Post-Acute Transition Care Coordination Platform Market
The Post-Acute Transition Care Coordination Platform Market Is Segmented By Deployment (Cloud, On-Premise, Hybrid), Module (Referral Management, Discharge Planning, Network Management, Authorization, Analytics), Care-Setting (Hospitals, SNFs, Home Health, Rehab Centers, ACOs), End User (Providers, Payers, Health Systems, Community Networks), Transition Type (Hospital-To-SNF, Hospital-To-Home, Hospital-To-Rehab, SNF-To-Home, Cross-Setting Follow-Up), And Region. Forecast For 2026 To 2036.
Historical Data Covered: 2016 to 2024 | Base Year: 2025 | Estimated Year: 2026 | Forecast Period: 2027 to 2036
Post-Acute Transition Care Coordination Platform Market Size, Market Forecast and Outlook By FMI
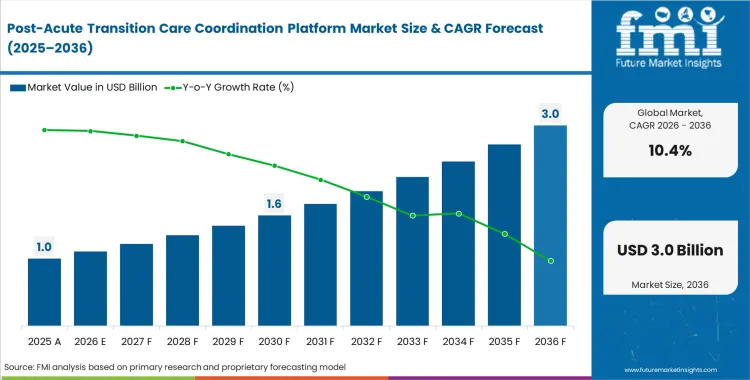
The post-acute transition care coordination platform market crossed a valuation of USD 0.9 billion in 2025, as the revenue is expected to grow USD 1.0 billion in 2026 at a CAGR of 10.4% during the forecast period. Rapid development in the industry demand lifts total valuation to USD 2.7 billion through 2036 as health systems face escalating readmission penalties tied directly to unstructured placement workflows.
Discharge planners face severe capacity bottlenecks that make manual facility matching commercially unviable. Placing high-acuity patients requires real-time bed visibility across multiple partner networks. Relying on phone inquiries extends hospital stays by days, costing facilities thousands per patient. Adopting home healthcare software integrations within a care transitions platform shifts placement from sequential calling to parallel digital broadcasting. Financial directors view post-discharge care coordination software not as an IT expense but as a direct length-of-stay reduction mechanism.
Summary of Post-Acute Transition Care Coordination Platform Market
- Market Snapshot
- In 2025, the post-acute transition care coordination platform market was worth USD 0.8 billion. Fast forward to 2036, and that total valuation is expected to hit USD 2.7 billion over the forecast period.
- That steady climb translates to a 10.8% compound annual growth rate between 2026 and 2036, effectively adding USD 1.7 billion in fresh revenue to the industry.
- At its core, this software is all about making the daily grind easier for nurses and case managers. Buyers are willing to spend money if a tool can visibly speed up discharges, track where referrals are going, and connect effortlessly with other facilities.
- Hospital administrators are finding it much easier to approve the budget for these platforms today, largely thanks to updated Medicare reimbursement rules and new national standards that strongly encourage better digital data sharing.
- Demand and Growth Drivers
- Nobody wants a patient taking up a hospital bed longer than medically necessary. That intense pressure is forcing health systems to figure out how to transition people to rehab, nursing homes, or home care without relying on messy, manual paperwork.
- Getting different computer systems to actually talk to each other is finally becoming a reality. Recent federal updates, like the 2025 SVAP and TEFCA rules, are giving hospitals the standardized framework they need to easily swap patient files with local clinics and nursing homes.
- Big health networks love standardizing their technology. With over 6,100 hospitals across the United States, most of which are community hospitals, there is a massive opportunity for tech buyers to roll out a single, unified platform across dozens of affiliated locations.
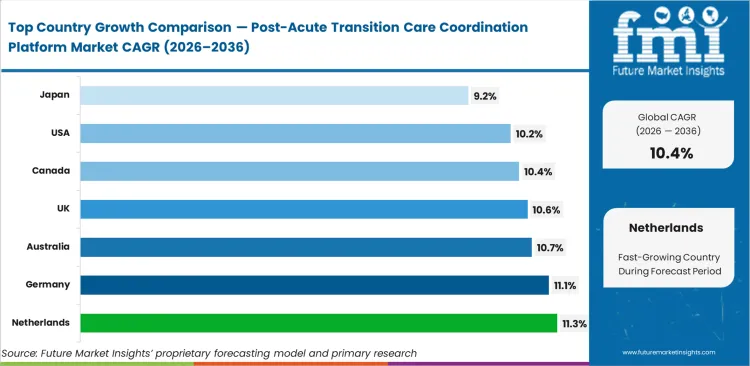
- Looking across the globe, the Netherlands is expanding the fastest with an 11.3% growth trajectory. Right behind it are Germany at 11.1% and Australia at 10.7%, followed closely by the United Kingdom at 10.6%, Canada at 10.4%, the United States at 10.2%, and Japan at 9.2%.
- Updating these new tools to older medical records is incredibly tough, especially when smaller nursing facilities still manage their admissions using faxes and phone calls.
- Product and Segment View
- This software automates the headache of finding an open bed, getting insurance approvals, and securely sending patient files through the cloud.
- Care teams rely on it every single day to coordinate a variety of moves, whether a patient is heading to a skilled nursing facility, going home with a visiting nurse, or transferring to a dedicated rehab center.
- As nobody wants to maintain expensive local servers, cloud-based systems completely dominate the space, easily capturing 62.0% of the industry.
- The most popular capability is referral management, taking up 29.0% of the share as it sits at the absolute center of the discharge process by showing case managers exactly who has an open bed and who is accepting new patients.
- The entire discharge journey starts the moment a patient is admitted, leading acute hospitals to being the biggest users, thereby making up 46.0% of the entire care-setting segment.
- When it comes to actually signing the software contracts, healthcare providers drive 58.0% of the demand, even though insurance companies are heavily invested in making sure these transitions go smoothly to avoid extra costs.
- Moving a patient from a hospital to a skilled nursing facility is incredibly complicated and risky, which is why that specific type of transition accounts for 34.0% of all platform usage.
- Reports an overview on tools built specifically to manage patient handoffs and track referral networks. General medical records, basic telehealth video apps, and standard health monitors do not make the cut.
- Geography and Competitive Outlook
- The United States still brings in the most reliable revenue because its massive hospital networks already have a strong foundation of installed software. Though European countries like the Netherlands and Germany are also experiencing fastest adoption rates.
- The vendor landscape seems fragmented. Winning a hospital's business usually comes down to how well the software plugs into their existing records, though occasionally these companies team up or buy each other out, like when Trella Health acquired Repisodic in 2025.
- Major names fighting for these contracts include WellSky (CarePort), Aidin, PointClickCare, Dina, Bamboo Health, Oracle Health, and Trella Health (Repisodic).
- Currently, WellSky (CarePort) is sitting at the forefront of the pack, earning the spot largely because they have spent years building a massive, pre-connected network of providers that new startups simply cannot match overnight.
