Hospital-at-Home Equipment Rental Market
The hospital-at-home equipment rental market is segmented by Equipment Type (Infusion pumps, Hospital beds, Respiratory devices, Patient monitors, Mobility aids), Rental Model (Monthly rental, Per-episode, On-demand, Fleet lease, Managed service), Care Model (Admission avoidance, Early discharge, Virtual wards, Home infusion, Post-surgical), End User (Health systems, HaH vendors, Home infusion, Homecare agencies, Payers), Clinical Use (Cardiopulmonary, Infection care, Oncology care, Post-surgical, Geriatric care), and Region. Forecast for 2026 to 2036.
Historical Data Covered: 2016 to 2024 | Base Year: 2025 | Estimated Year: 2026 | Forecast Period: 2027 to 2036
Hospital-at-Home Equipment Rental Market Size, Market Forecast and Outlook By FMI
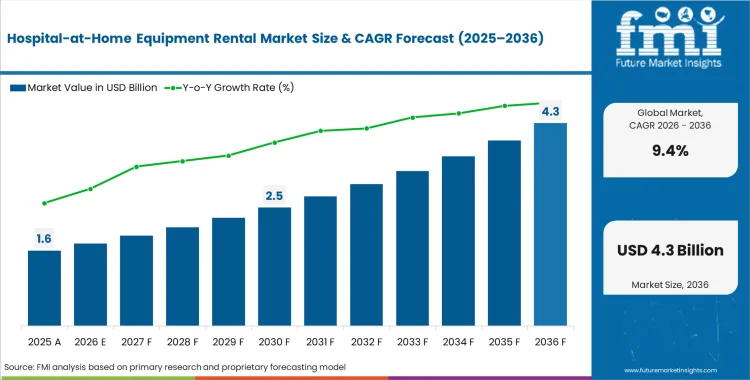
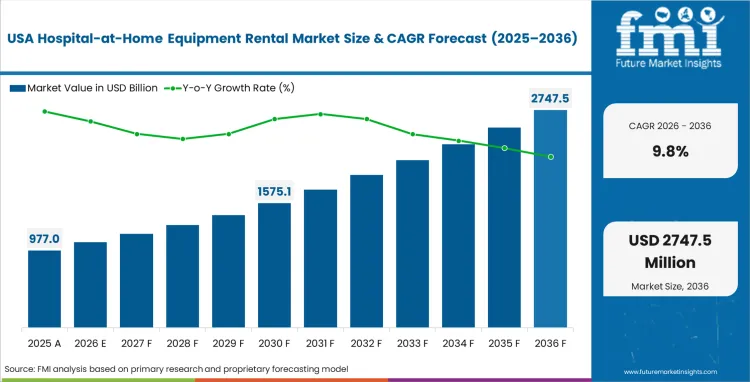
The hospital-at-home equipment rental market was valued at USD 1.4 billion in 2025. Demand is estimated to hit USD 1.6 billion in 2026 at a CAGR of 9.4% during the forecast period. Market revenue is expected to be USD 3.8 billion in 2036 as public health systems globally mandate acute-care decanting into residential settings.
Summary of Hospital-at-Home Equipment Rental Market
- Market Snapshot
- The hospital-at-home equipment rental market is valued at USD 1.42 billion in 2025 and is projected to reach USD 3.81 billion by 2036.
- The industry is expected to grow at a 9.4% CAGR from 2026 to 2036, creating an incremental opportunity of USD 2.26 billion.
- The market is a care-delivery infrastructure segment centered on rented beds, pumps, respiratory devices, monitors, and support equipment used to shift inpatient-grade treatment into the home.
- Structural demand is supported by formal hospital-at-home and virtual-ward programs, with CMS reporting 366 participating hospitals and more than 31,000 patients served in the USA by October 2024.
- Demand and Growth Drivers
- Demand increases because health systems move acute and step-down care out of expensive inpatient beds while preserving clinical monitoring and therapy intensity.
- Infusion and respiratory equipment are seeing strong rental uptake; these categories match the most equipment-intensive home pathways, including oxygen therapy, ventilation support, and home infusion.
- Program growth is also being supported by public-system adoption outside the U.S., including NHS virtual wards in England and the Virtual Hospital Pilot in Victoria, Australia.
- Among key countries, Australia leads at 10.4% CAGR, followed by the United States at 9.8%, Spain at 9.6%, the United Kingdom at 9.1%, France at 8.8%, Canada at 8.6%, and Japan at 8.2%.
- Growth is moderated by reimbursement complexity, uneven clinical eligibility rules, and the need to coordinate logistics, remote monitoring, and in-home clinical services as one package.
- Product and Segment View
- The market covers rented infusion pumps, hospital beds, respiratory devices, patient monitors, and mobility aids deployed in acute-at-home, virtual-ward, and early-discharge pathways.
- These devices are used across cardiopulmonary care, infection care, oncology care, post-surgical recovery, and geriatric support; patients need hospital-grade equipment without a traditional ward stay.
- Infusion pumps lead the Equipment Type segment with 29.0% share, reflecting medication-delivery intensity in home infusion and high-acuity discharge pathways.
- Monthly rental leads the Rental Model segment with 41.0% share, supported by recurring reimbursement structures for oxygen, ventilation, beds, and monitoring assets.
- Admission avoidance leads the Care Model segment with 35.0% share, as providers try to prevent inpatient admission for clinically eligible patients through home-based acute care.
- Health systems lead the End User segment with 46.0% share, because most scaled programs are still being launched and managed by hospitals and integrated delivery networks.
- Cardiopulmonary leads the Clinical Use segment with 27.0% share, reflecting sustained demand for oxygen, ventilation, pulse oximetry, and related support hardware.
- The scope includes rented equipment tied to hospital-at-home, virtual-ward, acute discharge, and high-acuity home infusion use, but excludes general long-term homecare supplies, retail OTC devices, and permanently sold home-use equipment.
- Geography and Competitive Outlook
- Australia, the United States, and Spain are the fastest-growing national markets in this modelled set, while the United Kingdom and France remain stable institutional demand bases.
- Competition is shaped by provider scale, fleet availability, repair capability, payer access, and the ability to bundle logistics, remote monitoring, and clinical support into one service layer.
- Key participants include AdaptHealth, Accendra Health / Apria, Quipt Home Medical, InfuSystem, Med One Group, US Med-Equip, and Agiliti.
- Market concentration remains low because rental demand is split across respiratory, infusion, bed, and alternate-site equipment niches.
| Metric | Details |
|---|---|
| Industry Size (2026) | USD 1.6 billion |
| Industry Value (2036) | USD 3.8 billion |
| CAGR (2026 to 2036) | 9.4% |
Source: Future Market Insights (FMI) analysis, based on proprietary forecasting model and primary research
The procurement department working within prominent, large-scale health systems are currently engaged in significant negotiations for comprehensive, multi-year durable medical equipment rental contracts. The primary goal of these long-term agreements is to decisively secure dedicated, reliable fleets of essential respiratory support and continuous patient monitoring hardware. Providing hospital-level treatment within residential settings necessitates identical uptime guarantees and immediate availability standards when compared to the highly controlled environment of an intensive care unit. Any delay in finalizing these critical hospital-at-home equipment rental market agreements compels clinical operations leaders to unnecessarily retain high-acuity patients in expensive physical hospital wards, immediately creating significant revenue bottlenecks and hindering patient throughput. Hardware availability and rapid deployment are now the primary factors dictating discharge velocity, often surpassing physician readiness alone.
Following the recent and crucial decision by national reimbursement authorities to formally approve new continuous patient monitoring codes specifically for residential deployment, localized pilot programs are now instantly and seamlessly converting into permanent, financially stable acute care at home equipment rental service lines. This comprehensive payer coverage fundamentally removes the financial risk previously associated with scaling these services for integrated delivery networks. The significant challenge of scaling logistics networks to ensure same-day bed and essential pump deployment across wide geographic areas now becomes financially viable and sustainable under these newly established, reliable recurring payment structures, enabling broader access to high-quality care outside traditional settings.
