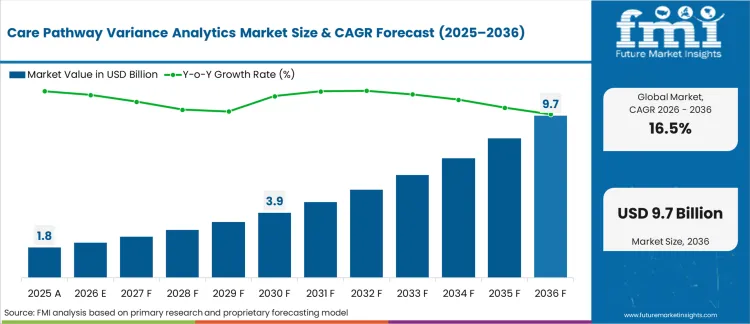
The care pathway variance analytics market reached USD 1.8 billion in 2025, driven primarily by mounting margin pressures associated with value‑based care penalties and payer denials. In response, hospital CFOs are prioritizing the adoption of pathway‑tracking solutions to mitigate near‑term revenue cycle risks and enforce cost discipline. The market is projected to expand at a 16.50% CAGR through 2036, reaching USD 9.7 billion, supported by the shift toward real‑time algorithmic decision support and the gradual replacement of retrospective clinical auditing.
Health systems that delay implementation risk losing leverage in negotiating favourable risk‑sharing agreements as standardized variance‑tracking capabilities become a contractual expectation.This commercial consequence compels institutions to abandon static order sets in favour of dynamic analytics that flag protocol deviations at the point of care. Real-time intervention capabilities differentiate advanced analytics platforms from legacy reporting tools.
| Metric | Details |
|---|---|
| Industry Size (2026) | USD 2.1 billion |
| Industry Value (2036) | USD 9.7 billion |
| CAGR (2026-2036) | 16.50% |
The integration of predictive algorithms into the physician's electronic workflow at the moment of order entry represents the critical inflection point. Clinical directors must intercept unjustified protocol deviations within the short diagnostic window before expensive procedures commence. Maturation of this capability transforms variance analytics from a backend administrative function into a frontline clinical navigation system.
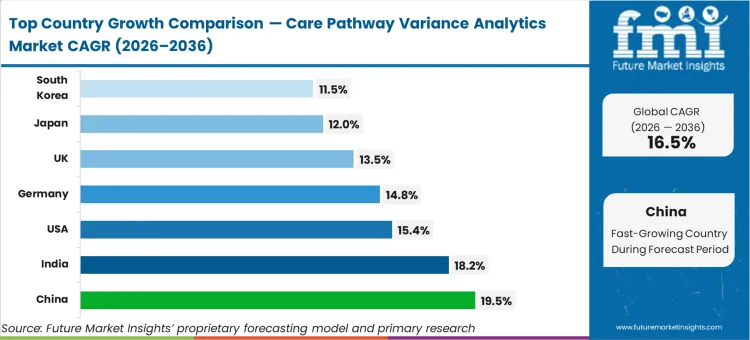
China advances at a 19.5% compound rate to 2036 driven by aggressive public hospital modernization mandates. India tracks at 18.2% as private tertiary networks expand evidence-based medicine frameworks. The United States grows at a 15.4% pace anchored by federal accountable care regulations. Germany expands at 14.8% while the UK follows at 13.5%. Japan records a 12.0% expansion, and South Korea posts an 11.5% trajectory. This geographic dispersion remains structural as diverse national reimbursement policies uniformly penalize unstandardized clinical delivery.