Once daily hospital occupancy reliably exceeds eighty-five percent, manual routing fails entirely. Case managers trigger network-wide automated referral broadcasting to prevent emergency department boarding. Crossing this occupancy threshold forces health systems to mandate digital responses from partner skilled nursing facilities via hospital to post-acute transition software. Facility administrators who refuse electronic integration lose access to high-reimbursement patient volumes.
The Netherlands is expected to lead this market, with demand rising at a CAGR of 11.3% through 2036 as national health data exchanges require structured transfer records across care settings. Germany follows at 11.1%, supported by strong hospital digitization funding and wider system integration efforts. Australia is projected to witness 10.7% CAGR during the forecast period due to integrated regional health districts seeking unified patient tracking. The United Kingdom is likely to grow at a CAGR of 10.6%, driven by public trust adoption of automated discharge pathways. Canada is anticipated to record 10.4% CAGR as provincial integration programs continue to support coordinated care workflows. The United States is set to post 10.2% CAGR, with value-based care models pushing providers toward remote healthcare placement tools that help reduce readmissions. Japan is forecast to expand at 9.2% through 2036, though stricter localized data privacy rules continue to slow cloud-based deployment.
Segmental Analysis
Post-Acute Transition Care Coordination Platform Market Analysis by Deployment
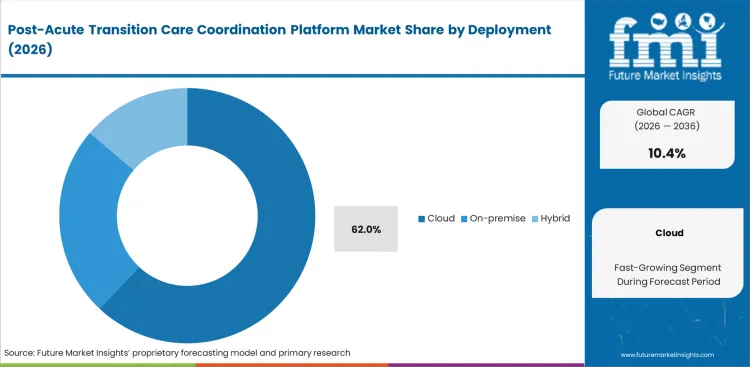
Legacy on-premise servers fail to connect unaffiliated nursing facilities operating outside hospital firewalls. IT directors at regional health systems approve cloud deployments to bypass complex VPN setups with dozens of small post-acute partners, explaining the 62.0% share reserved for this category of technology. FMI's assessment indicates multi-tenant architecture allows independent SNFs to receive broadcasted referrals without expensive local IT integration. Implementing AI powered care coordination via TEFCA post-acute interoperability software requires massive centralized datasets only accessible through scalable cloud infrastructure. What technology officers rarely emphasize is that cloud systems effectively shift security compliance burdens from small nursing homes to large platform vendors. Delaying cloud migration leaves hospital discharge teams manually faxing documents to facilities that have already moved to electronic workflows.
- Initial Trigger: IT directors authorize cloud platforms to eliminate point-to-point interface maintenance costs that rapidly bankrupt local technical resources. Chief information officers bypass legacy limitations.
- Qualification Gate: Security officers demand SOC 2 compliance and robust encryption standards before allowing patient payload transmission. Vendor certification libraries dictate procurement success.
- Expansion Motive: Chief medical officers scale cloud usage when real-time network visibility demonstrably reduces patient boarding hours in emergency departments. Network density accelerates adoption timelines.
Post-Acute Transition Care Coordination Platform Market Analysis by Module
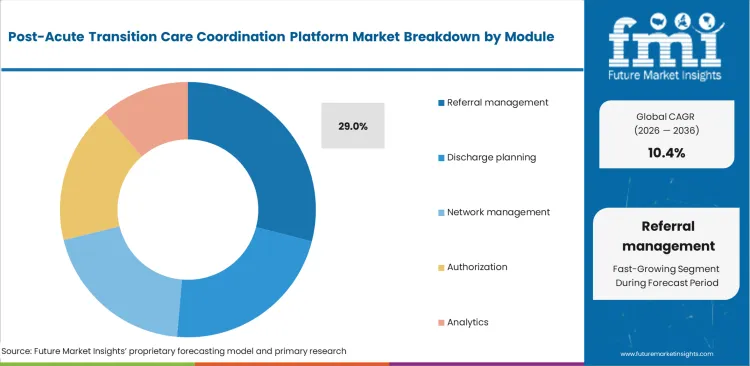
Broadcasting a single digital referral payload across dozens of facilities changes how placement teams manage discharge coordination for complex patients. Case managers in acute care settings use post-acute referral management software to place patients who need specialized bariatric or wound care beds. The referral management segment is estimated to account for 29.0% share in 2026, supported by the use of population health management platforms alongside referral data to identify facilities that are more likely to accept clinically complex cases. This improves referral precision and helps reduce unnecessary delays during patient transitions. Nursing administrators place greater importance on median time to first facility acceptance than on the total number of referrals sent. Case managers can assemble a single comprehensive clinical package and broadcast it immediately to a curated facility tier, reducing repeated phone-based coordination. Workflow efficiency weakens when receiving facilities face high notification volumes without proper acuity filtering. In such situations, admissions staff may overlook urgent placement requests, which slows transfer decisions for patients who are ready to leave acute care settings.
- Workflow Acceleration: Case managers compile a single comprehensive clinical package and broadcast it instantly to a curated facility tier. This replaces dozens of redundant telephone conversations.
- Hidden Friction: Admissions coordinators at receiving facilities suffer alert fatigue if platforms lack proper acuity filtering. High noise ratios cause staff to ignore critical placement requests.
- Lifecycle Outcome: Financial directors measure referral module success exclusively through reductions in avoidable inpatient days. Faster placement directly improves hospital operating margins.
Post-Acute Transition Care Coordination Platform Market Analysis by Care-Setting
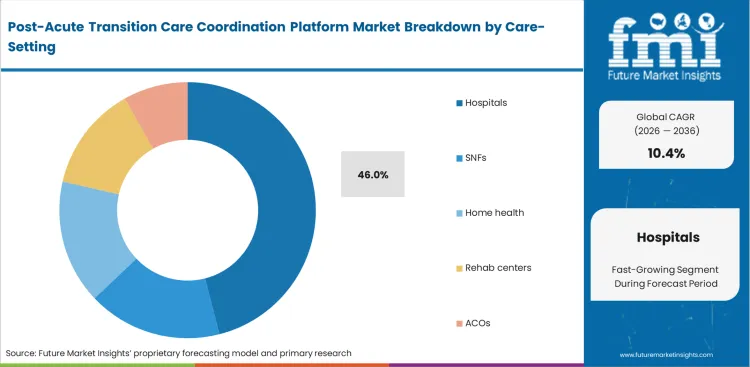
Financial penalties for excessive readmissions fall almost entirely on acute care facilities rather than receiving nursing homes. FMI notes that chief financial officers mandate care coordination software for hospitals to track patient trajectories after discharge. Discharge directors need real-time confirmation that a patient actually arrived at the designated post-acute bed. Utilizing patient engagement platforms in tandem ensures patients understand their transition destination before leaving the ward, enabling a capture of 46.0% share for hospitals in 2026. A surprising structural reality is that hospitals frequently pay software licensing fees on behalf of unaffiliated SNFs just to get them onto the communication network. Hospitals ignoring transition tracking risk millions in Medicare reimbursement clawbacks.
