Cardiometabolic-Sleep Comorbidity Treatment Market
Cardiometabolic-Sleep Comorbidity Treatment Market Size and Share Forecast Outlook 2026 to 2036
Historical Data Covered: 2016 to 2024 | Base Year: 2025 | Estimated Year: 2026 | Forecast Period: 2027 to 2036
Cardiometabolic-Sleep Comorbidity Treatment Market Forecast and Outlook 2026 to 2036
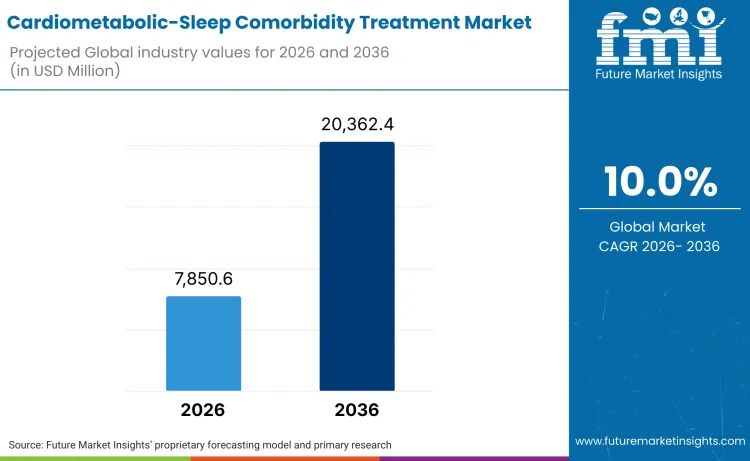
The global cardiometabolic-sleep comorbidity treatment sector is on track to achieve a valuation of USD 20,362.40 million by 2036, accelerating from USD 7,850.60 million in 2026 at a CAGR of 10.0%. As per Future Market Insights, expansion is structurally underpinned by clinical evidence demonstrating that obstructive sleep apnea treatment through continuous positive airway pressure therapy improves glycemic control in type 2 diabetes patients and reduces blood pressure in hypertensive populations, creating medical necessity for integrated care rather than parallel independent treatments.
This clinical evidence compels healthcare systems to establish integrated care pathways where sleep medicine specialists, endocrinologists, and cardiologists coordinate treatment rather than operating in independent silos that miss therapeutic synergies. Simultaneously the payer landscape is shifting from fee-for-service reimbursement toward value-based care contracts that reward outcome improvement across multiple conditions, creating financial incentives for providers to address sleep-disordered breathing as component of comprehensive cardiometabolic management rather than treating it as isolated respiratory disorder. By tapping these solutions, companies are aggressively earning profits. In its third quarter of fiscal year 2025, Resmed reported a surge in income from operations by 14%.
“Our positive fiscal year 2025 performance continued in the third quarter, with strong top-line revenue growth, margin expansion, and double-digit EPS growth resulting from solid customer demand for our best-in-class products and software solutions,” said Resmed’s Chairman and CEO, Mick Farrell.
The operational reality for healthcare providers is defined by care coordination complexity where integrated treatment requires electronic health record systems that share sleep study results, medication adherence data, and metabolic biomarkers across specialties rather than maintaining isolated documentation silos. Medicare and commercial insurance coverage policies are evolving to recognize bundled cardiometabolic-sleep treatment programs, creating reimbursement structures that support coordinated care models. This payment evolution is accelerating investment in remote patient monitoring platforms that track continuous positive airway pressure device usage, glucose levels, blood pressure, and weight through unified dashboards accessible to multidisciplinary care teams.
Summary of Cardiometabolic-Sleep Comorbidity Treatment Market
What Is Growth Outlook on Cardiometabolic-Sleep Comorbidity Treatment Market as per Future Market Insights Projection?
Future Market Insights projects the cardiometabolic-sleep comorbidity treatment market to expand at a CAGR of 10.0% from 2026 to 2036, increasing from USD 7,850.60 Million in 2026 to USD 20,362.40 Million by 2036.
FMI Research Approach: FMI proprietary forecasting model based on obstructive sleep apnea prevalence in cardiometabolic disease populations, integrated care pathway adoption trajectories, GLP-1 agonist prescription patterns in OSA patients, and value-based care contract penetration rates.