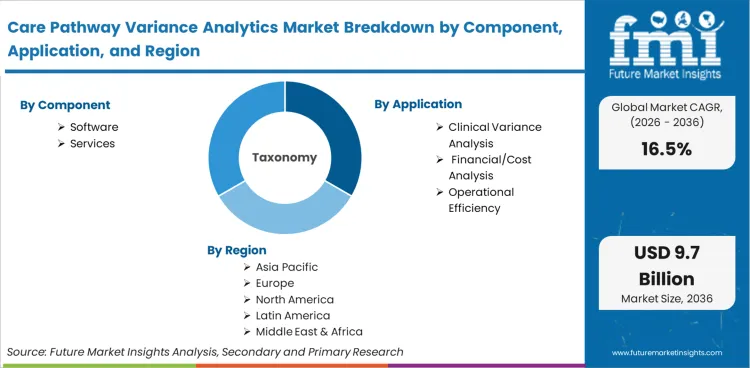
Care pathway variance analytics encompasses specialized software platforms and methodologies designed to measure actual clinical delivery against standardized evidence-based protocols. The ecosystem isolates unwarranted diagnostic, therapeutic, and length-of-stay deviations to quantify their impact on patient outcomes and episode costs, distinguishing this discipline from generalized hospital business intelligence.
The market scope includes clinical decision support engines, retrospective episode groupers, and cost-accounting algorithms mapped to specific disease pathways. Integration modules connecting electronic health records to predictive healthcare business intelligence dashboards fall within these boundaries. Advanced neural networks trained to identify positive clinical deviations for protocol updates are fully incorporated.
General ledger accounting software lacking clinical context and standalone electronic health record systems without dedicated variance tracking modules are excluded. Broad population health management tools that do not analyse specific intra-episode protocol adherence fall outside the defined parameters. Independent physician credentialing systems are explicitly omitted from the valuation.
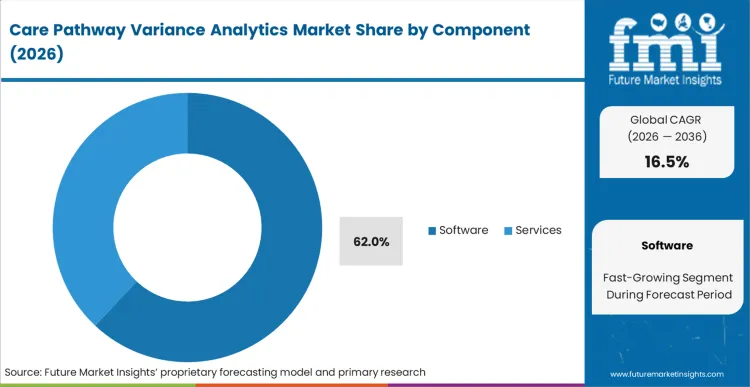
Dominating the investment domain, software commands a 62.0% share in 2026 as health systems prioritize scalable algorithmic engines over manual consulting reviews. Chief medical informatics officers demand automated platforms capable of ingesting vast unstructured clinical narratives to detect subtle protocol deviations. According to FMI's estimates, facilities transitioning to native virtual sleep clinics and broader variance tracking software realize measurable reductions in unnecessary diagnostic testing. The reliance on algorithmic processing eliminates the latency inherent in retrospective chart audits. Hospital administrators lacking automated detection capabilities face insurmountable manual labor costs when defending treatment choices against payer audits.
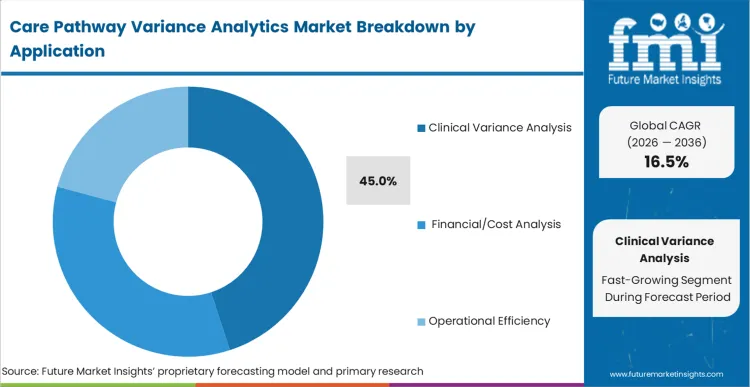
Retrospective financial reporting tools are failing, and an organized replacement toward clinical variance analysis is underway. This application holds a 45.0% share in 2026 as medical directors demand actionable insights into physician prescribing behaviour. Integrating these tools into value-based healthcare services frameworks ensures adherence to evidence-based medicine. By identifying the exact clinical moments where costs diverge from outcomes, these applications empower targeted intervention. FMI's research confirms that hospitals utilizing these applications rapidly eliminate low-value clinical practices. Network executives failing to implement standardized variance tracking forfeit their ability to negotiate shared-savings contracts with major insurers.