Global market growth rates demonstrate significant regional variation. The United States leads with 9.8% compound annual growth rate (CAGR), supported by clear acute care initiatives from CMS. Spain registers a 9.6% compound growth rate, with the United Kingdom progressing at 9.1%, a rate driven by public virtual ward equipment rental scaling. France expands at 8.8%, Canada grows at 8.6%, and Japan advances at 8.2%. Equipment funding mechanisms differ greatly; Europe sees state-sponsored procurement while North America is dominated by private payer contracting models for deployment.
Segmental Analysis
Hospital-at-Home Equipment Rental Market Analysis by Equipment Type
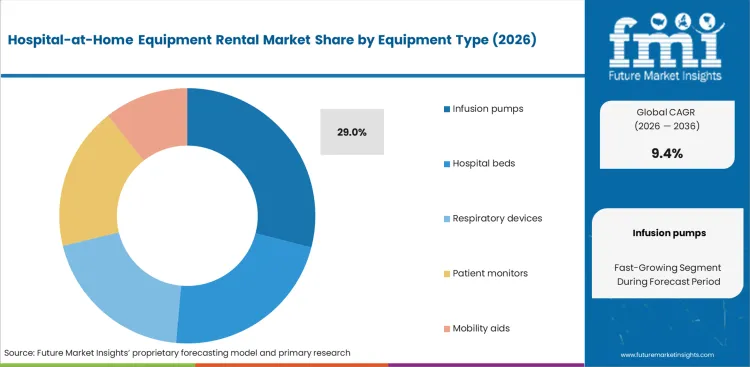
Oncology pharmacy leaders encounter difficulties with residential medication delivery limitations. Strict dosing requirements for chemotherapy and sophisticated antibiotics necessitate precise infusion pumps rental agreements. Infusion pumps segment secure a 29.0% share in 2026, based on these vital clinical thresholds, a primary element supporting compound growth. FMI's estimates suggest failure to deploy programmable smart pumps instantly makes patients ineligible for home treatment protocols. Most industry analysts assume bed rentals require the largest budget allocations. FMI notes infusion pumps in the hospital-at-home equipment rental market actually command premium billing rates, this is due to mandatory continuous software updates and stringent calibration cycles. Clinical operations executives face immediate workflow failures if the pump fleet size does not meet daily discharge targets.
- Initial validation: Smart pump integration determines program eligibility. Pharmacy personnel require continuous bi-directional data flow.
- Qualification standard: Software compatibility between rented pumps and hospital electronic records facilitates seamless entry points. Nursing staff must verify doses directly without manual transcription.
- Expansion driver: Programmable limits prevent residential dosing errors. Clinical officers demand hard-stop functionality on all leased assets before authorizing fleet expansions.
Hospital-at-Home Equipment Rental Market Analysis by Rental Model
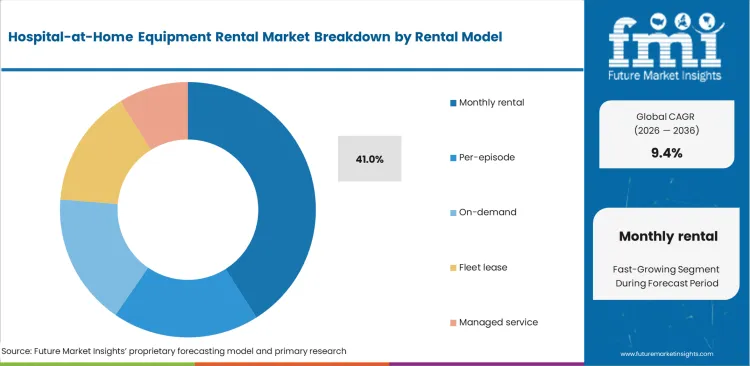
Procurement teams commonly use established billing structures for durable medical equipment. Financial controllers at integrated delivery networks require predictable operational expenses for expanding virtual capacity. FMI's assessment indicates payers prefer 30-day billing increments over intricate daily tracking systems. Monthly rental segment holds a 41.0% share in 2026, alongside elements supporting compound growth linked directly to legacy negative pressure wound therapy rental reimbursement frameworks. Surface-level analysis suggests on-demand leasing offers greater capital efficiency for varying patient volumes. Actual facility operators understand monthly commitments guarantee asset availability during sudden respiratory surge events, thereby protecting discharge pathways amid tightening equipment supply. Supply chain managers attempting purely episodic billing frequently experience stock-outs during peak admission periods.
- Procurement savings: 30-day contracts decrease administrative invoice processing. Supply chain personnel avoid daily reconciliation tasks.
- Hidden operational cost: Fixed monthly terms generate dead expense when patient recovery is faster than expected. Financial controllers pay for unused days.
- Lifecycle comparison: Blended monthly rates surpass episodic pricing across high-acuity cohorts. Procurement teams model costs using the average length of stay.
Hospital-at-Home Equipment Rental Market Analysis by Care Model
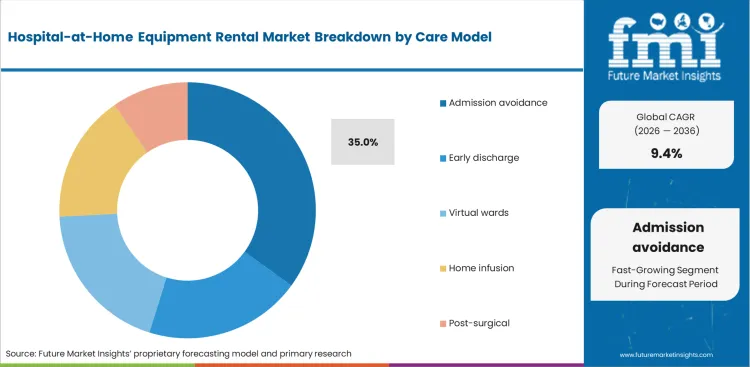
Emergency department executives face intense pressure to free up physical beds. Triage officers employ residential deployment criteria to redirect stable patients away from institutional admission. Admission avoidance segments accounts for 35.0% share in 2026, this is driven by elements supporting compound growth directly related to the high immediate return on investment for capacity-strained facilities. FMI's analysis suggests patient centered medical home services heavily rely on this specific diversion strategy. Hospital administrators focus intensely on early discharge metrics to improve throughput. True relief occurs only when triage teams prevent initial ward admission entirely through immediate home equipment deployment. Care coordination managers lose vital intervention time if rental providers fail to guarantee two-hour asset delivery to residential locations.
- Clinical failure prevented: Emergency room crowding initiates immediate home screening protocols. Triage personnel authorize rapid hospital bed rental for home hospitalization.
- Residual risk: Remote telemetry confirms patient stability within four hours, but requires constant connectivity. Clinical supervisors verify safety baselines continuously.
- Full benefit capture: Successful diversion cases justify larger continuous monitoring fleets. Financial officers approve subsequent rental volume increases based on avoided physical admissions.