Which Country Holds Largest Share in Global Cardiometabolic-Sleep Comorbidity Treatment Market?
The United States holds a significant share supported by Medicare reimbursement for home sleep apnea testing in cardiometabolic populations and commercial insurance coverage for weight-loss pharmacotherapy in obese patients with comorbid conditions.
FMI Research Approach: FMI country-level revenue modeling by OSA prevalence in diabetes and hypertension populations, integrated care reimbursement frameworks, and GLP-1 agonist access policies.
What Are Globally Unique Trends Shaping Cardiometabolic-Sleep Comorbidity Treatment Market?
Globally unique trends include artificial intelligence risk stratification algorithms that predict cardiovascular events from sleep study respiratory parameters combined with metabolic biomarkers, hybrid care models where patients receive initial in-person assessment followed by remote monitoring through connected devices, and pharmacogenomic testing guiding medication selection based on individual metabolism of both sleep-promoting agents and cardiometabolic drugs to optimize efficacy while minimizing drug-drug interactions.
FMI Research Approach: Connected health device adoption tracking, value-based care program proliferation analysis, and multidisciplinary treatment protocol development monitoring.
Cardiometabolic-Sleep Comorbidity Treatment Market Key Takeaways
| Metric | Value |
|---|---|
| Market Value (2026) | USD 7,850.60 million |
| Market Forecast Value (2036) | USD 20,362.40 million |
| Forecast CAGR (2026 to 2036) | 10.0% |
Source: Future Market Insights (FMI) analysis, based on proprietary forecasting model and primary research
What Factors Propel Adoption of Cardiometabolic-Sleep Comorbidity Treatment?
Clinical evidence demonstrating therapeutic interdependence serves as the primary catalyst, as research published in the National Library of Medicine validates that continuous positive airway pressure therapy improves insulin sensitivity and reduces HbA1c levels in type 2 diabetes patients with obstructive sleep apnea. This metabolic benefit creates medical necessity for sleep apnea screening and treatment in diabetic populations rather than addressing hyperglycemia through pharmaceutical intervention alone.
Payer value-based care initiatives accelerate adoption as Medicare Accountable Care Organizations and commercial insurance population health programs receive financial rewards for reducing cardiovascular events and diabetes complications across enrolled populations. These outcome-based contracts create economic incentives to address modifiable risk factors including untreated sleep apnea that independently contributes to adverse cardiometabolic outcomes. Owing to this factor, obesity-diabetes drugs have also garnered much attention lately. Healthcare systems participating in value-based arrangements are implementing systematic sleep apnea screening in high-risk populations using validated questionnaires and portable home testing, identifying treatment opportunities that fee-for-service payment models historically under-recognized due to fragmented specialist referral patterns.
How is the Cardiometabolic-Sleep Comorbidity Treatment Market Segmented?
The mental health sleep overlap market is segmented by treatment components that include PAP therapy and sleep apnea devices, weight loss pharmacotherapy such as GLP 1 agents, hypertension and diabetes medication optimization programs, remote monitoring with risk stratification analytics, and lifestyle supported care management services integrated into chronic care pathways. By comorbidity pathway, the market addresses OSA with obesity management, OSA with hypertension and cardiovascular risk control, OSA with type 2 diabetes management, heart failure with sleep disordered breathing, and other metabolic sleep phenotypes shaped by cardiometabolic risk clustering.
By end user, solutions are deployed across hospitals and cardiometabolic clinics, sleep clinics and DME networks, the retail pharmacy channel, and payers and population health managers managing longitudinal risk. By region, adoption spans North America, Europe, East Asia, South Asia, Latin America, and the Middle East and Africa, showing varied reimbursement models, care delivery maturity, and digital health readiness across healthcare systems.
Why Does PAP Therapy Hold Dominant Treatment Component Share?