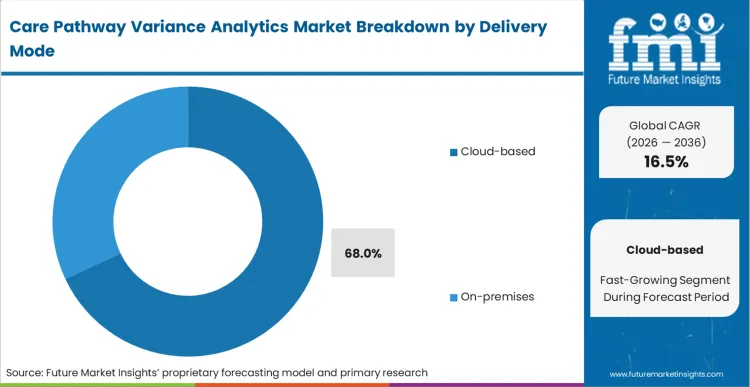
The absolute necessity of integrating disparate data streams forces hospitals to adopt cloud-based delivery, capturing 68.0% of the market in 2026. Health system chief information officers abandon isolated on-premises servers to facilitate seamless data exchange between acute and post-acute care settings. Based on FMI's assessment, cloud architecture provides the elastic computing power required to run complex predictive algorithms across millions of patient records simultaneously. This deployment model dramatically accelerates the implementation timeline for newly acquired community hospitals. IT directors resisting cloud migration face severe data silo constraints that critically compromise enterprise-wide quality reporting.
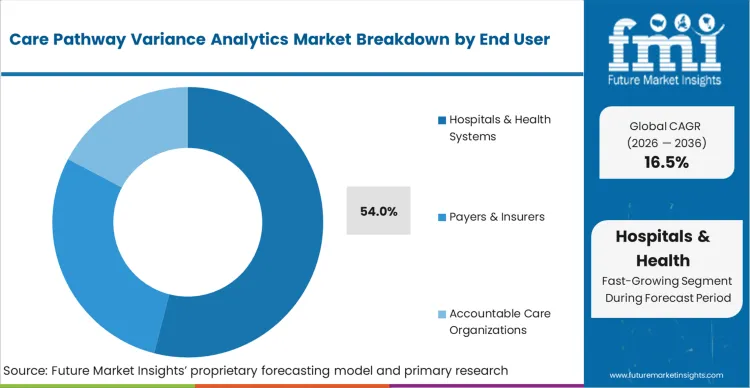
A prior failure to control episode costs created the massive demand from hospitals and health systems, anchoring a 54.0% share in 2026. Hospital chief financial officers deploy these tools to stem the bleeding from value-based care reimbursement penalties. By tracking every clinical decision against standardized pathways, facilities can proactively manage their financial risk. FMI analysts opine that this comprehensive oversight allows institutions to identify their most efficient practitioners and scale those specific techniques enterprise-wide. Clinical department heads lacking granular variance data remain unable to correct detrimental prescribing habits, triggering cascading financial losses.