Hospital-at-Home Equipment Rental Market Analysis by End User
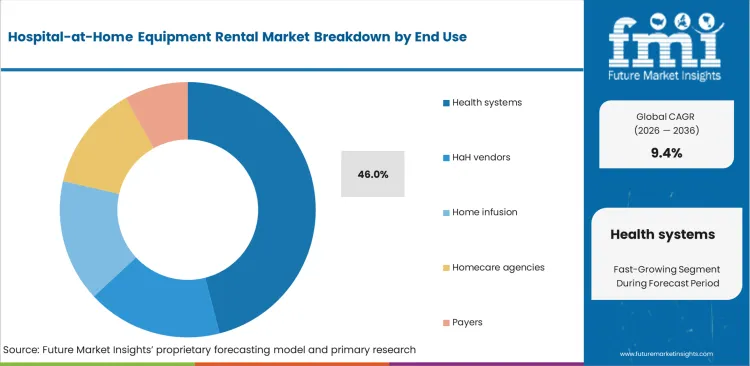
Centralized patient control remains critical for institutional liability management. Chief medical officers refuse to divide acute oversight among independent residential care providers. FMI views home healthcare software integration as demanding a single institutional purchaser. Third-party vendors often market directly to payers, promising lower episode costs. Health system executives actually prevent these vendor-direct models because fragmented equipment standards create severe blind spots in physician telemetry dashboards. Health systems segment maintain 46.0% share, this is driven by factors tied strictly to controlling all hardware provisioning for discharged populations. Technology procurement personnel risk systemic clinical liability upon failing to standardize hardware across all affiliated virtual wards.
- Early adoption: Academic medical centers pilot initial hardware deployments. Clinical innovation personnel establish safety protocols using standardized remote monitoring devices for hospital at home.
- Secondary expansion: Regional hospital networks follow established operational templates. Procurement teams replicate successful leasing agreements.
- Final conversion: Independent community hospitals ultimately embrace rental models. Facility administrators acknowledge the competitive necessity for residential care options.
Hospital-at-Home Equipment Rental Market Analysis by Clinical Use
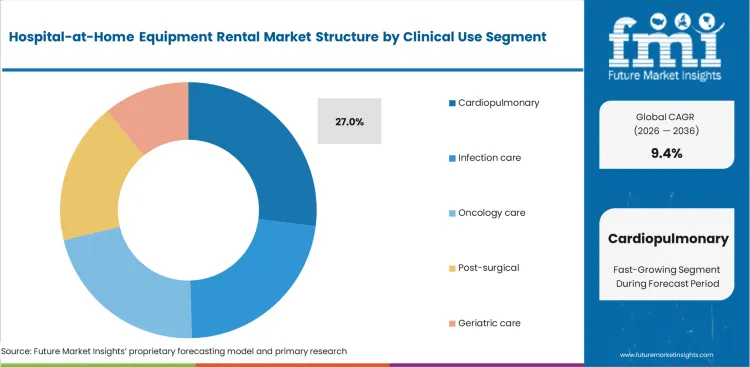
Cardiopulmonary segment dominates with 27.0% share, supported by factors including these heavy equipment requirements. Respiratory failure scenarios necessitate intensive hardware intervention. Pulmonologists require continuous positive airway pressure and oxygen concentration capabilities for residential deployment. FMI observes successful home respiratory therapy relies entirely on uninterrupted device functionality. General consensus suggests post-surgical recovery drives the highest volume of virtual beds. Post-acute respiratory management actually requires three times more hardware density per patient compared to standard surgical follow-up. Medical officers risk immediate readmission spikes if hospital-at-home respiratory equipment rental experiences sudden power or mechanical failure in residential settings.
- Performance baseline: Oxygen concentrator efficiency prevents immediate respiratory distress. Clinical supervisors initiate emergency medical transport if output drops.
- Edge condition vulnerability: Power outages neutralize continuous monitoring systems. Facility managers must deploy backup battery fleets to maintain cardiopulmonary support.
- Qualification standard: Redundant hardware provisioning ensures uninterrupted therapy. Supply chain personnel mandate secondary asset availability for critically unstable patients.
Hospital-at-Home Equipment Rental Market Drivers, Restraints, and Opportunities
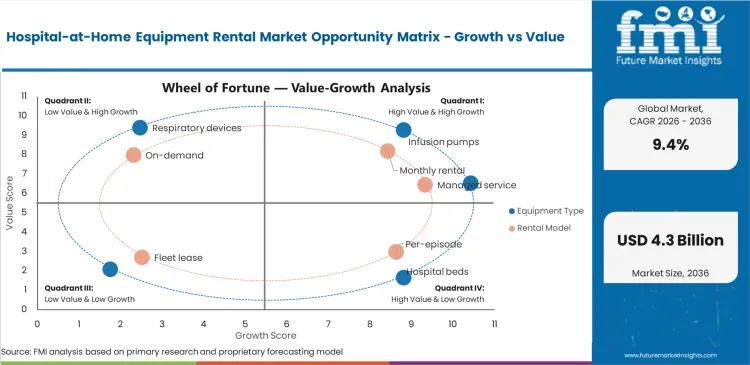
Reimbursement policy changes compel hospital administrators to rapidly expand residential care capacity. Medicare initiatives penalize extended inpatient stays while simultaneously creating distinct billing codes for virtual ward supervision. Delaying hardware procurement directly limits revenue generation capabilities for these new clinical pathways. Emergency department executives face constant patient backlogs, requiring aggressive early discharge protocols for resolution. Rented medical equipment provides the exact physical infrastructure necessary to execute these discharges safely. Supply chain vice presidents must secure reliable hardware fleets immediately to capitalize on favorable regulatory windows before payer policies become stricter.
Reverse logistics friction severely limits active patient capacity. Retrieving, sterilizing, and recalibrating complex medical hardware from residential settings necessitates highly specialized transport networks. General courier services lack proper certification for handling contaminated clinical assets. This operational bottleneck creates significant fleet inefficiencies for high acuity home care equipment rental. Rental providers are establishing localized cleaning hubs to speed up turnaround times. These regional facilities currently lack sufficient throughput necessary to support sudden regional admission surges.
Opportunities in Hospital-at-Home Equipment Rental Market
- Telemetry integration: Proprietary hardware communication limits data flow. Integrated telemedicine equipment vendors command premium rates by offering universal API connectivity for hospital-at-home patient monitoring equipment.
- Rural deployment: Geographic distance complicates asset retrieval. Regional logistics providers secure exclusive hospital contracts by resolving remote delivery constraints.
- Pediatric adaptation: Adult-sized hardware is often a poor fit for pediatric patients. Niche equipment lessors achieve high margins by stocking specialized neonatal monitoring fleets.
Regional Analysis
Based on regional analysis, the hospital-at-home equipment rental market is segmented into North America, Europe, Asia Pacific, Latin America, and Middle East & Africa.
.webp)
| Country | CAGR (2026 to 2036) |
|---|---|
| United States | 9.8% |
| Spain | 9.6% |
| United Kingdom | 9.1% |
| France | 8.8% |
| Canada | 8.6% |
| Japan | 8.2% |
Source: Future Market Insights (FMI) analysis, based on proprietary forecasting model and primary research
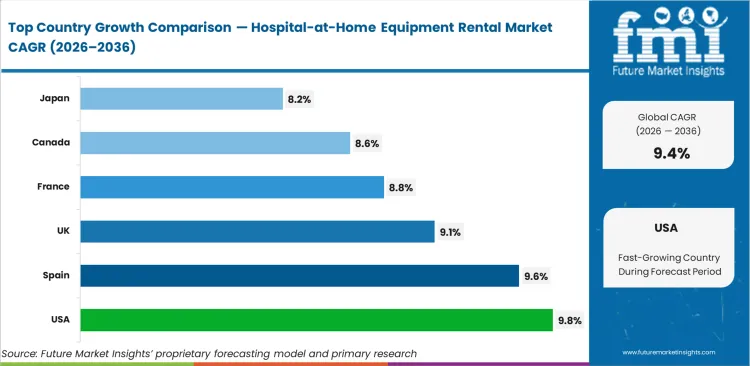
North America Hospital-at-Home Equipment Rental Market Analysis
Reimbursement structures define clinical hardware adoption across this region. Public health mandates actively transition institutional treatment into private residences. FMI analysts observe that United States durable medical equipment rental frameworks heavily influence health systems structuring virtual ward contracts. Payer consolidation establishes significant buyer leverage for regional hospital networks. Financial controllers necessitate comprehensive risk-sharing agreements from equipment suppliers for operational stability assurance.