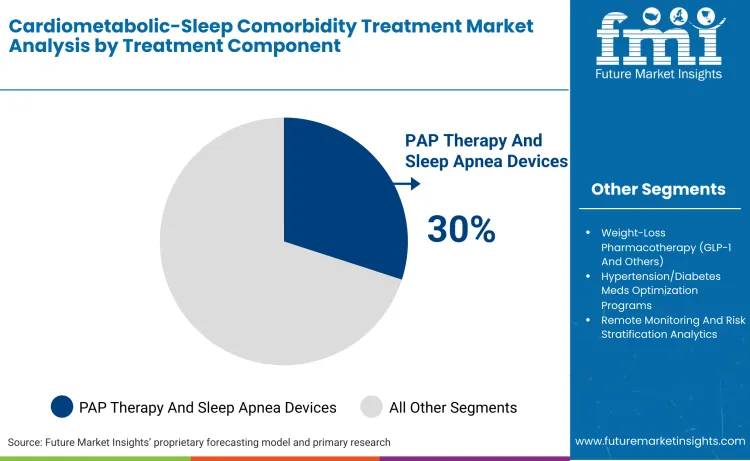
PAP therapy maintains 30% share driven by the awareness of sleep disordered breathing across both clinical and consumer health settings. Physicians are diagnosing obstructive sleep apnea earlier due to broader screening in primary care, cardiology, and metabolic clinics, where sleep disorders are recognized as contributors to hypertension, diabetes, and cardiovascular risk. Growing urbanization and sedentary lifestyles have increased obesity prevalence, which remains a major risk factor for airway obstruction during sleep. Aging populations are structural driver, since upper airway muscle tone declines with age, raising apnea incidence among older adults. The State Council of the People’s Republic of China reported 297 million population aged 60 and above in 2023. Health systems are prioritizing non invasive, home based management of chronic conditions, and PAP devices fit well within this care model by enabling long term therapy outside hospital environments.
Advances in device comfort, quieter motors, improved mask ergonomics, and adaptive pressure algorithms have reduced treatment discontinuation, encouraging sustained usage. Remote monitoring features now allow clinicians to track adherence and therapy effectiveness, supporting outcomes based care models and reimbursement decisions. Employer sponsored health programs and insurer backed screening initiatives are expanding access to diagnosis and therapy, while growing consumer acceptance of wearable and connected health devices is normalizing nightly device use.
Why Does OSA Plus Obesity Management Dominate Comorbidity Pathways?
OSA plus obesity management captures 34% of comorbidity pathway share as excess adipose tissue represents the primary modifiable risk factor for obstructive sleep apnea through upper airway soft tissue deposition and reduced lung volumes from truncal obesity. Epidemiological research estimates that 60-70% of obstructive sleep apnea patients have obesity, creating substantial addressable population for integrated weight management interventions. In addition, as per the WHO, 1 in every 8 people were diagnosed with obesity in 2022.
This pathway concentration is attracting pharmaceutical investment as obesity medication manufacturers position GLP-1 agonists for sleep apnea indication approval, with clinical trials specifically enrolling obese OSA populations to generate regulatory evidence supporting labeled usage beyond diabetes and general obesity indications.
What Trends Are Shaping Cardiometabolic-Sleep Comorbidity Treatment Industry Evolution?
Healthcare delivery is shifting toward virtual-first models where initial patient assessment occurs through telemedicine consultation combining questionnaire-based screening, remote pulse oximetry, and artificial intelligence-powered audio analysis of breathing sounds recorded via smartphone applications. This digital triage reduces barriers to care access by eliminating facility-based polysomnography requirements for uncomplicated cases, enabling primary care physicians to initiate treatment without sleep specialist referral delays that historically resulted in 30-40% patient attrition between referral and completed evaluation. Virtual care models particularly benefit rural populations lacking local sleep medicine specialists, with home testing devices shipped directly to patients following remote consultation.
Pharmaceutical development is focusing on once-daily oral medications targeting multiple cardiometabolic pathways simultaneously rather than single-disease treatments requiring complex polypharmacy regimens. Predictive analytics platforms are incorporating sleep parameters into cardiovascular risk algorithms where apnea-hypopnea index, oxygen desaturation frequency, and sleep fragmentation indices. For instance, ResMed Inc. uses cloud-connected systems and patient engagement platforms that analyse nightly sleep and therapy data to support remote monitoring and tailored feedback through its myAir and AirView services.
How Will Cardiometabolic-Sleep Comorbidity Treatment Market Expansion Unfold Across Key Global Regions?