- Defensive Tracking: Chief financial officers deploy preferred post-acute network management software to document proper transition protocols. Audit trails defend against readmission penalties during Medicare reviews.
- Blindspot Persistence: Facilities often lose visibility if patients transfer a second time from a SNF to home care. Single-setting platforms fail to capture multi-step patient journeys.
- Capture Requirement: Quality directors must mandate complete platform usage by floor nurses to ensure accurate compliance reporting. Partial adoption ruins predictive analytic models.
Post-Acute Transition Care Coordination Platform Market Analysis by End User
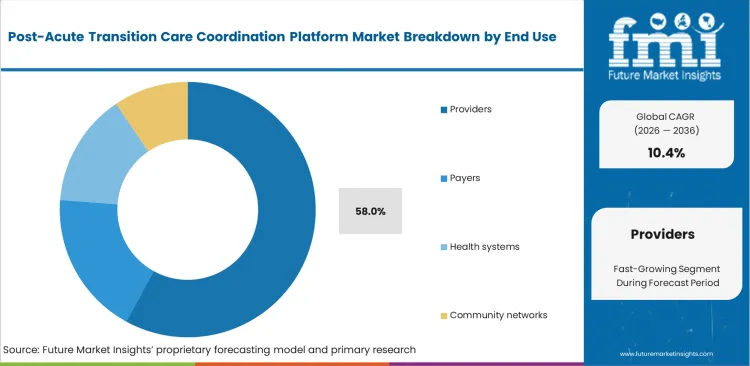
Care delivery organizations carry the operational burden of moving patients between available beds and care settings. FMI estimates suggest that clinical workflow demands influence adoption speed more strongly than payer reimbursement structures. Chief nursing officers adopt transitional care management workflow software because floor nurses spend too much time preparing transfer paperwork instead of focusing on patient care. The provider segment is estimated to account for 58.0% share in 2026. Integrating case management software reduces duplicate data entry across separate electronic medical record systems.
Health plan executives often assume providers exchange transition data smoothly, though the actual environment is far less cooperative. Competing hospitals may limit data sharing to retain control over patient networks and referral flows. This makes transition coordination more difficult for provider organizations managing discharge and transfer processes across multiple care settings. Groups that fail to streamline transitions often place more pressure on nursing teams, which can contribute to higher burnout and staff turnover.
- Primary Producers: Floor nurses generate the clinical payloads required for successful transitions. Software must pull data seamlessly from EMRs to prevent duplicate documentation tasks.
- Supply Limitations: Independent physicians frequently lack access to hospital-purchased coordination tools. This disconnect delays crucial medication reconciliation upon discharge.
- Future Trajectory: Chief medical officers will increasingly demand systems that automatically alert primary care doctors the moment a patient leaves the hospital building.
Post-Acute Transition Care Coordination Platform Market Analysis by Transition Type
Joint replacement and stroke pathways demand immediate high-intensity rehabilitation outside the acute hospital leading the hospital-to-SNF transitions claim 34.0% share in 2026. FMI's analysis indicates this specific pathway involves the highest density of clinical documentation exchange. Admissions managers at skilled nursing facilities require extensive medication lists, physical therapy notes, and physician orders before accepting liability for a patient via hospital to SNF discharge software. Adopting value based healthcare services forces facilities to monitor this exact transition for quality metric compliance. The operational irony is that a platform's success depends less on hospital IT architecture and more on whether a night-shift SNF nurse finds the interface usable. Delaying implementation of automated SNF routing guarantees prolonged emergency room bottlenecks.
- First Movers: Orthopedic service lines adopt digital transitions first due to predictable post-surgical pathways. Standardized protocols make these patients ideal candidates for automated placement.
- Subsequent Adopters: Complex medical oncology transitions follow as platforms improve capability to handle highly variable clinical payloads.
- Final Holdouts: Behavioral health transitions remain heavily manual due to severe bed shortages. Complex legal consent requirements restrict psychiatric data exchange capabilities.
Post-Acute Transition Care Coordination Platform Market Drivers, Restraints, and Opportunities
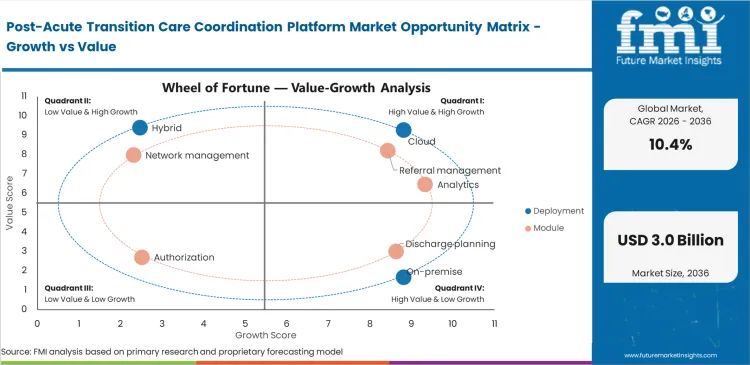
Hospital finance leaders face massive pressure as medicare now penalizes them if patients end up back in the hospital too soon. Discharge teams can no longer just hand a patient a stack of paper instructions and hope everything works out. The hospitals that fail to secure a right rehab bed or nursing facility, Medicare stops their funding directly. This harsh financial reality makes the financial return, or post-acute placement software, into something that the entire board of directors need to be careful about. By adopting digital healthcare tools, hospitals create a reliable digital paper trail, making it mandatory for them to prove electronically that they actually communicated with the next care team to guarantee a safe handoff.
The biggest roadblock is that not every nursing home uses modern digital records, which completely breaks down the coordination process. Many independent nursing facilities are stuck using older computer systems that simply cannot accept detailed patient files from a modern EHR-integrated discharge planning platform. Upgrading a healthcare contact center solution can help staff manage the back-and-forth communication, but it does not solve the core problem of different computer systems refusing to talk to each other. When a receiving facility lacks the right software, hospital case managers are forced to do the one thing they hate most that is to go back to sending complex medical histories via fax machine.
- Predictive Placement: Analytics engines flag patients highly likely to require complex SNF care upon admission rather than waiting until discharge day. Case managers begin placement searches 72 hours earlier.
- Transportation Integration: APIs connecting healthcare interoperability solutions directly to non-emergency medical transport fleets. Discharge planners secure a bed and a wheelchair van simultaneously.
- Specialty Matching: Routing a FHIR-based discharge coordination platform designed exclusively for dialysis or ventilator-dependent patients. Admissions directors filter out incompatible referrals instantly.
Regional Analysis
Based on regional analysis, the market is segmented into North America, Latin America, Western Europe, Eastern Europe, Asia Pacific, Middle East, and Africa across 40 plus countries.
