates an exponentially higher probability of coding discrepancies compared to outpatient encounters. Revenue cycle directors at these institutions use intelligence tools to simulate payer audits before the claim ever leaves the facility. Failure to intercept these discrepancies pre-submission results in cash-flow bottlenecks that can threaten a hospital's daily operational liquidity.
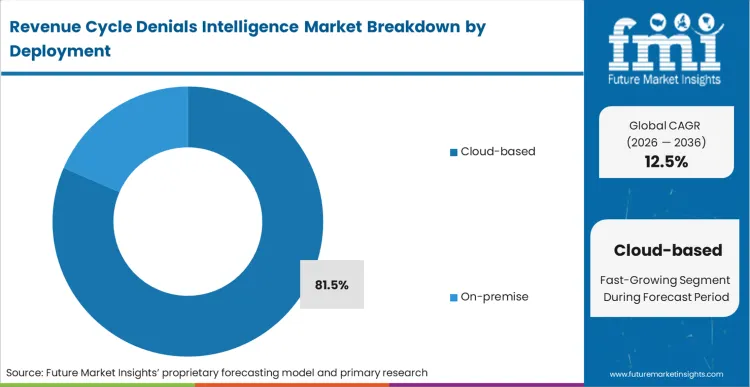
The commercial consequence of hardcoded, on-premise rules engines is their inability to update when external payers alter their adjudication logic. Cloud-based deployment captures 81.5% share because continuous algorithm updates are structurally mandatory to match shifting payer rules. Revenue cycle directors mandate cloud architectures to ensure their predictive models learn from denial patterns aggregated across thousands of cloud computing healthcare networks, rather than just their own isolated facility data. As per FMI's projection, this shared intelligence creates a network effect where a denial code generated in one state instantly trains the clearance algorithm for a hospital in another. Facilities trapped on legacy on-premise servers bear the entire cost of discovering new payer denial tactics through lost revenue.
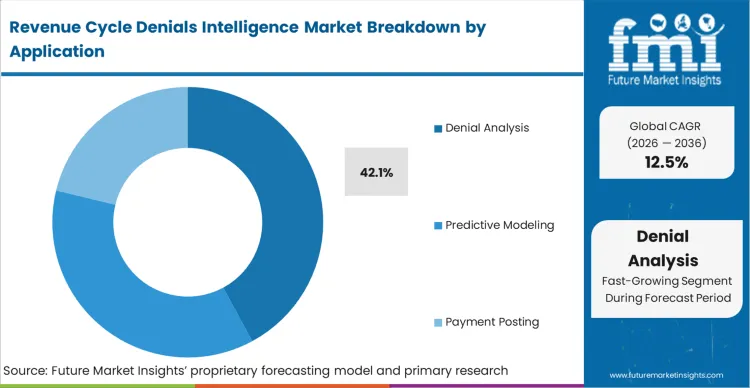
By 2036, the practice of waiting for a claim to reject before analyzing it will be viewed as an architectural failure. Denial Analysis currently leads with 42.1% share, providing the foundational root-cause visibility required before advanced predictive models can be trained. FMI analysts opine that health networks must first understand their historical failure modes before they can trust algorithms to clear claims autonomously. This application isolates exactly which physicians, codes, and payer combinations cause the most financial friction. Operations heads who ignore this analytical baseline and attempt to jump straight to automated posting end up scaling their existing errors rather than eliminating them.