The cardiometabolic-sleep comorbidity treatment market is poised for significant expansion with varying growth rates projected from 2026 to 2036. China leads with 14.0% CAGR driven by rapidly increasing obesity prevalence and expanding health insurance coverage for sleep disorder diagnosis and continuous positive airway pressure therapy. India follows at 12.5% benefiting from growing diabetes prevalence creating large OSA screening populations and increasing cardiometabolic disease awareness. The United States records 11.0% growth reflecting Medicare coverage expansion and value-based care program proliferation. Germany anticipates 9.5% CAGR from systematic cardiometabolic patient sleep screening protocols. France at 6.5%, United Kingdom at 5.0%, and Brazil at 3.5% show more moderate growth reflecting healthcare system constraints and reimbursement limitations.
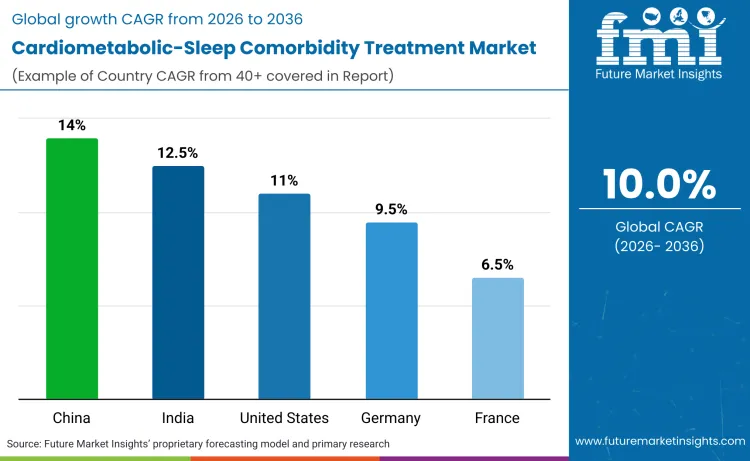
| Country | CAGR (2026 to 2036) |
|---|---|
| China | 14.0% |
| India | 12.5% |
| United States | 11.0% |
| Germany | 9.5% |
| France | 6.5% |
Source: Future Market Insights (FMI) analysis
How is Obesity Prevalence Growth Fueling China's 14.0% Expansion?
China's 14.0% expansion shows structural transformation as obesity rates doubled over the years. The National Health Commission incorporated sleep disorder screening into Healthy China 2030 chronic disease management initiatives, establishing policy frameworks supporting systematic evaluation in high-risk cardiometabolic populations. High demand for cardiometabolic sleep comorbidity treatment in China is being driven by rapid urbanization, aging demographics, and lifestyle patterns that elevate both metabolic and sleep related risk profiles.
Long working hours, night shift employment, and high screen exposure are contributing to widespread sleep deprivation, while dietary transitions and reduced physical activity continue to raise prevalence of obesity, diabetes, and hypertension. These conditions interact bidirectionally, with untreated sleep disorders such as obstructive sleep apnea worsening insulin resistance, blood pressure control, and cardiovascular risk, which heightens clinical urgency for integrated care pathways.
Why is Diabetes Burden Driving India's 12.5% Growth?
India's 12.5% growth is owing to the growing treatment requirement due to diabetes prevalence. India holds second position in terms of the number of adults (20-79 years) with diabetes in the world. High demand for cardiometabolic sleep comorbidity treatment in India is being shaped by accelerating urbanization, changing dietary patterns, and rising sedentary behavior across working age populations. Long commuting times, irregular work schedules, and late night screen use are contributing to chronic sleep disruption, while increasing intake of processed foods and reduced physical activity are driving higher rates of obesity, diabetes, and hypertension.
These conditions interact in ways that compound disease severity, as untreated sleep disorders worsen glycemic control, blood pressure stability, and cardiovascular risk. Large segments of the population present late in the disease course, increasing the clinical burden on hospitals and specialty clinics managing overlapping cardiology, endocrinology, and sleep disorders. Awareness of lifestyle linked chronic disease risks is improving among urban middle income groups, leading to higher screening uptake for sleep apnea and metabolic conditions.
How Does Medicare Coverage Support USA's 11.0% Growth?