.webp)
| Country | CAGR (2026 to 2036) |
|---|---|
| United States | 10.2% |
| Germany | 11.1% |
| United Kingdom | 10.6% |
| Canada | 10.4% |
| Australia | 10.7% |
| Netherlands | 11.3% |
| Japan | 9.2% |
Source: Future Market Insights (FMI) analysis, based on proprietary forecasting model and primary research
North America Post-Acute Transition Care Coordination Platform Market Analysis
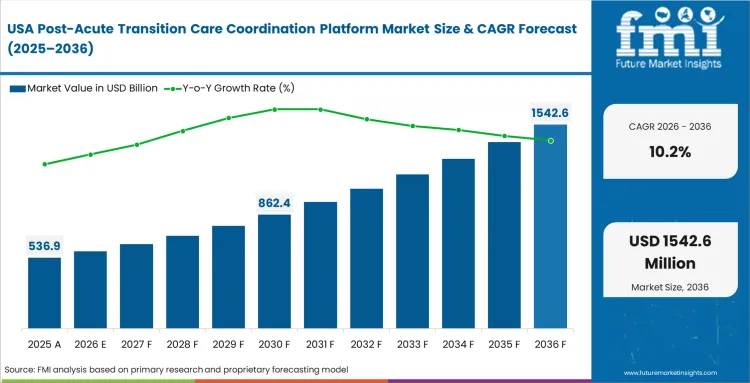
Across North America, the fear of financial penalties tied to patient readmissions is a massive catalyst forcing health systems to monitor transitions obsessively. Case management leaders are actively deploying prior authorization for post-acute placement software so that individuals transition into suitable facilities without getting stuck in administrative limbo. According to FMI's assessment, the underlying software architecture here is heavily shaped by strict federal interoperability mandates.
- United States: Hospital financial officers across the US post-acute care coordination platform market are aggressively purchasing coordination software to navigate strict Medicare readmission penalty programs. By leveraging remote patient monitoring system architectures, these networks can securely track individuals the moment they leave a skilled nursing facility. The push to lock down transition workflows against value-based care penalties sustains a 10.2% CAGR adoption rate across the sector.
- Canada: The Canada care transitions platform market is transforming with a rapid 10.4% CAGR through the coming decade, as provincial health authorities mandate unified regional discharge platforms to clear severe acute bed backlogs. Public hospitals are finally abandoning isolated legacy systems and utilizing clinical workflow solutions to standardize referral data across entire provinces. This shift finally gives chief medical officers real-time visibility into the actual availability of provincial SNF beds.
FMI's report includes Mexico and further involves assesses that the cross-border care networks slowly adopt basic referral portals to manage medical tourism transitions.
Western Europe Post-Acute Transition Care Coordination Platform Market Analysis
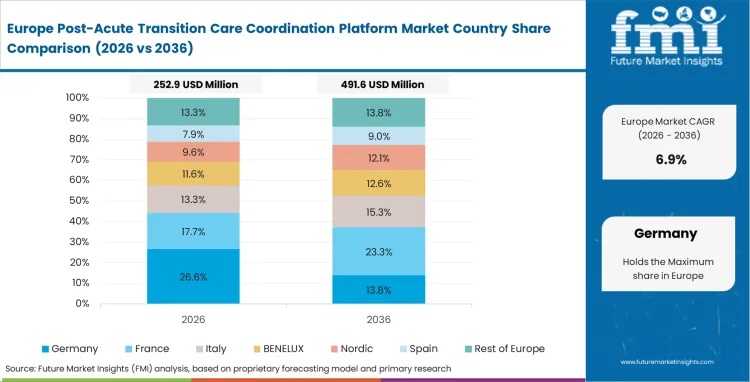
European transition workflows are being completely rewired by national directives that demand structured, electronic data sharing between care settings. Administrators running public trusts are moving away from isolated hospital software, favoring regional communication backbones instead. FMI notes that while rigorous privacy laws initially slowed the rollout of cloud tools, they are now actually fueling the need for highly secure, localized regional platforms.
- Netherlands: Every public health entity in the Netherlands care coordination platform market is now forced to digitize their entire workflow due to national mandates that require standardized digital transfer records. Vendors who can provide compliant data payloads are easily securing exclusive regional contracts. Because every facility must comply with these strict data exchange laws, adoption proceeds at an 11.3% pace over the forecast period.
- Germany: The Hospital Future Act is pumping massive capital directly into digital transition infrastructure across the Germany post-acute transition software market. The scramble among hospital administrators to secure federal funding before the deadlines expire fuels an 11.1% CAGR as facilities rapidly overhaul their systems. To satisfy grant requirements, many facilities are intelligently deploying connected RHM (remote healthcare monitoring) capabilities alongside their primary placement tools.
- United Kingdom: Establishing a robust 10.6% CAGR over the forecast horizon, the UK discharge planning software market is evolving as NHS trusts mandate automated placement workflows to combat chronic winter bed shortages. By integrating global digital health initiatives, health authorities are forcing scattered care homes to adopt standardized systems or face penalties for relying on outdated paper transitions. As a result, this allows ward managers to reclaim thousands of nursing hours previously wasted on endless phone calls.
FMI's assesses, the regional health authorities increasingly demand real-time visibility into post-acute capacity during infectious disease surges. The report includes France and Italy as well.
Asia Pacific Post-Acute Transition Care Coordination Platform Market Analysis
Healthcare systems across Asia are feeling the immense strain of severe demographic aging, which is rapidly depleting acute bed capacity. Hospital administrators are under intense pressure to quickly and safely discharge elderly patients into specialized care facilities. FMI observes that while highly fragmented post-acute networks make digital coordination complicated in this region, the sheer volume of patients makes these tools absolutely essential.
- Australia: Integrated care mandates within the Australia post-acute referral software market are pushing regional health districts to adopt unified placement platforms. State governments actively funding infrastructure to connect public hospitals with private aged care facilities push the sector at a 10.7% annual rate. This connectivity empowers discharge directors to completely eliminate the dangerous medication errors that frequently occur during manual paper transitions.
- Japan: Navigating the Japan discharge coordination software market requires vendors to build highly customized, region-specific data silos due to exceptionally strict localized privacy laws. Implementing architectures like a real time E-healthcare system means actively working around complex municipal regulations. Because of this ongoing friction between national healthcare goals and local compliance restrictions, the adoption pace sits at a more measured 9.2% compared to Western counterparts.
FMI's report includes China and India. Major metropolitan hospital networks begin trialing internal transition platforms to manage high-volume step-down facilities. Integrating hospital capacity management solutions becomes essential for maintaining flow in mega-facilities.
Competitive Aligners for Market Players
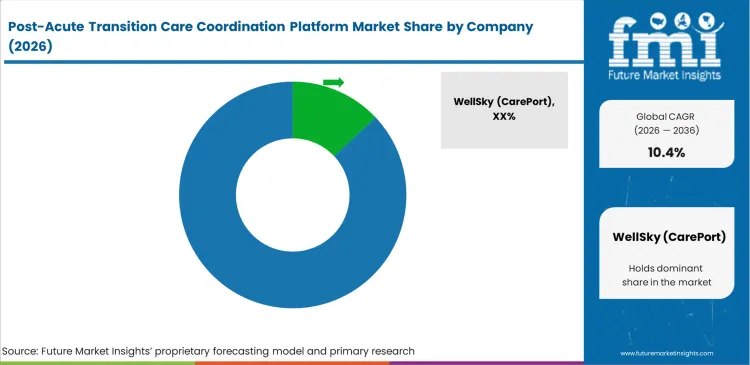
Winning contracts in this sector depends heavily on network depth. Hospital finance teams are not choosing software only for a clean interface. They want immediate access to a large, active network of nursing homes and rehab centers that can take patients quickly. WellSky (CarePort) and PointClickCare stay strong in many regional markets because so many receiving facilities already use their systems. Smaller vendors such as Aidin compete by making discharge work easier for care teams and by helping planners get faster responses to placement requests.
