Hospital Command Center Operations Market
The Hospital Command Center Operations Market is segmented by Solution Layer (Bed Orchestration, Transfer Coordination, Capacity Dashboards, Throughput Automation, Escalation Management), Deployment Model (Cloud, Hybrid, On-Premise), Hospital Type (Academic Centers, Health Systems, Community Hospitals, Specialty Hospitals), Primary Use Case (Bed Placement, Transfer Coordination, ED Flow Control, Discharge Acceleration, Surge Response), Commercial Model (SaaS Subscription, Enterprise License, Managed Service, Hybrid Contract), and Region. Forecast for 2026 to 2036.
Historical Data Covered: 2016 to 2024 | Base Year: 2025 | Estimated Year: 2026 | Forecast Period: 2027 to 2036
Hospital Command Center Operations Market Size, Market Forecast and Outlook By FMI
The hospital command center market crossed a valuation of USD 0.8 billion in 2025. The industry is expected to reach USD 0.9 billion in 2026 at a CAGR of 13.6% during the forecast period. Demand outlook carries the market valuation to USD 3.2 billion by 2036 as health systems pivot from reactive bed management toward a hospital throughput optimization platform that treats inpatient movement as a complex logistics challenge rather than a series of isolated nursing decisions.
Summary of Hospital Command Center Operations Market
- Hospital Command Center Operations Market Definition
- This market encompasses the specialized software and operational services that centralize hospital management. These platforms integrate disparate data streams from nursing, transport, and clinical units to optimize bed availability and patient transfers.
- Demand Drivers in the Market
- Chronic emergency department boarding forces hospital administrators to utilize ED boarding command center tools to prevent ambulance diversions.
- Severe clinical staffing shortages compel nursing directors to adopt prescriptive workflow automation hospital models that align provider availability with real-time patient acuity.
- Shrinking operating margins push Chief Financial Officers to seek a high transfer center ROI hospital wide through accelerated discharge and throughput automation.
- Key Segments Analyzed in the FMI Report
- Patient Flow And Bed Orchestration: 31.0% share in 2026, driven by the immediate ROI of reducing ICU-to-floor transition times.
- Cloud: 49.0% share through 2036, reflecting the need for digital healthcare platforms that can scale across multi-facility networks.
- Large IDNs And Academic Medical Centers: 41.0% share, as an academic medical center command center requires centralized logic to manage high-acuity patient volumes.
- India: A 14.8% CAGR, fueled by rapid private hospital expansion and a leapfrog transition directly into digital health infrastructure.
- Analyst Opinion at FMI
- Sabyasachi Ghosh, Principal Consultant for Healthcare at Future Market Insights, opines, “Our latest evaluation indicates that hospital command centers are evolving into data orchestration hubs. Integrating inputs from electronic health records, staffing systems, and diagnostic workflows enables predictive analytics for demand forecasting and resource allocation. Healthcare providers that leverage AI-driven insights within command centers will significantly enhance operational resilience.”
- Strategic Implications / Executive Takeaways
- Chief Operating Officers must empower command center staff with the formal authority to override department-level bed "hoarding" to realize hospital command center benefits.
- A hospital CIO operations command center should prioritize artificial intelligence in healthcare that integrates natively with existing EHRs to avoid creating another data silo.
- R&D Directors should utilize predictive capacity planning hospital tools to smooth the morning surgical intake spike.
- Methodology
- The research identifies the structural reality of hospital logistics by mapping the gap between theoretical bed capacity and operational bed availability. FMI validates these trends through primary interviews with the managers who actually staff these hubs.
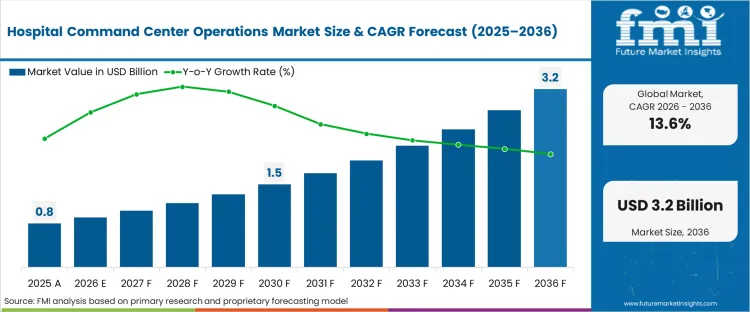
Health system executives currently face a decision landscape where the stakes of operational delay have moved from administrative friction to clinical risk. Chief Operating Officers are no longer evaluating hospital capacity management software market dynamics as a simple dashboarding exercise; they are calculating the daily financial bleed of "boarding" patients in the emergency department because of discharge bottlenecks. A non-obvious observation in this healthcare command center market is that the most successful hubs operate as "air traffic control" for human capital, not just physical beds. When a transfer center coordinator lacks real-time visibility into specialized nurse staffing levels, the most sophisticated patient placement software hospitals fail because a physical bed without a qualified clinician is functionally non-existent.
Surgical directors and emergency department heads act as the primary triggers for the critical structural gate: the transition from historical reporting to predictive analytics hospital command center capabilities. Growth becomes self-reinforcing once a patient flow command center market participant demonstrates that it can move a patient from a high-acuity ICU bed to a step-down unit two hours earlier through automated discharge triggers. This inflection removes the reliance on manual phone calls, creating a virtuous cycle where clinicians trust the data enough to follow the center's placement directives without negotiation.
India leads the hospital digital operations market forecast with a 14.8% CAGR, driven by the massive scale-up of private healthcare infrastructure, while Saudi Arabia tracks at 14.1% as the Kingdom’s Vision 2030 prioritizes digital transformation. United Kingdom follows at 13.1% compound growth, with NHS trusts seeking to mitigate occupancy crises through a hospital digital coordination center. United States is set for 12.8% growth, focusing on interfacility transfer coordination software, whereas Germany is likely to reach 12.4% as hospitals consolidate into regional networks. Canada and Australia are on track to record 12.2% and 13.3% respectively, reflecting a structural shift toward regionalized patient flow models.
Hospital Command Center Operations Market Definition
A smart hospital command center acts as a centralized operational hub that utilizes integrated data feeds to manage patient throughput, resource allocation, and clinical logistics across a healthcare system. These centers serve as the "brain" of the hospital, synchronizing bed management, transfer coordination, and predictive staffing. Functional boundaries are defined by the ability to provide real time situational awareness hospital wide, ingesting telemetry from EHRs to provide actionable visibility into bottlenecks before they result in ambulance diversions.
Hospital Command Center Operations Market Inclusions
Scope includes command center software for hospitals designed for healthcare analytics that power real-time dashboards and predictive modeling for patient placement. Services included encompass the managed service agreements and command center staffing models where vendors provide on-site or remote personnel to run the coordination hub. Managed service contracts and recurring subscriptions for healthcare business intelligence specifically tailored for acute care orchestration also fall within this boundary.
Hospital Command Center Operations Market Exclusions
General Electronic Health Record (EHR) systems are excluded unless they include a dedicated, standalone command center module with real-time predictive capabilities. Basic clinical decision support tools and general hospital workforce management software that lack a centralized "hub" interface for system-wide orchestration are outside the scope. Laboratory Information Management Systems (LIMS) and generic financial ERP systems are strictly excluded as they do not facilitate real-time patient flow.
Hospital Command Center Operations Market Research Methodology
- Primary Research: Interviews with Chief Operating Officers and Transfer Center Directors at Tier-1 health systems using a hospital access center platform.
- Desk Research: Analysis of clinical trial registries, hospital command center case study documentation, and AHRQ summit reports on ED boarding.
- Market-Sizing and Forecasting: Analysis anchored by the ratio of "command-center-enabled" beds to total acute care beds in mature versus emerging healthcare systems.
- Data Validation and Update Cycle: Cross-verification using vendor contract announcements and hospital capital expenditure filings to monitor adoption velocity.