U.S. maintains 11.0% CAGR owing to Medicare reimbursement expansion. In the United States, Medicare supports care delivery across a wide range of facility types that are certified to provide covered services to eligible beneficiaries. Acute care hospitals form the backbone of inpatient treatment under Medicare, providing medical, surgical, and specialty services for conditions that require hospitalization. Critical access hospitals serve rural communities with limited access to large medical centers, while inpatient rehabilitation facilities focus on post acute recovery for patients following stroke, trauma, or major surgery. Long term care hospitals manage medically complex cases that need extended inpatient treatment.
Outpatient and community based settings account for a large share of Medicare supported care. Ambulatory surgical centers deliver same day procedures, while federally qualified health centers and rural health clinics provide primary care and preventive services in underserved regions. Comprehensive outpatient rehabilitation facilities support physical therapy, occupational therapy, and speech therapy for functional recovery.
What Drives Germany's 9.5% CAGR in the Cardiometabolic-Sleep Comorbidity Treatment Market?
Germany's 9.5% expansion shows high prevalence of cardiovascular risk factors, and growing recognition of sleep disorders as contributors to chronic disease progression. A large proportion of adults live with hypertension, dyslipidemia, or type two diabetes, while sleep disruption linked to shift work, occupational stress, and digital device use is becoming more common across working age groups. These overlapping conditions interact clinically, as untreated sleep disorders worsen blood pressure control, glycemic stability, and long term cardiovascular outcomes, increasing the need for coordinated management.
Primary care and specialist services are reporting rising referrals for patients presenting with combined metabolic and sleep related complaints, creating demand for integrated care pathways. Strong preventive health orientation and routine screening practices support earlier identification of comorbid risks. Coverage through statutory health insurance improves access to diagnostics and long term therapy, while structured disease management programs encourage multidisciplinary coordination, driving sustained demand for comprehensive cardiometabolic and sleep focused treatment models across hospital and outpatient settings.
How Does U.K.'s NHS Integration Support 5.0% Growth?
United Kingdom's 5.0% growth operates within National Health Service budget constraints where integrated care systems are implementing risk-stratified pathways prioritizing severe OSA in high-risk cardiometabolic populations rather than universal screening approaches. Treatment approaches are placing greater emphasis on non pharmacological interventions such as structured lifestyle modification, weight management, and behavioral sleep therapy alongside standard cardiometabolic medications.
Service models are adapting to long term condition management frameworks that focus on sustained risk reduction rather than episodic treatment. These shifts are supported by digital care pathways, multidisciplinary coordination, and outcome tracking approaches that prioritize long term disease control, adherence support, and reduction of avoidable acute care utilization.
What Strategic Moves Are Defining Competitive Landscape of the Cardiometabolic-Sleep Comorbidity Treatment Market?
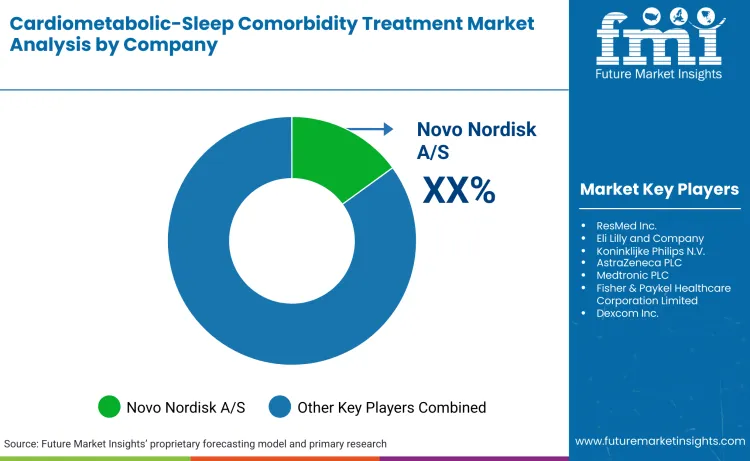
The competitive landscape experiences care model integration as device manufacturers partner with pharmaceutical companies and digital health platforms to offer comprehensive solutions rather than standalone products. ResMed's strategic investments in software development and remote patient monitoring create ecosystems connecting devices, data analytics, and clinical decision support, positioning the company as integrated care provider beyond traditional durable medical equipment supplier. These platform approaches enable recurring software subscription revenue augmenting one-time device sales.