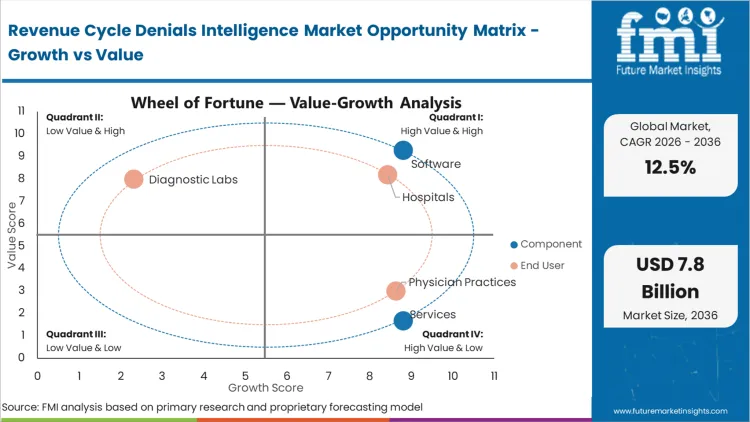
The structural shift from retrospective recovery to proactive margin defense requires revenue cycle directors to eliminate the administrative cost of the appeal process itself. As commercial payers increasingly deploy unannounced machine learning algorithms to auto-deny claims, human billing staff cannot process the volume of rejection codes quickly enough to prevent days in accounts receivable from ballooning. This forces Chief Financial Officers to procure intelligence layers that simulate payer adjudication pre-submission, shifting the operational focus from recovering lost money to ensuring the claim never fails the initial algorithmic check.
The primary friction slowing adoption is the existence of deeply siloed clinical and financial data lakes within legacy provider networks. Finance departments frequently purchase predictive algorithms that lack the structural access to read the clinical physician notes required to validate a complex claim. This architectural disconnect means the algorithm can flag a potential denial but cannot automatically append the missing clinical context. While clinical documentation improvements exist, their integration requires massive IT governance overhauls that paralyze procurement cycles.
Based on the regional analysis, the Revenue Cycle Denials Intelligence market is segmented into North America, Europe, Asia Pacific, and other regions across 40 plus countries.
.webp)
| Country | CAGR (2026 to 2036) |
|---|---|
| India | 15.5% |
| Brazil | 14.8% |
| China | 14.2% |
| Germany | 13.5% |
| UK | 12.8% |
| Japan | 11.8% |
| USA | 11.2% |
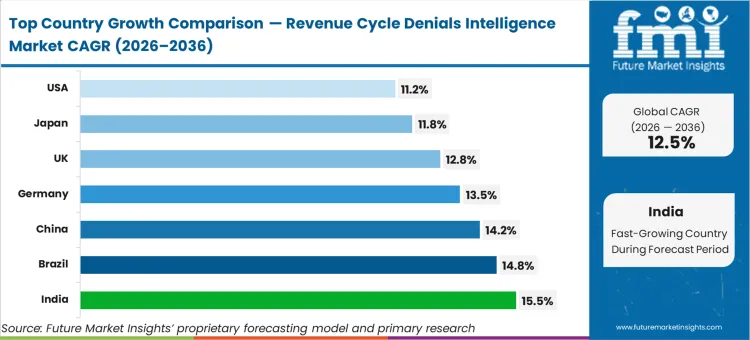
Cost structures, operating margins, and the aggressive posture of commercial insurance carriers dictate the architectural choices of healthcare networks in this region. The extreme fragmentation of payer rules forces facilities to invest heavily in predictive clearance just to maintain baseline solvency. Based on FMI's assessment, networks that rely on manual ledger review are rapidly absorbed by larger, tech-enabled health systems due to insurmountable administrative overhead. Fraud analytics frameworks overlap heavily with denial intelligence here, creating a high barrier to entry for generalized software vendors.
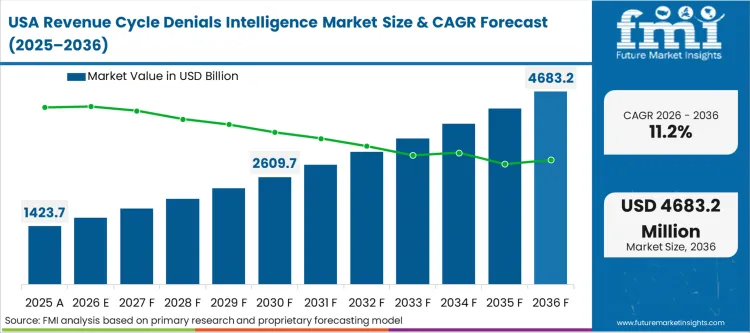
FMI's report includes Canada and Mexico. The cross-border expansion of managed care models from the USA forces these adjacent networks to begin establishing basic electronic tracking infrastructures.