Segmental Analysis
Hospital Command Center Operations Market Analysis by Solution Layer
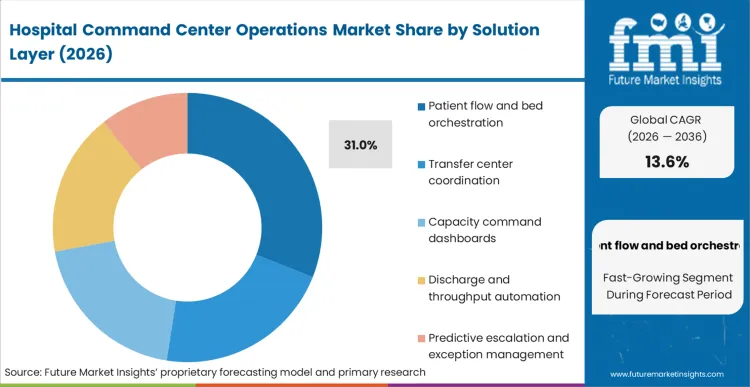
Operational logic in this segment is dictated by the immediate pressure to resolve bed-assignment bottlenecks. Patient flow and bed orchestration platforms dominate the landscape, holding 31.0% share because they solve the most visible pain point: the empty-but-uncleaned bed. FMI's view is that the value of these solutions lies in their ability to automate the "dirty-to-ready" workflow. Procurement directors at large academic centers are shifting away from manual bed-tracking to an AI hospital operations platform that predicts census surges before they occur. A practitioner reality is that while a real time hospital operations dashboard provides high-level visibility, it often lacks the "last mile" connectivity to nursing assignments. Large systems that delay the implementation of hospital discharge command center software face a cumulative loss of bed-days that effectively neutralizes any gains from expanding physical bed capacity.
- Automated-Discharge-Triggering: Integrated logic identifies patients meeting clinical discharge criteria and automatically alerts transport and pharmacy teams to prepare for departure. Operations leads utilize these triggers to ensure a command center reduces hospital length of stay metrics by eliminating noon discharge delays.
- Interfacility-Transfer-Logic: Centralized coordination modules allow transfer center directors to evaluate incoming patient acuity against real-time sub-specialty physician availability. This mechanism, central to the hospital transfer center software market, prevents the common failure mode of accepting a patient at a facility that lacks the specific surgical specialty required.
- Predictive-Census-Modeling: Software algorithms ingest historical admission patterns and current clinic schedules to project bed needs 48 hours in advance. Operations managers use hospital census dashboard software to adjust elective surgery schedules or surge staffing, preventing the operational friction associated with last-minute procedure cancellations.
Hospital Command Center Operations Market Analysis by Deployment Model
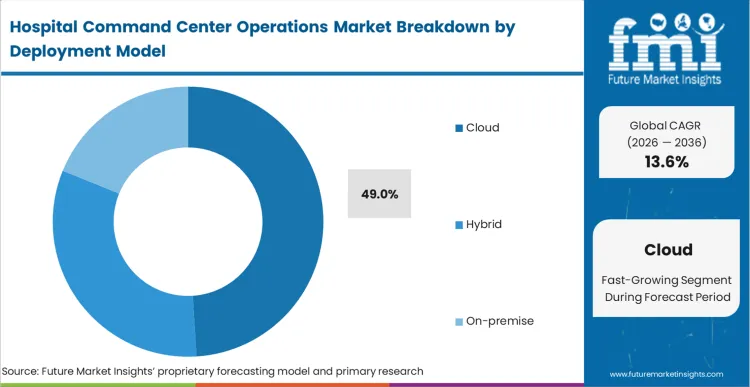
Cloud architecture has moved from a technical preference to a structural requirement for modern health systems. A cloud hospital command center holds 49.0% share because it enables the seamless aggregation of data across geographically dispersed hospitals within a single network. Based on FMI's assessment, the scalability of AI-powered-care-coordination is fundamentally tied to cloud-native environments that can process high-velocity EHR data feeds without the latency of on-premise servers. Chief Information Officers favor these models for their ability to push algorithm updates across the entire enterprise simultaneously. What the share figure does not tell you is that a hybrid hospital operations platform is often maintained as a "failsafe" for critical patient placement data during internet outages. Organizations that remain tethered to on premise hospital command center software find themselves increasingly isolated from the third-party analytical ecosystems that are now developed exclusively for the cloud.
- Multi-Facility-Orchestration: Centralized cloud hubs allow a single team of coordinators to manage the patient flow for ten or more hospitals from a remote location. Regional COOs utilize this centralized visibility to "load balance" patients across the system, ensuring that one facility isn't on diversion while another has open capacity.
- Real-Time-Telemetry-Streaming: Cloud-native platforms ingest live feeds from cardiac monitors and ventilators to identify patients who are ready for de-escalation from the ICU. Clinical leads use this data within a bed management command center market context to prioritize step-down transfers, directly improving high-acuity bed turnover and surgical throughput.
- Rapid-Algorithm-Deployment: Technical teams push updated predictive models for patient deterioration or discharge readiness without requiring local server downtime at individual hospital sites. IT directors at mid-sized systems treat a SaaS patient flow platform hospital as a significant cost-reduction mechanism, as it eliminates the need for facility-specific maintenance teams.
Hospital Command Center Operations Market Analysis by Hospital Type

Structural complexity at academic medical centers and large IDNs makes them the primary adopters of command center logic. These institutions act as the "hub" of a regional spoke-and-wheel model, necessitating sophisticated clinical communication and collaboration to manage the constant influx of high-acuity transfers. FMI observes that for a surgical director at a major teaching hospital, a capacity command center hospitals model is less about bed tracking and more about "OR-to-ICU" throughput synchronization. A practitioner will note that while a community hospital command center is adopting these tools, they often use simplified versions focused purely on staffing. The non-obvious observation is that specialty hospitals actually require the highest level of predictive modeling because their patient populations cannot be easily "flexed" to other units. Currently capturing 41.0% share, health systems that fail to integrate their community hospitals into a regional health system operations center often experience "clogging" at their main academic campus.
- High-Acuity-Transfer-Triage: Specialized coordinators at academic centers evaluate incoming trauma or stroke transfers to ensure they are routed to the specific team with the highest current capacity. This mechanism reduces the "door-to-intervention" time, a critical clinical outcome that also improves the hospital's reputation and reimbursement levels.
- Networked-Capacity-Leveling: Regional health systems use the command center to identify "empty" beds in suburban community hospitals where patients can be transferred for recovery. Patient flow directors utilize this strategy to keep high-cost ICU beds at the main campus open for incoming emergency cases, maximizing the system's total revenue potential.
- Specialty-Staffing-Synchronization: Command centers in cardiac or orthopedic specialty hospitals align the surgical schedule with post-operative bed availability and specialized physical therapy staffing. Operations leads use this orchestration to ensure that a patient’s recovery is never delayed by the unavailability of a specific rehabilitation resource.
Hospital Command Center Operations Market Analysis By Primary Use Case
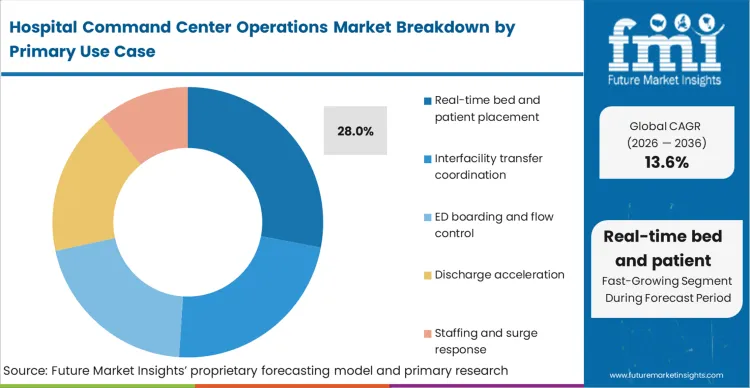
Real-time bed and patient placement remains the foundational use case, as hospitals struggle with post-pandemic occupancy stress. According to FMI's estimates, the focus is shifting toward population health management within the hospital walls, treating the inpatient population as a managed cohort. Interfacility transfer coordination is a critical sub-segment, as health systems realize that "leakage" is a major revenue drain, accounting for 28.0% share. A practitioner knows that discharge acceleration is difficult to implement because it requires changing the behavior of hundreds of physicians. The aspect that the data does not show is that hospital command center staffing visibility is increasingly used to manage "traveler" nurse costs by predicting precisely where supplemental staff will be needed 12 hours before the shift starts. Facilities that do not master the discharge acceleration use case will continue to experience "afternoon gridlock," regardless of how well they manage their initial patient placement.
- Discharge-Milestone-Tracking: Command centers monitor the completion of critical discharge tasks, such as final lab results or durable medical equipment delivery, in real-time. Discharge planners use this visibility to intervene when a specific task is stalling a patient’s departure, preventing a bed from being "locked" for an extra four to six hours.