- United States: CMS waiver programs furnish explicit operational blueprints for hospital administrators. Procurement teams utilize these guidelines to standardize hardware leasing requirements across extensive hospital networks. Equipment vendors attaining preferred supplier status with major integrated delivery networks capture substantial commercial volume in United States hospital-at-home equipment rental market contracts, ensuring sustained long-term revenue predictability. The move toward decentralized healthcare directly accelerates these specific vendor contracts across urban medical centers. The United States exhibits 9.8% compound growth, a CAGR supported by factors including rigorous adherence to national health infrastructure upgrades and robust private payer involvement.
- Canada: Provincial health budgets constrain capital expenditure for permanent equipment purchases. Supply chain executives employ episodic rental models to manage fluctuating seasonal admission volumes effectively. Canada expands at 8.6% compound growth, driven by factors supporting this CAGR such as the urgent requirement to alleviate severe public hospital overcrowding during winter respiratory spikes. Regional health authorities establish dedicated logistics networks to support rural hardware deployment. Securing continuous monitoring fleets allows provincial administrators to uphold rigorous safety standards without violating strict capitation budget limits, establishing a permanent operational shift. Rental agencies offering bundled respiratory and telemetry packages directly benefit from these specialized public health tenders, achieving dominance in the provincial supply chain.
Europe Hospital-at-Home Equipment Rental Market Analysis
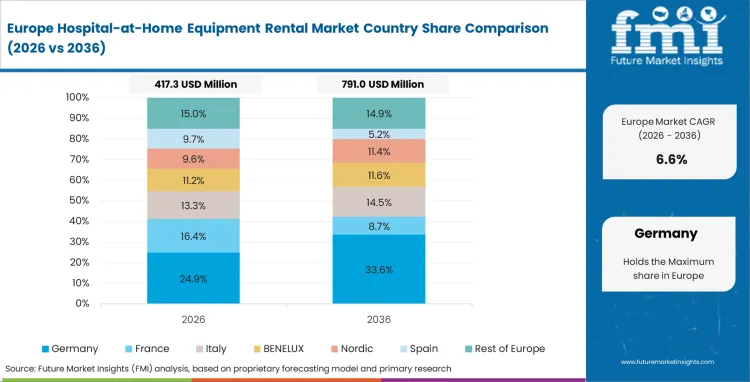
State-funded health services mandate standardized care pathways for entire national populations. Procurement efficiency relies on centralized tender processes for clinical hardware. FMI's estimates suggest that these massive public contracts reduce margins for smaller rental agencies. Clinical leaders enforce strict quality control standards for any device deployed to residential locations.
- United Kingdom: The United Kingdom registers 9.1% compound growth, a rate backed by factors supporting this CAGR like dedicated government funding strictly allocated for decentralized care frameworks. National virtual ward objectives necessitate immediate infrastructure expansion. NHS procurement officials execute substantial long-term leasing agreements to secure adequate infusion and respiratory fleets. Successful contractors integrate deep asset tracking capabilities directly into NHS digital dashboards. Medical device lessors capable of meeting these rigorous interoperability standards secure exclusive multi-year contracts, effectively excluding non-compliant competitors from the lucrative public health procurement pipeline entirely.
- France: Specialized chronic disease management initiatives drive hardware utilization. Respiratory therapy specialists require sophisticated ventilation equipment for severe pulmonary patients.Strict data privacy laws complicate remote telemetry transmission, requiring rental providers to develop highly localized, compliant server architectures. France advances at 8.8% compound growth, a trajectory supported by factors including aggressive state-sponsored homecare subsidies and an aging population profile demanding intensive cardiopulmonary support. Equipment providers mastering these specialized privacy constraints secure dominant negotiating positions with regional health ministries seeking reliable residential care solutions.
- Spain: Regional health ministries aggressively fund admission avoidance pathways. Triage officers heavily utilize remote telemetry devices to monitor stable cardiac patients at home. Independent rental agencies here face intense pressure to match public pricing benchmarks. Spain market revenue grows at 9.6% compound growth, fueled by factors supporting this CAGR such as the immediate cost-saving benefits realized by public hospitals discharging stable patients early. Vendors achieving extreme logistical efficiency manage to defend profitability against these compressed margins, capturing significant market share through guaranteeing rapid reverse logistics and sterilization turnarounds.
Asia Pacific Hospital-at-Home Equipment Rental Market Analysis
Geographic dispersion presents challenges for traditional centralized hospital models. State governments actively fund decentralized clinical infrastructure to serve remote populations. FMI's projection indicates technology procurement teams prioritize ruggedized hardware capable of operating under variable connectivity conditions. Telehealth integration remains a core technical requirement for all leased assets.
- Japan: Japan tracks at 8.2% compound growth, reinforced by factors supporting this CAGR including robust long-term care insurance programs directly reimbursing specialized medical hardware rentals. Super-aging demographics overwhelm available physical hospital beds. Geriatric care coordinators deploy complex mobility and monitoring suites directly into multi-generational homes. Domestic japan durable medical equipment rental specialists maintain tight control over specialized geriatric hardware supply lines. International challengers attempting to enter this sector encounter immense cultural and regulatory barriers, allowing the dominant local rental agencies to capture all incremental revenue generated by the expanding elderly patient base.
Competitive Aligners for Market Players
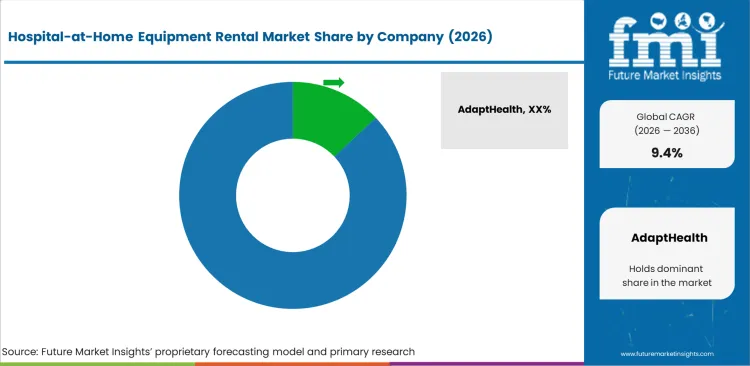
Network density dictates operational viability in this specific hardware sector. Agiliti and Med One Group compete primarily on asset retrieval speed and sterilization turnaround metrics among hospital-at-home equipment rental companies. Clinical hardware sitting idle in residential settings generates zero revenue while blocking new hospital discharges simultaneously. Procurement directors at integrated delivery networks evaluate rental partners strictly on these turnaround SLAs.
Established vendors possess distinct regulatory compliance advantages. InfuSystem maintains deep certification libraries for complex programmable pumps. Challengers face massive capital requirements just to build equivalent patient monitoring system fleets. Reverse logistics networks require specialized biohazard handling protocols absent in standard courier services. Incumbent providers leverage these compliance hurdles to block new market entrants effectively.
Major health systems actively resist sole-source vendor lock-in. Supply chain vice presidents split massive geographic territories between Quipt Home Medical and USA Med-Equip to maintain pricing leverage. Fragmented equipment standards across these different hospital-at-home equipment rental suppliers create severe data integration headaches for clinical staff. Interoperability demands force rental agencies to adopt universal API standards to remain competitive during future bidding cycles.