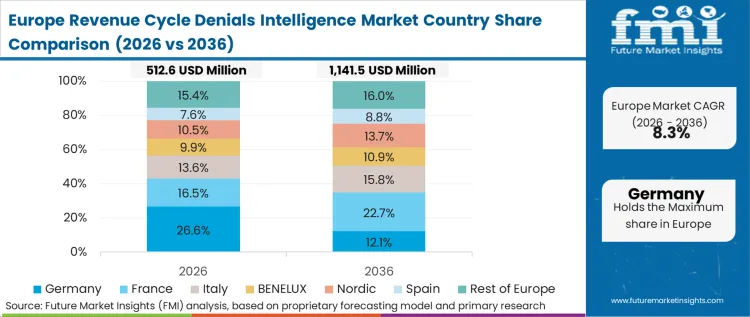
The regulatory environment and centralized procurement frameworks shape how intelligence platforms are deployed across these single-payer and hybrid systems. Unlike regions fighting commercial payer algorithms, European adoption is driven by strict government mandates demanding transparency in hospital resource allocation. In FMI's view, software is implemented primarily to ensure compliance with clinical coding standards rather than to maximize competitive revenue recovery.
FMI's report includes France, Italy, and Spain. Across these heavily regulated networks, procurement cycles prioritize vendors offering native interoperability with existing national health databases over proprietary standalone predictive capabilities.
The digital infrastructure condition of this region heavily skews its adoption pattern, sharply dividing highly scaled outsourcing hubs from rapidly modernizing domestic hospital networks. Large-scale healthcare BPO operations dominate the software consumption, utilizing advanced algorithms to process massive volumes of Western claims. As per FMI's projection, domestic facilities are leapfrogging legacy on-premise servers entirely, adopting cloud-based intelligence from day one.
FMI's report includes South Korea and Australia. These markets demonstrate a high readiness for automated pre-authorization modules, driven by government initiatives to digitize the entire patient financial journey.
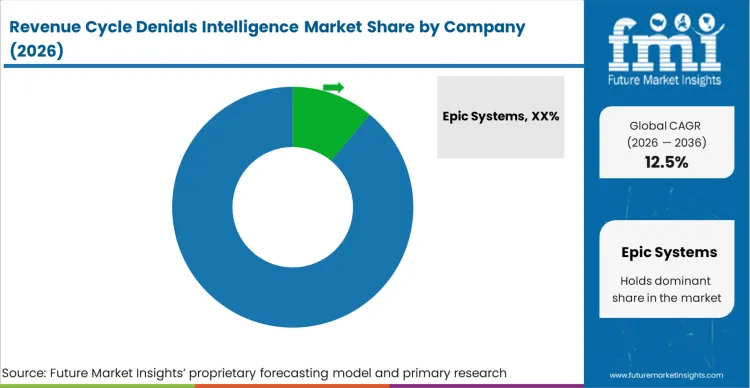
The architectural requirement to integrate directly with core electronic health records drives the concentrated nature of this market at the platform level. Buyers distinguish qualified from unqualified vendors entirely on their ability to ingest and normalize data from legacy systems and Epic Systems without requiring custom API engineering for every hospital wing. A vendor offering a theoretically superior predictive algorithm will be disqualified immediately if it requires the hospital's internal IT department to manually route the daily EDI feeds.
Incumbents such as Experian Health maintain their structural advantage through the sheer volume of historical adjudication data they process daily. This massive data lake allows their machine learning models to identify subtle shifts in payer algorithms weeks before a smaller competitor's model would even trigger an alert. To replicate this, a challenger must build proprietary data-sharing consortiums among mid-tier hospitals to aggregate enough baseline training data to make their predictive revenue integrity software viable.