Established vendors are protected by how difficult hospital integration work can be. Building a dependable two-way connection with highly customized hospital record systems usually takes years of security reviews, technical mapping, and internal coordination. Oracle Health has a clear advantage because it already sits close to core hospital record infrastructure. Bamboo Health benefits from its background in tracking admissions and patient movement across unaffiliated care settings. Startups often discover that pulling an accurate and current medication list from a large hospital database is far more difficult than expected. Vendors with hospital capacity management solutions can build on that advantage by supporting faster bed matching.
Large health systems still use contract renewals to avoid depending too heavily on one vendor. Chief information officers increasingly want platforms that can share data easily and push transition metrics into internal dashboards. That creates opportunities for Dina, which connects hospitals with fragmented home-based care networks, and Trella Health (Repisodic), which gives discharge teams performance data on nursing homes at the time of referral. Hospitals reviewing discharge planning platforms know that control over transition data gives them leverage. Platforms that make data export difficult are more likely to lose ground to vendors that treat interoperability as a basic expectation.
Key Players in Post-Acute Transition Care Coordination Platform Market
- WellSky (CarePort)
- Aidin
- PointClickCare
- Dina
- Bamboo Health
- Oracle Health
- Trella Health (Repisodic)
Scope of the Report
| Metric | Value |
|---|---|
| Quantitative Units | USD 1.0 billion to USD 2.7 billion, at a CAGR of 10.4% |
| Market Definition | Post-Acute Transition Care Coordination Platform consists of digital infrastructure routing patient clinical data and placement requests between acute hospitals and secondary care facilities to minimize length-of-stay and readmissions. |
| Segmentation | By Deployment, By Module, By Care-Setting, By End User, By Transition Type, and Region |
| Regions Covered | North America, Latin America, Western Europe, Eastern Europe, Asia Pacific, Middle East and Africa |
| Countries Covered | United States, Germany, United Kingdom, Canada, Australia, Netherlands, Japan, Mexico, France, Italy, China, India |
| Key Companies Profiled | WellSky (CarePort), Aidin, PointClickCare, Dina, Bamboo Health, Oracle Health, Trella Health (Repisodic) |
| Forecast Period | 2026 to 2036 |
| Approach | Annual discharge volumes routed through electronic clearinghouses provide baseline valuation models. |
Source: Future Market Insights (FMI) analysis, based on proprietary forecasting model and primary research
Post-Acute Transition Care Coordination Platform Market Segments
Deployment
- Cloud
- On-premise
- Hybrid
Module
- Referral management
- Discharge planning
- Network management
- Authorization
- Analytics
Care-Setting
- Hospitals
- SNFs
- Home health
- Rehab centers
- ACOs
End User
- Providers
- Payers
- Health systems
- Community networks
Transition Type
- Hospital-to-SNF
- Hospital-to-home
- Hospital-to-rehab
- SNF-to-home
- Cross-setting follow-up
Regions:
- North America
- United States
- Canada
- Latin America
- Brazil
- Mexico
- Europe
- Netherlands
- Germany
- United Kingdom
- France
- Italy
- Spain
- Asia-Pacific & ASEAN
- China
- Japan
- South Korea
- India
- Australia
Bibliography
- Anderson, T. S., O’Donoghue, A. L., Herzig, S. J., Cohen, M. L., Aung, N., Dechen, T., Landon, B. E., & Stevens, J. P. (2024). Differences in primary care follow-up after acute care discharge within and across health systems: A retrospective cohort study. Journal of General Internal Medicine, 39(8), 1431-1437.
- Barrett, J. B., Trambley, A., Blessinger, E. K., Sexton, M. M., Lupica, M., Hasselblad, M., Cunningham, K. E., Kripalani, S., & Choma, N. N. (2025). Reduced hospital readmissions through personalized care: Implementation of a patient, risk-focused hospital-wide discharge care center. NEJM Catalyst Innovations in Care Delivery, 6(6).
- Centers for Medicare & Medicaid Services. (2024, January 17). CMS interoperability and prior authorization final rule (CMS-0057-F).
- Gabriel, M. H., Richwine, C., Strawley, C., Barker, W., & Everson, J. (2024). Interoperable exchange of patient health information among USA hospitals: 2023 (Data Brief No. 71). Office of the National Coordinator for Health Information Technology.
- Office of the National Coordinator for Health Information Technology, Department of Health and Human Services. (2024, January 9). Health data, technology, and interoperability: Certification program updates, algorithm transparency, and information sharing. Federal Register.
This bibliography is provided for reader reference. The full FMI report contains the complete reference list with primary source documentation.
This Report Addresses
- Discharge planning directors evaluating cloud platforms for immediate referral broadcasting.
- Chief medical officers requiring structured clinical payloads to prevent SNF admission rejections.
- IT administrators managing VPN connections replacing legacy on-premise systems with multi-tenant networks.
- Financial directors tracking readmission penalties directly tied to manual post-acute placement failures.
- Admissions coordinators at skilled nursing facilities needing automated acuity filtering to reduce alert fatigue.
- Orthopedic service lines demanding specialized hospital to home transition platform workflows.
- Quality directors mandating platform compliance to secure Medicare value-based reimbursement metrics.
- Regional health districts implementing unified cross-facility networks to eliminate emergency department boarding.
Frequently Asked Questions
What is the valuation of the industry in 2026?
Revenue is expected to cross USD 1.0 billion in 2026.
What is the projected value by 2036?
Sustained investment lifts total valuation to USD 2.7 billion by 2036.
What is the expected CAGR for this sector?
Demand expands at a compound annual growth rate of 10.4% from 2026 to 2036.
Which deployment type holds the largest share?
Cloud deployment captures 62.0% share because it enables unaffiliated nursing facilities to access hospital networks without complex local IT integration.
Why does referral management dominate module selection?
Case managers rely on referral management modules to broadcast patient payloads simultaneously, drastically reducing median placement time.
Which care setting drives the most demand?
Hospitals hold 46.0% share because acute facilities bear almost all financial penalties associated with excessive readmissions.
Why do providers lead end-user adoption?
Providers command 58.0% share as floor nurses require integrated tools to compile clinical data without redundant electronic medical record documentation.
What makes hospital-to-SNF the dominant transition type?
High-volume orthopedic and stroke pathways require extensive clinical documentation exchange before nursing facilities accept liability.
How does Netherlands maintain its growth rate?
Netherlands tracks at 11.3% driven entirely by strict national mandates requiring structured digital data exchange between all public health entities.
Why does Japan lag behind European growth?
Japan expands at 9.2% as highly localized data privacy regulations prevent the deployment of efficient centralized cloud networks.
What drives adoption of discharge planning and referral automation software?
Hospital financial officers mandate these tools because value-based care models penalize facilities for unstructured patient leakage and readmissions.
How do TEFCA and FHIR affect post-acute coordination software demand?
These frameworks standardize interoperability protocols, allowing disparate software systems to securely exchange patient payloads across unaffiliated care settings.
Why are hospitals buying care transitions platforms now?
Severe bed capacity constraints compel discharge directors to broadcast placement requests simultaneously rather than relying on sequential phone calls.
How is this niche different from long-term post-acute care software?
This software specifically handles the routing and placement logistics between facilities rather than the long-term clinical management of the patient.
What are the main barriers to adoption?
Uneven electronic medical record capabilities among independent nursing facilities prevent seamless receipt of digital clinical payloads.
Which vendors offer post-acute referral automation?
Major providers include WellSky, Aidin, PointClickCare, Dina, Bamboo Health, Oracle Health, and Trella Health.
How do platforms reduce emergency department boarding?
Automated routing algorithms place complex patients faster by instantly matching required medical acuity with available regional bed inventory.