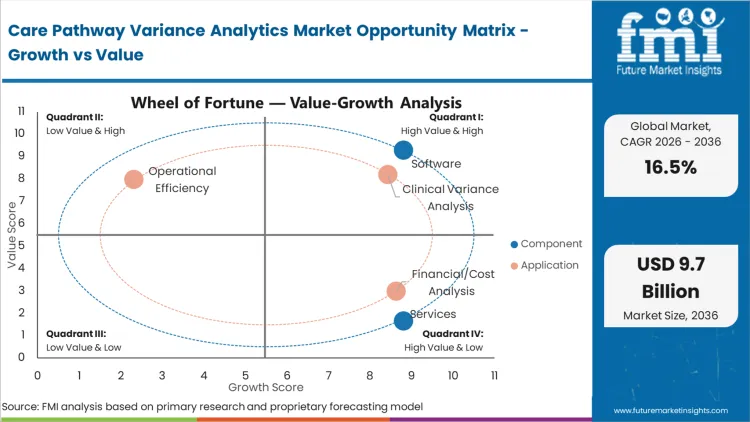
Fixed-fee reimbursement structures drive the market as hospital administrators face severe financial penalties for unstandardized care. Chief medical officers facing these penalties must deploy variance analytics to achieve predictable episode costs. This transition allows facilities to secure shared-savings bonuses while isolating inefficient clinical practices. Institutions that fail to adopt these algorithms lose the leverage needed to survive in value-based contracting environments.
Fragmented electronic health record deployments present a severe operational friction. Data integration specialists struggle to extract clean, normalized clinical data from disparate legacy systems. Facilities attempt to bridge these gaps with custom application programming interfaces, but this workaround has severe scaling limits across large hospital networks.
Based on the regional analysis, the Care Pathway Variance Analytics market is segmented into North America, Latin America, Europe, East Asia, South Asia, Oceania and Middle East & Africa across 40 plus countries.
.webp)
| Country | CAGR (2026 to 2036) |
|---|---|
| China | 19.5% |
| India | 18.2% |
| USA | 15.4% |
| Germany | 14.8% |
| UK | 13.5% |
| Japan | 12.0% |
| South Korea | 11.5% |
Source: Future Market Insights (FMI) analysis, based on proprietary forecasting model and primary research
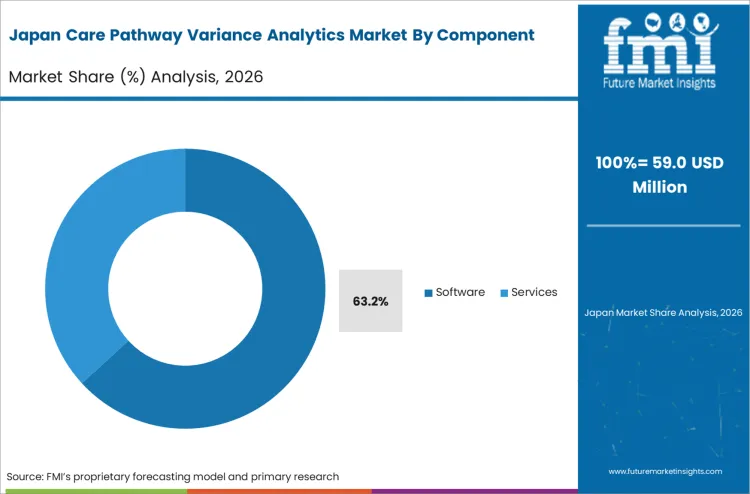
Aggressive public healthcare modernization mandates make this region structurally distinct. FMI's analysis indicates that ministries of health are bypassing legacy quality reporting mechanisms and directly funding intelligent hospital infrastructure. This clean-slate digital transformation sets up a massive deployment footprint for advanced analytical engines.
FMI's report includes detailed assessments of Australia, Indonesia, and Taiwan. The structural pattern across these additional countries reveals a rapid transition toward digital-first quality accreditation programs, heavily subsidizing analytics adoption.
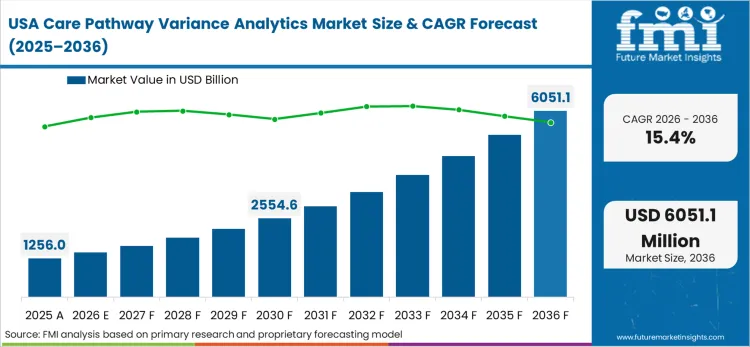
The dominance of commercial accountable care organizations creates a unique structural condition in this region. Private health insurers aggressively transfer financial risk onto provider networks, compelling massive investments in cost-containment technologies. This environment establishes the perfect catalyst for ubiquitous variance tracking implementation.