Large hospital networks resist vendor lock-in by demanding modularity, purchasing base platforms from dominant EHR providers while sourcing specialized, high-performance denial algorithms from niche developers. This structural tension between the hospital's desire for best-of-breed analytics and the incumbent's incentive to bundle closed-ecosystem tools will define the competitive trajectory through 2036. The market remains concentrated at the data-routing layer but highly fragmented in the deployment of specialty-specific predictive models.
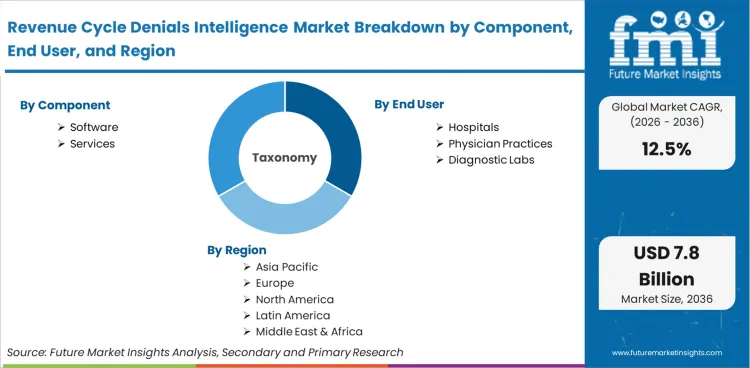
| Metric | Value |
|---|---|
| Quantitative Units | USD 2.4 billion to USD 7.8 billion, at a CAGR of 12.50% |
| Market Definition | The software algorithms and analytical frameworks deployed by healthcare providers to predict, identify, and resolve rejected or unpaid medical claims by simulating payer adjudication logic. |
| Component Segmentation | Software, Services |
| End User Segmentation | Hospitals, Physician Practices, Diagnostic Labs |
| Deployment Segmentation | Cloud-based, On-premise |
| Application Segmentation | Claim Tracking, Denial Analysis, Predictive Modeling, Payment Posting |
| Regions Covered | North America, Europe, Asia Pacific, Latin America, Middle East & Africa |
| Countries Covered | India, Brazil, China, Germany, UK, Japan, USA, and 40 plus countries |
| Key Companies Profiled | Epic Systems, Experian Health, Waystar, R1 RCM, AGS Health, Conifer Health Solutions |
| Forecast Period | 2026 to 2036 |
| Approach | Interviews with hospital CFOs and revenue cycle directors. Baseline models anchored to verifiable clearinghouse electronic transaction volumes. Forecasts validated against publicly reported IT capital expenditure of major health networks. |
This bibliography is provided for reader reference. The full FMI report contains the complete reference list with primary source documentation.
How large is the Revenue Cycle Denials Intelligence in 2026?
The valuation hits USD 2.4 billion. This figure represents the immediate capital deployed by health networks to defend against the rising volume of unannounced commercial payer algorithm updates.
What will it be valued at by 2036?
The sector reaches USD 7.8 billion. This trajectory signals a total operational shift from managing manual appeals to sustaining continuous, pre-submission algorithmic clearance architectures.
What CAGR is projected?
The 12.50% CAGR reflects the speed of the algorithmic arms race. It is constrained only by the ability of legacy hospital IT departments to modernize their deeply siloed clinical and financial data lakes.
Which Component segment leads?
Software holds 68.4% share. Human billing staff physically cannot review and map the daily volume of automated 835/837 EDI rejection codes without a predictive machine learning layer.
Which End User segment leads?
Hospitals dominate with 54.2% share. Their concentration of complex, multi-day inpatient care episodes generates the highest density of clinical variables, attracting maximum payer scrutiny.
Which Deployment segment leads?
Cloud-based systems command 81.5% share. Revenue cycle directors mandate cloud architectures to ensure their predictive models are continuously retrained by denial patterns aggregated across thousands of external facilities.
What drives rapid growth?