In the UK, the cardiometabolic sleep comorbidity treatment market is shifting from fragmented, condition specific care toward more integrated, pathway based management models. Clinical practice is moving away from treating sleep disorders, diabetes, and cardiovascular disease in isolation and toward coordinated assessment within primary care and specialist referral networks. Screening for sleep apnea and insomnia is increasingly being incorporated into cardiometabolic risk assessments, supporting earlier identification of overlapping disease burdens. Care delivery is expanding beyond hospital based sleep clinics toward community settings, supported by virtual consultations and home based diagnostic tools that reduce waiting times and improve follow up continuity.
Key Industry Developments:
- In June 2025, Philips expanded its long-standing deal with Medtronic to enhance access to patient monitoring solutions
- In May 2025, Resmed acquired VirtuOx, a leading independent diagnostic testing facility (IDTF) for sleep, respiratory, and cardiac conditions to broaden its product portfolio.
Key Players in Cardiometabolic-Sleep Comorbidity Treatment Market
- Novo Nordisk A/S
- ResMed Inc.
- Eli Lilly and Company
- Koninklijke Philips N.V.
- AstraZeneca PLC
- Medtronic PLC
- Fisher & Paykel Healthcare Corporation Limited
- Dexcom Inc.
- Omron Healthcare Co. Ltd.
- Teladoc Health Inc.
Market Definition
The cardiometabolic-sleep comorbidity treatment market encompasses integrated clinical services, therapeutic interventions, and care coordination models designed to manage the overlapping burden of sleep disorders and cardiometabolic conditions, including obesity, type 2 diabetes, hypertension, cardiovascular disease, and heart failure. The market includes sleep apnea diagnosis and therapy platforms, cardiometabolic pharmacotherapy optimization programs, remote patient monitoring systems, and multidisciplinary care pathway solutions that align sleep medicine with cardiology and endocrinology workflows. Market size is measured in USD billion and analyzed over the 2026 to 2036 period.
The market comprises treatment components spanning positive airway pressure therapy, weight-loss pharmacotherapy, cardiometabolic medication optimization, digital monitoring tools, and structured care management services delivered through hospitals, sleep clinics, cardiometabolic specialty centers, home care networks, and payer-supported population health programs. Market expansion reflects growing clinical recognition of sleep-disordered breathing as a modifiable risk factor that directly influences cardiometabolic outcomes, driving demand for coordinated, pathway-based treatment models.
Market Inclusion
The cardiometabolic-sleep comorbidity treatment market scope includes clinical interventions categorized by treatment component such as sleep apnea devices and PAP therapy, pharmacological weight management including GLP-1 class therapies, hypertension and diabetes medication optimization programs, remote monitoring platforms integrating sleep and metabolic biomarkers, and lifestyle-supported care management services. Segmentation encompasses comorbidity pathways including OSA with obesity management, OSA with hypertension and cardiovascular risk control, OSA with type 2 diabetes management, heart failure with sleep-disordered breathing, and other metabolic sleep phenotypes.
The scope includes deployment across application settings such as hospitals and cardiometabolic clinics, sleep clinics and durable medical equipment networks, retail pharmacy-supported care programs, and payer-led population health management platforms. End users include healthcare providers, integrated delivery networks, digital health service providers, and payers implementing value-based care models. Geographic coverage spans North America, Europe, East Asia, South Asia, Latin America, and the Middle East and Africa, reflecting variations in reimbursement frameworks, digital health maturity, and integrated care adoption across healthcare systems.
Market Exclusion
The market excludes standalone sleep disorder management that is not linked to cardiometabolic disease pathways, as well as isolated cardiometabolic treatment programs that do not incorporate sleep disorder screening or therapy. General respiratory sleep care not connected to obesity, diabetes, hypertension, or cardiovascular risk management falls outside the defined scope.
The scope excludes consumer wellness applications focused on sleep tracking without clinical integration into cardiometabolic care pathways, lifestyle wellness programs without medical oversight, and general fitness or weight management products not prescribed or managed within clinical treatment frameworks. Non-clinical sleep aids, over-the-counter supplements, and generic digital wellness platforms lacking regulated therapeutic intent or professional healthcare integration are not included in the market analysis.