- Surge-Capacity-Activation: Algorithms detect when the emergency department volume exceeds a specific threshold and automatically trigger surge protocols. A hospital command center for surge management allows nursing directors at urban trauma centers to pull in backup staff before the waiting room becomes unmanageable.
- Transfer-Leakage-Prevention: Real-time visibility into the entire system’s bed capacity allows transfer center agents to accept incoming patients within minutes rather than hours. Commercial leads treat this speed as a competitive advantage that ensures high-margin specialty cases remain within their network.
Hospital Command Center Operations Market Analysis By Commercial Model
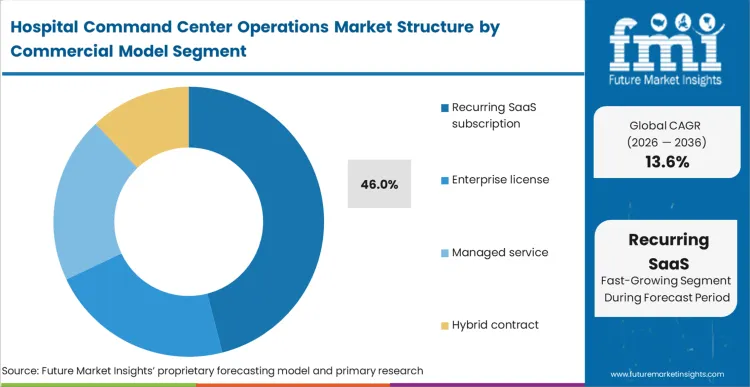
Recurring SaaS subscriptions have become the dominant commercial model, capturing 46.0% share by lowering the initial capital barrier. FMI's view indicates that the shift away from enterprise licenses is driven by the need for continuous software evolution in remote healthcare and coordination. Managed service models are gaining traction among systems that have the budget for technology but lack the internal expertise to staff a 24/7 center. A practitioner reality is that the "hybrid contract" is often the most successful because it aligns the vendor’s incentives with the hospital’s throughput goals. What procurement directors often miss is that enterprise licenses for legacy software often carry "hidden" maintenance costs that eventually exceed the cost of a modern SaaS subscription. Systems that stick with legacy enterprise licenses often find themselves five years behind in algorithm development, as vendors prioritize their SaaS customers for the latest AI and machine learning rollouts.
- Performance-Based-Incentives: Newer commercial models tie vendor payments to a specific hospital command center ROI milestone, such as a 5.0% reduction in emergency department wait times. COOs favor this alignment because it ensures the vendor remains an active partner in the center’s operational success.
- Scalable-License-Tiers: SaaS models allow hospitals to "turn on" additional modules, such as remote ICU monitoring, as their operational maturity grows. IT directors utilize this flexibility to manage capital budgets while still maintaining a roadmap for future digital transformation.
- Outsourced-Staffing-Resiliency: Managed service agreements provide a "co-sourcing" model where the vendor provides experienced flow coordinators to supplement the hospital’s internal team. This mechanism ensures that the command center remains operational during local labor shortages or peak flu seasons when internal staff are often redeployed to the bedside.
Hospital Command Center Operations Market Drivers, Restraints, and Opportunities
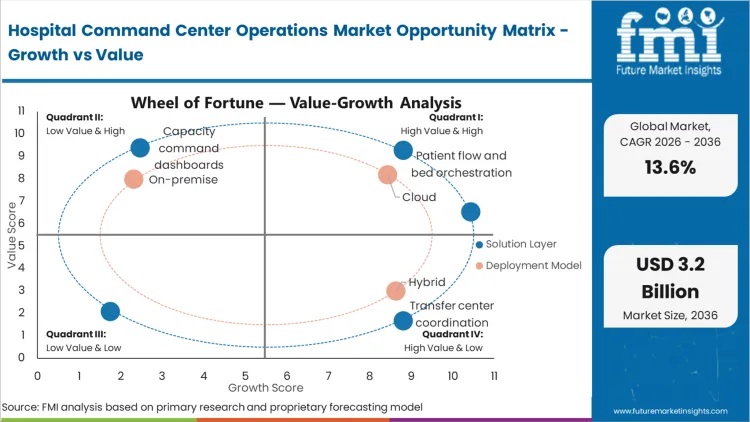
Chronic emergency department boarding creates a commercial pressure where health systems lose thousands of dollars per hour in diverted ambulance revenue and lost surgical intake. This forcing condition is pushing Chief Operating Officers to adopt patient engagement platforms that can coordinate with the command center to streamline the intake and discharge process. The stakes of delay are high; a hospital that cannot move patients through the "middle" of their stay, from the ICU to the med-surg floor, is functionally paralyzed, leading to a permanent loss of market share as patients and surgeons migrate to more efficient competitors.
Internal organizational friction remains the primary structural obstacle, specifically the "autonomy gap" between centralized coordinators and unit-based charge nurses. Even when a command center identifies an available bed, the local nursing unit may "hide" the bed by delaying the status update in the EHR to prevent a new admission during a shift change. This friction persists because hospital incentive structures usually reward department-level metrics rather than system-wide throughput. While patient portals and automated updates provide partial visibility, they cannot solve the underlying cultural resistance to centralized control without a fundamental change in hospital governance.
- Regional-Care-Orchestration: Expanding command center logic beyond a single facility to manage the entire home healthcare software and post-acute transition cycle creates a massive opportunity for systems to reduce readmission penalties.
- Predictive-Staffing-Integration: Integrating healthcare contact center solution data with real-time census projections allows hospitals to proactively manage patient inquiries and scheduling before they turn into operational bottlenecks.
- AI-Augmented-Triage: Developing machine learning models that can predict which patients are likely to deteriorate in the next six hours allows the command center to proactively move those patients to higher-acuity beds before a "Code Blue" occurs.
Regional Analysis
.webp)
The hospital command center operations market is currently defined by a structural shift from siloed department management to integrated, system-wide orchestration across 40 plus countries. This geographic progression is shaped by local digital maturity levels and the unique pressures inherent in different public and private healthcare infrastructures.
| Country | CAGR (2026 to 2036) |
|---|---|
| India | 14.8% |
| Saudi Arabia | 14.1% |
| Australia | 13.3% |
| United Kingdom | 13.1% |
| United States | 12.8% |
| Germany | 12.4% |
| Canada | 12.2% |
Source: Future Market Insights (FMI) analysis, based on proprietary forecasting model and primary research
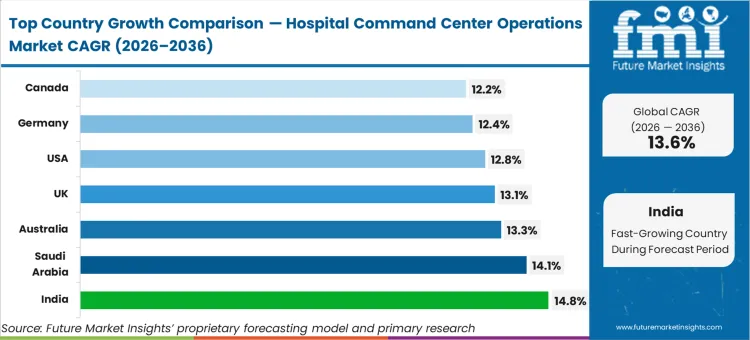
North America Hospital Command Center Operations Market Analysis
North American integrated networks are moving beyond basic value-based care incentives toward a model of absolute operational necessity by utilizing a "single pane of glass" to oversee thousands of beds. The adoption curve across this region is driven by a need to unify independent data streams into a single mission control to mitigate clinical risks associated with emergency department boarding. Within this landscape, the primary technical challenge involves harmonizing legacy EHR systems with a modern real time e-healthcare system to achieve transparent, system-wide visibility.
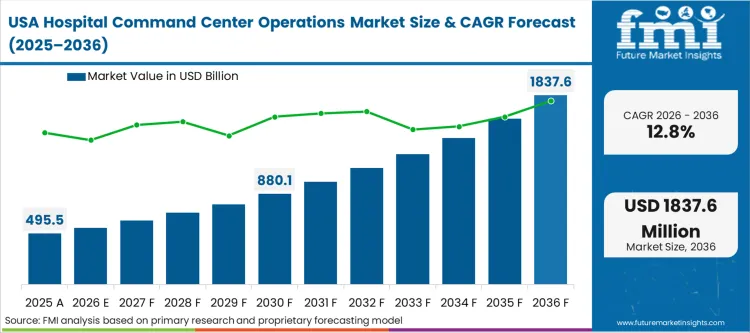
- United States: By establishing off-site coordination hubs that oversee placement for twenty or more facilities, health system leaders are pursuing a strategy expected to result in a CAGR of 12.8% through 2036. This trajectory provides a major commercial opening for technology providers who can successfully normalize disparate data into a high-functioning hospital orchestration platform.