Key Players in Hospital-at-Home Equipment Rental Market
- AdaptHealth
- Accendra Health / Apria
- Quipt Home Medical
- InfuSystem
- Med One Group
- US Med-Equip
- Agiliti
Scope of the Report

| Metric | Value |
|---|---|
| Quantitative Units | USD 1.6 billion to USD 3.8 billion, at a CAGR of 9.4% |
| Market Definition | Hardware leasing mechanisms supporting institutional-grade medical care within residential settings. Coverage requires devices deployed for acute intervention rather than chronic condition management. |
| Segmentation | Equipment Type, Rental Model, Care Model, End User, Clinical Use, Region |
| Regions Covered | North America, Europe, Asia Pacific, Latin America, Middle East & Africa |
| Countries Covered | United States, Canada, Germany, United Kingdom, France, Italy, Spain, China, Japan, South Korea, Taiwan, Singapore, Brazil, Mexico, Argentina, GCC Countries, South Africa, Israel, Rest of Middle East & Africa |
| Key Companies Profiled | AdaptHealth, Accendra Health / Apria, Quipt Home Medical, InfuSystem, Med One Group, US Med-Equip, Agiliti |
| Forecast Period | 2026 to 2036 |
| Approach | Active patient daily census across recognized virtual hospital programs anchors the baseline volume. |
Source: Future Market Insights (FMI) analysis, based on proprietary forecasting model and primary research
Hospital-at-Home Equipment Rental Market Analysis by Segments
Equipment Type:
- Infusion pumps
- Hospital beds
- Respiratory devices
- Patient monitors
- Mobility aids
Rental Model:
- Monthly rental
- Per-episode
- On-demand
- Fleet lease
- Managed service
Care Model:
- Admission avoidance
- Early discharge
- Virtual wards
- Home infusion
- Post-surgical
End User:
- Health systems
- HaH vendors
- Home infusion
- Homecare agencies
- Payers
Clinical Use:
- Cardiopulmonary
- Infection care
- Oncology care
- Post-surgical
- Geriatric care
Region:
- North America
- United States
- Canada
- Europe
- Germany
- United Kingdom
- France
- Italy
- Spain
- Asia Pacific
- China
- Japan
- South Korea
- Taiwan
- Singapore
- Latin America
- Brazil
- Mexico
- Argentina
- Middle East & Africa
- GCC Countries
- South Africa
- Israel
- Rest of Middle East & Africa
Bibliography
- Centra Health. (2024, June 4). Centra’s remote home monitoring program enhances patient care through technology.
- Medical Guardian. (2025, April). Medical Guardian expands remote monitoring to strengthen chronic disease management and reduce hospital readmissions.
- Larsen, A. T., et al. (2026, January). Assessing the expected costs of continuous remote monitoring at home after hospital discharge.
- McKnight’s Home Care. (2025, March). DispatchHealth, Medically Home to merge.
- HME News. (2024, May). Medically Home shores up hospital-at-home with Siemens, BrightStar Care.
This bibliography is provided for reader reference. The full FMI report contains the complete reference list with primary source documentation.
This Report Addresses
- Procurement strategies for respiratory and monitoring hardware fleets
- Triage diversion pathways utilizing continuous telemetry deployment
- Turnaround lag constraints affecting infusion pump utilization
- Thirty-day billing models dominating current payer frameworks
- Bi-directional data flow requirements for smart pump integration
- Power redundancy provisioning for residential cardiopulmonary patients
- API connectivity standards required by integrated delivery networks
- Reverse logistics scaling requirements across massive geographic territories
Frequently Asked Questions
What equipment is needed for hospital at home?
Programs require clinical-grade hospital beds, continuous patient monitors, portable ventilators, and smart infusion pumps. Triage directors mandate this specific hardware stack to ensure residential care matches intensive care unit capabilities. Lacking any of these components blocks admission avoidance protocols.
How big is the hospital-at-home equipment rental sector?
Valuation sits at USD 1.6 billion in 2026, advancing to USD 3.8 billion by 2036. Assessing the hospital-at-home equipment rental CAGR reveals a 9.4% growth trajectory driven by public health mandates forcing acute care decanting.
Why are hospitals renting equipment for home care?
Facilities avoid massive capital expenditures tied to rapidly depreciating clinical hardware. Financial controllers at integrated delivery networks prefer recurring operational expenses that align perfectly with episodic payer reimbursement structures.
Which devices are most rented in hospital-at-home programs?
Infusion pumps lead adoption because oncology and infection pathways demand precise medication delivery. Cardiopulmonary pathways simultaneously drive heavy leasing volumes for oxygen concentrators and continuous positive airway pressure units.
Who are the key companies in hospital-at-home equipment rental?
AdaptHealth leads through scale, alongside US Med-Equip, Med One Group, Quipt Home Medical, and Agiliti. These suppliers compete strictly on reverse logistics speed and specialized biohazard sterilization capabilities rather than pure hardware pricing.
How does virtual ward equipment rental work?
Hospitals sign monthly or episodic lease agreements for complete hardware bundles. The rental provider handles direct-to-home logistics, setup, maintenance, and ultimate retrieval. This managed service model removes asset tracking burdens from nursing staff.
Is hospital-at-home equipment rental reimbursed?
Medicare waiver programs and private payer contracts explicitly cover equipment costs bundled within daily episodic rates. Financial officers rely on these defined reimbursement pathways to justify scaling continuous monitoring fleets.
How does hospital-at-home durable medical equipment differ from standard homecare devices?
Acute devices require continuous bi-directional data flow, programmable dosing limits, and rigorous calibration cycles. Standard homecare equipment serves chronic condition management without requiring intensive telemetry integration into physician dashboards.
What limits infusion pump deployment in residential settings?
Software mismatches between rented hardware and institutional electronic records block deployments. Pharmacy directors require seamless bi-directional data flow to prevent manual dosing errors. Lack of API connectivity automatically disqualifies equipment from high-acuity oncology protocols.
Why do payers prefer monthly billing increments?
Thirty-day contracts reduce administrative reconciliation burdens for financial controllers. This predictable operational expense structure aligns perfectly with legacy wound therapy models. Financial officers avoid complex daily tracking matrices entirely.
How does reverse logistics impact patient capacity?
Contaminated clinical assets require specialized biohazard transport and quarantine sterilization cycles. This turnaround lag forces procurement teams to over-lease hardware by forty percent. Idle equipment waiting for transport creates artificial patient admission caps.
Why do health systems block vendor-direct rental models?
Fragmented equipment standards create severe blind spots in physician telemetry dashboards. Chief medical officers refuse to split acute oversight across multiple incompatible platforms. Technology procurement directors standardize hardware to contain systemic clinical liability.
What difference drives Australia faster than France?
State-level health departments in Australia explicitly formalize distinct virtual hospital frameworks with mandated data flow standards. France relies on specialized chronic disease management initiatives which face intense data privacy complications regarding remote telemetry transmission.