Scope of the Report
| Items | Values |
|---|---|
| Quantitative Units | USD million |
| Treatment Component | PAP Therapy And Sleep Apnea Devices; Weight-Loss Pharmacotherapy (GLP-1 And Others); Hypertension/Diabetes Meds Optimization Programs; Remote Monitoring And Risk Stratification Analytics; Lifestyle And Care-Management Services |
| Comorbidity Pathway | OSA + Obesity Management; OSA + Hypertension / CV Risk Control; OSA + Type-2 Diabetes Management; Heart Failure + Sleep-Disordered Breathing; Other Metabolic Sleep Phenotypes |
| End User | Hospitals And Cardiometabolic Clinics; Sleep Clinics / DME Networks; Retail Pharmacy Channel; Payers / Population Health Managers |
| Regions Covered | North America, Europe, East Asia, South Asia, Latin America, Middle East & Africa |
| Countries Covered | China, India, United States, Germany, France, and 40+ countries |
| Key Companies Profiled | Novo Nordisk A/S; ResMed Inc.; Eli Lilly and Company; Koninklijke Philips N.V.; AstraZeneca PLC; Others |
| Additional Attributes | Revenue analysis by treatment component, comorbidity pathway, and end user; performance in integrated care applications and coordination capabilities across hospitals, sleep clinics, and cardiometabolic specialty centers; treatment effectiveness enhancement, care pathway optimization, and platform benefits under clinical applications; impact on patient outcomes, treatment precision, and care coordination during implementation processes; compatibility with clinical protocols and treatment preferences; adoption dynamics driven by value-based care positioning, integrated care programs, and long-term patient management partnerships. |
Cardiometabolic-Sleep Comorbidity Treatment Market by Segments
By Treatment Component:
- PAP Therapy And Sleep Apnea Devices
- Weight-Loss Pharmacotherapy (GLP-1 And Others)
- Hypertension/Diabetes Meds Optimization Programs
- Remote Monitoring And Risk Stratification Analytics
- Lifestyle And Care-Management Services
By Comorbidity Pathway:
- OSA + Obesity Management
- OSA + Hypertension / CV Risk Control
- OSA + Type-2 Diabetes Management
- Heart Failure + Sleep-Disordered Breathing
- Other Metabolic Sleep Phenotypes
By End User:
- Hospitals And Cardiometabolic Clinics
- Sleep Clinics / DME Networks
- Retail Pharmacy Channel
- Payers / Population Health Managers
By Region:
- North America
- Europe
- East Asia
- South Asia
- Latin America
- Middle East & Africa
Bibliography
- State Council of the People’s Republic of China. (2023). China population development report 2023.
- Centers for Medicare & Medicaid Services. (2023). National coverage determination for continuous positive airway pressure (CPAP) therapy for obstructive sleep apnea (OSA).
- USA Food and Drug Administration. (2023). Digital health center of excellence.
Frequently Asked Questions
What is the current global market size for cardiometabolic-sleep comorbidity treatment?
The global market is slated to be valued at USD 7,850.60 million in 2026.
What is the projected compound annual growth rate (CAGR) for the cardiometabolic-sleep comorbidity treatment market over the next 10 years?
The market is projected to grow at 10.0% CAGR from 2026 to 2036, reaching USD 20,362.40 million by 2036.
Which countries are experiencing the fastest expansion in cardiometabolic-sleep comorbidity treatment market?
China leads with 14.0% growth, followed by India at 12.5% and the United States at 11.0%, driven by rising obesity rates, expanding diabetes burden, and Medicare coverage expansion respectively.
What are the primary drivers for cardiometabolic-sleep comorbidity treatment demand?
Clinical evidence demonstrating therapeutic interdependence where CPAP therapy improves metabolic control and payer value-based care initiatives rewarding multi-condition outcome improvement are fueling integrated care pathway adoption.
Who are the leading companies in the cardiometabolic-sleep comorbidity treatment industry?
Novo Nordisk, ResMed, Eli Lilly, Philips, and AstraZeneca are key players, differentiating through GLP-1 agonist development for OSA populations, connected PAP device ecosystems, digital health platform integration, and cardiometabolic pharmaceutical portfolios addressing multiple comorbid conditions.