- Canada: Provincial health authorities are deploying digital tools to manage extreme occupancy stress and streamline the movement of Alternate Level of Care (ALC) patients. A CAGR of 12.2% is the investment pace used by these authorities to modernize infrastructure, representing a practitioner reality where data-driven insights are used to advocate for critical post-acute resources.
FMI reports, these findings highlight how North American providers are successfully deploying predictive logic to close the gap between theoretical bed capacity and actual operational availability.
Europe Hospital Command Center Operations Market Analysis
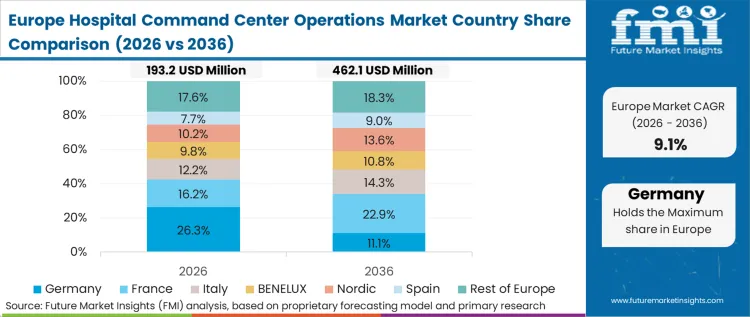
European public health sectors are turning to command center logic as a strategic response to rising labor costs and the recurring threat of winter-system collapse. In the United Kingdom, Integrated Care Boards (ICBs) now require real-time regional occupancy data to prevent total service breakdowns during peak demand periods. Meanwhile, German facilities are consolidating into regional networks and increasingly incorporating hospital service robots into their hubs to automate logistics and alleviate the physical workload on nursing staff.
- United Kingdom: A CAGR value of 13.1% is projected as NHS Trusts implement a digital coordination center hospital implementation to manage occupancy levels that frequently exceed 95%. This positioning allows the public sector to maximize existing bed utility before relying on expensive private-sector overflow contracts.
- Germany: Capital provided by the federal "Hospital Future Act" (KHZG) is fueling an expansion in coordination tools to ensure facilities meet new national standards for data transparency. By the end of the forecast period, a 12.4% growth will have effectively transitioned the country from localized management to a unified operational model.
FMI analyses, market dynamics in Europe reflect a pivot toward regionalized coordination as a vital survival mechanism against increasing patient volumes and persistent resource constraints.
Middle-East Hospital Command Center Operations Market Analysis
National mandates, such as Saudi Arabia’s Vision 2030, are accelerating digital health transformation by prioritizing the development of "smart" healthcare infrastructure. Regional decision-makers are investing in centralized hubs to manage high-acuity patient flow and optimize resource allocation within rapidly expanding medical cities. These initiatives are centered on building a robust hospital throughput optimization platform capable of managing the patient journey from initial triage through post-acute follow-up.
- Saudi Arabia: The Kingdom is enhancing its operational efficiency at a CAGR of 14.1%, utilizing health clusters to standardize clinical quality across its various regions. This growth pace supports the creation of a virtual health network, providing a structural trajectory where high-acuity care is managed via a centralized, predictive lens.
FMI's report includes additional countries not in bullets. The Middle Eastern landscape is defined by a "leapfrog" transition where new facilities are designed as fully orchestrated digital nodes from the ground up.
Asia-Pacific Hospital Command Center Operations Market Analysis
The Asia-Pacific region is seeing a surge in adoption as private hospital chains in India and public health departments in Australia seek to manage massive patient volumes through centralized oversight. Private sector growth is creating a structural reliance on automated logic to manage 1,000-plus bed facilities where manual flow is no longer sustainable. In Australia, the market is moving toward "Virtual Hospitals," applying a patient flow command center market approach to oversee high-acuity care delivered directly in the home environment.
- India: Projected to expand at a CAGR of 14.8%, corporate hospital chains are using command centers to standardize the patient experience across emerging Tier-2 cities. This growth enables private providers to scale operations while maintaining high occupancy rates, offering a commercial opportunity for vendors supporting rapid multi-site rollouts.
- Australia: State health departments are leading a transition toward regional coordination hubs designed to manage the patient journey across a digital network. At a CAGR of 13.3%, this shift reflects a practitioner reality where the acute facility is viewed as one high-acuity node within a much larger system of care.
Per FMI’s assessments, Asia-Pacific dynamics are characterized by the urgent need to manage vast patient cohorts through aggressive digital orchestration and centralized clinical oversight.
Competitive Aligners for Market Players
The hospital operations command center market is shaped by a clear split between EHR-linked platforms and specialist command center providers. Oracle Health and GE HealthCare benefit from their broad installed base and can position command center tools as part of a wider enterprise relationship. Specialized vendors still hold an important place in the market because many health systems see stronger depth in bed management, patient flow, and operating room optimization from those platforms. In comparisons such as TeleTracking and Qventus, buyers tend to focus heavily on whether frontline staff can rely on the recommendations. If bed status, discharge timing, or transport readiness is not accurate, adoption can fall quickly. That makes trust in the data one of the most important competitive factors.
Established providers also benefit from years of integration work across hospital operations. Their advantage comes from knowing how clinical workflows behave in practice, especially in areas such as environmental services, transport coordination, and room turnover. A newer entrant may bring a capable interface or a strong analytics layer, though it is much harder to replicate the operational logic that has been refined over time. When health systems compare alternatives to GE HealthCare command center offerings, they usually look for a platform that can work across legacy medical devices, connect with multiple hospital systems, and support everyday orchestration without adding friction.
At the same time, large health systems do not want to be boxed into one vendor’s environment. Many are asking for open API structures so they can use one platform for emergency department visibility and another for operating room scheduling or inpatient flow. That is pushing hospital command center software providers toward a more modular approach, where interoperability matters much more than before. Over time, the market is likely to separate more clearly between broad enterprise-level hubs and focused operational tools built to solve specific departmental problems. That tension will shape how hospitals spend on digital operations platforms in the years ahead.
Key Players in Hospital Command Center Operations Market
- TeleTracking
- GE HealthCare
- LeanTaaS
- Qventus
- Oracle Health
- Palantir
- Systematic (Columna Flow)
- Central Logic (Envisage)
- Care.ai
- Vizzia Technologies
Scope of the Report
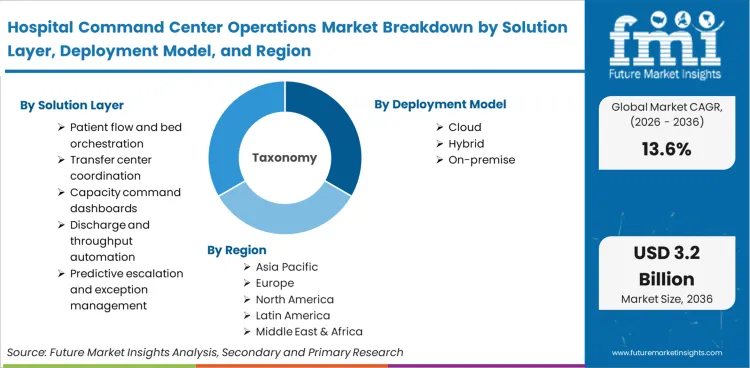
| Metric | Value |
|---|---|
| Quantitative Units | USD 0.9 billion in 2026 to USD 3.2 billion by 2036, at a CAGR of 13.6% |
| Market Definition | Centralized operational hubs that utilize real-time data feeds and predictive algorithms to manage patient throughput, resource allocation, and clinical logistics across healthcare systems. |
| Segmentation | Solution layer, Deployment model, Hospital type, Primary use case, Commercial model, and Region. |
| Regions Covered | North America, Europe, Asia-Pacific, Middle-East, and Africa. |
| Countries Covered | United States, Canada, United Kingdom, Germany, India, Saudi Arabia, Australia, and 40 others. |
| Key Companies Profiled | TeleTracking, GE HealthCare, LeanTaaS, Qventus, Oracle Health, Palantir, Systematic, and others. |
| Forecast Period | 2026 to 2036 |
| Approach | Multi-modal forecasting model cross-referencing bed-to-hub ratios with clinical staffing trends and regional healthcare IT investment cycles. |
Source: Future Market Insights (FMI) analysis, based on proprietary forecasting model and primary research
Key Segments:
Solution Layer
- Patient flow and bed orchestration
- Transfer center coordination
- Capacity command dashboards
- Discharge and throughput automation
- Predictive escalation and exception management
Deployment Model
- Cloud
- Hybrid
- On-premise
Hospital Type
- Large IDNs and academic medical centers
- Regional health systems
- Community hospitals
- Specialty hospitals
Primary Use Case
- Real-time bed and patient placement
- Interfacility transfer coordination
- ED boarding and flow control
- Discharge acceleration
- Staffing and surge response
Commercial Model
- Recurring SaaS subscription
- Enterprise license
- Managed service
- Hybrid contract
Regions:
- Asia Pacific
- India
- China
- Japan
- South Korea
- Indonesia
- Australia & New Zealand
- ASEAN
- Rest of Asia Pacific
- Europe
- Germany
- Italy
- France
- United Kingdom
- Spain
- Benelux
- Nordics
- Central & Eastern Europe
- Rest of Europe
- North America
- United States
- Canada
- Mexico
- Latin America
- Brazil
- Argentina
- Chile
- Rest of Latin America
- Middle East & Africa
- Kingdom of Saudi Arabia
- United Arab Emirates
- South Africa
- Turkey
- Rest of Middle East & Africa
Bibliography
- Agency for Healthcare Research and Quality. (2025, February). AHRQ summit to address emergency department boarding. USA Department of Health and Human Services.