FMI's report includes comprehensive analysis of Canada and Mexico. The structural pattern across these additional countries highlights a growing emphasis on optimizing resource allocation within constrained public health budgets.
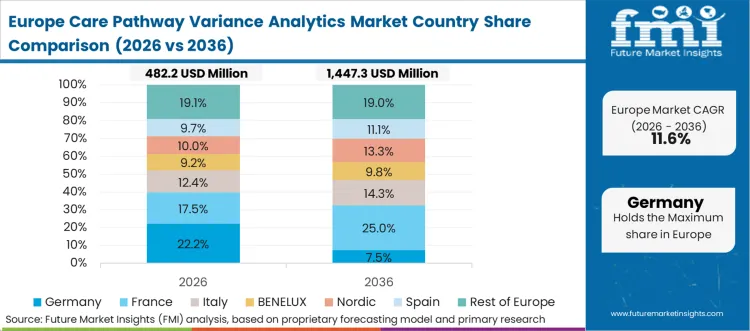
Strict statutory health insurance quality benchmarks define the European structural landscape. Regional health authorities demand exhaustive documentation proving that expensive therapeutic interventions adhere strictly to clinical guidelines. This compliance burden necessitates automated pathway tracking to avoid crippling administrative overhead.
FMI's report includes extensive coverage of France, Italy, and the Nordics. The structural pattern across these additional countries emphasizes the deployment of analytics to support decentralized, community-based care models.
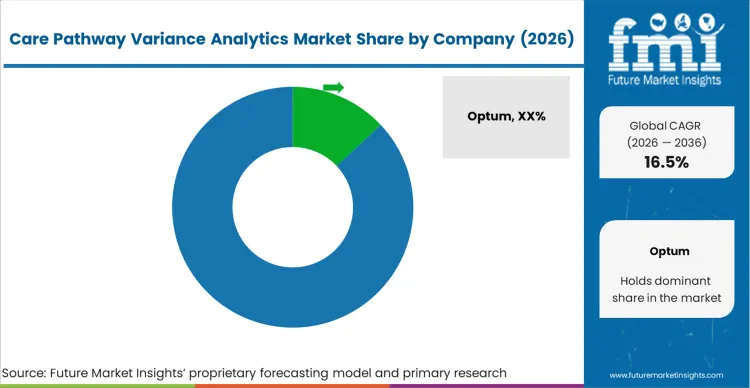
The care pathway variance analytics market remains concentrated among established healthcare IT conglomerates and specialized clinical intelligence firms. High barriers to entry, specifically the requirement for deep electronic health record integration and vast troves of training data, insulate incumbents. Companies like Optum, Health Catalyst, and Merative leverage their massive installed bases to block agile challengers. Buyers rely on vendor track records of successful electronic health record integration to distinguish qualified platforms from unproven software.
These dominant players maintain distinct structural advantages through proprietary digital health for obesity and pathway algorithms trained on billions of historical patient encounters. This immense data gravity allows established vendors to offer superior predictive accuracy that new entrants cannot replicate without decades of data collection. To compete, challengers must build highly specialized niche algorithms or offer radically superior user interfaces. For niche developers, this implies partnering with specific medical societies to validate their targeted variance engines.