Why do incumbents hold a competitive advantage?
Established vendors possess certified bi-directional API connections with legacy hospital EMRs that take startups years to replicate.
How do large health systems resist vendor lock-in?
Chief information officers demand standards-based data payloads capable of exporting placement analytics to internal data lakes.
What role does SOC 2 compliance play in procurement?
Hospital security officers strictly reject platforms lacking robust encryption standards due to the massive volume of protected health information transmitted.
Why is alert fatigue a problem for receiving facilities?
Admissions coordinators ignore digital referrals when platforms fail to properly filter cases matching their specific clinical capabilities.
How do APIs improve the discharge process?
Connecting placement platforms directly to non-emergency medical transport fleets allows planners to secure a bed and a ride simultaneously.
Why are behavioral health transitions difficult to automate?
Complex legal consent requirements regarding psychiatric data exchange prevent seamless automated clinical payload transfers.
What changes when occupancy exceeds eighty-five percent?
Manual sequential phone calling fails completely, forcing administrators to mandate automated referral broadcasting to maintain hospital flow.
Table of Content
- Executive Summary
- Global Market Outlook
- Demand to side Trends
- Supply to side Trends
- Technology Roadmap Analysis
- Analysis and Recommendations
- Market Overview
- Market Coverage / Taxonomy
- Market Definition / Scope / Limitations
- Research Methodology
- Chapter Orientation
- Analytical Lens and Working Hypotheses
- Market Structure, Signals, and Trend Drivers
- Benchmarking and Cross-market Comparability
- Research Design and Evidence Framework
- Desk Research Programme (Secondary Evidence)
- Company Annual and Sustainability Reports
- Peer-reviewed Journals and Academic Literature
- Corporate Websites, Product Literature, and Technical Notes
- Earnings Decks and Investor Briefings
- Statutory Filings and Regulatory Disclosures
- Technical White Papers and Standards Notes
- Trade Journals, Industry Magazines, and Analyst Briefs
- Conference Proceedings, Webinars, and Seminar Materials
- Government Statistics Portals and Public Data Releases
- Press Releases and Reputable Media Coverage
- Specialist Newsletters and Curated Briefings
- Sector Databases and Reference Repositories
- FMI Internal Proprietary Databases and Historical Market Datasets
- Subscription Datasets and Paid Sources
- Social Channels, Communities, and Digital Listening Inputs
- Additional Desk Sources
- Expert Input and Fieldwork (Primary Evidence)
- Primary Modes
- Qualitative Interviews and Expert Elicitation
- Quantitative Surveys and Structured Data Capture
- Blended Approach
- Why Primary Evidence is Used
- Field Techniques
- Interviews
- Surveys
- Presidents and Vice Presidents
- R&D and Innovation Heads
- Technical Specialists
- Domain Subject-matter Experts
- Scientists
- Physicians and Other Healthcare Professionals
- Governance, Ethics, and Data Stewardship
- Research Ethics
- Data Integrity and Handling
- Primary Modes
- Tooling, Models, and Reference Databases
- Desk Research Programme (Secondary Evidence)
- Data Engineering and Model Build
- Data Acquisition and Ingestion
- Cleaning, Normalisation, and Verification
- Synthesis, Triangulation, and Analysis
- Quality Assurance and Audit Trail
- Market Background
- Market Dynamics
- Drivers
- Restraints
- Opportunity
- Trends
- Scenario Forecast
- Demand in Optimistic Scenario
- Demand in Likely Scenario
- Demand in Conservative Scenario
- Opportunity Map Analysis
- Product Life Cycle Analysis
- Supply Chain Analysis
- Investment Feasibility Matrix
- Value Chain Analysis
- PESTLE and Porter’s Analysis
- Regulatory Landscape
- Regional Parent Market Outlook
- Production and Consumption Statistics
- Import and Export Statistics
- Market Dynamics
- Global Market Analysis 2021 to 2025 and Forecast, 2026 to 2036
- Historical Market Size Value (USD Million) Analysis, 2021 to 2025
- Current and Future Market Size Value (USD Million) Projections, 2026 to 2036
- Y to o to Y Growth Trend Analysis
- Absolute $ Opportunity Analysis
- Global Market Pricing Analysis 2021 to 2025 and Forecast 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Deployment
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Deployment , 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Deployment , 2026 to 2036
- Cloud
- On-premise
- Hybrid
- Cloud
- Y to o to Y Growth Trend Analysis By Deployment , 2021 to 2025
- Absolute $ Opportunity Analysis By Deployment , 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Module
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Module, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Module, 2026 to 2036
- Referral management
- Discharge planning
- Network management
- Authorization
- Analytics
- Referral management
- Y to o to Y Growth Trend Analysis By Module, 2021 to 2025
- Absolute $ Opportunity Analysis By Module, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Care-Setting
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Care-Setting, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Care-Setting, 2026 to 2036
- Hospitals
- SNFs
- Home health
- Rehab centers
- ACOs
- Hospitals
- Y to o to Y Growth Trend Analysis By Care-Setting, 2021 to 2025
- Absolute $ Opportunity Analysis By Care-Setting, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By End Use
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By End Use, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By End Use, 2026 to 2036
- Providers
- Payers
- Health systems
- Community networks
- Providers
- Y to o to Y Growth Trend Analysis By End Use, 2021 to 2025
- Absolute $ Opportunity Analysis By End Use, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Region
- Introduction
- Historical Market Size Value (USD Million) Analysis By Region, 2021 to 2025
- Current Market Size Value (USD Million) Analysis and Forecast By Region, 2026 to 2036
- North America
- Latin America
- Western Europe
- Eastern Europe
- East Asia
- South Asia and Pacific
- Middle East & Africa
- Market Attractiveness Analysis By Region
- North America Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- USA
- Canada
- Mexico
- By Deployment
- By Module
- By Care-Setting
- By End Use
- By Country
- Market Attractiveness Analysis
- By Country
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Key Takeaways
- Latin America Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Brazil
- Chile
- Rest of Latin America
- By Deployment
- By Module
- By Care-Setting
- By End Use
- By Country
- Market Attractiveness Analysis
- By Country
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Key Takeaways
- Western Europe Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Germany
- UK
- Italy
- Spain
- France
- Nordic
- BENELUX
- Rest of Western Europe
- By Deployment
- By Module
- By Care-Setting
- By End Use
- By Country
- Market Attractiveness Analysis
- By Country
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Key Takeaways
- Eastern Europe Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Russia
- Poland
- Hungary
- Balkan & Baltic
- Rest of Eastern Europe
- By Deployment
- By Module
- By Care-Setting
- By End Use
- By Country
- Market Attractiveness Analysis
- By Country
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Key Takeaways
- East Asia Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- China
- Japan
- South Korea
- By Deployment
- By Module
- By Care-Setting
- By End Use
- By Country
- Market Attractiveness Analysis
- By Country
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Key Takeaways