- Butler-Henderson, K., McLoone, K., Macdonald, B., Arabi, S., & Nicol, K. (2025, August). Final report: Health operation centres in healthcare. RMIT University.
- Johnson, O. A., McCrorie, C., McInerney, C., et al. (2024, July). Implementing an artificial intelligence command centre in the NHS: A mixed-methods study. Health and Social Care Delivery Research.
- NHS England. (2024, September). Improvement guide: Acute and emergency care acute patient flow.
- Pardo, J. L., Garifullin, M. V., Farquhar, N. M., et al. (2025, March). Designing a hospital command center with proven ROI: The University of Michigan M2C2 model. NEJM Catalyst.
This bibliography is provided for reader reference. The full FMI report contains the complete reference list with primary source documentation.
This Report Addresses
- Operational consequences of emergency department boarding for urban trauma centers and regional health systems.
- Structural differences between EHR-native command center modules and specialized top hospital command center companies.
- Impact of cloud-based deployment on the scalability of predictive census modeling across integrated delivery networks.
- Strategic implications of the "autonomy gap" between centralized flow coordinators and local nursing unit leadership.
- Role of interfacility transfer coordination in preventing revenue leakage to competing regional healthcare providers.
- Adoption velocity of discharge acceleration tools among academic medical centers versus community specialty hospitals.
- Commercial shift from enterprise software licenses to recurring SaaS and performance-based hospital command center ROI models.
- Hospital command center trends 2026 including the growth trajectory in emerging APAC hubs like India and Australia.
Frequently Asked Questions
What is the projected value of the hospital command center operations market by 2036?
The revenue is anticipated to reach USD 3.2 billion by 2036, reflecting a structural shift toward predictive clinical logistics.
Why does Patient flow and bed orchestration lead the solution segment?
This segment holds a 31.0% share because it directly addresses the most visible operational failure: bed-turnover delay.
What structural mechanism makes the Cloud deployment model dominant?
Cloud architecture allows health systems to aggregate data across multiple facilities without the massive infrastructure costs of local servers.
How do large IDNs and academic centers use command centers differently from smaller hospitals?
Large systems use these hubs as a triage engine to coordinate complex, high-acuity transfers from a wide geographic region.
What are the primary hospital command center KPIs used to measure success?
Success is typically measured by metrics including length of stay (LOS), emergency department boarding time, and bed-turnover speed.
Why is India the fastest-growing country in this sector at 14.8% CAGR?
Rapid private hospital expansion is creating a leapfrog effect where new multi-site systems are built with digital command centers as a foundational requirement.
What is the "non-obvious" insight regarding command center ROI?
The real ROI stems from reducing "boarding hours" in the emergency department, as every hour spent waiting represents a cumulative loss of throughput capacity.
How does predictive staffing integrate into the command center workflow?
Advanced algorithms predict census surges twelve hours in advance, allowing the center to proactively call in supplemental staff and reduce traveler nurse costs.
What distinguishes specialized vendors from EHR-native command modules?
Specialized vendors provide deep, workflow-specific algorithms that account for minute operational details like elevator wait times which generic modules often lack.
What is the significance of the 13.6% CAGR for this market?
This growth rate reflects the structural transition from reactive to proactive hospital management in a low-margin, high-occupancy environment.
How does interfacility transfer coordination prevent "revenue leakage"?
By accepting transfers in minutes rather than hours, a health system ensures high-margin specialty cases remain within their network rather than being diverted to rivals.
What is the role of AI in discharge acceleration?
AI identifies patients meeting clinical discharge criteria to prompt physicians for earlier orders, freeing up beds for afternoon surgical intakes.
Why are managed service models gaining traction among community hospitals?
These hospitals utilize managed services to obtain 24/7 coordination expertise without increasing the local recruitment burden for specialized staff.
How do command centers manage "surge" conditions?
Centers coordinate the rapid discharge of ready patients to decompress the emergency department when occupancy hits specific thresholds.
What is the impact of recurring SaaS models on hospital capital budgets?
SaaS models democratize access to throughput technology by shifting costs from capital expenditure to more manageable operational expenditure.
How does regional care orchestration reduce readmission penalties?
Monitoring post-acute transitions allows centers to identify patients missing follow-up care and intervene before they return to the emergency department.
Why is the "autonomy gap" considered a structural friction rather than a temporary hurdle?
This friction is built into historical governance where department heads maintain nearly total control over their local unit resources.
What role does real-time telemetry play in ICU throughput?
Live telemetry feeds allow coordinators to identify stabilized ICU patients who can be safely moved to step-down care, freeing high-acuity beds.
What is the "Timing Disconnect" mentioned by FMI analysts?
A disconnect exists when administrators expect immediate bed relief while clinical rounding patterns and discharge behaviors remain unchanged.
How do corporate hospital chains in India use command centers to standardize care?
Centralized hubs allow specialists to oversee clinical protocols and flow efficiency across dozens of satellite hospitals in different cities.
What is the end-state for hospital operations by 2036?
Hospitals will operate as fully orchestrated nodes in digital networks with nearly all patient movements dictated by predictive algorithms.