Large health systems actively prevent vendor lock-in by mandating strict adherence to open data standards like Fast Healthcare Interoperability Resources. This structural requirement limits the pricing power of dominant analytics providers, forcing them to compete on continuous algorithmic improvement rather than data hostage tactics. A core structural tension exists between health systems demanding total data portability and vendors attempting to construct walled data gardens. As per FMI's projection, the competitive structure will inevitably shift toward modular, easily swappable analytical applications over the forecast period.
| Metric | Value |
|---|---|
| Quantitative Units | USD 2.1 billion to USD 9.7 billion, at a CAGR of 16.50% |
| Market Definition | Care pathway variance analytics encompasses specialized software platforms and methodologies designed to measure actual clinical delivery against standardized evidence-based protocols. |
| Component Segmentation | Software, Services |
| Application Segmentation | Clinical Variance Analysis, Financial/Cost Analysis, Operational Efficiency |
| Delivery Mode Segmentation | Cloud-based, On-premises |
| End User Segmentation | Hospitals & Health Systems, Payers & Insurers, Accountable Care Organizations |
| Regions Covered | North America, Latin America, Europe, East Asia, South Asia, Oceania, Middle East & Africa |
| Countries Covered | China, India, USA, Germany, UK, Japan, South Korea, and 40 plus countries |
| Key Companies Profiled | Optum, McKesson, Merative, Health Catalyst, SAS Institute, Oracle Health, Innovaccer |
| Forecast Period | 2026 to 2036 |
| Approach | Primary interviews mapped specific decision gates triggering analytics upgrades. The baseline derives from a bottom-up aggregation of software deployments, validated against reported health system capital expenditure. |
Source: Future Market Insights (FMI) analysis, based on proprietary forecasting model and primary research
This bibliography is provided for reader reference. The full FMI report contains the complete reference list with primary source documentation.
How large is the Care Pathway Variance Analytics Market in 2026?
The market is expected to reach USD 2.1 billion in 2026. Hospital chief financial officers face imminent revenue cycle deficits and must deploy pathway tracking solutions.
What will the Care Pathway Variance Analytics Market be valued at by 2036?
The valuation will reach USD 9.7 billion by 2036. Real-time algorithmic decision support consistently replaces retrospective clinical auditing.
What CAGR is projected for Care Pathway Variance Analytics Market from 2026 to 2036?
A compound expansion at 16.50% sustains the market over the decade. The permanent structural shift from volume-based compensation to risk-bearing contracts anchors this trajectory.
Which segment leads by Component in 2026?
Software captures a 62.0% share in 2026. Health systems prioritize scalable algorithmic engines over manual consulting reviews to process vast clinical narratives.
Which segment dominates by Application?
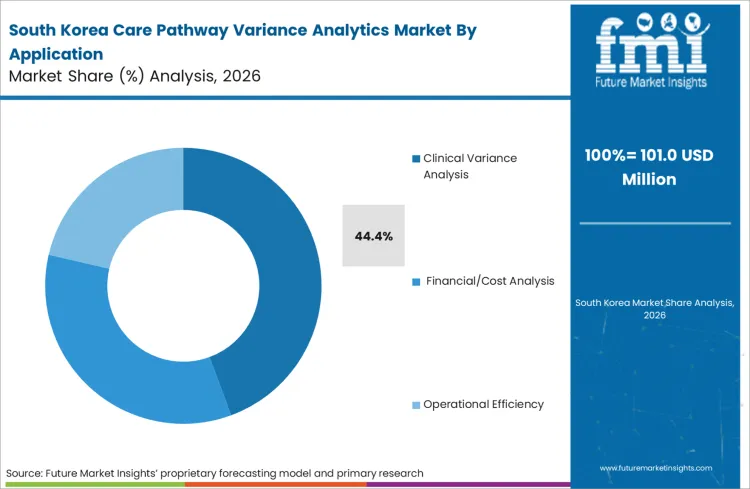
Clinical Variance Analysis holds a 45.0% share in 2026. Medical directors demand actionable insights into physician prescribing behavior to align practices with evidence-based medicine.
Which segment commands the Delivery Mode landscape?
Cloud-based delivery accounts for 68.0% of the market in 2026. Chief information officers abandon isolated servers to facilitate seamless data exchange between acute and post-acute settings.