Table of Content
- Executive Summary
- Global Market Outlook
- Demand to side Trends
- Supply to side Trends
- Technology Roadmap Analysis
- Analysis and Recommendations
- Market Overview
- Market Coverage / Taxonomy
- Market Definition / Scope / Limitations
- Research Methodology
- Chapter Orientation
- Analytical Lens and Working Hypotheses
- Market Structure, Signals, and Trend Drivers
- Benchmarking and Cross-market Comparability
- Market Sizing, Forecasting, and Opportunity Mapping
- Research Design and Evidence Framework
- Desk Research Programme (Secondary Evidence)
- Company Annual and Sustainability Reports
- Peer-reviewed Journals and Academic Literature
- Corporate Websites, Product Literature, and Technical Notes
- Earnings Decks and Investor Briefings
- Statutory Filings and Regulatory Disclosures
- Technical White Papers and Standards Notes
- Trade Journals, Industry Magazines, and Analyst Briefs
- Conference Proceedings, Webinars, and Seminar Materials
- Government Statistics Portals and Public Data Releases
- Press Releases and Reputable Media Coverage
- Specialist Newsletters and Curated Briefings
- Sector Databases and Reference Repositories
- FMI Internal Proprietary Databases and Historical Market Datasets
- Subscription Datasets and Paid Sources
- Social Channels, Communities, and Digital Listening Inputs
- Additional Desk Sources
- Expert Input and Fieldwork (Primary Evidence)
- Primary Modes
- Qualitative Interviews and Expert Elicitation
- Quantitative Surveys and Structured Data Capture
- Blended Approach
- Why Primary Evidence is Used
- Field Techniques
- Interviews
- Surveys
- Focus Groups
- Observational and In-context Research
- Social and Community Interactions
- Stakeholder Universe Engaged
- C-suite Leaders
- Board Members
- Presidents and Vice Presidents
- R&D and Innovation Heads
- Technical Specialists
- Domain Subject-matter Experts
- Scientists
- Physicians and Other Healthcare Professionals
- Governance, Ethics, and Data Stewardship
- Research Ethics
- Data Integrity and Handling
- Primary Modes
- Tooling, Models, and Reference Databases
- Desk Research Programme (Secondary Evidence)
- Data Engineering and Model Build
- Data Acquisition and Ingestion
- Cleaning, Normalisation, and Verification
- Synthesis, Triangulation, and Analysis
- Quality Assurance and Audit Trail
- Market Background
- Market Dynamics
- Drivers
- Restraints
- Opportunity
- Trends
- Scenario Forecast
- Demand in Optimistic Scenario
- Demand in Likely Scenario
- Demand in Conservative Scenario
- Opportunity Map Analysis
- Product Life Cycle Analysis
- Supply Chain Analysis
- Investment Feasibility Matrix
- Value Chain Analysis
- PESTLE and Porter’s Analysis
- Regulatory Landscape
- Regional Parent Market Outlook
- Production and Consumption Statistics
- Import and Export Statistics
- Market Dynamics
- Global Market Analysis 2021 to 2025 and Forecast, 2026 to 2036
- Historical Market Size Value (USD Million) Analysis, 2021 to 2025
- Current and Future Market Size Value (USD Million) Projections, 2026 to 2036
- Y to o to Y Growth Trend Analysis
- Absolute $ Opportunity Analysis
- Global Market Pricing Analysis 2021 to 2025 and Forecast 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Equipment Type
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Equipment Type , 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Equipment Type , 2026 to 2036
- Infusion pumps
- Hospital beds
- Respiratory devices
- Patient monitors
- Mobility aids
- Infusion pumps
- Y to o to Y Growth Trend Analysis By Equipment Type , 2021 to 2025
- Absolute $ Opportunity Analysis By Equipment Type , 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Rental Model
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Rental Model, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Rental Model, 2026 to 2036
- Monthly rental
- Per-episode
- On-demand
- Fleet lease
- Managed service
- Monthly rental
- Y to o to Y Growth Trend Analysis By Rental Model, 2021 to 2025
- Absolute $ Opportunity Analysis By Rental Model, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Care Model
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Care Model, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Care Model, 2026 to 2036
- Admission avoidance
- Early discharge
- Virtual wards
- Home infusion
- Post-surgical
- Admission avoidance
- Y to o to Y Growth Trend Analysis By Care Model, 2021 to 2025
- Absolute $ Opportunity Analysis By Care Model, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By End Use
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By End Use, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By End Use, 2026 to 2036
- Health systems
- HaH vendors
- Home infusion
- Homecare agencies
- Payers
- Health systems
- Y to o to Y Growth Trend Analysis By End Use, 2021 to 2025
- Absolute $ Opportunity Analysis By End Use, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Clinical Use
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Clinical Use, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Clinical Use, 2026 to 2036
- Cardiopulmonary
- Infection care
- Oncology care
- Post-surgical
- Geriatric care
- Cardiopulmonary
- Y to o to Y Growth Trend Analysis By Clinical Use, 2021 to 2025
- Absolute $ Opportunity Analysis By Clinical Use, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Region
- Introduction
- Historical Market Size Value (USD Million) Analysis By Region, 2021 to 2025
- Current Market Size Value (USD Million) Analysis and Forecast By Region, 2026 to 2036
- North America
- Latin America
- Western Europe
- Eastern Europe
- East Asia
- South Asia and Pacific
- Middle East & Africa
- Market Attractiveness Analysis By Region
- North America Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- USA
- Canada
- Mexico
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- By Country
- Market Attractiveness Analysis
- By Country
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Key Takeaways
- Latin America Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Brazil
- Chile
- Rest of Latin America
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- By Country
- Market Attractiveness Analysis
- By Country
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Key Takeaways
- Western Europe Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Germany
- UK
- Italy
- Spain
- France
- Nordic
- BENELUX
- Rest of Western Europe
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- By Country
- Market Attractiveness Analysis
- By Country
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Key Takeaways
- Eastern Europe Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Russia
- Poland
- Hungary
- Balkan & Baltic
- Rest of Eastern Europe
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- By Country
- Market Attractiveness Analysis
- By Country
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Key Takeaways
- East Asia Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- China
- Japan
- South Korea
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- By Country
- Market Attractiveness Analysis
- By Country
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Key Takeaways
- South Asia and Pacific Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- India
- ASEAN
- Australia & New Zealand
- Rest of South Asia and Pacific
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- By Country
- Market Attractiveness Analysis
- By Country
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Key Takeaways
- Middle East & Africa Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Kingdom of Saudi Arabia
- Other GCC Countries
- Turkiye
- South Africa
- Other African Union
- Rest of Middle East & Africa
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- By Country
- Market Attractiveness Analysis
- By Country
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Key Takeaways
- Key Countries Market Analysis
- USA
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Canada
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Mexico
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Brazil
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Chile
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Germany
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- UK
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Italy
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Spain
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- France
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- India
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- ASEAN
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Australia & New Zealand
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- China