Table of Content
- Executive Summary
- Global Market Outlook
- Demand to side Trends
- Supply to side Trends
- Technology Roadmap Analysis
- Analysis and Recommendations
- Market Overview
- Market Coverage / Taxonomy
- Market Definition / Scope / Limitations
- Research Methodology
- Chapter Orientation
- Analytical Lens and Working Hypotheses
- Market Structure, Signals, and Trend Drivers
- Benchmarking and Cross-market Comparability
- Market Sizing, Forecasting, and Opportunity Mapping
- Research Design and Evidence Framework
- Desk Research Programme (Secondary Evidence)
- Company Annual and Sustainability Reports
- Peer-reviewed Journals and Academic Literature
- Corporate Websites, Product Literature, and Technical Notes
- Earnings Decks and Investor Briefings
- Statutory Filings and Regulatory Disclosures
- Technical White Papers and Standards Notes
- Trade Journals, Industry Magazines, and Analyst Briefs
- Conference Proceedings, Webinars, and Seminar Materials
- Government Statistics Portals and Public Data Releases
- Press Releases and Reputable Media Coverage
- Specialist Newsletters and Curated Briefings
- Sector Databases and Reference Repositories
- FMI Internal Proprietary Databases and Historical Market Datasets
- Subscription Datasets and Paid Sources
- Social Channels, Communities, and Digital Listening Inputs
- Additional Desk Sources
- Expert Input and Fieldwork (Primary Evidence)
- Primary Modes
- Qualitative Interviews and Expert Elicitation
- Quantitative Surveys and Structured Data Capture
- Blended Approach
- Why Primary Evidence is Used
- Field Techniques
- Interviews
- Surveys
- Focus Groups
- Observational and In-context Research
- Social and Community Interactions
- Stakeholder Universe Engaged
- C-suite Leaders
- Board Members
- Presidents and Vice Presidents
- R&D and Innovation Heads
- Technical Specialists
- Domain Subject-matter Experts
- Scientists
- Physicians and Other Healthcare Professionals
- Governance, Ethics, and Data Stewardship
- Research Ethics
- Data Integrity and Handling
- Primary Modes
- Tooling, Models, and Reference Databases
- Desk Research Programme (Secondary Evidence)
- Data Engineering and Model Build
- Data Acquisition and Ingestion
- Cleaning, Normalisation, and Verification
- Synthesis, Triangulation, and Analysis
- Quality Assurance and Audit Trail
- Market Background
- Market Dynamics
- Drivers
- Restraints
- Opportunity
- Trends
- Scenario Forecast
- Demand in Optimistic Scenario
- Demand in Likely Scenario
- Demand in Conservative Scenario
- Opportunity Map Analysis
- Product Life Cycle Analysis
- Supply Chain Analysis
- Investment Feasibility Matrix
- Value Chain Analysis
- PESTLE and Porter’s Analysis
- Regulatory Landscape
- Regional Parent Market Outlook
- Production and Consumption Statistics
- Import and Export Statistics
- Market Dynamics
- Global Market Analysis 2021 to 2025 and Forecast, 2026 to 2036
- Historical Market Size Value (USD Million) Analysis, 2021 to 2025
- Current and Future Market Size Value (USD Million) Projections, 2026 to 2036
- Y to o to Y Growth Trend Analysis
- Absolute $ Opportunity Analysis
- Global Market Pricing Analysis 2021 to 2025 and Forecast 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Solution Layer
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Solution Layer , 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Solution Layer , 2026 to 2036
- Patient flow and bed orchestration
- Transfer center coordination
- Capacity command dashboards
- Discharge and throughput automation
- Predictive escalation and exception management
- Patient flow and bed orchestration
- Y to o to Y Growth Trend Analysis By Solution Layer , 2021 to 2025
- Absolute $ Opportunity Analysis By Solution Layer , 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Deployment Model
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Deployment Model, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Deployment Model, 2026 to 2036
- Cloud
- Hybrid
- On-premise
- Cloud
- Y to o to Y Growth Trend Analysis By Deployment Model, 2021 to 2025
- Absolute $ Opportunity Analysis By Deployment Model, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Hospital Type
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Hospital Type, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Hospital Type, 2026 to 2036
- Large IDNs and academic medical centers
- Regional health systems
- Community hospitals
- Specialty hospitals
- Large IDNs and academic medical centers
- Y to o to Y Growth Trend Analysis By Hospital Type, 2021 to 2025
- Absolute $ Opportunity Analysis By Hospital Type, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Primary Use Case
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Primary Use Case, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Primary Use Case, 2026 to 2036
- Real-time bed and patient placement
- Interfacility transfer coordination
- ED boarding and flow control
- Discharge acceleration
- Staffing and surge response
- Real-time bed and patient placement
- Y to o to Y Growth Trend Analysis By Primary Use Case, 2021 to 2025
- Absolute $ Opportunity Analysis By Primary Use Case, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Commercial Model
- Introduction / Key Findings
- Historical Market Size Value (USD Million) Analysis By Commercial Model, 2021 to 2025
- Current and Future Market Size Value (USD Million) Analysis and Forecast By Commercial Model, 2026 to 2036
- Recurring SaaS subscription
- Enterprise license
- Managed service
- Hybrid contract
- Recurring SaaS subscription
- Y to o to Y Growth Trend Analysis By Commercial Model, 2021 to 2025
- Absolute $ Opportunity Analysis By Commercial Model, 2026 to 2036
- Global Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Region
- Introduction
- Historical Market Size Value (USD Million) Analysis By Region, 2021 to 2025
- Current Market Size Value (USD Million) Analysis and Forecast By Region, 2026 to 2036
- North America
- Latin America
- Western Europe
- Eastern Europe
- East Asia
- South Asia and Pacific
- Middle East & Africa
- Market Attractiveness Analysis By Region
- North America Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- USA
- Canada
- Mexico
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- By Country
- Market Attractiveness Analysis
- By Country
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Key Takeaways
- Latin America Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Brazil
- Chile
- Rest of Latin America
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- By Country
- Market Attractiveness Analysis
- By Country
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Key Takeaways
- Western Europe Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Germany
- UK
- Italy
- Spain
- France
- Nordic
- BENELUX
- Rest of Western Europe
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- By Country
- Market Attractiveness Analysis
- By Country
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Key Takeaways
- Eastern Europe Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Russia
- Poland
- Hungary
- Balkan & Baltic
- Rest of Eastern Europe
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- By Country
- Market Attractiveness Analysis
- By Country
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Key Takeaways
- East Asia Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- China
- Japan
- South Korea
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- By Country
- Market Attractiveness Analysis
- By Country
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Key Takeaways
- South Asia and Pacific Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- India
- ASEAN
- Australia & New Zealand
- Rest of South Asia and Pacific
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- By Country
- Market Attractiveness Analysis
- By Country
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Key Takeaways
- Middle East & Africa Market Analysis 2021 to 2025 and Forecast 2026 to 2036, By Country
- Historical Market Size Value (USD Million) Trend Analysis By Market Taxonomy, 2021 to 2025
- Market Size Value (USD Million) Forecast By Market Taxonomy, 2026 to 2036
- By Country
- Kingdom of Saudi Arabia
- Other GCC Countries
- Turkiye
- South Africa
- Other African Union
- Rest of Middle East & Africa
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- By Country
- Market Attractiveness Analysis
- By Country
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Key Takeaways
- Key Countries Market Analysis
- USA
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Canada
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Mexico
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Brazil
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Chile
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Germany
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- UK
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Italy
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Spain
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- France
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- India
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- ASEAN