- South Asia and Pacific Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- India
- ASEAN
- Australia & New Zealand
- Rest of South Asia and Pacific
- By Deployment
- By Module
- By Care-Setting
- By End Use
- By Country
- Market Attractiveness Analysis
- By Country
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Key Takeaways
- Middle East & Africa Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Kingdom of Saudi Arabia
- Other GCC Countries
- Turkiye
- South Africa
- Other African Union
- Rest of Middle East & Africa
- By Deployment
- By Module
- By Care-Setting
- By End Use
- By Country
- Market Attractiveness Analysis
- By Country
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Key Takeaways
- Key Countries Market Analysis
- USA
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Canada
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Mexico
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Brazil
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Chile
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Germany
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- UK
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Italy
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Spain
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- France
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- India
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- ASEAN
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Australia & New Zealand
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- China
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Japan
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- South Korea
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Russia
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Poland
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Hungary
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Kingdom of Saudi Arabia
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Turkiye
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- South Africa
- Pricing Analysis
- Market Share Analysis, 2025
- By Deployment
- By Module
- By Care-Setting
- By End Use
- USA
- Market Structure Analysis
- Competition Dashboard
- Competition Benchmarking
- Market Share Analysis of Top Players
- By Regional
- By Deployment
- By Module
- By Care-Setting
- By End Use
- Competition Analysis
- Competition Deep Dive
- WellSky (CarePort)
- Overview
- Product Portfolio
- Profitability by Market Segments (Product/Age /Sales Channel/Region)
- Sales Footprint
- Strategy Overview
- Marketing Strategy
- Product Strategy
- Channel Strategy
- Aidin
- PointClickCare
- Dina
- Bamboo Health
- Oracle Health
- Trella Health (Repisodic)
- WellSky (CarePort)
- Competition Deep Dive
- Assumptions & Acronyms Used
List of Tables
- Table 1: Global Market Value (USD Million) Forecast by Region, 2021 to 2036
- Table 2: Global Market Value (USD Million) Forecast by Deployment , 2021 to 2036
- Table 3: Global Market Value (USD Million) Forecast by Module, 2021 to 2036
- Table 4: Global Market Value (USD Million) Forecast by Care-Setting, 2021 to 2036
- Table 5: Global Market Value (USD Million) Forecast by End Use, 2021 to 2036
- Table 6: North America Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 7: North America Market Value (USD Million) Forecast by Deployment , 2021 to 2036
- Table 8: North America Market Value (USD Million) Forecast by Module, 2021 to 2036
- Table 9: North America Market Value (USD Million) Forecast by Care-Setting, 2021 to 2036
- Table 10: North America Market Value (USD Million) Forecast by End Use, 2021 to 2036
- Table 11: Latin America Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 12: Latin America Market Value (USD Million) Forecast by Deployment , 2021 to 2036
- Table 13: Latin America Market Value (USD Million) Forecast by Module, 2021 to 2036
- Table 14: Latin America Market Value (USD Million) Forecast by Care-Setting, 2021 to 2036
- Table 15: Latin America Market Value (USD Million) Forecast by End Use, 2021 to 2036
- Table 16: Western Europe Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 17: Western Europe Market Value (USD Million) Forecast by Deployment , 2021 to 2036
- Table 18: Western Europe Market Value (USD Million) Forecast by Module, 2021 to 2036
- Table 19: Western Europe Market Value (USD Million) Forecast by Care-Setting, 2021 to 2036
- Table 20: Western Europe Market Value (USD Million) Forecast by End Use, 2021 to 2036
- Table 21: Eastern Europe Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 22: Eastern Europe Market Value (USD Million) Forecast by Deployment , 2021 to 2036
- Table 23: Eastern Europe Market Value (USD Million) Forecast by Module, 2021 to 2036
- Table 24: Eastern Europe Market Value (USD Million) Forecast by Care-Setting, 2021 to 2036
- Table 25: Eastern Europe Market Value (USD Million) Forecast by End Use, 2021 to 2036
- Table 26: East Asia Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 27: East Asia Market Value (USD Million) Forecast by Deployment , 2021 to 2036
- Table 28: East Asia Market Value (USD Million) Forecast by Module, 2021 to 2036
- Table 29: East Asia Market Value (USD Million) Forecast by Care-Setting, 2021 to 2036
- Table 30: East Asia Market Value (USD Million) Forecast by End Use, 2021 to 2036
- Table 31: South Asia and Pacific Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 32: South Asia and Pacific Market Value (USD Million) Forecast by Deployment , 2021 to 2036
- Table 33: South Asia and Pacific Market Value (USD Million) Forecast by Module, 2021 to 2036
- Table 34: South Asia and Pacific Market Value (USD Million) Forecast by Care-Setting, 2021 to 2036
- Table 35: South Asia and Pacific Market Value (USD Million) Forecast by End Use, 2021 to 2036
- Table 36: Middle East & Africa Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 37: Middle East & Africa Market Value (USD Million) Forecast by Deployment , 2021 to 2036
- Table 38: Middle East & Africa Market Value (USD Million) Forecast by Module, 2021 to 2036
- Table 39: Middle East & Africa Market Value (USD Million) Forecast by Care-Setting, 2021 to 2036
- Table 40: Middle East & Africa Market Value (USD Million) Forecast by End Use, 2021 to 2036
List of Figures
- Figure 1: Global Market Pricing Analysis
- Figure 2: Global Market Value (USD Million) Forecast 2021-2036
- Figure 3: Global Market Value Share and BPS Analysis by Deployment , 2026 and 2036
- Figure 4: Global Market Y-o-Y Growth Comparison by Deployment , 2026-2036
- Figure 5: Global Market Attractiveness Analysis by Deployment
- Figure 6: Global Market Value Share and BPS Analysis by Module, 2026 and 2036
- Figure 7: Global Market Y-o-Y Growth Comparison by Module, 2026-2036
- Figure 8: Global Market Attractiveness Analysis by Module
- Figure 9: Global Market Value Share and BPS Analysis by Care-Setting, 2026 and 2036
- Figure 10: Global Market Y-o-Y Growth Comparison by Care-Setting, 2026-2036
- Figure 11: Global Market Attractiveness Analysis by Care-Setting
- Figure 12: Global Market Value Share and BPS Analysis by End Use, 2026 and 2036
- Figure 13: Global Market Y-o-Y Growth Comparison by End Use, 2026-2036
- Figure 14: Global Market Attractiveness Analysis by End Use
- Figure 15: Global Market Value (USD Million) Share and BPS Analysis by Region, 2026 and 2036
- Figure 16: Global Market Y-o-Y Growth Comparison by Region, 2026-2036
- Figure 17: Global Market Attractiveness Analysis by Region
- Figure 18: North America Market Incremental Dollar Opportunity, 2026-2036
- Figure 19: Latin America Market Incremental Dollar Opportunity, 2026-2036
- Figure 20: Western Europe Market Incremental Dollar Opportunity, 2026-2036
- Figure 21: Eastern Europe Market Incremental Dollar Opportunity, 2026-2036
- Figure 22: East Asia Market Incremental Dollar Opportunity, 2026-2036