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Japan
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- South Korea
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Russia
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Poland
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Hungary
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Kingdom of Saudi Arabia
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Turkiye
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- South Africa
- Pricing Analysis
- Market Share Analysis, 2025
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- USA
- Market Structure Analysis
- Competition Dashboard
- Competition Benchmarking
- Market Share Analysis of Top Players
- By Regional
- By Equipment Type
- By Rental Model
- By Care Model
- By End Use
- By Clinical Use
- Competition Analysis
- Competition Deep Dive
- AdaptHealth
- Overview
- Product Portfolio
- Profitability by Market Segments (Product/Age /Sales Channel/Region)
- Sales Footprint
- Strategy Overview
- Marketing Strategy
- Product Strategy
- Channel Strategy
- Accendra Health / Apria
- Quipt Home Medical
- InfuSystem
- Med One Group
- US Med-Equip
- Agiliti
- AdaptHealth
- Competition Deep Dive
- Assumptions & Acronyms Used
List of Tables
- Table 1: Global Market Value (USD Million) Forecast by Region, 2021 to 2036
- Table 2: Global Market Value (USD Million) Forecast by Equipment Type , 2021 to 2036
- Table 3: Global Market Value (USD Million) Forecast by Rental Model, 2021 to 2036
- Table 4: Global Market Value (USD Million) Forecast by Care Model, 2021 to 2036
- Table 5: Global Market Value (USD Million) Forecast by End Use, 2021 to 2036
- Table 6: Global Market Value (USD Million) Forecast by Clinical Use, 2021 to 2036
- Table 7: North America Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 8: North America Market Value (USD Million) Forecast by Equipment Type , 2021 to 2036
- Table 9: North America Market Value (USD Million) Forecast by Rental Model, 2021 to 2036
- Table 10: North America Market Value (USD Million) Forecast by Care Model, 2021 to 2036
- Table 11: North America Market Value (USD Million) Forecast by End Use, 2021 to 2036
- Table 12: North America Market Value (USD Million) Forecast by Clinical Use, 2021 to 2036
- Table 13: Latin America Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 14: Latin America Market Value (USD Million) Forecast by Equipment Type , 2021 to 2036
- Table 15: Latin America Market Value (USD Million) Forecast by Rental Model, 2021 to 2036
- Table 16: Latin America Market Value (USD Million) Forecast by Care Model, 2021 to 2036
- Table 17: Latin America Market Value (USD Million) Forecast by End Use, 2021 to 2036
- Table 18: Latin America Market Value (USD Million) Forecast by Clinical Use, 2021 to 2036
- Table 19: Western Europe Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 20: Western Europe Market Value (USD Million) Forecast by Equipment Type , 2021 to 2036
- Table 21: Western Europe Market Value (USD Million) Forecast by Rental Model, 2021 to 2036
- Table 22: Western Europe Market Value (USD Million) Forecast by Care Model, 2021 to 2036
- Table 23: Western Europe Market Value (USD Million) Forecast by End Use, 2021 to 2036
- Table 24: Western Europe Market Value (USD Million) Forecast by Clinical Use, 2021 to 2036
- Table 25: Eastern Europe Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 26: Eastern Europe Market Value (USD Million) Forecast by Equipment Type , 2021 to 2036
- Table 27: Eastern Europe Market Value (USD Million) Forecast by Rental Model, 2021 to 2036
- Table 28: Eastern Europe Market Value (USD Million) Forecast by Care Model, 2021 to 2036
- Table 29: Eastern Europe Market Value (USD Million) Forecast by End Use, 2021 to 2036
- Table 30: Eastern Europe Market Value (USD Million) Forecast by Clinical Use, 2021 to 2036
- Table 31: East Asia Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 32: East Asia Market Value (USD Million) Forecast by Equipment Type , 2021 to 2036
- Table 33: East Asia Market Value (USD Million) Forecast by Rental Model, 2021 to 2036
- Table 34: East Asia Market Value (USD Million) Forecast by Care Model, 2021 to 2036
- Table 35: East Asia Market Value (USD Million) Forecast by End Use, 2021 to 2036
- Table 36: East Asia Market Value (USD Million) Forecast by Clinical Use, 2021 to 2036
- Table 37: South Asia and Pacific Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 38: South Asia and Pacific Market Value (USD Million) Forecast by Equipment Type , 2021 to 2036
- Table 39: South Asia and Pacific Market Value (USD Million) Forecast by Rental Model, 2021 to 2036
- Table 40: South Asia and Pacific Market Value (USD Million) Forecast by Care Model, 2021 to 2036
- Table 41: South Asia and Pacific Market Value (USD Million) Forecast by End Use, 2021 to 2036
- Table 42: South Asia and Pacific Market Value (USD Million) Forecast by Clinical Use, 2021 to 2036
- Table 43: Middle East & Africa Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 44: Middle East & Africa Market Value (USD Million) Forecast by Equipment Type , 2021 to 2036
- Table 45: Middle East & Africa Market Value (USD Million) Forecast by Rental Model, 2021 to 2036
- Table 46: Middle East & Africa Market Value (USD Million) Forecast by Care Model, 2021 to 2036
- Table 47: Middle East & Africa Market Value (USD Million) Forecast by End Use, 2021 to 2036
- Table 48: Middle East & Africa Market Value (USD Million) Forecast by Clinical Use, 2021 to 2036
List of Figures
- Figure 1: Global Market Pricing Analysis
- Figure 2: Global Market Value (USD Million) Forecast 2021-2036
- Figure 3: Global Market Value Share and BPS Analysis by Equipment Type , 2026 and 2036
- Figure 4: Global Market Y-o-Y Growth Comparison by Equipment Type , 2026-2036
- Figure 5: Global Market Attractiveness Analysis by Equipment Type
- Figure 6: Global Market Value Share and BPS Analysis by Rental Model, 2026 and 2036
- Figure 7: Global Market Y-o-Y Growth Comparison by Rental Model, 2026-2036
- Figure 8: Global Market Attractiveness Analysis by Rental Model
- Figure 9: Global Market Value Share and BPS Analysis by Care Model, 2026 and 2036
- Figure 10: Global Market Y-o-Y Growth Comparison by Care Model, 2026-2036
- Figure 11: Global Market Attractiveness Analysis by Care Model
- Figure 12: Global Market Value Share and BPS Analysis by End Use, 2026 and 2036
- Figure 13: Global Market Y-o-Y Growth Comparison by End Use, 2026-2036
- Figure 14: Global Market Attractiveness Analysis by End Use
- Figure 15: Global Market Value Share and BPS Analysis by Clinical Use, 2026 and 2036
- Figure 16: Global Market Y-o-Y Growth Comparison by Clinical Use, 2026-2036
- Figure 17: Global Market Attractiveness Analysis by Clinical Use
- Figure 18: Global Market Value (USD Million) Share and BPS Analysis by Region, 2026 and 2036
- Figure 19: Global Market Y-o-Y Growth Comparison by Region, 2026-2036
- Figure 20: Global Market Attractiveness Analysis by Region
- Figure 21: North America Market Incremental Dollar Opportunity, 2026-2036
- Figure 22: Latin America Market Incremental Dollar Opportunity, 2026-2036
- Figure 23: Western Europe Market Incremental Dollar Opportunity, 2026-2036
- Figure 24: Eastern Europe Market Incremental Dollar Opportunity, 2026-2036
- Figure 25: East Asia Market Incremental Dollar Opportunity, 2026-2036
- Figure 26: South Asia and Pacific Market Incremental Dollar Opportunity, 2026-2036
- Figure 27: Middle East & Africa Market Incremental Dollar Opportunity, 2026-2036
- Figure 28: North America Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 29: North America Market Value Share and BPS Analysis by Equipment Type , 2026 and 2036
- Figure 30: North America Market Y-o-Y Growth Comparison by Equipment Type , 2026-2036
- Figure 31: North America Market Attractiveness Analysis by Equipment Type
- Figure 32: North America Market Value Share and BPS Analysis by Rental Model, 2026 and 2036
- Figure 33: North America Market Y-o-Y Growth Comparison by Rental Model, 2026-2036
- Figure 34: North America Market Attractiveness Analysis by Rental Model
- Figure 35: North America Market Value Share and BPS Analysis by Care Model, 2026 and 2036
- Figure 36: North America Market Y-o-Y Growth Comparison by Care Model, 2026-2036
- Figure 37: North America Market Attractiveness Analysis by Care Model
- Figure 38: North America Market Value Share and BPS Analysis by End Use, 2026 and 2036
- Figure 39: North America Market Y-o-Y Growth Comparison by End Use, 2026-2036
- Figure 40: North America Market Attractiveness Analysis by End Use
- Figure 41: North America Market Value Share and BPS Analysis by Clinical Use, 2026 and 2036