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Australia & New Zealand
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- China
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Japan
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- South Korea
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Russia
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Poland
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Hungary
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Kingdom of Saudi Arabia
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Turkiye
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- South Africa
- Pricing Analysis
- Market Share Analysis, 2025
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- USA
- Market Structure Analysis
- Competition Dashboard
- Competition Benchmarking
- Market Share Analysis of Top Players
- By Regional
- By Solution Layer
- By Deployment Model
- By Hospital Type
- By Primary Use Case
- By Commercial Model
- Competition Analysis
- Competition Deep Dive
- TeleTracking
- Overview
- Product Portfolio
- Profitability by Market Segments (Product/Age /Sales Channel/Region)
- Sales Footprint
- Strategy Overview
- Marketing Strategy
- Product Strategy
- Channel Strategy
- GE HealthCare
- LeanTaaS
- Qventus
- Oracle Health
- Palantir
- Systematic (Columna Flow)
- Central Logic (Envisage)
- Care.ai
- Vizzia Technologies
- TeleTracking
- Competition Deep Dive
- Assumptions & Acronyms Used
List of Tables
- Table 1: Global Market Value (USD Million) Forecast by Region, 2021 to 2036
- Table 2: Global Market Value (USD Million) Forecast by Solution Layer , 2021 to 2036
- Table 3: Global Market Value (USD Million) Forecast by Deployment Model, 2021 to 2036
- Table 4: Global Market Value (USD Million) Forecast by Hospital Type, 2021 to 2036
- Table 5: Global Market Value (USD Million) Forecast by Primary Use Case, 2021 to 2036
- Table 6: Global Market Value (USD Million) Forecast by Commercial Model, 2021 to 2036
- Table 7: North America Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 8: North America Market Value (USD Million) Forecast by Solution Layer , 2021 to 2036
- Table 9: North America Market Value (USD Million) Forecast by Deployment Model, 2021 to 2036
- Table 10: North America Market Value (USD Million) Forecast by Hospital Type, 2021 to 2036
- Table 11: North America Market Value (USD Million) Forecast by Primary Use Case, 2021 to 2036
- Table 12: North America Market Value (USD Million) Forecast by Commercial Model, 2021 to 2036
- Table 13: Latin America Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 14: Latin America Market Value (USD Million) Forecast by Solution Layer , 2021 to 2036
- Table 15: Latin America Market Value (USD Million) Forecast by Deployment Model, 2021 to 2036
- Table 16: Latin America Market Value (USD Million) Forecast by Hospital Type, 2021 to 2036
- Table 17: Latin America Market Value (USD Million) Forecast by Primary Use Case, 2021 to 2036
- Table 18: Latin America Market Value (USD Million) Forecast by Commercial Model, 2021 to 2036
- Table 19: Western Europe Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 20: Western Europe Market Value (USD Million) Forecast by Solution Layer , 2021 to 2036
- Table 21: Western Europe Market Value (USD Million) Forecast by Deployment Model, 2021 to 2036
- Table 22: Western Europe Market Value (USD Million) Forecast by Hospital Type, 2021 to 2036
- Table 23: Western Europe Market Value (USD Million) Forecast by Primary Use Case, 2021 to 2036
- Table 24: Western Europe Market Value (USD Million) Forecast by Commercial Model, 2021 to 2036
- Table 25: Eastern Europe Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 26: Eastern Europe Market Value (USD Million) Forecast by Solution Layer , 2021 to 2036
- Table 27: Eastern Europe Market Value (USD Million) Forecast by Deployment Model, 2021 to 2036
- Table 28: Eastern Europe Market Value (USD Million) Forecast by Hospital Type, 2021 to 2036
- Table 29: Eastern Europe Market Value (USD Million) Forecast by Primary Use Case, 2021 to 2036
- Table 30: Eastern Europe Market Value (USD Million) Forecast by Commercial Model, 2021 to 2036
- Table 31: East Asia Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 32: East Asia Market Value (USD Million) Forecast by Solution Layer , 2021 to 2036
- Table 33: East Asia Market Value (USD Million) Forecast by Deployment Model, 2021 to 2036
- Table 34: East Asia Market Value (USD Million) Forecast by Hospital Type, 2021 to 2036
- Table 35: East Asia Market Value (USD Million) Forecast by Primary Use Case, 2021 to 2036
- Table 36: East Asia Market Value (USD Million) Forecast by Commercial Model, 2021 to 2036
- Table 37: South Asia and Pacific Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 38: South Asia and Pacific Market Value (USD Million) Forecast by Solution Layer , 2021 to 2036
- Table 39: South Asia and Pacific Market Value (USD Million) Forecast by Deployment Model, 2021 to 2036
- Table 40: South Asia and Pacific Market Value (USD Million) Forecast by Hospital Type, 2021 to 2036
- Table 41: South Asia and Pacific Market Value (USD Million) Forecast by Primary Use Case, 2021 to 2036
- Table 42: South Asia and Pacific Market Value (USD Million) Forecast by Commercial Model, 2021 to 2036
- Table 43: Middle East & Africa Market Value (USD Million) Forecast by Country, 2021 to 2036
- Table 44: Middle East & Africa Market Value (USD Million) Forecast by Solution Layer , 2021 to 2036
- Table 45: Middle East & Africa Market Value (USD Million) Forecast by Deployment Model, 2021 to 2036
- Table 46: Middle East & Africa Market Value (USD Million) Forecast by Hospital Type, 2021 to 2036
- Table 47: Middle East & Africa Market Value (USD Million) Forecast by Primary Use Case, 2021 to 2036
- Table 48: Middle East & Africa Market Value (USD Million) Forecast by Commercial Model, 2021 to 2036
List of Figures
- Figure 1: Global Market Pricing Analysis
- Figure 2: Global Market Value (USD Million) Forecast 2021-2036
- Figure 3: Global Market Value Share and BPS Analysis by Solution Layer , 2026 and 2036
- Figure 4: Global Market Y-o-Y Growth Comparison by Solution Layer , 2026-2036
- Figure 5: Global Market Attractiveness Analysis by Solution Layer
- Figure 6: Global Market Value Share and BPS Analysis by Deployment Model, 2026 and 2036
- Figure 7: Global Market Y-o-Y Growth Comparison by Deployment Model, 2026-2036
- Figure 8: Global Market Attractiveness Analysis by Deployment Model
- Figure 9: Global Market Value Share and BPS Analysis by Hospital Type, 2026 and 2036
- Figure 10: Global Market Y-o-Y Growth Comparison by Hospital Type, 2026-2036
- Figure 11: Global Market Attractiveness Analysis by Hospital Type
- Figure 12: Global Market Value Share and BPS Analysis by Primary Use Case, 2026 and 2036
- Figure 13: Global Market Y-o-Y Growth Comparison by Primary Use Case, 2026-2036
- Figure 14: Global Market Attractiveness Analysis by Primary Use Case
- Figure 15: Global Market Value Share and BPS Analysis by Commercial Model, 2026 and 2036
- Figure 16: Global Market Y-o-Y Growth Comparison by Commercial Model, 2026-2036
- Figure 17: Global Market Attractiveness Analysis by Commercial Model
- Figure 18: Global Market Value (USD Million) Share and BPS Analysis by Region, 2026 and 2036
- Figure 19: Global Market Y-o-Y Growth Comparison by Region, 2026-2036
- Figure 20: Global Market Attractiveness Analysis by Region
- Figure 21: North America Market Incremental Dollar Opportunity, 2026-2036
- Figure 22: Latin America Market Incremental Dollar Opportunity, 2026-2036
- Figure 23: Western Europe Market Incremental Dollar Opportunity, 2026-2036
- Figure 24: Eastern Europe Market Incremental Dollar Opportunity, 2026-2036
- Figure 25: East Asia Market Incremental Dollar Opportunity, 2026-2036
- Figure 26: South Asia and Pacific Market Incremental Dollar Opportunity, 2026-2036
- Figure 27: Middle East & Africa Market Incremental Dollar Opportunity, 2026-2036
- Figure 28: North America Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 29: North America Market Value Share and BPS Analysis by Solution Layer , 2026 and 2036
- Figure 30: North America Market Y-o-Y Growth Comparison by Solution Layer , 2026-2036
- Figure 31: North America Market Attractiveness Analysis by Solution Layer
- Figure 32: North America Market Value Share and BPS Analysis by Deployment Model, 2026 and 2036
- Figure 33: North America Market Y-o-Y Growth Comparison by Deployment Model, 2026-2036
- Figure 34: North America Market Attractiveness Analysis by Deployment Model
- Figure 35: North America Market Value Share and BPS Analysis by Hospital Type, 2026 and 2036
- Figure 36: North America Market Y-o-Y Growth Comparison by Hospital Type, 2026-2036
- Figure 37: North America Market Attractiveness Analysis by Hospital Type
- Figure 38: North America Market Value Share and BPS Analysis by Primary Use Case, 2026 and 2036
- Figure 39: North America Market Y-o-Y Growth Comparison by Primary Use Case, 2026-2036
- Figure 40: North America Market Attractiveness Analysis by Primary Use Case
- Figure 41: North America Market Value Share and BPS Analysis by Commercial Model, 2026 and 2036