- Figure 23: South Asia and Pacific Market Incremental Dollar Opportunity, 2026-2036
- Figure 24: Middle East & Africa Market Incremental Dollar Opportunity, 2026-2036
- Figure 25: North America Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 26: North America Market Value Share and BPS Analysis by Deployment , 2026 and 2036
- Figure 27: North America Market Y-o-Y Growth Comparison by Deployment , 2026-2036
- Figure 28: North America Market Attractiveness Analysis by Deployment
- Figure 29: North America Market Value Share and BPS Analysis by Module, 2026 and 2036
- Figure 30: North America Market Y-o-Y Growth Comparison by Module, 2026-2036
- Figure 31: North America Market Attractiveness Analysis by Module
- Figure 32: North America Market Value Share and BPS Analysis by Care-Setting, 2026 and 2036
- Figure 33: North America Market Y-o-Y Growth Comparison by Care-Setting, 2026-2036
- Figure 34: North America Market Attractiveness Analysis by Care-Setting
- Figure 35: North America Market Value Share and BPS Analysis by End Use, 2026 and 2036
- Figure 36: North America Market Y-o-Y Growth Comparison by End Use, 2026-2036
- Figure 37: North America Market Attractiveness Analysis by End Use
- Figure 38: Latin America Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 39: Latin America Market Value Share and BPS Analysis by Deployment , 2026 and 2036
- Figure 40: Latin America Market Y-o-Y Growth Comparison by Deployment , 2026-2036
- Figure 41: Latin America Market Attractiveness Analysis by Deployment
- Figure 42: Latin America Market Value Share and BPS Analysis by Module, 2026 and 2036
- Figure 43: Latin America Market Y-o-Y Growth Comparison by Module, 2026-2036
- Figure 44: Latin America Market Attractiveness Analysis by Module
- Figure 45: Latin America Market Value Share and BPS Analysis by Care-Setting, 2026 and 2036
- Figure 46: Latin America Market Y-o-Y Growth Comparison by Care-Setting, 2026-2036
- Figure 47: Latin America Market Attractiveness Analysis by Care-Setting
- Figure 48: Latin America Market Value Share and BPS Analysis by End Use, 2026 and 2036
- Figure 49: Latin America Market Y-o-Y Growth Comparison by End Use, 2026-2036
- Figure 50: Latin America Market Attractiveness Analysis by End Use
- Figure 51: Western Europe Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 52: Western Europe Market Value Share and BPS Analysis by Deployment , 2026 and 2036
- Figure 53: Western Europe Market Y-o-Y Growth Comparison by Deployment , 2026-2036
- Figure 54: Western Europe Market Attractiveness Analysis by Deployment
- Figure 55: Western Europe Market Value Share and BPS Analysis by Module, 2026 and 2036
- Figure 56: Western Europe Market Y-o-Y Growth Comparison by Module, 2026-2036
- Figure 57: Western Europe Market Attractiveness Analysis by Module
- Figure 58: Western Europe Market Value Share and BPS Analysis by Care-Setting, 2026 and 2036
- Figure 59: Western Europe Market Y-o-Y Growth Comparison by Care-Setting, 2026-2036
- Figure 60: Western Europe Market Attractiveness Analysis by Care-Setting
- Figure 61: Western Europe Market Value Share and BPS Analysis by End Use, 2026 and 2036
- Figure 62: Western Europe Market Y-o-Y Growth Comparison by End Use, 2026-2036
- Figure 63: Western Europe Market Attractiveness Analysis by End Use
- Figure 64: Eastern Europe Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 65: Eastern Europe Market Value Share and BPS Analysis by Deployment , 2026 and 2036
- Figure 66: Eastern Europe Market Y-o-Y Growth Comparison by Deployment , 2026-2036
- Figure 67: Eastern Europe Market Attractiveness Analysis by Deployment
- Figure 68: Eastern Europe Market Value Share and BPS Analysis by Module, 2026 and 2036
- Figure 69: Eastern Europe Market Y-o-Y Growth Comparison by Module, 2026-2036
- Figure 70: Eastern Europe Market Attractiveness Analysis by Module
- Figure 71: Eastern Europe Market Value Share and BPS Analysis by Care-Setting, 2026 and 2036
- Figure 72: Eastern Europe Market Y-o-Y Growth Comparison by Care-Setting, 2026-2036
- Figure 73: Eastern Europe Market Attractiveness Analysis by Care-Setting
- Figure 74: Eastern Europe Market Value Share and BPS Analysis by End Use, 2026 and 2036
- Figure 75: Eastern Europe Market Y-o-Y Growth Comparison by End Use, 2026-2036
- Figure 76: Eastern Europe Market Attractiveness Analysis by End Use
- Figure 77: East Asia Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 78: East Asia Market Value Share and BPS Analysis by Deployment , 2026 and 2036
- Figure 79: East Asia Market Y-o-Y Growth Comparison by Deployment , 2026-2036
- Figure 80: East Asia Market Attractiveness Analysis by Deployment
- Figure 81: East Asia Market Value Share and BPS Analysis by Module, 2026 and 2036
- Figure 82: East Asia Market Y-o-Y Growth Comparison by Module, 2026-2036
- Figure 83: East Asia Market Attractiveness Analysis by Module
- Figure 84: East Asia Market Value Share and BPS Analysis by Care-Setting, 2026 and 2036
- Figure 85: East Asia Market Y-o-Y Growth Comparison by Care-Setting, 2026-2036
- Figure 86: East Asia Market Attractiveness Analysis by Care-Setting
- Figure 87: East Asia Market Value Share and BPS Analysis by End Use, 2026 and 2036
- Figure 88: East Asia Market Y-o-Y Growth Comparison by End Use, 2026-2036
- Figure 89: East Asia Market Attractiveness Analysis by End Use
- Figure 90: South Asia and Pacific Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 91: South Asia and Pacific Market Value Share and BPS Analysis by Deployment , 2026 and 2036
- Figure 92: South Asia and Pacific Market Y-o-Y Growth Comparison by Deployment , 2026-2036
- Figure 93: South Asia and Pacific Market Attractiveness Analysis by Deployment
- Figure 94: South Asia and Pacific Market Value Share and BPS Analysis by Module, 2026 and 2036
- Figure 95: South Asia and Pacific Market Y-o-Y Growth Comparison by Module, 2026-2036
- Figure 96: South Asia and Pacific Market Attractiveness Analysis by Module
- Figure 97: South Asia and Pacific Market Value Share and BPS Analysis by Care-Setting, 2026 and 2036
- Figure 98: South Asia and Pacific Market Y-o-Y Growth Comparison by Care-Setting, 2026-2036
- Figure 99: South Asia and Pacific Market Attractiveness Analysis by Care-Setting
- Figure 100: South Asia and Pacific Market Value Share and BPS Analysis by End Use, 2026 and 2036
- Figure 101: South Asia and Pacific Market Y-o-Y Growth Comparison by End Use, 2026-2036
- Figure 102: South Asia and Pacific Market Attractiveness Analysis by End Use
- Figure 103: Middle East & Africa Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 104: Middle East & Africa Market Value Share and BPS Analysis by Deployment , 2026 and 2036
- Figure 105: Middle East & Africa Market Y-o-Y Growth Comparison by Deployment , 2026-2036
- Figure 106: Middle East & Africa Market Attractiveness Analysis by Deployment
- Figure 107: Middle East & Africa Market Value Share and BPS Analysis by Module, 2026 and 2036
- Figure 108: Middle East & Africa Market Y-o-Y Growth Comparison by Module, 2026-2036
- Figure 109: Middle East & Africa Market Attractiveness Analysis by Module
- Figure 110: Middle East & Africa Market Value Share and BPS Analysis by Care-Setting, 2026 and 2036
- Figure 111: Middle East & Africa Market Y-o-Y Growth Comparison by Care-Setting, 2026-2036
- Figure 112: Middle East & Africa Market Attractiveness Analysis by Care-Setting
- Figure 113: Middle East & Africa Market Value Share and BPS Analysis by End Use, 2026 and 2036
- Figure 114: Middle East & Africa Market Y-o-Y Growth Comparison by End Use, 2026-2036
- Figure 115: Middle East & Africa Market Attractiveness Analysis by End Use
- Figure 116: Global Market - Tier Structure Analysis
- Figure 117: Global Market - Company Share Analysis