Table of Content
- Cardiometabolic-Sleep Comorbidity Treatment Market Size and Share Forecast Outlook (2026 to 2036)
- Cardiometabolic-Sleep Comorbidity Treatment Market Forecast and Outlook (2026 to 2036)
- Cardiometabolic-Sleep Comorbidity Treatment Market Key Takeaways
- Key Shifts in the Cardiometabolic-Sleep Comorbidity Treatment Market from 2026 to 2036
- Cardiometabolic-Sleep Comorbidity Treatment Market Segmentation Analysis
- By Treatment Component
- PAP Therapy and Sleep Apnea Devices
- Weight-Loss Pharmacotherapy (GLP-1 and Others)
- Hypertension and Diabetes Medication Optimization Programs
- Remote Monitoring and Risk Stratification Analytics
- Lifestyle and Care-Management Services
- By Comorbidity Pathway
- OSA + Obesity Management
- OSA + Hypertension and Cardiovascular Risk Control
- OSA + Type 2 Diabetes Management
- Heart Failure + Sleep-Disordered Breathing
- Other Metabolic Sleep Phenotypes
- By End User
- Hospitals and Cardiometabolic Clinics
- Sleep Clinics and DME Networks
- Retail Pharmacy Channel
- Payers and Population Health Managers
- By Region
- By Treatment Component
- Market Dynamics and Growth Analysis
- Growth Drivers
- Market Restraints
- Strategic Trends
- Cardiometabolic-Sleep Comorbidity Treatment Market Global Analysis
- East Asia
- South Asia
- North America
- Europe
- Latin America
- Middle East & Africa
- Competitive Landscape Analysis
- Key Players in the Cardiometabolic-Sleep Comorbidity Treatment Market
- Market Definition, Inclusion, and Exclusion Criteria
- Scope of the Cardiometabolic-Sleep Comorbidity Treatment Market Report
- Cardiometabolic-Sleep Comorbidity Treatment Market by Segment
- Bibliography
- Frequently Asked Questions (FAQs)
List of Tables
- Global Cardiometabolic-Sleep Comorbidity Treatment Market Size (USD Million), 2021-2036
- Cardiometabolic-Sleep Comorbidity Treatment Market Y-o-Y Growth (%), 2021-2036
- Global Market Share by Treatment Component, 2026
- Global Market Share by Comorbidity Pathway, 2026
- Global Market Share by End User, 2026
- Cardiometabolic-Sleep Comorbidity Treatment Market Share by Region, 2026
- Market Share by Treatment Component (USD Million), 2026-2036
- Market Share by End User (USD Million), 2026-2036
- Key Player Market Share in the Cardiometabolic-Sleep Comorbidity Treatment Market
- Cardiometabolic-Sleep Comorbidity Treatment Market Absolute $ Opportunity (USD Million), 2026-2036
- Cardiometabolic-Sleep Comorbidity Treatment Market CAGR (%) by Region, 2026-2036
List of Figures
- Global Cardiometabolic-Sleep Comorbidity Treatment Market Size (USD Million), 2021-2036
- Cardiometabolic-Sleep Comorbidity Treatment Market Y-o-Y Growth (%) from 2021-2036
- Cardiometabolic-Sleep Comorbidity Treatment Market Share by Treatment Component (%) in 2026
- Cardiometabolic-Sleep Comorbidity Treatment Market Share by Comorbidity Pathway (%) in 2026
- Global Cardiometabolic-Sleep Comorbidity Treatment Market by Region (%) 2026-2036
- Global Cardiometabolic-Sleep Comorbidity Treatment Market by End User
- Competitive Landscape of Key Cardiometabolic-Sleep Comorbidity Treatment Market Players
- Market Trends in Cardiometabolic-Sleep Comorbidity Treatment
- Cardiometabolic-Sleep Comorbidity Treatment Adoption by Region
Full Research Suite comprises of:
Market outlook & trends analysis
Interviews & case studies
Strategic recommendations
Vendor profiles & capabilities analysis
5-year forecasts
8 regions and 60+ country-level data splits
Market segment data splits
12 months of continuous data updates
DELIVERED AS:
PDF EXCEL ONLINE