- Figure 42: North America Market Y-o-Y Growth Comparison by Clinical Use, 2026-2036
- Figure 43: North America Market Attractiveness Analysis by Clinical Use
- Figure 44: Latin America Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 45: Latin America Market Value Share and BPS Analysis by Equipment Type , 2026 and 2036
- Figure 46: Latin America Market Y-o-Y Growth Comparison by Equipment Type , 2026-2036
- Figure 47: Latin America Market Attractiveness Analysis by Equipment Type
- Figure 48: Latin America Market Value Share and BPS Analysis by Rental Model, 2026 and 2036
- Figure 49: Latin America Market Y-o-Y Growth Comparison by Rental Model, 2026-2036
- Figure 50: Latin America Market Attractiveness Analysis by Rental Model
- Figure 51: Latin America Market Value Share and BPS Analysis by Care Model, 2026 and 2036
- Figure 52: Latin America Market Y-o-Y Growth Comparison by Care Model, 2026-2036
- Figure 53: Latin America Market Attractiveness Analysis by Care Model
- Figure 54: Latin America Market Value Share and BPS Analysis by End Use, 2026 and 2036
- Figure 55: Latin America Market Y-o-Y Growth Comparison by End Use, 2026-2036
- Figure 56: Latin America Market Attractiveness Analysis by End Use
- Figure 57: Latin America Market Value Share and BPS Analysis by Clinical Use, 2026 and 2036
- Figure 58: Latin America Market Y-o-Y Growth Comparison by Clinical Use, 2026-2036
- Figure 59: Latin America Market Attractiveness Analysis by Clinical Use
- Figure 60: Western Europe Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 61: Western Europe Market Value Share and BPS Analysis by Equipment Type , 2026 and 2036
- Figure 62: Western Europe Market Y-o-Y Growth Comparison by Equipment Type , 2026-2036
- Figure 63: Western Europe Market Attractiveness Analysis by Equipment Type
- Figure 64: Western Europe Market Value Share and BPS Analysis by Rental Model, 2026 and 2036
- Figure 65: Western Europe Market Y-o-Y Growth Comparison by Rental Model, 2026-2036
- Figure 66: Western Europe Market Attractiveness Analysis by Rental Model
- Figure 67: Western Europe Market Value Share and BPS Analysis by Care Model, 2026 and 2036
- Figure 68: Western Europe Market Y-o-Y Growth Comparison by Care Model, 2026-2036
- Figure 69: Western Europe Market Attractiveness Analysis by Care Model
- Figure 70: Western Europe Market Value Share and BPS Analysis by End Use, 2026 and 2036
- Figure 71: Western Europe Market Y-o-Y Growth Comparison by End Use, 2026-2036
- Figure 72: Western Europe Market Attractiveness Analysis by End Use
- Figure 73: Western Europe Market Value Share and BPS Analysis by Clinical Use, 2026 and 2036
- Figure 74: Western Europe Market Y-o-Y Growth Comparison by Clinical Use, 2026-2036
- Figure 75: Western Europe Market Attractiveness Analysis by Clinical Use
- Figure 76: Eastern Europe Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 77: Eastern Europe Market Value Share and BPS Analysis by Equipment Type , 2026 and 2036
- Figure 78: Eastern Europe Market Y-o-Y Growth Comparison by Equipment Type , 2026-2036
- Figure 79: Eastern Europe Market Attractiveness Analysis by Equipment Type
- Figure 80: Eastern Europe Market Value Share and BPS Analysis by Rental Model, 2026 and 2036
- Figure 81: Eastern Europe Market Y-o-Y Growth Comparison by Rental Model, 2026-2036
- Figure 82: Eastern Europe Market Attractiveness Analysis by Rental Model
- Figure 83: Eastern Europe Market Value Share and BPS Analysis by Care Model, 2026 and 2036
- Figure 84: Eastern Europe Market Y-o-Y Growth Comparison by Care Model, 2026-2036
- Figure 85: Eastern Europe Market Attractiveness Analysis by Care Model
- Figure 86: Eastern Europe Market Value Share and BPS Analysis by End Use, 2026 and 2036
- Figure 87: Eastern Europe Market Y-o-Y Growth Comparison by End Use, 2026-2036
- Figure 88: Eastern Europe Market Attractiveness Analysis by End Use
- Figure 89: Eastern Europe Market Value Share and BPS Analysis by Clinical Use, 2026 and 2036
- Figure 90: Eastern Europe Market Y-o-Y Growth Comparison by Clinical Use, 2026-2036
- Figure 91: Eastern Europe Market Attractiveness Analysis by Clinical Use
- Figure 92: East Asia Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 93: East Asia Market Value Share and BPS Analysis by Equipment Type , 2026 and 2036
- Figure 94: East Asia Market Y-o-Y Growth Comparison by Equipment Type , 2026-2036
- Figure 95: East Asia Market Attractiveness Analysis by Equipment Type
- Figure 96: East Asia Market Value Share and BPS Analysis by Rental Model, 2026 and 2036
- Figure 97: East Asia Market Y-o-Y Growth Comparison by Rental Model, 2026-2036
- Figure 98: East Asia Market Attractiveness Analysis by Rental Model
- Figure 99: East Asia Market Value Share and BPS Analysis by Care Model, 2026 and 2036
- Figure 100: East Asia Market Y-o-Y Growth Comparison by Care Model, 2026-2036
- Figure 101: East Asia Market Attractiveness Analysis by Care Model
- Figure 102: East Asia Market Value Share and BPS Analysis by End Use, 2026 and 2036
- Figure 103: East Asia Market Y-o-Y Growth Comparison by End Use, 2026-2036
- Figure 104: East Asia Market Attractiveness Analysis by End Use
- Figure 105: East Asia Market Value Share and BPS Analysis by Clinical Use, 2026 and 2036
- Figure 106: East Asia Market Y-o-Y Growth Comparison by Clinical Use, 2026-2036
- Figure 107: East Asia Market Attractiveness Analysis by Clinical Use
- Figure 108: South Asia and Pacific Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 109: South Asia and Pacific Market Value Share and BPS Analysis by Equipment Type , 2026 and 2036
- Figure 110: South Asia and Pacific Market Y-o-Y Growth Comparison by Equipment Type , 2026-2036
- Figure 111: South Asia and Pacific Market Attractiveness Analysis by Equipment Type
- Figure 112: South Asia and Pacific Market Value Share and BPS Analysis by Rental Model, 2026 and 2036
- Figure 113: South Asia and Pacific Market Y-o-Y Growth Comparison by Rental Model, 2026-2036
- Figure 114: South Asia and Pacific Market Attractiveness Analysis by Rental Model
- Figure 115: South Asia and Pacific Market Value Share and BPS Analysis by Care Model, 2026 and 2036
- Figure 116: South Asia and Pacific Market Y-o-Y Growth Comparison by Care Model, 2026-2036
- Figure 117: South Asia and Pacific Market Attractiveness Analysis by Care Model
- Figure 118: South Asia and Pacific Market Value Share and BPS Analysis by End Use, 2026 and 2036
- Figure 119: South Asia and Pacific Market Y-o-Y Growth Comparison by End Use, 2026-2036
- Figure 120: South Asia and Pacific Market Attractiveness Analysis by End Use
- Figure 121: South Asia and Pacific Market Value Share and BPS Analysis by Clinical Use, 2026 and 2036
- Figure 122: South Asia and Pacific Market Y-o-Y Growth Comparison by Clinical Use, 2026-2036
- Figure 123: South Asia and Pacific Market Attractiveness Analysis by Clinical Use
- Figure 124: Middle East & Africa Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 125: Middle East & Africa Market Value Share and BPS Analysis by Equipment Type , 2026 and 2036
- Figure 126: Middle East & Africa Market Y-o-Y Growth Comparison by Equipment Type , 2026-2036
- Figure 127: Middle East & Africa Market Attractiveness Analysis by Equipment Type
- Figure 128: Middle East & Africa Market Value Share and BPS Analysis by Rental Model, 2026 and 2036
- Figure 129: Middle East & Africa Market Y-o-Y Growth Comparison by Rental Model, 2026-2036
- Figure 130: Middle East & Africa Market Attractiveness Analysis by Rental Model
- Figure 131: Middle East & Africa Market Value Share and BPS Analysis by Care Model, 2026 and 2036
- Figure 132: Middle East & Africa Market Y-o-Y Growth Comparison by Care Model, 2026-2036
- Figure 133: Middle East & Africa Market Attractiveness Analysis by Care Model
- Figure 134: Middle East & Africa Market Value Share and BPS Analysis by End Use, 2026 and 2036
- Figure 135: Middle East & Africa Market Y-o-Y Growth Comparison by End Use, 2026-2036
- Figure 136: Middle East & Africa Market Attractiveness Analysis by End Use
- Figure 137: Middle East & Africa Market Value Share and BPS Analysis by Clinical Use, 2026 and 2036
- Figure 138: Middle East & Africa Market Y-o-Y Growth Comparison by Clinical Use, 2026-2036
- Figure 139: Middle East & Africa Market Attractiveness Analysis by Clinical Use
- Figure 140: Global Market - Tier Structure Analysis
- Figure 141: Global Market - Company Share Analysis
Full Research Suite comprises of:
Market outlook & trends analysis
Interviews & case studies
Strategic recommendations
Vendor profiles & capabilities analysis
5-year forecasts
8 regions and 60+ country-level data splits
Market segment data splits
12 months of continuous data updates
DELIVERED AS:
PDF EXCEL ONLINE