What End User segment captures the most market share?
Hospitals & Health Systems anchor a 54.0% share in 2026. Facilities proactively manage their financial risk by tracking every clinical decision against standardized pathways.
Which region presents the highest growth rate?
China expands at a 19.5% CAGR as greenfield smart hospitals mandate natively integrated clinical algorithms.
What forces drive demand in India?
Private tertiary networks drive an 18.2% CAGR for the market in India. Corporate hospital chains face intense competition for international medical tourists, requiring verifiable proof of clinical excellence.
What sustains growth in the USA?
The United States tracks at a 15.4% CAGR as value-based reimbursement penalties force rapid compliance. Predictive engines allow administrators to intercept protocol deviations before they trigger federal financial penalties.
What anchors demand in Germany?
Germany advances at a 14.8% CAGR due to stringent statutory insurance quality benchmarks. The national mandate for evidence-based medicine forces clinical directors to continuously audit physician prescribing patterns.
What accelerates adoption in the UK?
The UK expands at a 13.5% CAGR shaped by National Health Service efficiency directives. Trust executives require granular visibility into operational bottlenecks to maximize clinical throughput.
What operational friction acts as a restraint?
Fragmented electronic health record deployments prevent clean data extraction. Facilities struggle to normalize data from disparate legacy systems without breaking customized application programming interfaces.
What primary capability triggers algorithm upgrades?
The integration of predictive algorithms into the physician's electronic workflow at the moment of order entry represents the critical inflection point. This transforms variance analytics from a backend function into a frontline navigation system.
How do large buyers influence vendor pricing?
Large health systems mandate strict adherence to open data standards like Fast Healthcare Interoperability Resources. This limits pricing power by forcing vendors to compete on continuous algorithmic improvement rather than proprietary data lock-in.
What structural transformation shapes the outlook?
The shift from retrospective financial reporting tools to real-time clinical variance analysis forces hospitals to abandon static order sets. This requires dynamic analytics that flag protocol deviations at the point of care.
What distinguishes South Korea's adoption pattern?
South Korea expands at an 11.5% CAGR as tertiary facility throughput pressures mount. High-volume surgical centers rely on precision timing and standardized protocols to maximize operating room utilization.
How is Japan responding to demographic challenges?
Japan tracks at a 12.0% CAGR optimizing geriatric care pathways. Algorithms continuously track complex comorbidity treatments to minimize unnecessary hospital readmissions among elderly patients.
What defines the market definition?
Care pathway variance analytics encompasses specialized software platforms designed to measure actual clinical delivery against standardized evidence-based protocols. This isolates unwarranted diagnostic and therapeutic deviations to quantify their impact on episode costs.
What specific capability drives the Software segment?
Advanced machine learning models identify hidden correlations between subtle protocol deviations and eventual hospital readmissions. This eliminates the latency inherent in retrospective chart audits.
How is the scope bounded regarding exclusions?
General ledger accounting software lacking clinical context and standalone electronic health record systems without dedicated variance tracking modules are explicitly excluded.
What methodological approach validates the forecast?
The baseline derives from a bottom-up aggregation of analytics software deployments, applying region-specific modernization curves. Projections undergo cross-validation against quarterly software subscription revenues.
What specific takeaway should hospital executives action?
Healthcare network executives must mandate the integration of variance alerts directly into physician order entry interfaces. This intercepts unjustified protocol deviations within the diagnostic window before expensive procedures commence.
What regulatory standard shapes product development?
Interoperability regulations demand total data portability. Vendors must construct modular, easily swappable analytical applications rather than maintaining closed proprietary networks.
Full Research Suite comprises of:
Market outlook & trends analysis
Interviews & case studies
Strategic recommendations
Vendor profiles & capabilities analysis
5-year forecasts
8 regions and 60+ country-level data splits
Market segment data splits
12 months of continuous data updates
DELIVERED AS:
PDF EXCEL ONLINE

Thank you!
You will receive an email from our Business Development Manager. Please be sure to check your SPAM/JUNK folder too.