Growth is driven by commercial payers deploying machine learning to auto-deny claims. This forces Chief Financial Officers to procure opposing intelligence layers to prevent cash-flow bottlenecks and maintain baseline collection rates.
What is the primary restraint?
The structural disconnect between clinical and financial data lakes. Predictive algorithms frequently flag potential coding anomalies but lack the architectural access to automatically read unstructured physician notes to correct them.
Which country grows fastest?
India advances at 15.5%, followed by Brazil at 14.8%. India's acceleration is driven by outsourced Global Capability Centers deploying high-volume AI tools, whereas Brazil relies on modernizing deeply fragmented domestic billing networks.
How do government procurement directives shape European adoption?
In markets like the UK, centralized NHS mandates obligate regional trusts to adopt standardized tracking software. The goal is to eliminate internal administrative waste associated with internal funding requests, rather than fighting commercial insurers.
Why is real-time NLP integration critical for hospitals?
Legacy platforms wait for a claim to reject before analyzing it. Natural language processing intercepts incomplete physician notes during the patient encounter, forcing clinical addendums before the billing department ever processes the file.
How do niche developers compete against major EHR providers?
Massive EHR incumbents dominate the data-routing platform layer. Challengers bypass this by offering highly specialized, specialty-specific predictive models trained on localized regional payer adjudication histories that general platforms miss.
What specific operational bottleneck does Denial Analysis solve?
Denial Analysis isolates exactly which provider, code, and payer combination causes routine friction. Operations heads use this baseline visibility to restructure the workflow before they deploy automated models, preventing the scaling of existing errors.
Why do manual ledger systems fail in the current environment?
Manual systems rely on retrospective recovery. When commercial payers deploy auto-adjudication, the administrative cost of human staff appealing individual claims quickly exceeds the margin of the recovered revenue.
How do Global Capability Centers impact software consumption?
GCCs handling outsourced Western claims operate on razor-thin margins and massive volumes. They consume advanced software to ensure their labor force only interacts with claims that strictly require complex human intervention.
Why are cloud systems favored in total cost of ownership comparisons?
On-premise servers hide the massive continuous IT costs of model retraining. Cloud systems shift the burden of algorithmic updates entirely to the vendor, ensuring hospitals always run logic matching the latest payer shifts.
What forces physician practices to adopt predictive tracking?
Smaller practices face shrinking appeal windows and lack the cash reserves to absorb delayed payments. They adopt automated tracking because outsourcing their rising denial volume to third-party collection agencies becomes financially unsustainable.
How does predictive modeling change the procurement timeline?
Procurement shifts from buying periodic software updates to subscribing to continuous intelligence feeds. Hospitals demand proof that a vendor's algorithm can adapt to mid-year commercial payer logic changes without requiring manual IT intervention.
What happens to facilities that delay integration?
They suffer deteriorating days in accounts receivable. As their manual appeals fail against automated payer checks, they forfeit access to preferred procurement networks that demand strict electronic financial clearance.
How do updated EHR and regional compliance standards affect billing?
Strict federal reimbursement criteria, such as Germany's hospital financing legislation, penalize poor documentation. This forces facilities to use denial intelligence to align exactly with state regulations to secure their operational funding.
Why are value-based care payments driving intelligence adoption?
Value-based contracts require precise tracking of patient outcomes against cost. Algorithms ensure that complex episodes of care are coded correctly the first time, preventing funding clawbacks from managed care organizations.
What makes the USA market structurally unique?
The USA features extreme payer fragmentation. Hospital CFOs must continuously retrain models to anticipate unannounced logic shifts from dozens of different major commercial insurers simultaneously, driving intense continuous software investment.
Full Research Suite comprises of:
Market outlook & trends analysis
Interviews & case studies
Strategic recommendations
Vendor profiles & capabilities analysis
5-year forecasts
8 regions and 60+ country-level data splits
Market segment data splits
12 months of continuous data updates
DELIVERED AS:
PDF EXCEL ONLINE

Thank you!
You will receive an email from our Business Development Manager. Please be sure to check your SPAM/JUNK folder too.