- Figure 42: North America Market Y-o-Y Growth Comparison by Commercial Model, 2026-2036
- Figure 43: North America Market Attractiveness Analysis by Commercial Model
- Figure 44: Latin America Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 45: Latin America Market Value Share and BPS Analysis by Solution Layer , 2026 and 2036
- Figure 46: Latin America Market Y-o-Y Growth Comparison by Solution Layer , 2026-2036
- Figure 47: Latin America Market Attractiveness Analysis by Solution Layer
- Figure 48: Latin America Market Value Share and BPS Analysis by Deployment Model, 2026 and 2036
- Figure 49: Latin America Market Y-o-Y Growth Comparison by Deployment Model, 2026-2036
- Figure 50: Latin America Market Attractiveness Analysis by Deployment Model
- Figure 51: Latin America Market Value Share and BPS Analysis by Hospital Type, 2026 and 2036
- Figure 52: Latin America Market Y-o-Y Growth Comparison by Hospital Type, 2026-2036
- Figure 53: Latin America Market Attractiveness Analysis by Hospital Type
- Figure 54: Latin America Market Value Share and BPS Analysis by Primary Use Case, 2026 and 2036
- Figure 55: Latin America Market Y-o-Y Growth Comparison by Primary Use Case, 2026-2036
- Figure 56: Latin America Market Attractiveness Analysis by Primary Use Case
- Figure 57: Latin America Market Value Share and BPS Analysis by Commercial Model, 2026 and 2036
- Figure 58: Latin America Market Y-o-Y Growth Comparison by Commercial Model, 2026-2036
- Figure 59: Latin America Market Attractiveness Analysis by Commercial Model
- Figure 60: Western Europe Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 61: Western Europe Market Value Share and BPS Analysis by Solution Layer , 2026 and 2036
- Figure 62: Western Europe Market Y-o-Y Growth Comparison by Solution Layer , 2026-2036
- Figure 63: Western Europe Market Attractiveness Analysis by Solution Layer
- Figure 64: Western Europe Market Value Share and BPS Analysis by Deployment Model, 2026 and 2036
- Figure 65: Western Europe Market Y-o-Y Growth Comparison by Deployment Model, 2026-2036
- Figure 66: Western Europe Market Attractiveness Analysis by Deployment Model
- Figure 67: Western Europe Market Value Share and BPS Analysis by Hospital Type, 2026 and 2036
- Figure 68: Western Europe Market Y-o-Y Growth Comparison by Hospital Type, 2026-2036
- Figure 69: Western Europe Market Attractiveness Analysis by Hospital Type
- Figure 70: Western Europe Market Value Share and BPS Analysis by Primary Use Case, 2026 and 2036
- Figure 71: Western Europe Market Y-o-Y Growth Comparison by Primary Use Case, 2026-2036
- Figure 72: Western Europe Market Attractiveness Analysis by Primary Use Case
- Figure 73: Western Europe Market Value Share and BPS Analysis by Commercial Model, 2026 and 2036
- Figure 74: Western Europe Market Y-o-Y Growth Comparison by Commercial Model, 2026-2036
- Figure 75: Western Europe Market Attractiveness Analysis by Commercial Model
- Figure 76: Eastern Europe Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 77: Eastern Europe Market Value Share and BPS Analysis by Solution Layer , 2026 and 2036
- Figure 78: Eastern Europe Market Y-o-Y Growth Comparison by Solution Layer , 2026-2036
- Figure 79: Eastern Europe Market Attractiveness Analysis by Solution Layer
- Figure 80: Eastern Europe Market Value Share and BPS Analysis by Deployment Model, 2026 and 2036
- Figure 81: Eastern Europe Market Y-o-Y Growth Comparison by Deployment Model, 2026-2036
- Figure 82: Eastern Europe Market Attractiveness Analysis by Deployment Model
- Figure 83: Eastern Europe Market Value Share and BPS Analysis by Hospital Type, 2026 and 2036
- Figure 84: Eastern Europe Market Y-o-Y Growth Comparison by Hospital Type, 2026-2036
- Figure 85: Eastern Europe Market Attractiveness Analysis by Hospital Type
- Figure 86: Eastern Europe Market Value Share and BPS Analysis by Primary Use Case, 2026 and 2036
- Figure 87: Eastern Europe Market Y-o-Y Growth Comparison by Primary Use Case, 2026-2036
- Figure 88: Eastern Europe Market Attractiveness Analysis by Primary Use Case
- Figure 89: Eastern Europe Market Value Share and BPS Analysis by Commercial Model, 2026 and 2036
- Figure 90: Eastern Europe Market Y-o-Y Growth Comparison by Commercial Model, 2026-2036
- Figure 91: Eastern Europe Market Attractiveness Analysis by Commercial Model
- Figure 92: East Asia Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 93: East Asia Market Value Share and BPS Analysis by Solution Layer , 2026 and 2036
- Figure 94: East Asia Market Y-o-Y Growth Comparison by Solution Layer , 2026-2036
- Figure 95: East Asia Market Attractiveness Analysis by Solution Layer
- Figure 96: East Asia Market Value Share and BPS Analysis by Deployment Model, 2026 and 2036
- Figure 97: East Asia Market Y-o-Y Growth Comparison by Deployment Model, 2026-2036
- Figure 98: East Asia Market Attractiveness Analysis by Deployment Model
- Figure 99: East Asia Market Value Share and BPS Analysis by Hospital Type, 2026 and 2036
- Figure 100: East Asia Market Y-o-Y Growth Comparison by Hospital Type, 2026-2036
- Figure 101: East Asia Market Attractiveness Analysis by Hospital Type
- Figure 102: East Asia Market Value Share and BPS Analysis by Primary Use Case, 2026 and 2036
- Figure 103: East Asia Market Y-o-Y Growth Comparison by Primary Use Case, 2026-2036
- Figure 104: East Asia Market Attractiveness Analysis by Primary Use Case
- Figure 105: East Asia Market Value Share and BPS Analysis by Commercial Model, 2026 and 2036
- Figure 106: East Asia Market Y-o-Y Growth Comparison by Commercial Model, 2026-2036
- Figure 107: East Asia Market Attractiveness Analysis by Commercial Model
- Figure 108: South Asia and Pacific Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 109: South Asia and Pacific Market Value Share and BPS Analysis by Solution Layer , 2026 and 2036
- Figure 110: South Asia and Pacific Market Y-o-Y Growth Comparison by Solution Layer , 2026-2036
- Figure 111: South Asia and Pacific Market Attractiveness Analysis by Solution Layer
- Figure 112: South Asia and Pacific Market Value Share and BPS Analysis by Deployment Model, 2026 and 2036
- Figure 113: South Asia and Pacific Market Y-o-Y Growth Comparison by Deployment Model, 2026-2036
- Figure 114: South Asia and Pacific Market Attractiveness Analysis by Deployment Model
- Figure 115: South Asia and Pacific Market Value Share and BPS Analysis by Hospital Type, 2026 and 2036
- Figure 116: South Asia and Pacific Market Y-o-Y Growth Comparison by Hospital Type, 2026-2036
- Figure 117: South Asia and Pacific Market Attractiveness Analysis by Hospital Type
- Figure 118: South Asia and Pacific Market Value Share and BPS Analysis by Primary Use Case, 2026 and 2036
- Figure 119: South Asia and Pacific Market Y-o-Y Growth Comparison by Primary Use Case, 2026-2036
- Figure 120: South Asia and Pacific Market Attractiveness Analysis by Primary Use Case
- Figure 121: South Asia and Pacific Market Value Share and BPS Analysis by Commercial Model, 2026 and 2036
- Figure 122: South Asia and Pacific Market Y-o-Y Growth Comparison by Commercial Model, 2026-2036
- Figure 123: South Asia and Pacific Market Attractiveness Analysis by Commercial Model
- Figure 124: Middle East & Africa Market Value Share and BPS Analysis by Country, 2026 and 2036
- Figure 125: Middle East & Africa Market Value Share and BPS Analysis by Solution Layer , 2026 and 2036
- Figure 126: Middle East & Africa Market Y-o-Y Growth Comparison by Solution Layer , 2026-2036
- Figure 127: Middle East & Africa Market Attractiveness Analysis by Solution Layer
- Figure 128: Middle East & Africa Market Value Share and BPS Analysis by Deployment Model, 2026 and 2036
- Figure 129: Middle East & Africa Market Y-o-Y Growth Comparison by Deployment Model, 2026-2036
- Figure 130: Middle East & Africa Market Attractiveness Analysis by Deployment Model
- Figure 131: Middle East & Africa Market Value Share and BPS Analysis by Hospital Type, 2026 and 2036
- Figure 132: Middle East & Africa Market Y-o-Y Growth Comparison by Hospital Type, 2026-2036
- Figure 133: Middle East & Africa Market Attractiveness Analysis by Hospital Type
- Figure 134: Middle East & Africa Market Value Share and BPS Analysis by Primary Use Case, 2026 and 2036
- Figure 135: Middle East & Africa Market Y-o-Y Growth Comparison by Primary Use Case, 2026-2036
- Figure 136: Middle East & Africa Market Attractiveness Analysis by Primary Use Case
- Figure 137: Middle East & Africa Market Value Share and BPS Analysis by Commercial Model, 2026 and 2036
- Figure 138: Middle East & Africa Market Y-o-Y Growth Comparison by Commercial Model, 2026-2036
- Figure 139: Middle East & Africa Market Attractiveness Analysis by Commercial Model
- Figure 140: Global Market - Tier Structure Analysis
- Figure 141: Global Market - Company Share Analysis
Full Research Suite comprises of:
Market outlook & trends analysis
Interviews & case studies
Strategic recommendations
Vendor profiles & capabilities analysis
5-year forecasts
8 regions and 60+ country-level data splits
Market segment data splits
12 months of continuous data updates
DELIVERED AS:
PDF EXCEL ONLINE

